Luke Anhalt can’t tell you how many times he has played basketball.
In his 17 years, he has taken countless shots, run up and down the court, dribbled and passed the ball, legs pumping, heart pounding, sweat dripping.
He took it all for granted.
He loved it, of course. Worked hard at it. But he didn’t fully grasp what it meant until the day his heart stopped. He hit the floor, essentially lifeless, in cardiac arrest.
Call his survival a miracle or a product of modern medicine, or a combination of both. To Luke, it was also a moment of realization.
“Every time you step on the court is a gift,” he said. “Every time you step off is a gift, too.”
Quick action by teammates and Luke’s coach made all the difference for Luke when his heart stopped, said Christopher Ratnasamy, MD, a pediatric cardiologist specializing in electrophysiology at Spectrum Health Helen DeVos Children’s Hospital.
“They did it by the book. They did everything perfectly,” Dr. Ratnasamy said.
‘In tip-top shape’
Luke, a senior at Calvary Christian High School in Fruitport, Michigan, suffered the cardiac arrest during basketball practice on Dec. 13, 2018.
At first, he had no recollection of the entire day. But eventually, he came to remember eating breakfast that morning. At school, he got ready for tests.
“We had chapel that day,” he said. “I remember getting ready for (basketball) practice but that’s it. There is this hole.”
Friends and family members have filled in the details. During a free-throw drill, Luke suddenly dropped to the ground. A friend looked at him, realized this was no ordinary injury, and called to Coach Jeff Zehr.
As Zehr tended to him, his son Zach—Luke’s best friend—ran for the gym’s automated electronic defibrillator.
Following the AED instructions, the coach performed chest compressions. Then he shocked Luke’s heart. He resumed compressions and placed the AED on Luke’s chest again. It signaled the need for a second shock. At that point, the first responders arrived and took over.
Dr. Ratnasamy praised the coach for his handling of the crisis, particularly for checking to see if the heart went back into arrhythmia.
“It was a miraculous survival to have two shocks,” Dr. Ratnasamy said. “It was a really good save.”
Luke’s heart began to beat and he had a steady pulse by the time they wheeled him to the ambulance.
His parents, Samantha and Jeff Anhalt, were notified and word spread through the school.
When Samantha arrived, she found her two younger children, 14-year-old Cate and 12-year-old Will, in a cluster of students gathered outside the gym, heads bowed in prayer.
Luke went first to a local hospital and then transferred to Helen DeVos Children’s Hospital that evening.
By Saturday, he became more aware of his surroundings. He asked his family repeatedly how he ended up in the hospital. Told about the cardiac arrest, he laughed and shook his head.
“My heart is superb,” he said. “I’m in tip-top shape.”
An MRI, CT scan, echocardiogram and multiple EKGs showed no damage to the heart muscle. His heart function had returned to normal.
The tests also did not reveal why Luke’s heart suddenly stopped on the court.
Four days after the cardiac arrest, Luke underwent surgery to get an implanted cardiac defibrillator, which will shock his heart if he suffers a repeat episode.
“The defibrillator is like a guardian angel to protect him if he ever goes into arrhythmia,” Dr. Ratnasamy said.
The device sits beneath the skin on the left side of his back. It protrudes a bit, a physical reminder of what he endured.
“I’m getting used to it. It’s my old friend now,” Luke said. “It’s good to know if something ever does go funky with the heart rate, it will recognize it and will shock it back to where it’s supposed to be.”
A new view on life
Luke recovered from the cardiac arrest and surgery over Christmas vacation.
Sitting at the kitchen table of the Anhalts’ Spring Lake home, he talked about the most difficult part of recovery: being sedentary. A competitive soccer and basketball player, rest and relaxation did not come easily for Luke.
He spoke with admiration for his coach’s cool head and quick action.
“He did great CPR,” Luke said. “I am definitely grateful for that.”
Next fall, he plans to attend Spring Arbor University as a pre-med student. But he may rethink his plan to follow in his father’s footsteps as an orthopedic surgeon.
“That might change based on recent events,” he said. “The cardiology side might be a little more interesting.”
His experience also gave him a new perspective on sports—and a deeper appreciation for what it means to be a good sport.
“I don’t like to lose. That won’t ever go away,” he said. “I still want to compete and I still want to win. But I think the sportsmanship will be a little different.”
Of those who suffer a cardiac arrest outside of a hospital, about 90 percent die, according to the American Heart Association.
