It’s Feb. 26, 2019.
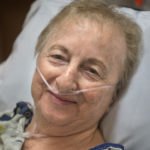
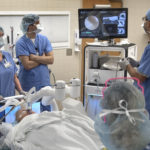
When the doors to Operating Room No. 28 at Spectrum Health Fred and Lena Meijer Heart Center open, Caroline Laney, 76, lies on the surgical table in the center of the room.
She’s in a deep sleep only anesthesia can render.
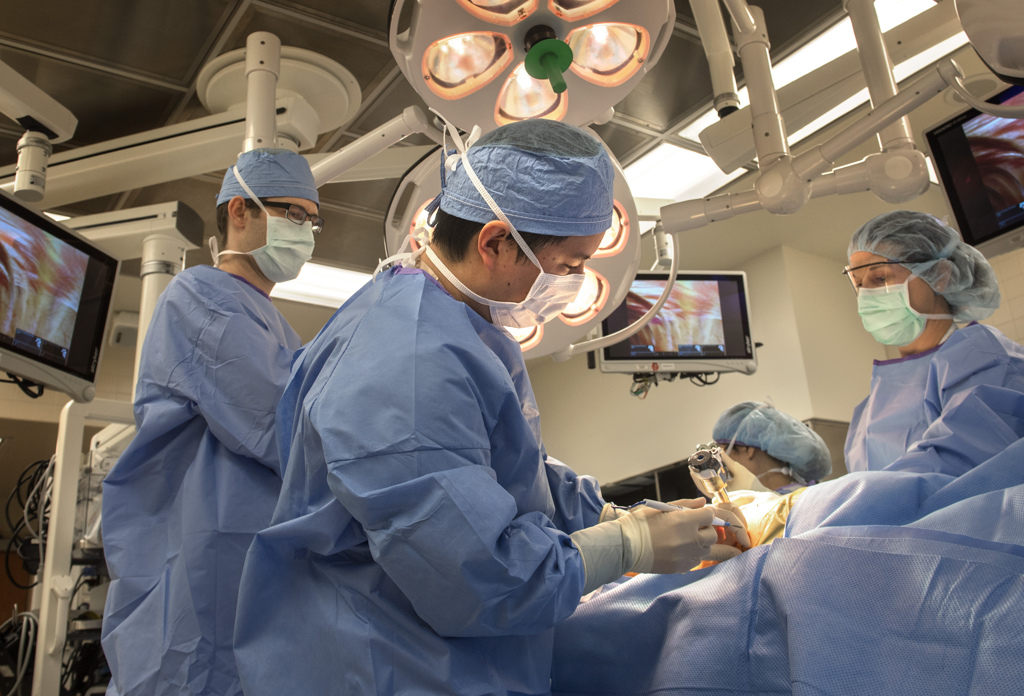
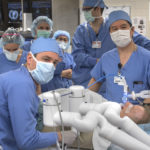
Surrounding her are several surgeons and her medical team. And two robots.
Well, not robots, per se. At least not the WALL-E or R2-D2 types.
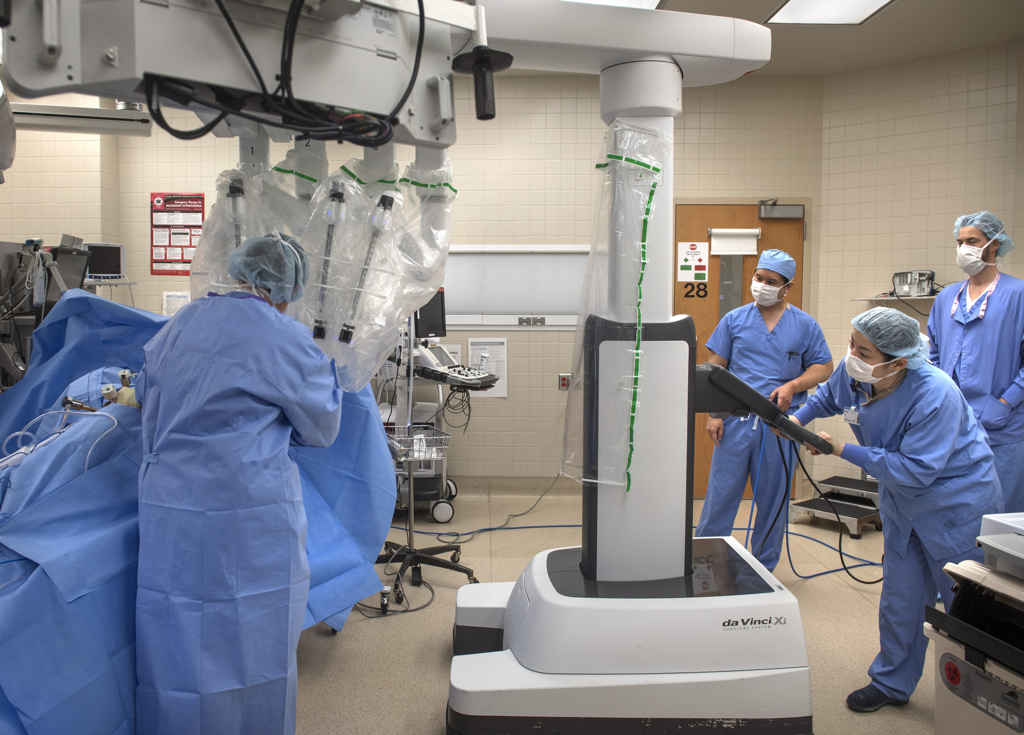
These immense machines are robotic surgical systems, more akin to human-assisted computerized machines. And they are among the most advanced systems of their kind in today’s operating rooms.
