In the days before his jaw surgery, Wyatt Peterson kept hearing the same question: Are you ready for it?
His answer: Yes and no.
“I’m a little nervous,” he said. “But I’m excited for the end result. I can’t wait.”
Wyatt’s lower right jaw did not develop properly before birth.
Now 18, he prepared to undergo facial reconstruction using an innovative technique pioneered by two pediatric craniofacial plastic surgeons at Spectrum Health Helen DeVos Children’s Hospital.
They planned to implant a prosthetic jawbone and joint, custom-designed for Wyatt’s face, to bring the right side into alignment with the left.
Having that symmetry, for the first time in his life, was a longtime dream.
“Now that I’m grown up, it’s not that big of a deal,” Wyatt said. “But as a kid, I really wanted it done.”
‘Little warrior’
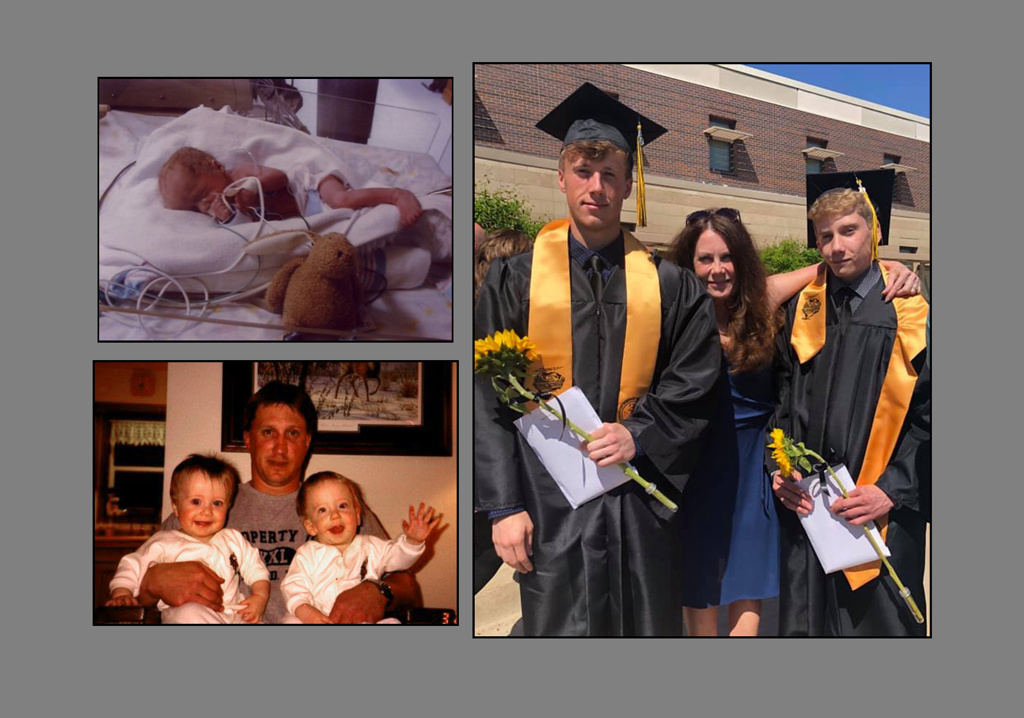
Eighteen years ago, Wyatt arrived—with his twin brother, Logan—about seven weeks early.
Each baby weighed about 3 1/2 pounds. They could nestle into the palm of one hand, said their dad, Joe Peterson. They spent the first month in a neonatal intensive care unit, gaining strength and weight.
But Wyatt faced an extra challenge. On his first day of life, he had to undergo surgery to connect his esophagus to his stomach.
And within a few days, doctors told his parents Wyatt had Goldenhar syndrome, a rare condition that affects the development of the eye, ear and spine.
It often affects the structure of the face.
For the blue-eyed, blond-haired Wyatt, it meant a very small right jawbone.
As Wyatt’s mom, Kris Peterson, absorbed the news of his diagnosis, she vowed to keep it in perspective.
“We decided we weren’t going to label him with that,” she said. “He is so much more than that.”
He faced unique medical challenges as he grew.
As an infant, he received extensive occupational therapy to learn how to eat, with the restricted opening in his jaw.
He had scoliosis in his back and the vertebrae in his neck were fused together. He underwent surgery to repair a cleft in his jaw and surgery to remove skin tags. Doctors also removed a dermoid in his eye.
But Wyatt lived up to his name, which means “little warrior.”
