Long before anyone ever heard of COVID-19, Lois Stanton Van Dahm knew more than most people about global pandemics.
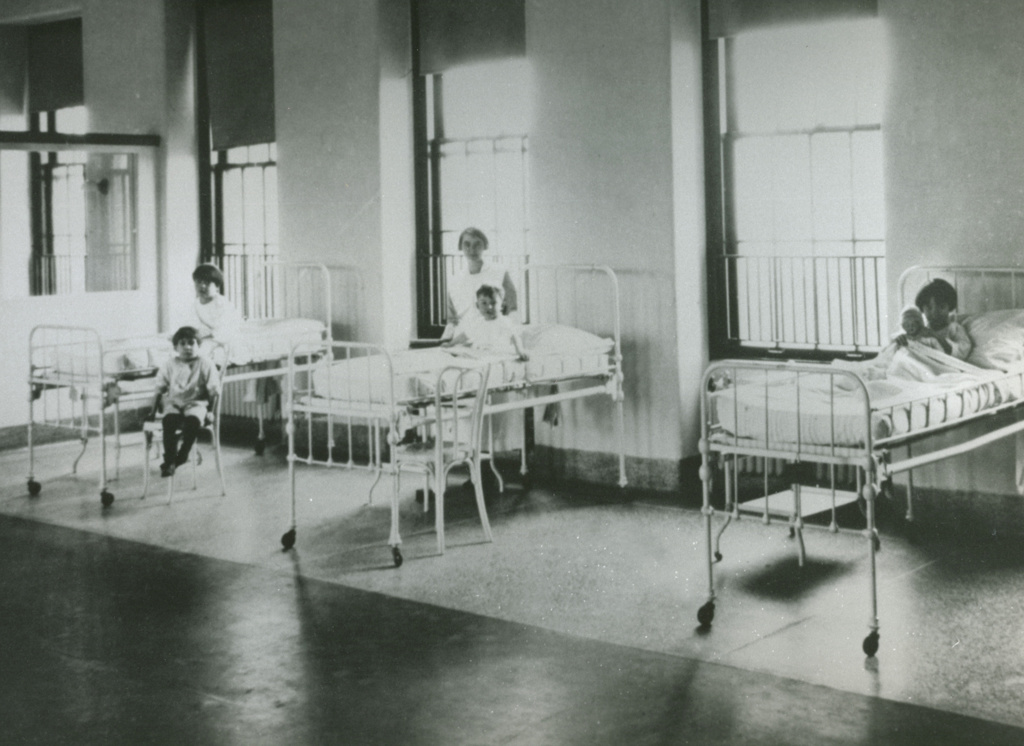
After finishing her nurse’s training in Grand Rapids, Michigan, in 1947, she worked on the polio ward at what is now Spectrum Health Blodgett Hospital, watching patients struggle with paralysis, respiratory failure and worse.
“One little boy particularly stands out,” she said. “It was at the end of my day, and this child—I remember he was a twin and his family had been on a camping trip when he got sick—came in.”
Van Dahm, who was born in Allendale, can still recall his face all these years later. “There was just something about him that touched my heart right away,” she said.
“I went straight to his room when I came back on duty the next morning, and he had died overnight,” she recalled. “Polio didn’t discriminate. And it could kill people so quickly.”
Parallels between the pandemics
Now 93, she can’t help drawing parallels between polio, the virus that shaped her early career, and the COVID-19 pandemic that currently keeps her and Tom, her husband of 69 years, self-isolating in their Kenosha, Wisconsin, condominium.
Polio was once one of the most feared diseases in the U.S., but it was no stranger. It had been around for decades before Van Dahm entered nursing and was believed to have caused the paralysis that Franklin Delano Roosevelt developed in 1921.
In the late 1940s, just as she began her career, the Centers for Disease Control and Prevention saw polio outbreaks swell to epidemic levels.
Most people who contracted the highly contagious disease had no symptoms. About one in four people developed flu-like symptoms that went away on their own, usually in just a few days.
But in the worst cases, polio caused paralysis. Two out of 10 of those with paralysis died, usually because it affected the muscles required for breathing.
Polio peaked in 1952, with 58,000 reported cases in the U.S. that year, which resulted in 21,000 cases of paralysis and 3,000 deaths. It terrified parents, who often kept kids home and inside during the summer months, frightened their children would catch it.
Authorities tried to protect people by closing sources of transmission.