One is the Monarch Platform. The other is the da Vinci Xi Surgical System.
They—humans and machines—are all about to begin surgery on Laney to remove what may or may not be lung cancer.
If the mass the surgeons are about to remove is biopsied and sent to the lab—and the lab says it is indeed malignant—they will continue with the surgery to remove the entire mass, along with a lobe of Laney’s lung.
All without a surgeon ever touching the patient.
Robot hands
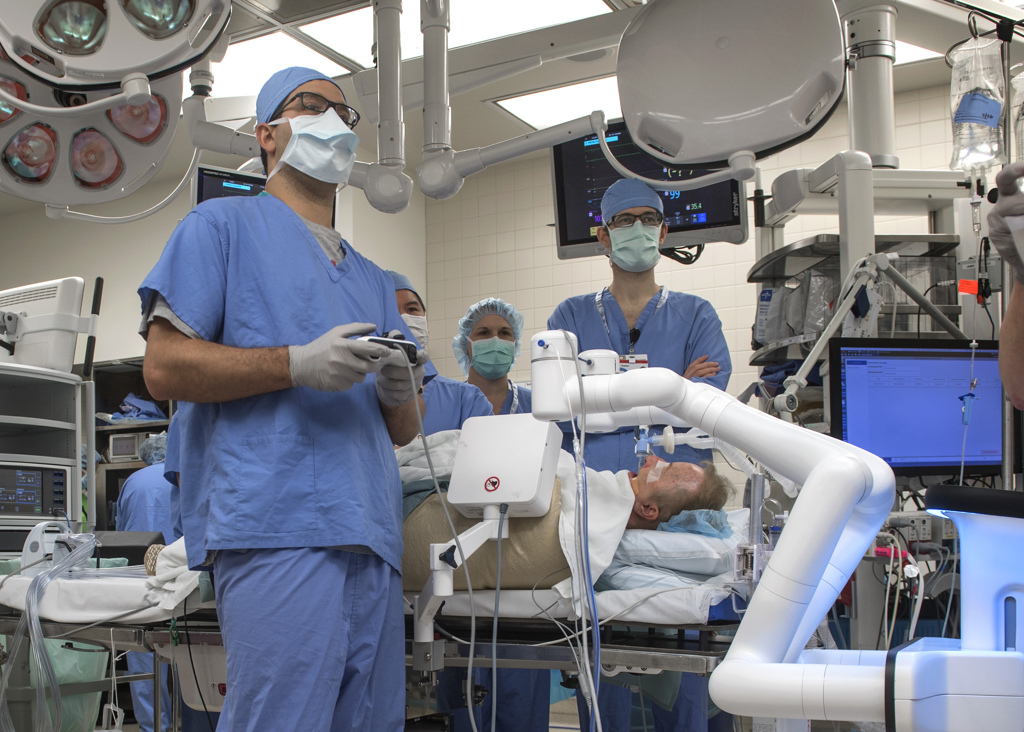
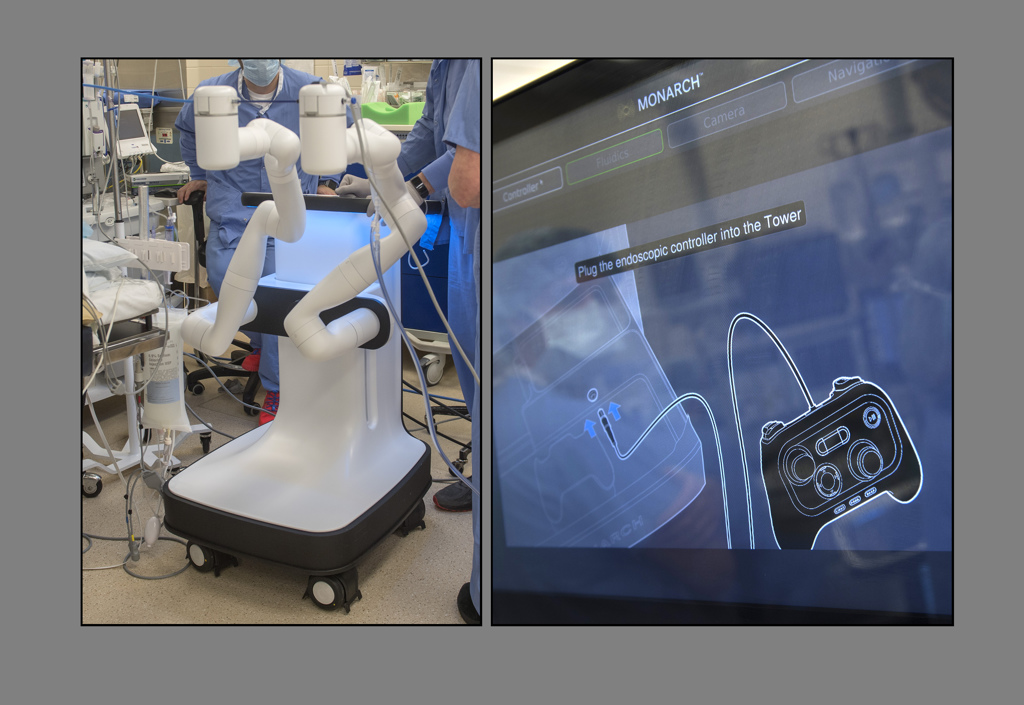
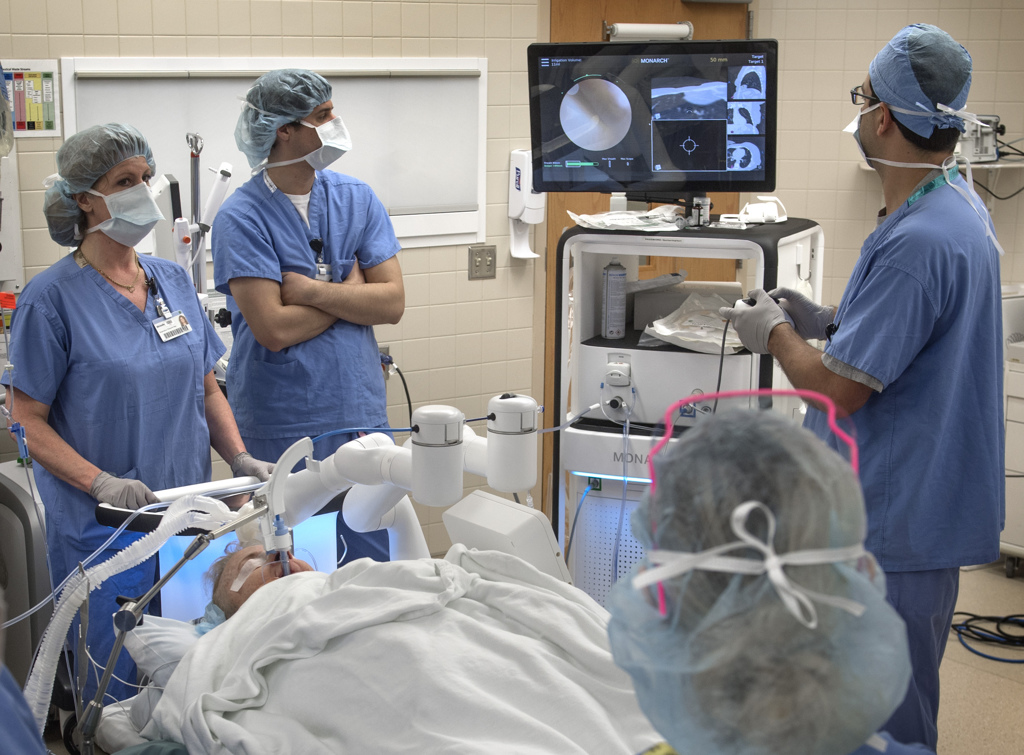
As surgery begins, Gustavo Cumbo-Nacheli, MD, an interventional pulmonologist and critical care medicine and pulmonary medicine physician at Spectrum Health, prepares to work with the Monarch Platform.
“This is the second such surgery done at Spectrum Health,” Dr. Cumbo says. “Caroline would have been the first, but we had to reschedule her surgery due to icy weather, so this is our second. We are fifth in the country to have this kind of technology available for our patients.”
The Monarch Platform is the newer of the two systems. It’s currently used for diagnostic and therapeutic bronchoscopic procedures, although future possibilities are limitless, Dr. Cumbo says.
Working alongside Dr. Cumbo is John Egan, MD. Dr. Egan has been performing navigational bronchoscopy since 2012.
He and Dr. Cumbo now often work together, and on this day, they are both on the Monarch Platform.
“The robotic component has been the biggest improvement I’ve seen in the technology at this time,” Dr. Egan says. “I think one day we will be able to diagnose, stage, and even cure early stage lung cancer in a single procedure. Before this is possible, we still have a lot to learn about the technology and more research needs to be done, but now, more than ever, there is hope for people with this form of cancer.”
Above his surgical mask, Dr. Cumbo’s eyes are alight. It’s clear he’s excited to work with this new technology.
