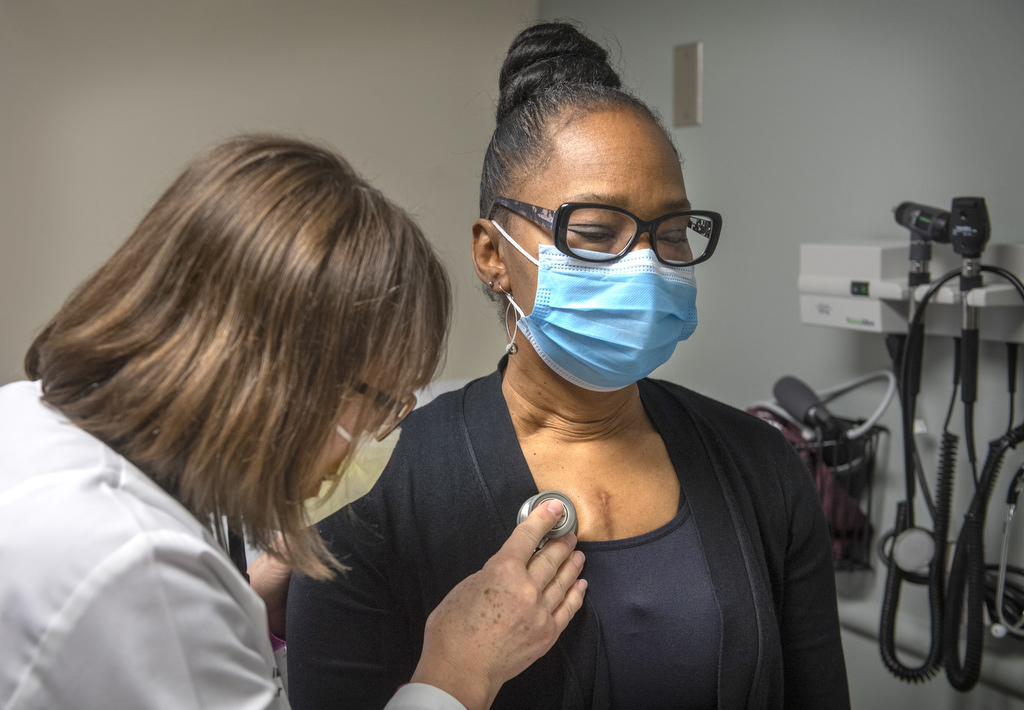
People who worked alongside Katie Watkins at their church’s after-school enrichment program wouldn’t have guessed she was navigating heart failure.
Watkins didn’t look like someone with cardiomyopathy. She served as education director for the after-school program and did school pickups for her young grandchildren and other kids. She kept her calendar packed with activities.
“I was doing the grandma thing, doing the volunteer thing, just doing everything,” said Watkins, 58, a retired U.S. Department of Defense supervisor from Battle Creek, Michigan, who’s known to her grandkids as “Gram-Gram.”
Watkins kept moving at this pace nearly right up to her heart transplant in June 2021.
Month after month, she “miraculously continued to feel great,” she said. But in the fall of 2020, quarterly visits with her local cardiologist began to tell a different story.
Unexpected news
Watkins had become a cardiac patient in 2017, when she first developed symptoms that led to a diagnosis of heart failure—shortness of breath and a persistent cough.
Her cardiologist prescribed appropriate medications and set her up with an external heart monitor. Later that year, Watkins had a biventricular pacemaker implanted to help keep her heart rhythm in sync.
Her health remained stable for the next three years.
But in 2020, her cardiac function declined. Even with adjusted medications, her heart no longer responded to drug therapy.
“In my mind, I was still moving around and doing things I normally do, but not realizing I was operating at a much slower pace,” Watkins said.
When an echocardiogram showed that her weakened heart had become further enlarged, her longtime cardiologist expressed concern.
He referred Watkins to the Advanced Heart Failure program at Spectrum Health Fred and Lena Meijer Heart Center.