Competitive, quick-witted and determined, he kept up with his twin, Logan, and younger brother, Connor.
“He was not going to be left behind,” Joe said.
He excelled at school. He spent a lot of time fishing with his family in the backyard pond.
And he loved sports. He played baseball, soccer and basketball.
“His twin brother is naturally athletic,” Kris said. “Wyatt has always had to work really hard at that.
“But I always said Wyatt has the mind of an athlete.”
He found his own sports niche in a unique way.
When medical issues forced him to quit the high school basketball team after his freshman year, he became a team manager.
He held the position for the next three years. He did so well he earned a scholarship to manage the basketball team at Mount Mercy University in Iowa—the first such scholarship the school ever awarded.
Ready for a new jaw
After he graduated from high school and before he started college, the time came for the last major surgery on his jaw.
His mom researched the options available before they settled on the technique pioneered by John Polley, MD, and John Girotto, MD, at Helen DeVos Children’s Hospital.
The operation involves a prosthetic jawbone and joint, like the implants created for people who have severe arthritis or injuries to the face. Those implants are designed to replace the person’s existing jaw.
But for Wyatt and those born with little or no jawbone, the surgeons must use specialized computer software to determine the unique dimensions and shape of the implant needed.
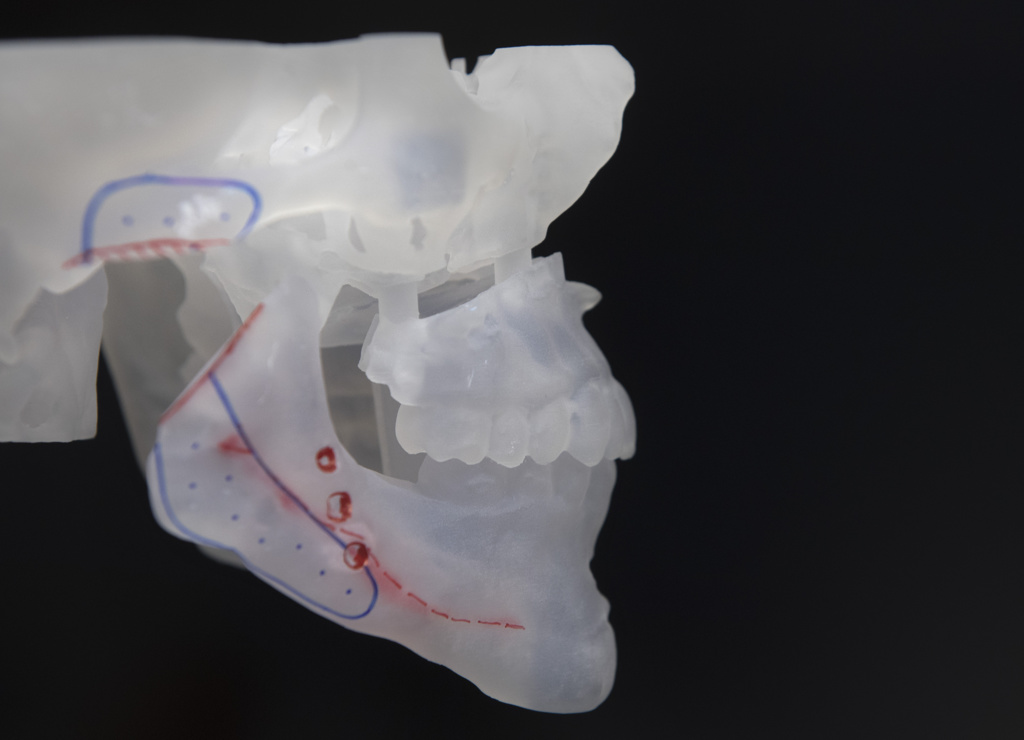
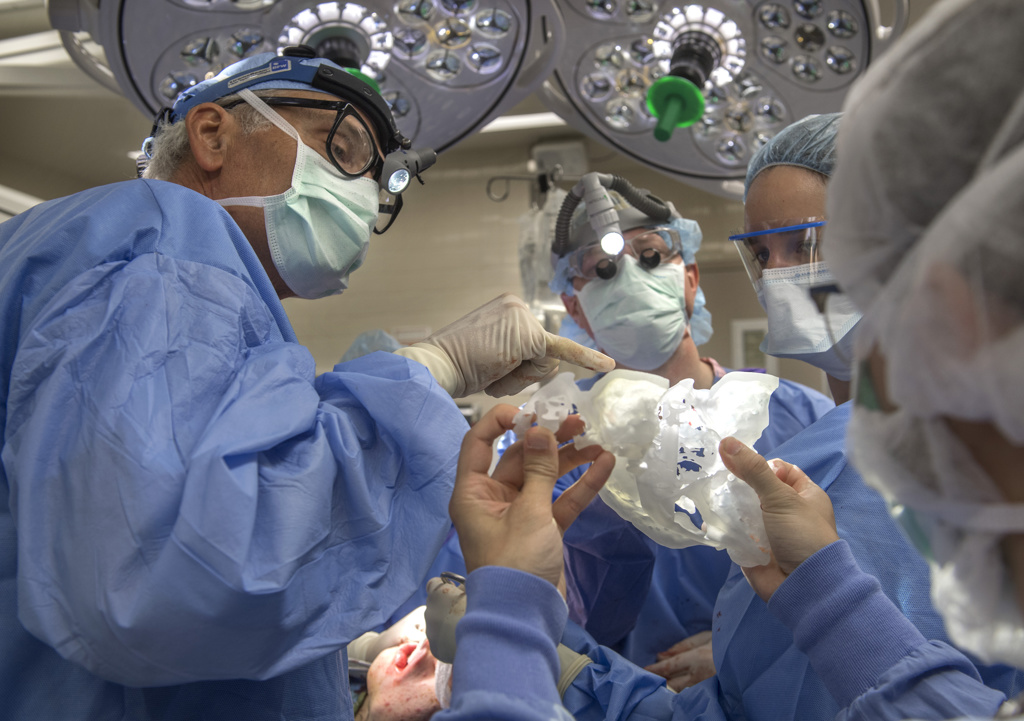
Using the surgeons’ data, TMJ Concepts, a California company, fabricates a custom silicone joint and titanium jawbone. They also print a 3D model of the patient’s face, which shows how the prosthesis will fit.
The surgeons hope this new approach will help other children born with hemifacial microsomia—the congenital condition in which one side of the face is underdeveloped.
In December 2018, they published a study in the Cleft Palate Craniofacial Journal, which discusses the successful use of the technique in 10 patients. In September 2019, Dr. Polley presented his findings at the International Society for Craniofacial Surgeons’ conference in Paris.
“In the past, a lot of patients have had distraction (a surgical technique) to try to stretch the bone,” Dr. Polley said. “The bottom line is there is just not enough of his own material to put things into a normal position.
“We think this (new approach) is the technique of choice now for these patients, in terms of functional rehabilitation and aesthetics.”
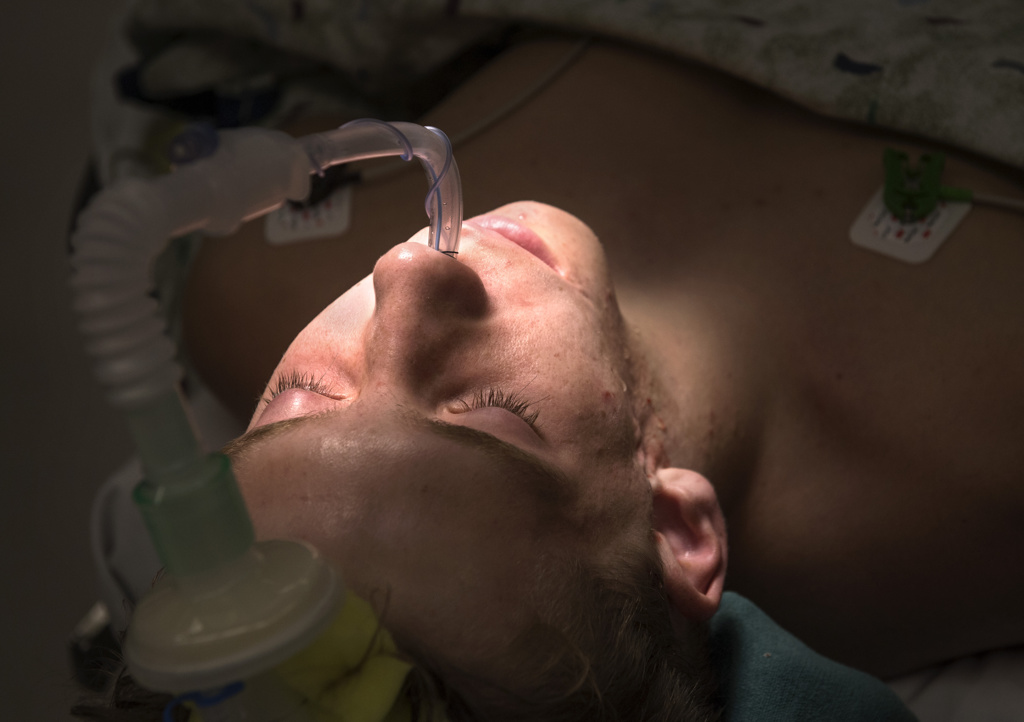
In early July, Wyatt and his parents drove six hours from their home in Center Point, Iowa, to Grand Rapids, Michigan, for the surgery.