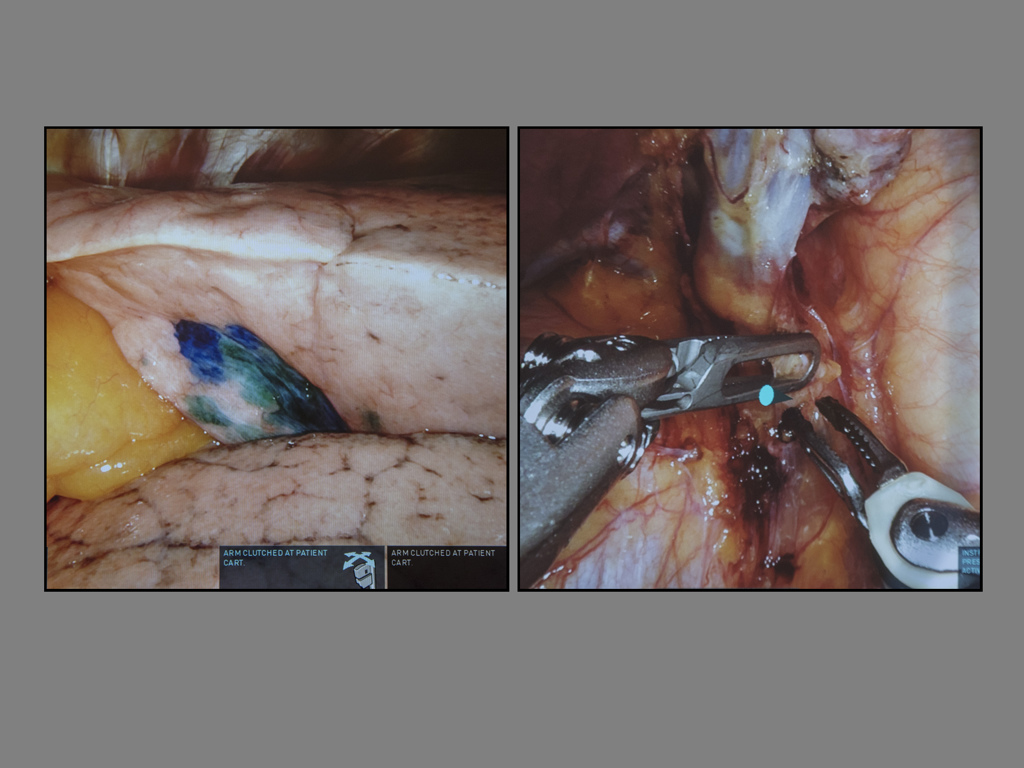
“Robotic surgery allows us to get to areas we couldn’t reach before,” Dr. Cumbo says. “The Monarch will be used to tattoo the area of concern with a dye where the next surgeon needs to operate using the da Vinci. I’m the marksman, he’s the shooter.”
The cardiothoracic surgeon who operates the da Vinci that Dr. Cumbo called the shooter is Geoffrey Lam, MD. Dr. Lam has logged about 100 robotic surgeries in the past year at Spectrum Health.
“Robotic surgery is very different than using our hands,” Dr. Lam says. “We are able to avoid making a larger incision on the patient. And that means less pain and faster recovery.”
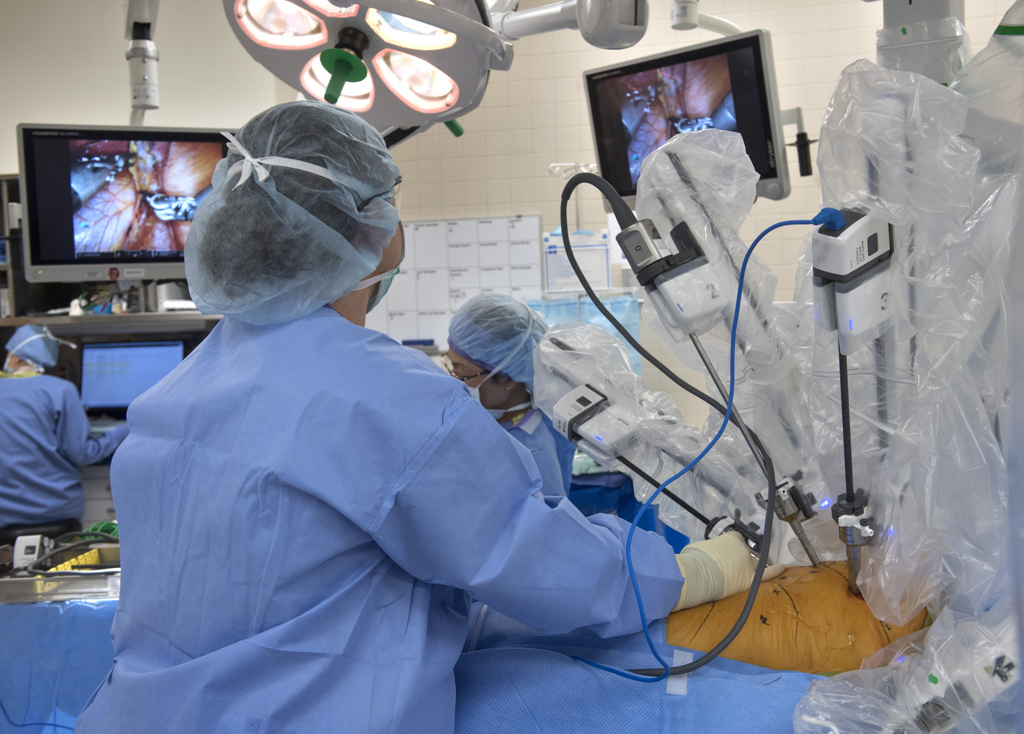
The da Vinci system lets everyone in the operating room see the procedure with improved clarity. It displays magnified 3D images onto multiple screens visible to surgeons and the medical team.