“Her cardiologist said, ‘Though she seems to be fine, this echo shows a further decline. I think it’s better if she’s evaluated at a larger center, just in case she needs advanced therapies,’” said Renzo Loyaga-Rendon, MD, PhD, an advanced heart failure specialist with the Spectrum Health HOPE (Heart OPtimization and Evaluation) clinic.
That turned out to be a timely decision.
Dr. Loyaga reviewed Watkins’ case and confirmed her cardiologist’s concerns.
“Though she was stable, she was a high-risk patient with a chance of decompensating very quickly, in a few months,” he said.
Watkins and her husband, Levi, didn’t fully understand the implications of the referral when they first met Dr. Loyaga in November 2020. So Dr. Loyaga walked the couple through her cardiac journey leading to that day.
After recommending two tests to further evaluate her risk, he delivered some unexpected news: Watkins was a good candidate for a heart transplant or a mechanical heart pump called an LVAD.
“I think the first reaction from her and her husband was a bit like—you know, they couldn’t believe it. Like, ‘I’m feeling fine. How come you’re now talking about all this?’” he said.
It took time for the shock to wear off.
“That was a quiet ride home,” Watkins said. “For a little while it didn’t even seem like it was real.”
Second opinion
Despite talk of a heart transplant, Watkins felt well enough to continue her volunteer work.
Her church had opened a virtual learning center in the early months of the COVID-19 pandemic to support K-12 schoolchildren whose parents still had to go to work. She directed the program.
Meanwhile, she returned to Spectrum Health for a cardiopulmonary stress test and a right cardiac catheterization. Results supported Dr. Loyaga’s concerns and led to a comprehensive pre-transplant evaluation.
At the multidisciplinary committee meeting that followed, Watkins’ testing data prompted the team to act.
“This was one of the very few meetings where we said, ‘Well, the patient feels fine. Her symptoms are minimal. She’s never been admitted to the hospital for a heart failure exacerbation. However, the objective data is serious,’” Dr. Loyaga said.
“So we recommended that she be listed for transplant.”
Watkins acknowledged the doctors’ recommendation but wasn’t ready to say yes. Facing a decision this big, she wanted confirmation from a second source.
Dr. Loyaga agreed to share her records with another advanced heart center of her choice.
“I explained to her that I’m a supporter of second opinions,” he said. “The only recommendation I had is that she gets it very soon.”
Watkins set up a consultation in March 2021 with an out-of-state transplant cardiologist, who ended up agreeing with the Spectrum Health team’s recommendation.
“Dr. Loyaga took the time to research the hospital and the cardiologist with us ahead of time to ensure we were comfortable and made an informed choice,” she said. “It just helped me to say, ‘Go ahead, let’s do it.’”
When she returned to Dr. Loyaga, he underscored the urgency of her situation.
“He sat down and said, ‘I’ll tell you like I would if I was talking to my mom: I would go ahead and do it sooner rather than later,’” she said.
“The way he said it and the concern I could feel … made me very comfortable and confident, really, about saying, ‘OK, today is the day to say OK.’”
Stroke and delay
Watkins didn’t anticipate the disruption waiting around the corner.
No sooner had she signed the papers initiating the heart transplant process than she experienced a setback that made her temporarily ineligible for the transplant list.
In mid-April 2021, while preparing for a meeting at her church, Watkins temporarily lost the use of her right arm. She dropped what she was holding and needed help to make it to a chair.
She went to a local emergency department, where doctors ordered a CT scan and diagnosed her with a transient ischemic attack, or TIA, sometimes called a mini-stroke.
Her neurologic function returned to normal.
“It had no impact—I didn’t lose any memory, I didn’t lose any functionality of any limbs or anything like that. That is a blessing from the Lord,” she said.
Still, Watkins reported the experience to Dr. Loyaga, who called her to Grand Rapids for further assessment. When she arrived that day, he admitted her to the hospital and officially listed her for transplant.