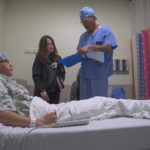
Dr. Polley and Dr. Girotto performed the surgery with assistance from Thomas O’Toole, MD, an otolaryngologist who specializes in head and neck surgery.
They first removed the metal plates and screws from his previous surgery. Then they implanted his prosthetic jawbone and joint. They also reworked the upper jaw, bringing it forward and shifting it over a bit so it aligned with the center of his face.
The surgery complete, they wired his jaws shut to give everything time to heal.
‘I really like the outcome’
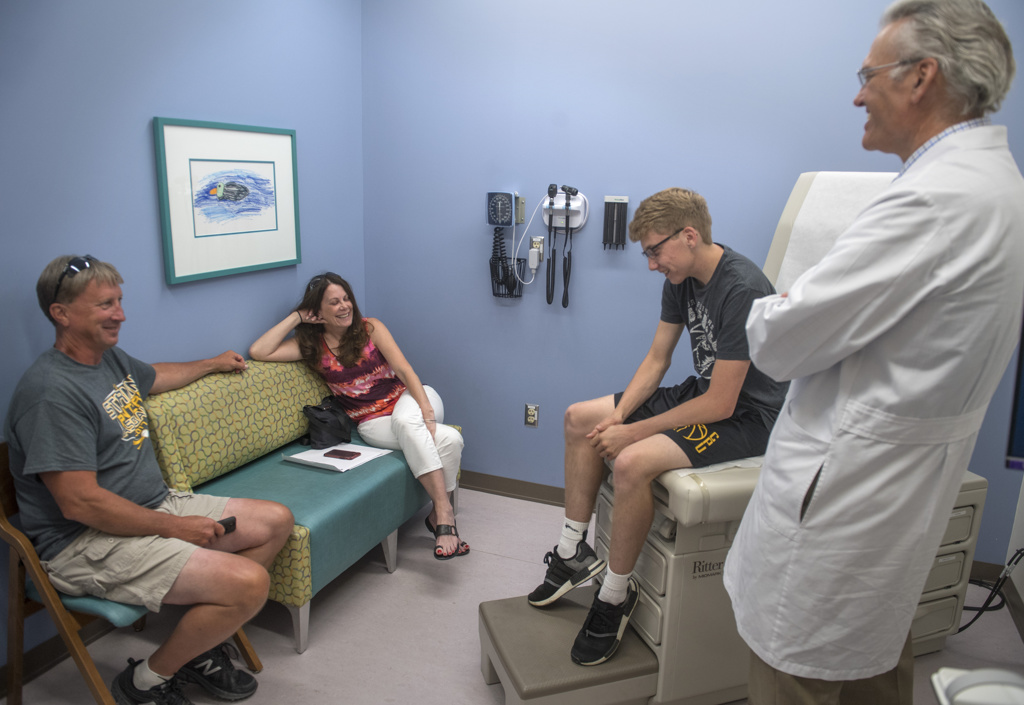
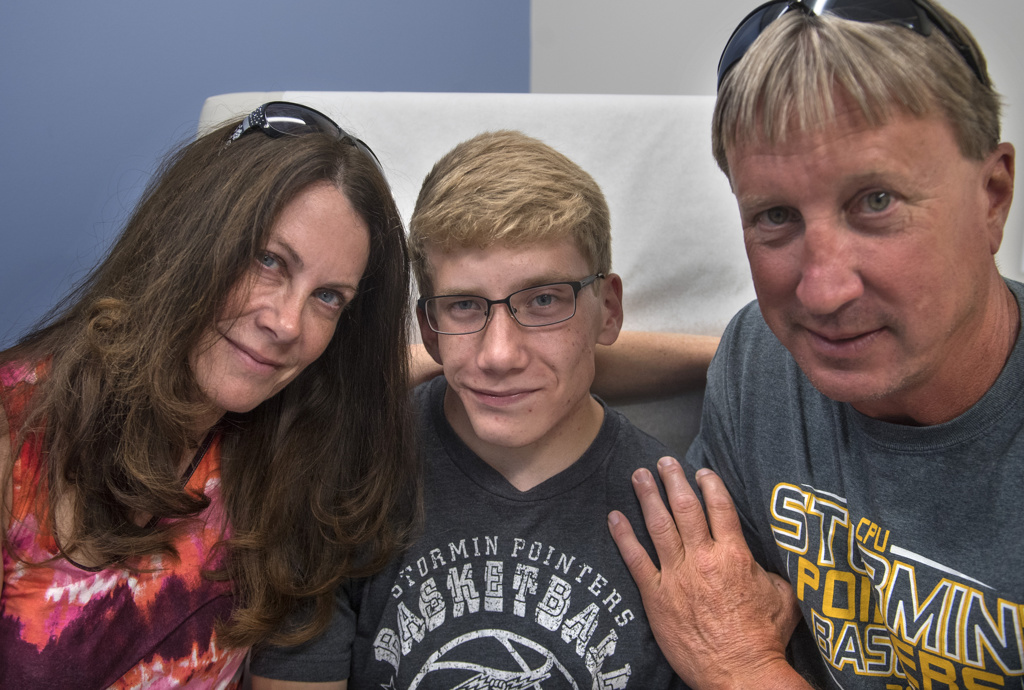