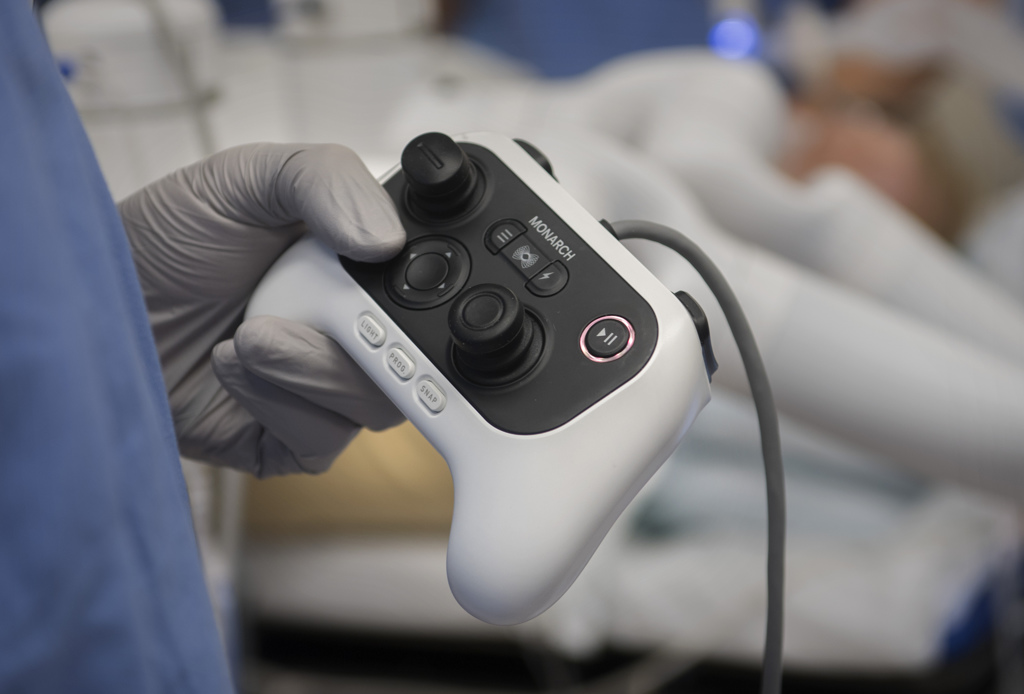
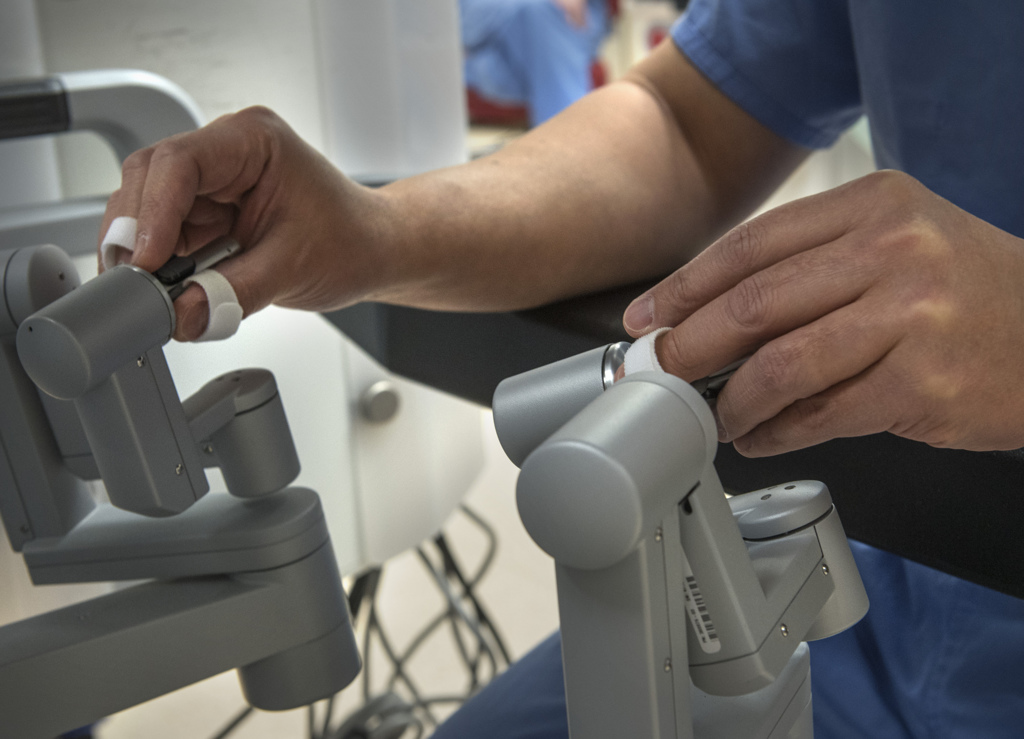
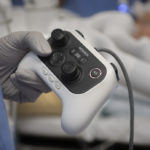
The surgeon controls tiny instruments at the end of the robotic arms, much like a gaming system. The implements can bend and rotate with more dexterity than a human hand, even as the surgeon controls every movement from the console.
