When Alan Barchett showed up for his doctor’s appointment one day in March 2019, he suspected he had a urinary tract infection.
He’d been waking each night to use the bathroom.
“And then I’d realize I was really thirsty and pour myself a big glass of juice,” he said.
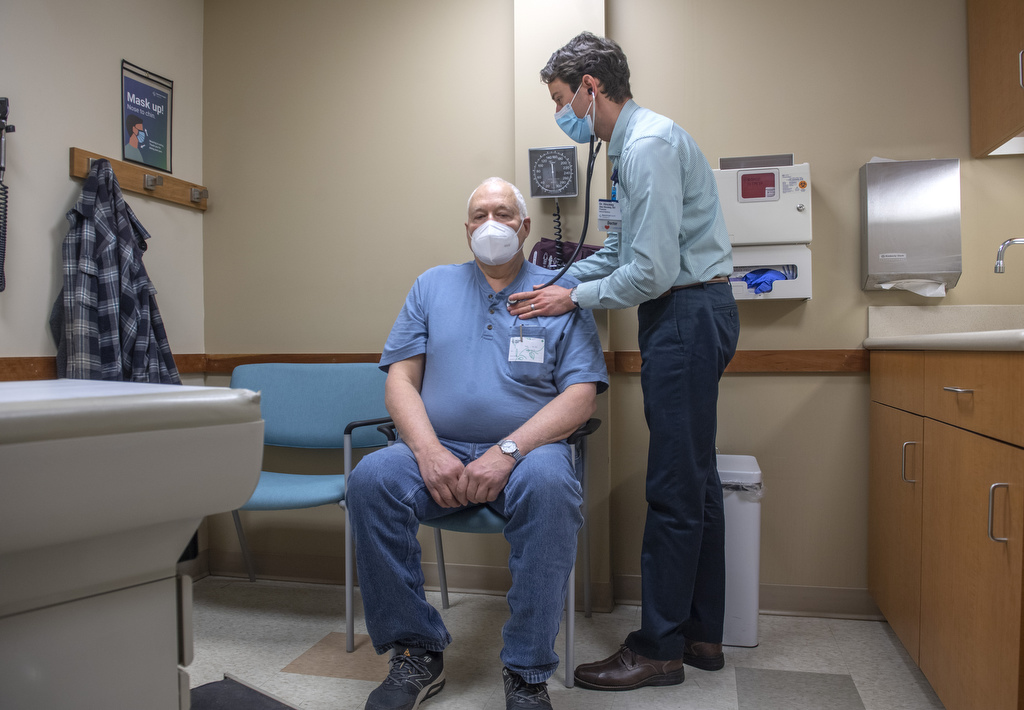
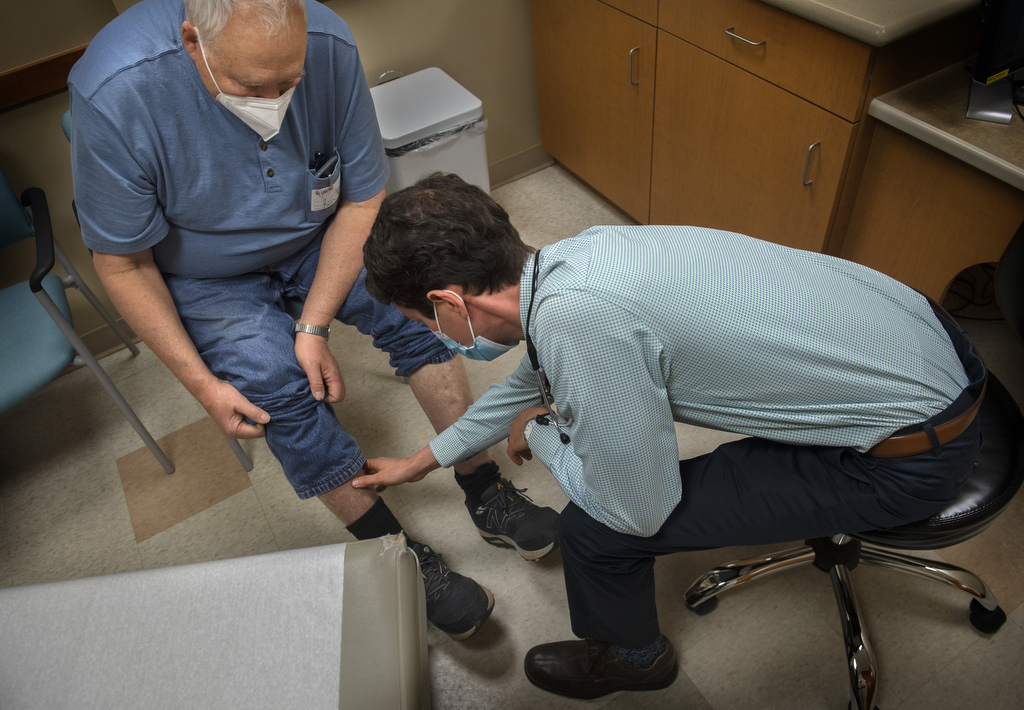
He anticipated that Alexander Hinckley, DO, his doctor at Spectrum Health Lakeland Medical Center, would agree. And he figured he’d leave the office with a prescription for antibiotics and be on his way home in no time.