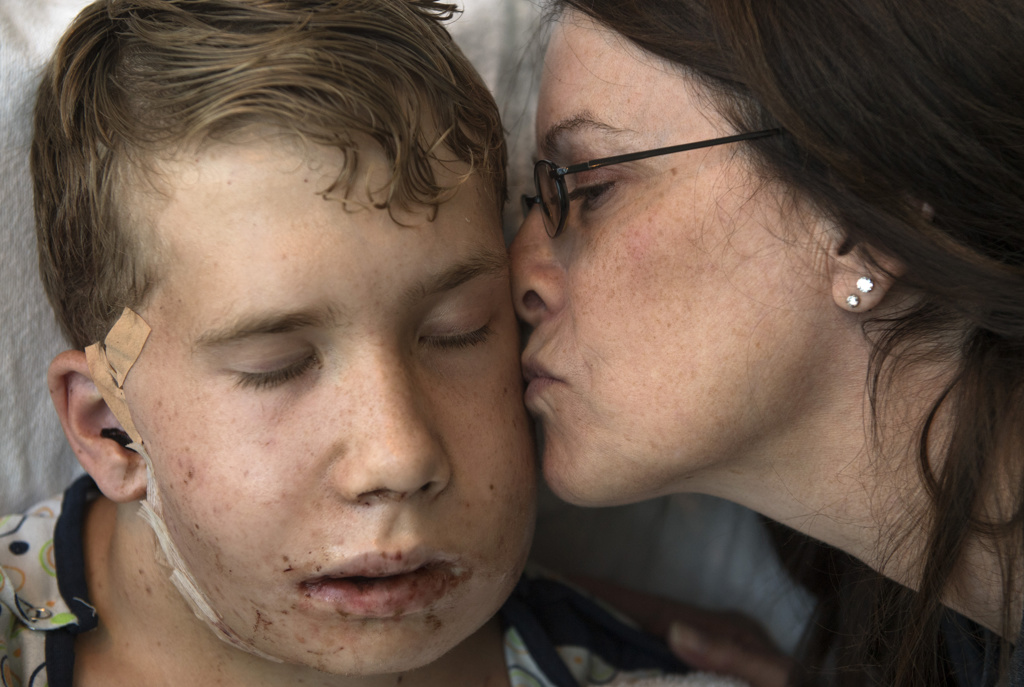
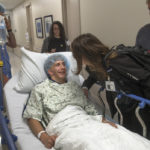
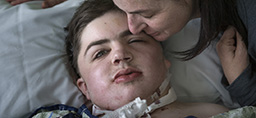
Six weeks after surgery, Wyatt sat at the edge of an exam table at the pediatric craniofacial clinic, wearing sneakers, a Nike sweatshirt and a big smile.
“I like how it turned out,” he said.
The surgery experience didn’t surprise him. It wasn’t easy, but he has undergone many other operations.
What proved most difficult? The aftermath—living three weeks with his jaws wired shut.
At home he hung out with friends, but it became difficult to socialize because he could barely talk. He spent a lot of time fishing.
And the liquid diet became tiresome.