Explains Dr. Lam: “This combined robotic procedure—the Monarch robotic bronchoscopy system, along with the da Vinci Xi robot—is used to localize lung nodules that are suspicious for cancer.
“Dye marking, followed by wedge resection, allows for a minimally invasive approach to make a diagnosis, then proceed with the appropriate surgical treatment based on that information—all done in one operation, without the morbidity, pain and discomfort of a larger incision.”
And so it begins.
Moment of truth
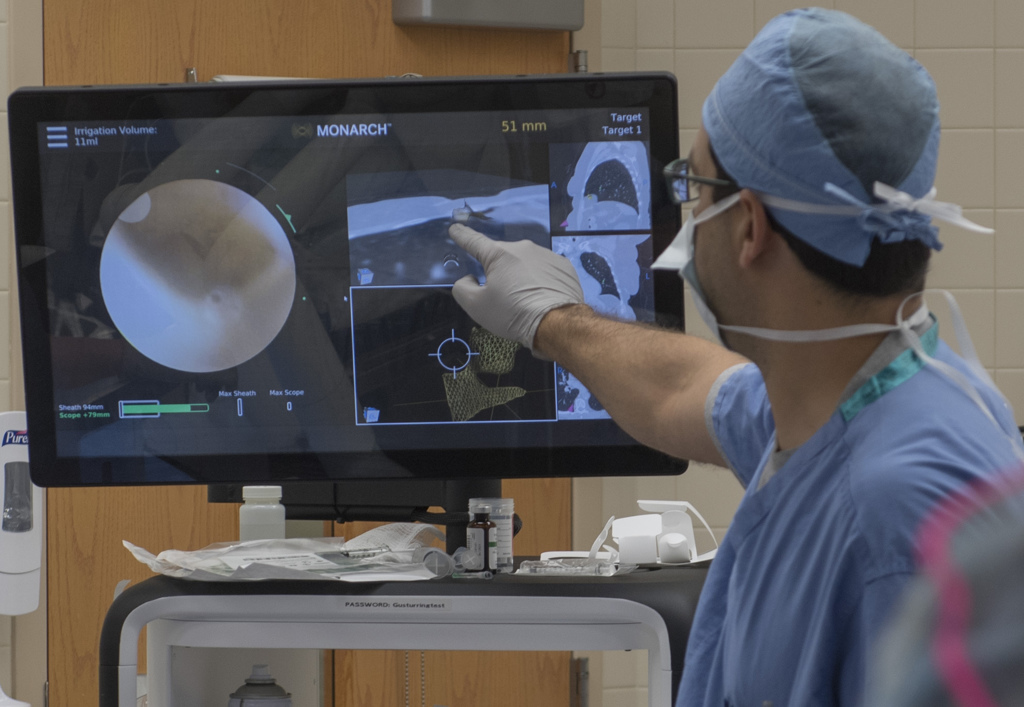
Dr. Cumbo steps in as his team pulls the Monarch Platform closer to the patient. An image appears on a screen as a tiny camera—a flexible robotic endoscope—moves past the patient’s trachea through Laney’s lungs, targeting the mass for removal.
“Ready? Ok, let’s do it, here we go,” he says.
More images appear, each in great detail showing parts of Laney’s affected lung.
Dr. Cumbo locates the precise area and releases a dye to mark it.
Done.
By precisely marking the target, the surgeon reduces the risk of partially resected or false negative results, as well as minimizing the possibility of damage to the lung during surgery.
Then it’s Dr. Lam’s turn. He uses the da Vinci.