That’s not what happened.
“I told him that he had horribly uncontrolled diabetes,” Dr. Hinckley said.
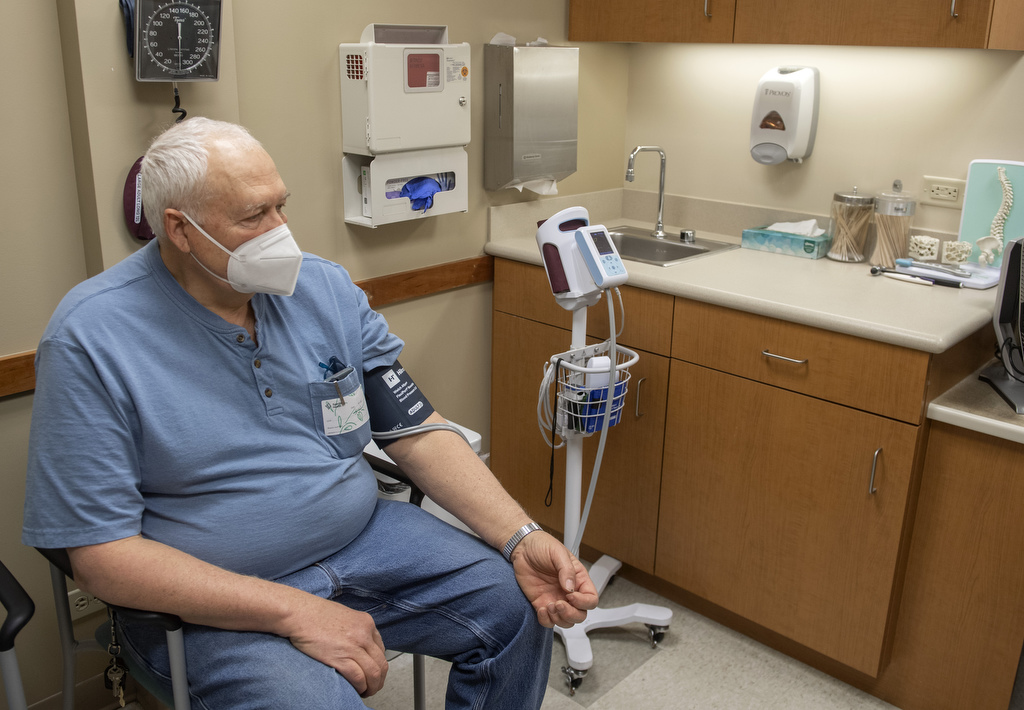
Barchett’s blood sugar levels registered in the 400s. Healthy levels are below 99 mg/dL.
The news stunned Barchett.
“In hindsight, it’s funny that I could have been so oblivious to what I now know are classic diabetes symptoms,” he said.
Barchett would need to inject daily insulin, likely for the rest of his life, Dr. Hinckley said. And he’d need to change his diet drastically.
“You mean, like starting today?” Barchett remembers asking.
“Yes, starting today,” Dr. Hinckley advised.
An abrupt change
Dr. Hinckley had no idea how seriously Barchett would take him.
Barchett met with Spectrum Health patient educators, who explained how to administer insulin injections on his own. They also suggested he change his diet.
“I asked if there was anything I could do to change this, to not need the insulin anymore,” he recalled.
“They told me that some people—although by no means all—can reverse symptoms by lifestyle changes alone,” he said. “And if I would radically change the way I eat, I might be able to use less of the medication. Or maybe even none at all.”