“If it was a TIA—even if it was already resolved—that TIA was coming from her heart, and that’s a big problem,” he said. “If it was a TIA, she needed to be transplanted right away.”
He wasn’t willing to risk a recurrence.
The next day, however, an MRI showed evidence of a stroke, not simply a transient ischemic attack. Watkins came under the care of a neurologist—and her name came off the active transplant list.
“With a new stroke and the chance of bleeding, she became transplant ineligible for a few months,” Dr. Loyaga explained.
Once stable, Watkins went home to give her body time to recover from the stroke. The transplant team kept close tabs on her while she waited.
“I was worried about Katie the whole time,” said Jenee Carney, RN, BSN, her pre-transplant coordinator.
“I was very excited when we activated her, but then having to inactivate her for the stroke was kind of stressful. Just like, ‘How long do we have before she has another complication?’”
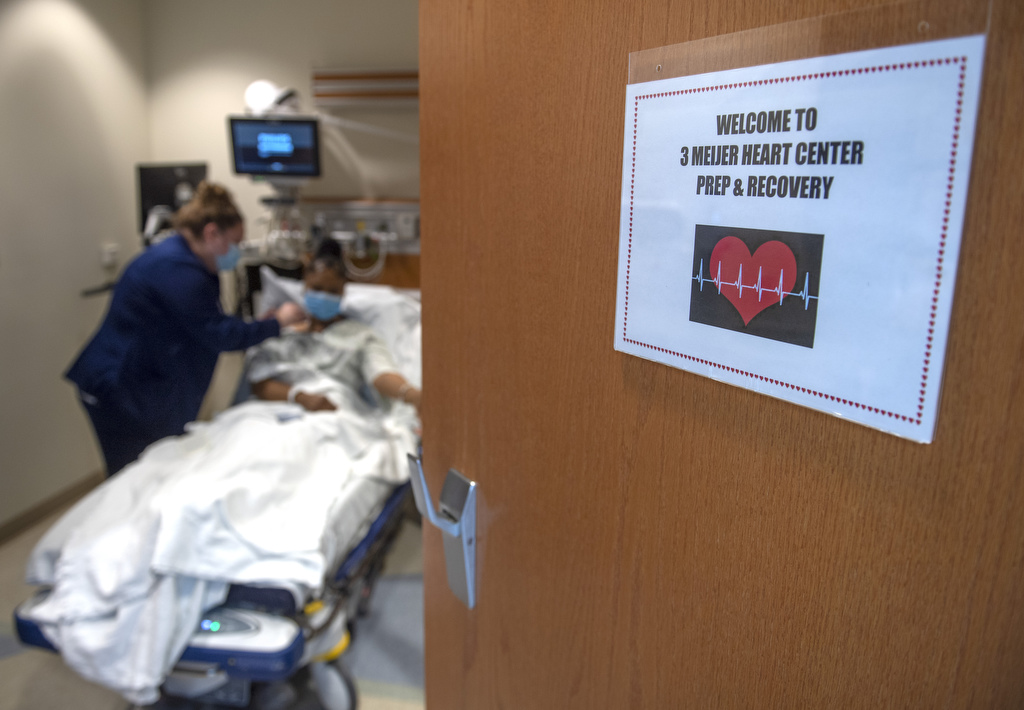
Heart transplant
Watkins’ weekly bloodwork showed evidence of declining cardiac function. By early June, the transplant team felt they couldn’t wait any longer, so Dr. Loyaga called her back to the hospital.
“We decided that it was the time for transplant,” he said. “So she was (re)activated in the transplant list.”