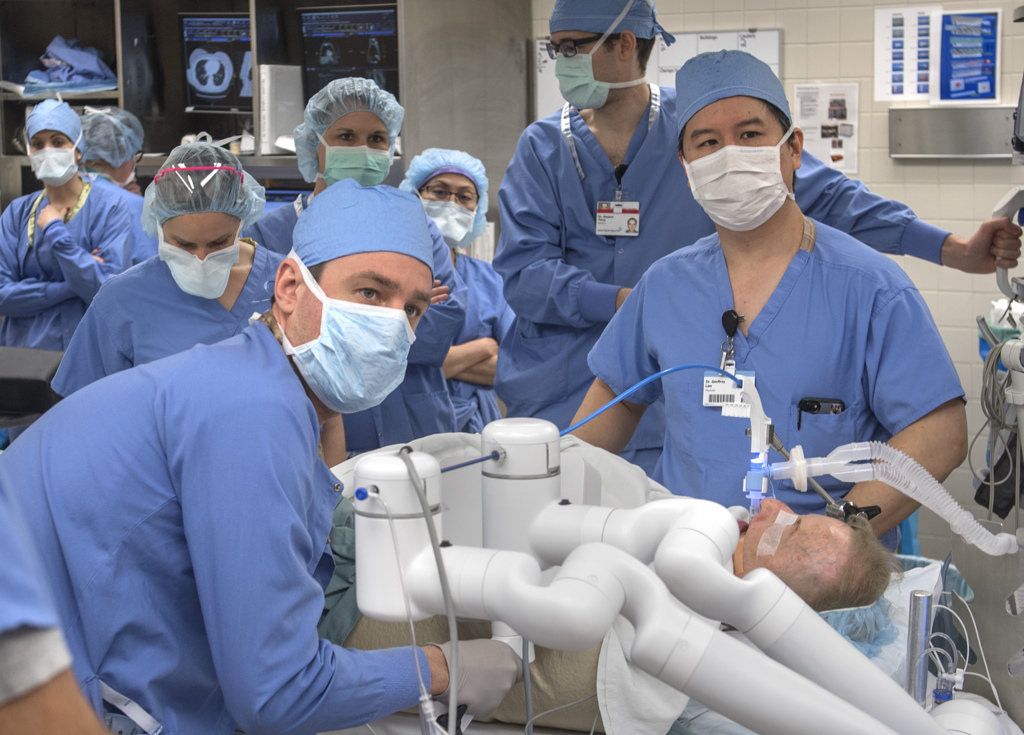
More images appear, encircling the operating table. Dr. Lam sits at a console at the foot of the table. His hands are inserted into a wrist instrument that controls corresponding instruments used on the patient.
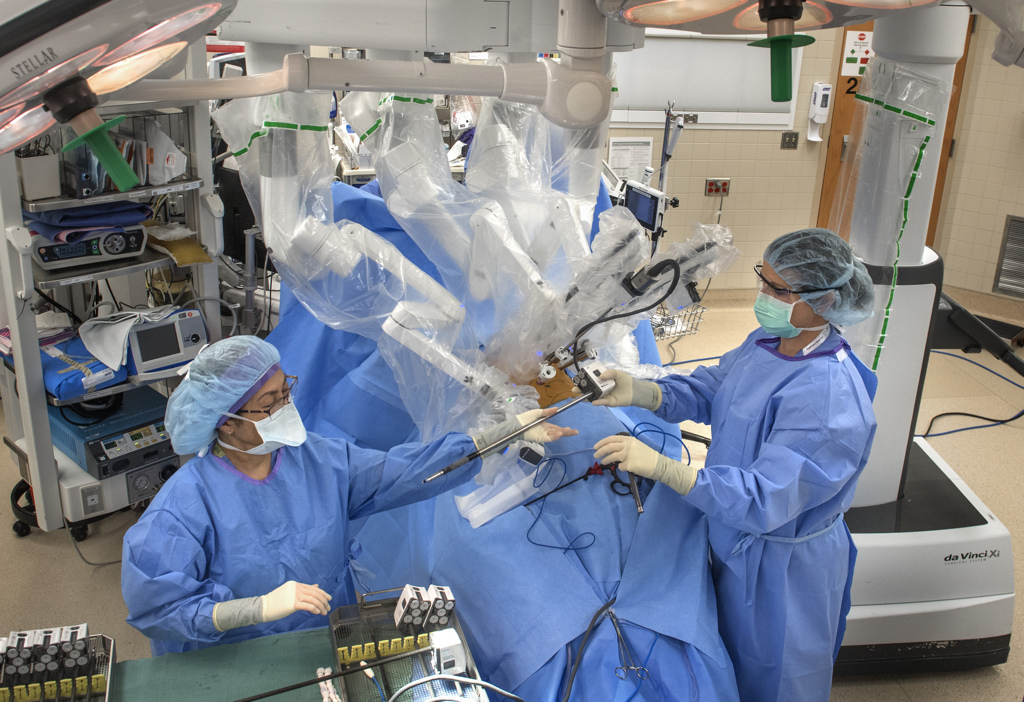
The medical team lowers over the operating table another part of the machine—a circle of robotic arms that can rotate and pivot into most any position.
Dr. Lam’s assistants attach instruments to each arm.
The operation begins.
Dr. Lam’s eyes focus on the screen in front of him. He manipulates the tiny instruments through Laney’s affected lung. His feet press on pedals underneath the console, directing the robotic movements. He seeks out the tattooed area and finds it.
A tiny snip extracts a piece of the mass, which is quickly sent off to the lab.
They wait for the phone to ring.