That’s all Barchett, now 68, needed to hear.
“I changed everything, cold turkey,” he said.
Although they told him he could maintain a healthy diet by carefully monitoring the carbs he consumed, Barchett wanted a stricter approach.
“I cut out all the carbohydrates,” he said. “No potatoes, rice, pasta, bread. I eliminated all that.”
Several months later, he returned for a checkup. By then, he’d lost weight and dramatically lowered his A1C level.
“Dr. Hinckley cut my insulin dosage by half,” Barchett said.
Then, at his next visit several months later, those numbers were even lower. Again, Dr. Hinckley decreased the insulin.
“And at the visit after that, he told me my sugar levels had improved so much that I didn’t need insulin,” Barchett said.
Dr. Hinckley switched Barchett to metformin, an oral medication used to help manage blood sugar. After several months, his A1C had improved so much that Dr. Hinckley took him off that, too.
“He told me I didn’t need to take anything,” Barchett said.
“Within one year, Alan went from having blood sugar readings in the 400s to not being a diabetic at all,” Dr. Hinckley said.
That kind of remission is possible, but not easy, the doctor said.
It typically requires weight loss and careful eating—the kind of lifestyle changes many people find difficult to maintain.
Dr. Hinckley estimates that, among his many patients with diabetes, only about half a dozen have achieved healthy blood-sugar levels with no medication.
But most can significantly improve their condition with less extreme effort.
Ongoing research from the Diabetes Prevention Program shows that losing 5% to 7% of body weight and logging an average of 150 minutes of physical activity each week can reduce the risk of developing diabetes by 58%.
And it can help reduce the need for medication for those who have already been diagnosed.
Dr. Hinckley said Barchett also has a secret weapon in his efforts: a supportive family. Marilyn, Barchett’s wife, has been on board from the beginning.
Often, Dr. Hinckley said, “patients find the diabetes diagnosis very discouraging. So when we have a spouse who is willing to help, it’s like finding the golden ticket.”
A new way of eating
It can often take people some time to truly enjoy a new eating style, as Barchett has, Dr. Hinckley said.
He often counsels patients to explore a Mediterranean diet with plenty of vegetables, fruits and healthy oils.
And he urges them to explore online resources.
Spectrum Health Lifestyle Medicine provides a wealth of healthy recipe ideas.
The American Diabetes Association offers helpful information, along with plenty of recipes. MyPlate has quizzes, recipes and more to help people identify healthier and easy-to-follow eating plans.
Dr. Hinckley also likes the resources at the Culinary Medicine Program, a collaboration of health care providers, nutritionists and researchers.
The point is to find an approach to carb-counting that can help get glucose readings back in range and sustainable over time.
For many people, that might be a less draconian approach than Barchett’s.
“It’s got to be about meeting the patient where they are and assessing what they’re willing to do,” Dr. Hinckley said. “Patient engagement plays the biggest role here. If they’re willing to make drastic changes, I’ll meet them there.”
Barchett has found it easy to stick with his new way of eating. He weighs 34 pounds less than on the day of his diagnosis.
“I keep away from all candies, ice cream, pies and cakes,” he said. “I haven’t had a doughnut in three years. Not even a fast-food hamburger.”
A rare cheat meal might entail sharing a few of his wife’s french fries when they go out to eat. His only sweets are fresh fruits.
“My idea of a splurge is a banana or some grapes,” Barchett said.
At restaurants, he chooses broiled fish or a salad.
“I’ve even gotten used to them without Thousand Island dressing, my old favorite.”
And he still monitors his blood sugar levels periodically to ensure he’s on the right path.
Exercise is part of his routine, too. He walks the country roads near his farm in Watervliet, Michigan, and often picks up trash along the way to keep things interesting.
“The other day, I picked up $5 in cans.”
Staying active is critical, Dr. Hinckley said.
“It helps mobilize your insulin, which allows glucose to be taken up by your body better,” he said.
Exercise also helps control blood sugar levels and reduces the risk of heart disease and nerve damage.
Barchett has turned his life around, Dr. Hinckley said.
“I’ve never had anybody who’s been quite so proactive about managing their health,” he said. “And I’m so glad. I use him as a benchmark for proving that dietary changes really can help.”













 /a>
/a>
 /a>
/a>
 /a>
/a>
So inspiring! Well done, Mr Barchett! Keep up the amazing work!