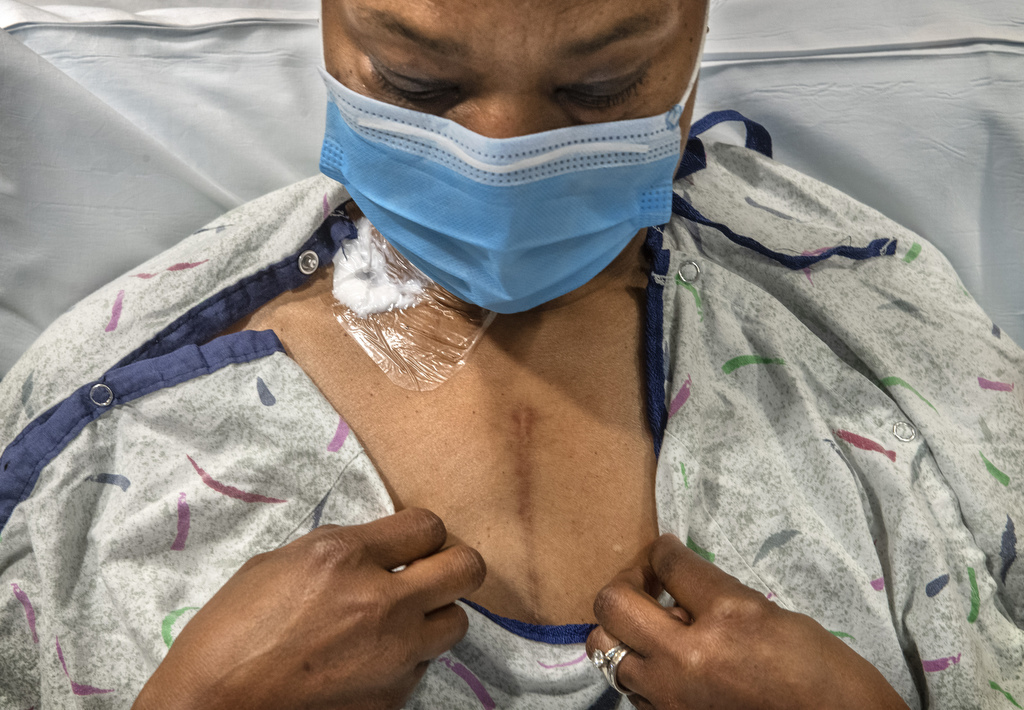
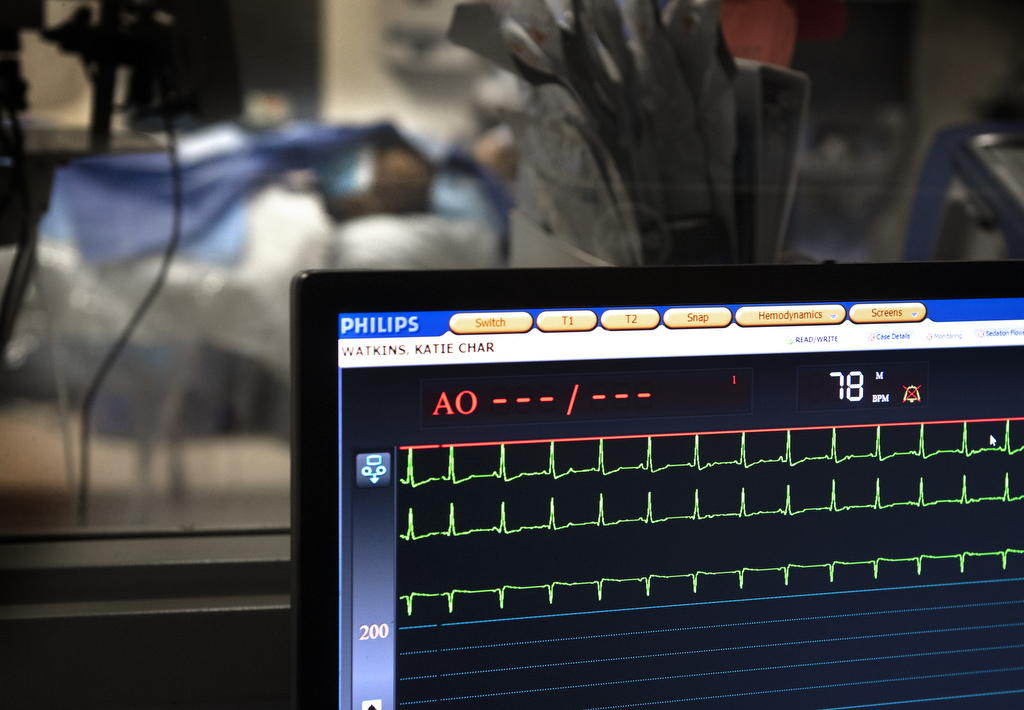
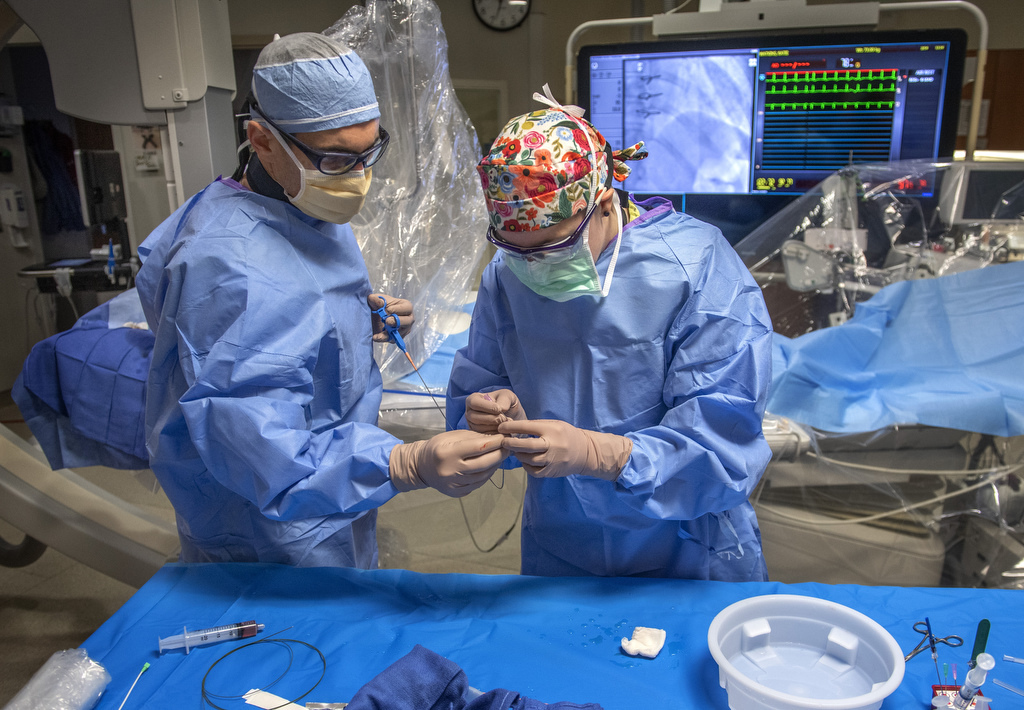
Watkins returned to Spectrum Health on June 9. Using Swan-Ganz catheterization to monitor her cardiac output, doctors saw “she was in trouble,” according to Marzia Leacche, MD, the cardiothoracic surgeon who would eventually perform her transplant.
Two days later, interventional cardiologist Duane Berkompas, MD, placed a balloon pump in her aorta to support her heart while she waited for a donor match.
The waiting could have lasted three months, but it took only three days.
Watkins’ husband hadn’t yet arrived for the day when Dr. Leacche walked into her room on June 14.
“She said, ‘We found a heart … and we’re going to propose to give it to you,’” Watkins said. “And immediately I, of course, just started to cry.”
It’s unusual for a matching donor heart to come through so quickly, especially when a patient hasn’t yet moved up to the highest priority status, Dr. Leacche said. In Watkins’ case, there were two reasons for the speedy match—her small body size and her Type B blood.
“In heart transplantation, if you’re a smaller size and you have a different blood type than the majority of the people, then you have more chance to get the heart sooner,” she said.
“So this was something that thankfully came to her quite quickly. … I was very excited to deliver the news.”