But in Michigan, Dr. Ratnasamy believes the odds of survival are increasing, particularly among young people, because of community awareness campaigns. A statewide push to provide schools with AEDs and training in cardiopulmonary resuscitation has been lifesaving for students like Luke.
“The odds of survival depend on effective CPR and the availability of AEDs,” Dr. Ratnasamy said. “The biggest thing is the AED. They got it quickly and effectively did CPR.”
‘God is here’
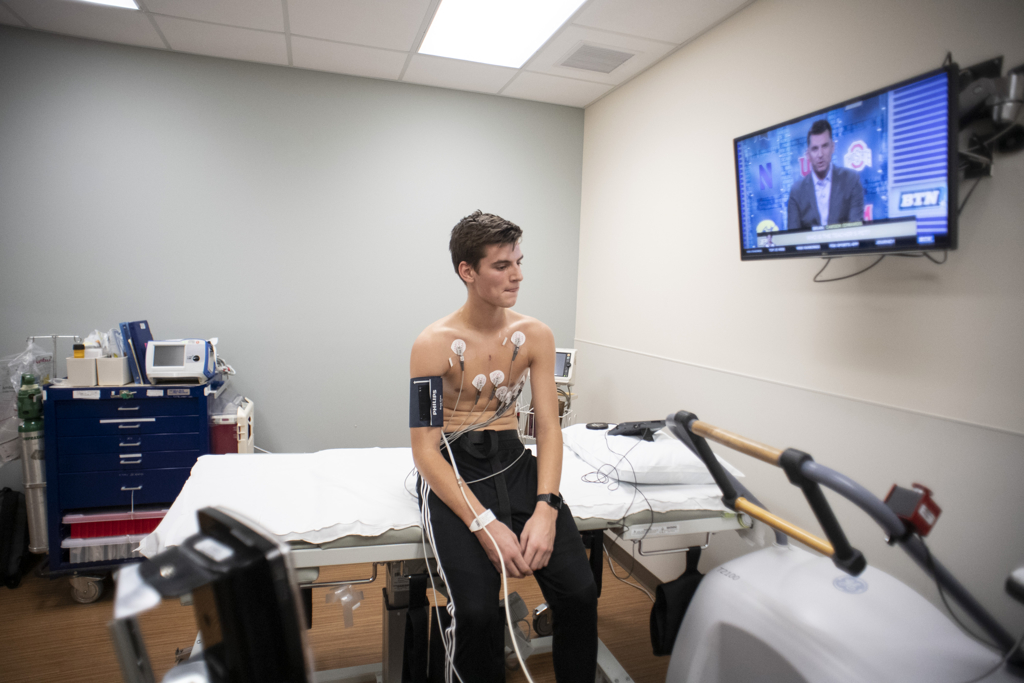
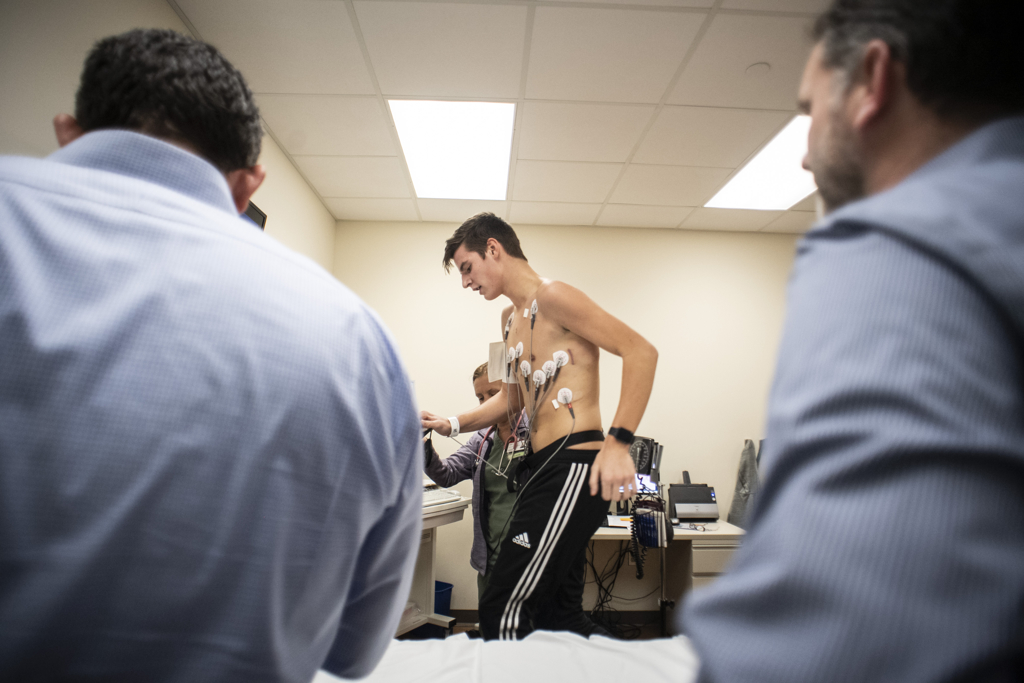
Six weeks after the cardiac arrest, Luke returned to the Congenital Heart Center at Helen DeVos Children’s Hospital for a stress test and follow-up visit.