“We made every kind of pureed food you can imagine,” Joe said.
His overall assessment: “It was definitely harder than I thought it was going to be, but I thought it was worth it. I really like the outcome.”
Once the wires on his jaw were removed, he began to eat more, sticking with soft foods. He went back to his job at Subway restaurant. And he began to prepare for his move to college.
Dr. Polley examined Wyatt’s jaw, told him to give a big smile, to open wide and bite down.
“You look dynamite,” he said.
As healing continues, he predicted the results will look even better.
“It takes time for these things to settle down,” he said.
Later, he may do a follow-up surgery adding to and centering Wyatt’s chin.
In addition to the cosmetic changes, Dr. Polley said the jaw operation opened up Wyatt’s nasal airway. And it will make it easier for him to eat.
He gave Wyatt jaw exercises to perform daily. And he told him he could start eating a greater variety of food, including meat, as long as he cuts it into small pieces.
Wyatt welcomed the news just as he prepared for his freshman year at college, where he has a 24-7 meal plan.
At Mount Mercy, he plans to study nursing. His experience in hospitals has taught him to appreciate the valuable role nurses play in in health care.
“They can help you heal faster and make you feel better,” he said.
His new look, with his new jaw, will make a difference in the years to come, he said.
“It’s going to give me more confidence to be more symmetrical,” he said.








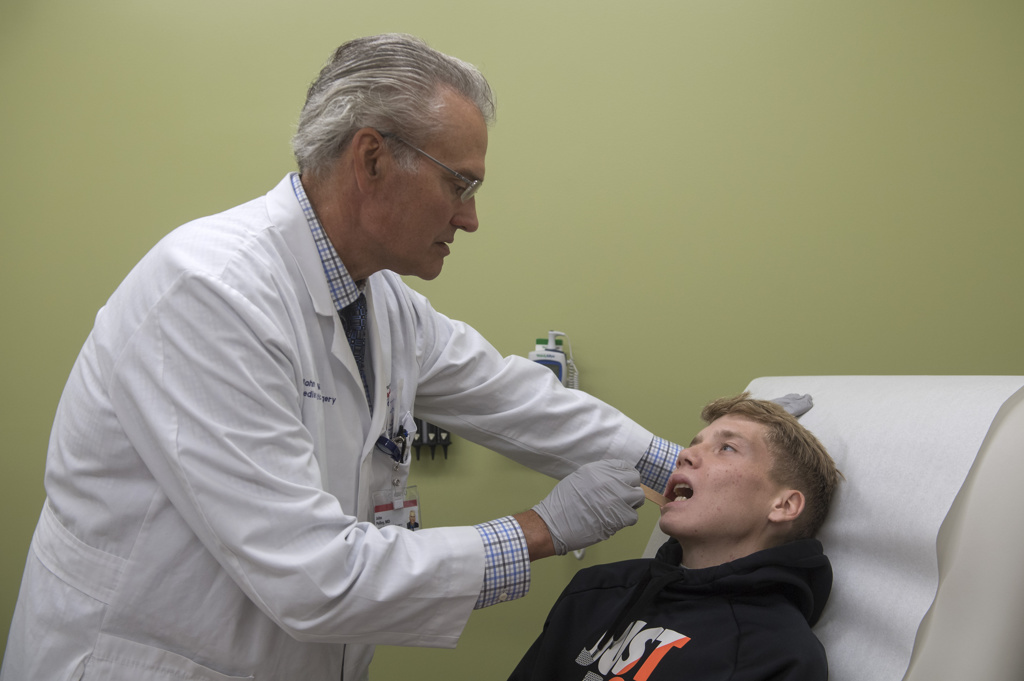


















 /a>
/a>
 /a>
/a>
 /a>
/a>
What a wonderful outcome and a “new” life for that young man. You work miracles!
He’s bright and talented young man — I’m sure good things lie ahead for him. Thanks for reading!
I’m so glad he decided to come to Grand Rapids.They will do a great job on his jaw.He will be happy with it.I have two
grandchildren working at Specetrum.
This article was so inspiring! It’s awesome what doctors can do now to change a life.
Wyatt sounds like a very special guy. I’m so happy for him and others that need these operations. I’m sure this article gives others hope.
God bless him and the doctors!
Awww, thank you so much for your kind message and comments, Sheila! We’re so glad Health Beat can be your daily dose of inspiration! Cheers, Cheryl
He is a great young man.
inspiring article