Both the transplant surgery and Watkins’ recovery went smoothly, Dr. Leacche said. What stands out for her is Watkins’ emotional strength.
“She really trusted the medical team and she was able to really wrap her head around all these challenges that she would face in a very short period of time,” Dr. Leacche said.
“She was very resilient.”
Support from family and friends bolstered her during this intense time, Watkins said.
“I didn’t know till afterwards,” she said, her voice breaking, “that between my family and my friends … they actually stayed up from the time I went to surgery until the surgery was over and Levi told them I was done, just praying and talking to each other.”
That level of support is a testament to the kind of person Watkins is, her transplant coordinators said.
“She’s just a delightful person. Anybody who meets her instantly falls in love with her,” Carney said.
“She is a very kind soul,” echoed Megan Stickroe, RN, BSN, Watkins’ post-transplant coordinator. “And she’s really fun to teach because she really enjoys knowing and understanding why we do what we do.”
Return to health
After Watkins’ discharge in July, Stickroe met with her weekly, then monthly, to coordinate her post-op rehab and testing. December 2021 marked six months post-transplant.
“She’s medically been kind of flying by,” Stickroe said. “It’s fun to see her have her energy back.”
Watkins has already started easing back into her daily routines, driving her grandkids to and from the after-school program at church. When she feels strong enough, she plans to return to the program full time.
She also wants to be a resource for patients with heart issues and those facing a transplant.
Watkins’ case is a perfect example of the body’s ability to adapt when things go wrong, Dr. Loyaga said—and the fact that her original cardiologist knew when to refer her is a critical part of her story.
“If the heart function declines slowly over time, our body just adapts to that decreased function,” he said. “However, her doctor was able to identify a couple of signs that she was in a poor trajectory.
“He sent her to us at just the right time.”









 /a>
/a>
 /a>
/a>
 /a>
/a>
I am truly proud of my dear friend, my sister in Christ. Her strength in the Lord through this journey is a testament to her faith and love of the Lord, family, and friends. I’m a witness to her resilience, fortitude, and determination to be victorious in all aspects of her life. I’m blessed to have her in my life.
What a beautiful story for a beautiful lady! Thank you to all of the medical personnel that worked with her. Thank you Katie for being my friend and sharing your story. To GOD be all the glory for the great things he has done…
Katie is a walking miracle, and a true woman of God. Watching her go through thus journey and seeing God take her to the other side is truly inspirational. The doctors, the family, the friends, all played a part. She is truly deserving.
We thank God for her life, and thank the donor for checking that box.
Praise God 🙏🏿
I’m so happy that divine intervention happened at the right time at the right moment and at the right place for my college friend. It’s all God and the knowledge and insight he gave her physicians and medical personnel. What a great and inspirational story and may God continue to gift the medical personnel to become even better at their craft and may Katie go on to do great things in her journey on Earth
I feel and believe the Holy Spirit leading, intervening and guiding every aspect of sister Katie’s Heart/ Life from the letter A in the beginning sentence,. “A New Heart for Gram Gram”!
I have had the opportunity to interact with sister Katie in some extremely fun and good times as well as some extremely difficult situations.
I have the utmost respect for her as a person, I affectionately call her (Mrs. Obama), I consider her my friend as I believe she is to anyone she encounters BUT more than anything I believe her life is a reflection of her belief and faith in God our Father, our Lord Jesus Christ I believe her not only filled with the Holy Spirit but lead…She Is A Saint!
Her Miracle testimonies (seeds) her life will plant, water and grow much Harvest.
I am blessed to know you.
I Thank God for you
Much love ❤sister🍒cherry
Beautiful story and the beautiful person you are inside and out..
God is so amazing, always at the right place at the right time! Katie is a dear friend and I’m glad God allowed her to continue to live out his will! Thank you to all the doctors, nurses and staff who have been apart of this journey! We have been truly blessed to still have Katie with us because our your diligence! I’m overwhelmed with joy! To God I give all the glory! Love you Katie!!!