He ran on a treadmill for 13 minutes, with Dr. Ratnasamy and exercise specialist Laura Zochowski monitoring his heart rate and blood pressure.
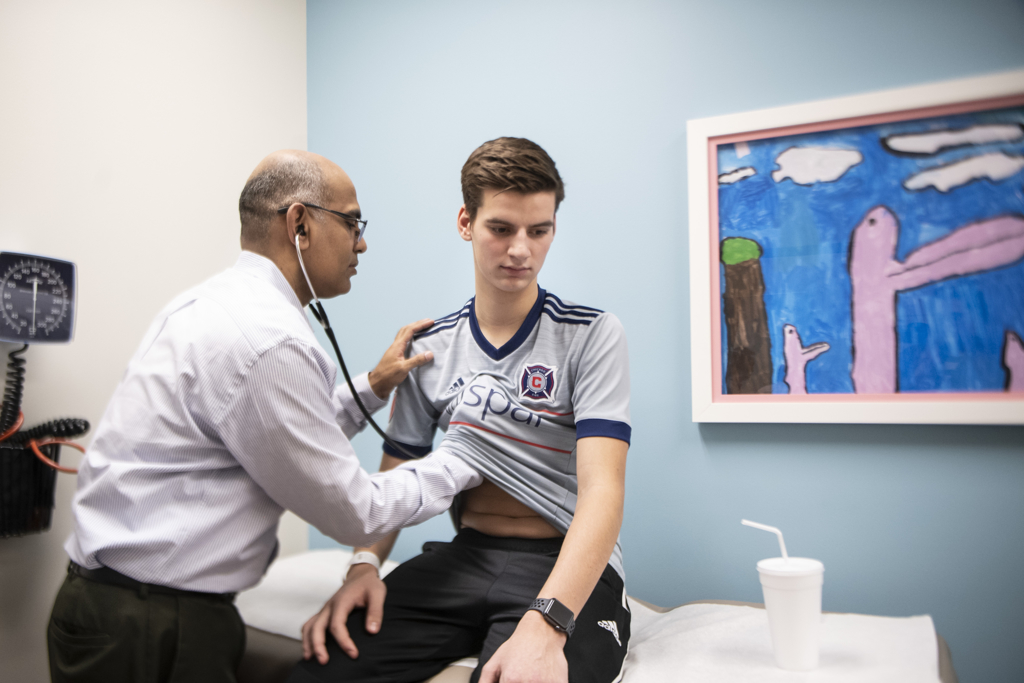
When Luke sat down on the exam table, catching his breath, Dr. Ratnasamy asked if he felt any pain or discomfort.
“Just my legs,” Luke said. “It’s been a long time. It feels good to sweat and be running.”
The stress test showed no arrhythmia, Dr. Ratnasamy said. He will continue to monitor Luke. Research into arrhythmia may someday reveal the cause of his sudden cardiac arrest.
Dr. Ratnasamy said Luke could resume physical activities, though he should give himself time to get back in shape and also keep his heart rate under 180.
The weekend after his stress test, Luke celebrated key milestones of his high school years. He played in the homecoming basketball game, with dad in the stands monitoring his heart rate. He was crowned homecoming king—elected in a vote held before his cardiac arrest.
Looking ahead, he said he doesn’t worry much about another cardiac arrest. He hopes it never happens again but, if it does he’s reassured to know he has a cardiac defibrillator implanted.
He wonders more about what he will do with this new chance at life.