‘Minimize disruption’
News from the lab: the mass is indeed malignant.
It’s only been a matter of minutes but the team is prepared to proceed with surgery to remove the targeted mass and the affected lobe.
The entire operation takes approximately two hours.
They remove all of Laney’s cancer.
As the robotic surgical systems are wheeled away, Laney is taken into recovery with only a few small incisions in her upper body.
Dr. Lam says the new technology enables doctors to provide patients with the highest quality, evidence-based treatment.
“If we can reduce the normal pain and discomfort associated with traditional larger incisions into the chest cavity, then patients will have more rapid recovery and return to their normal daily routine,” Dr. Lam says. “And that’s the point—minimize disruption to the patient and their family, get them through surgery and then have them continue on with their lives.”
The team has removed Laney’s cancer without affecting the lymph nodes, so she’ll require no further treatment other than follow-up appointments with her physician to monitor healing.
‘I chose surgery’
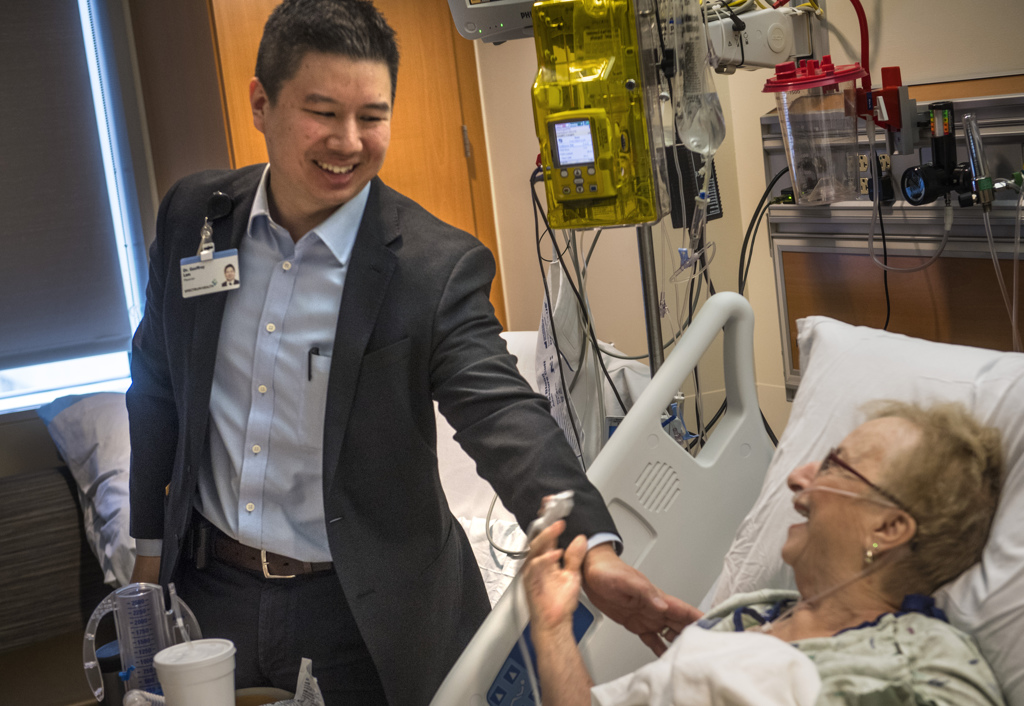
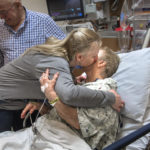
Outside the operating room is Laney’s husband, Doug, and her daughter, Denise, one of five siblings. They smile bright and wide when they hear the surgery has been successful.
“We weren’t nervous at all,” Denise says. “We had total confidence in her doctors.”
After five days in the hospital, Laney is ready to talk about her experience. She exudes her family’s confidence and positive attitude.
“This all began in September 2018,” she says. “I was having upper respiratory issues, although I have struggled with allergies and asthma since the 1950s. I’d had allergy shots for 10 years, used an inhaler, but this felt different, so I went in to see my doctor, who recommended a pulmonologist.”
Her physicians ordered a CT scan and then a PET scan on her lungs. This revealed the mass in her upper left lung.
“I’ve been through this before,” Laney says. “I’m a breast cancer survivor from 2001. I was a smoker but I quit in 1994. Dr. Lam told me I could wait and see if the mass grows or I could choose surgery. I chose surgery.”
She says there has been minimal pain during the recovery.
She does breathing exercises every few hours, critical steps in regaining lung capacity.
“Every day is a little better,” she says. “What I want others to know about my experience is that you need to communicate with your doctor. Tell them how you feel. That’s why my lung cancer was caught early.”
But she’s also quick to credit her doctors—and their robots.



















 /a>
/a>
 /a>
/a>
 /a>
/a>
Dr. Lam performed the same robotic lung cancer surgery on me in June of 2018. All of the cancer was removed, requiring no follow-up treatment. I was able to go on a family vacation that summer! We are blessed to have Dr. Lam, his colleagues and this technology here!