“It’s been important to see that now, since I have this second opportunity, that I’m here for a reason,” he said. “God is here and he is watching. He didn’t just spin the world and walk away. He is still involved and his hands are still working.”
What that will mean in the future, he is not sure. He plans to leave that up to God.
“Honestly, I don’t know,” he said. “I’m just hoping he keeps directing me in that. Whatever I’m going to do I’m just going to do with a whole heart and all for his glory.”





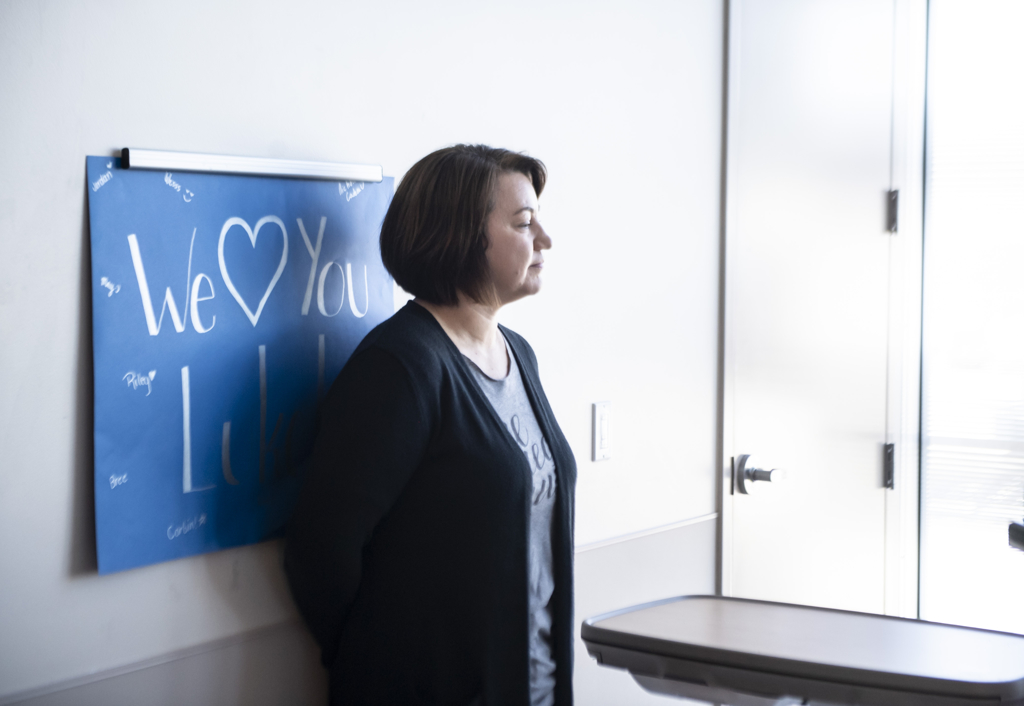









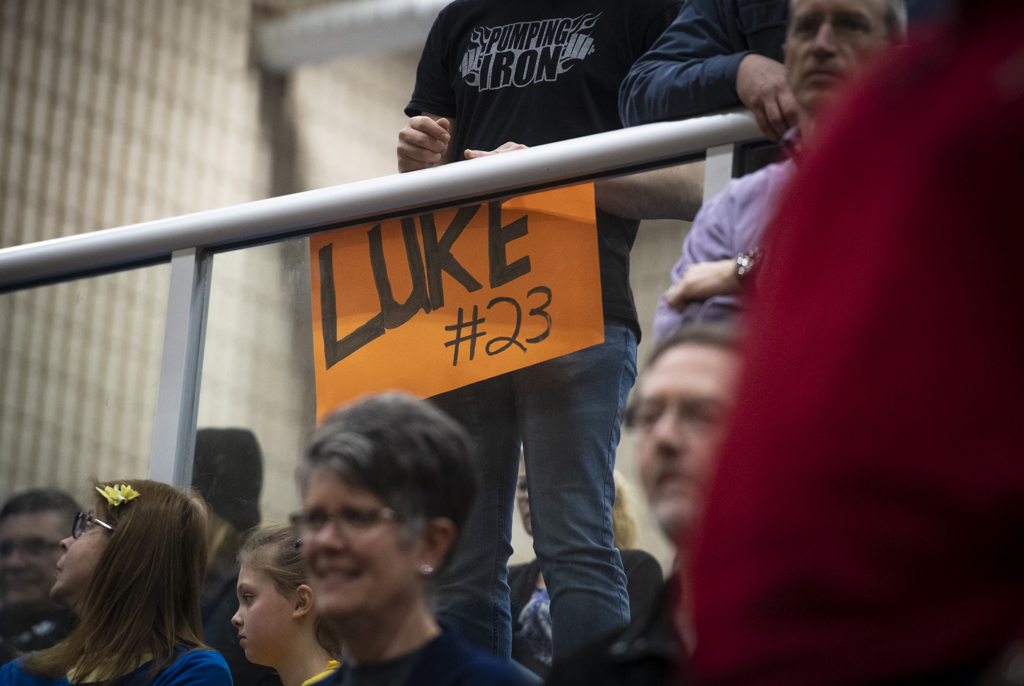






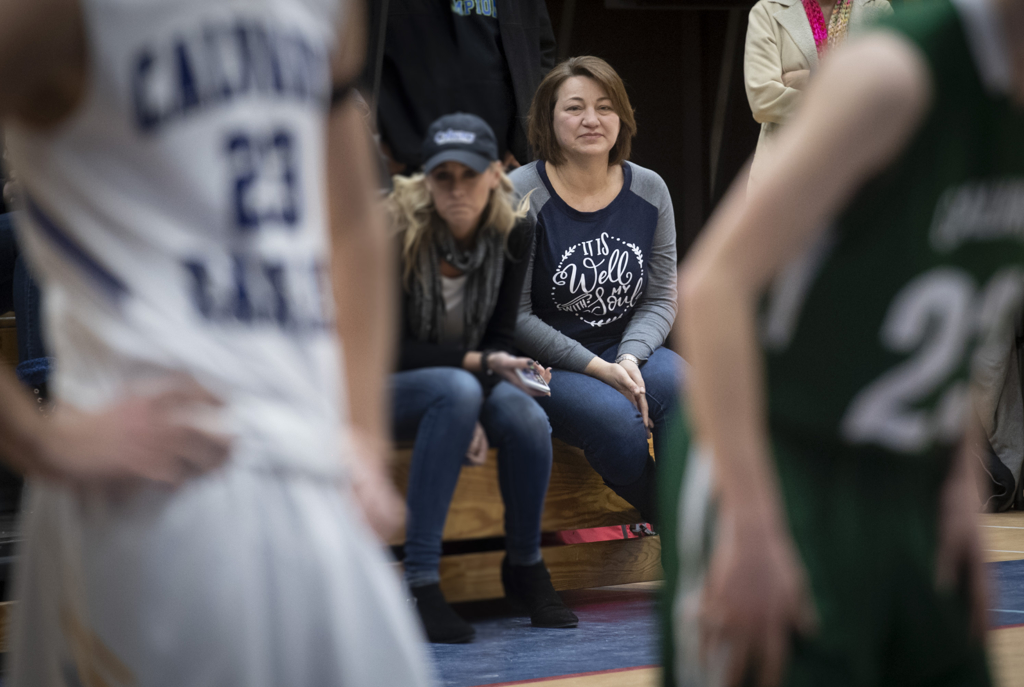










































 /a>
/a>
 /a>
/a>
 /a>
/a>
Wow! What a remarkable young man! Love his story and his heart for God.
Agreed. I was so impressed by his insights and positive attitude. Thanks for reading!
This is good news about a great young man.
Thank you Lord! Wonderful story.
Amen❣
I love your attitude on life and your love for God! Keep up that attitude young man and you will do well no matter what field of medicine you choose.
What an awesome young man! Thanks for sharing your story!
Thanks to Spectrum Health and the author of this article for the excellent job in reporting this story.
Great story. Thanks for sharing. I always tell my kids this,” there are no guarantees in life.” Be thankful each day you are living.
Absolutely, Brian! Life is good. 🙂
I would like to talk with this young Man. I have a similar situation.
Great story of care, determination and faith. Makes one proud to be a part of the Spectrum Health family.
Thank you for your fantastic comment, Scott!
…”Whatever I’m going to do I’m just going to do with a whole heart and all for his glory.”
This kid has it all figured out at his young age.
Wonderful story!
God is here! But, just in case, I have my defibrillator. 🤥🤫