“Justifiably, they shut down beaches and pools and public areas,” Van Dahm said, “because that’s how the disease was being spread. And in Michigan, with all its lakes, that was hard.”
Public health officials also sometimes imposed quarantines, restricted travel and commerce in efforts to isolate affected areas.
As is true with COVID-19, there was no cure.
“We tried to make patients comfortable,” she said, “but the standard of care was the Sister Kenny treatment.” That involved hot packs, muscle stretching and massages.
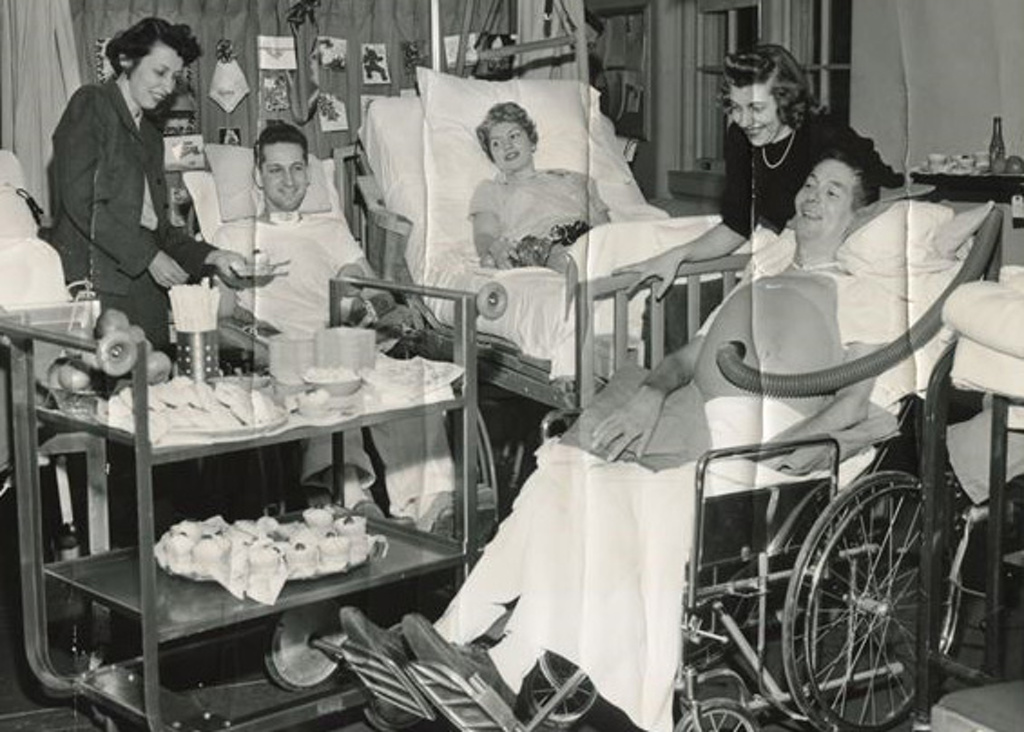
Long recoveries became common, often involving respirators and breathing devices called iron lungs. That gave nurses like Van Dahm time to form genuine friendships as they got to know patients.
“I even corresponded with one young man for decades,” she said. “We tried hard to make life as normal as possible, propping up books so they could read and helping them keep up with schoolwork while they tried to get better.”
And the bonds she formed with other nurses also lasted. She graduated from Grand Rapids Junior College. The curriculum involved training at Butterworth, St. Mary’s and Blodgett hospitals.
The young nurses “felt the pressure to prove to those around us that we were well-trained and necessary. We were prepared not just for hospital work, but to care for people in their homes, too. We gave baths and backrubs. We learned to make beds with very neat corners.”
Even at the height of polio outbreaks, “we knew scientists around the world were working feverishly to develop a vaccine.”
What polio can teach us
The story of how America defeated polio offers plenty of insights that can make slogging through the COVID-19 era a little easier, said Russell Lampen, DO, an infectious disease specialist at Spectrum Health. Among the lessons are faith in science and persistence.
“People are understandably frustrated by restrictions related to COVID-19,” he said. “But it’s only been going on for months. Polio existed for a long time—for years.”
While massive polio vaccine trials began in the U.S. in 1954, progress didn’t move in a straight line. It wasn’t until the 1960s that the oral vaccine, developed by Albert Sabin and tested widely in what was then the Soviet Union, became the standard in America. It replaced Jonas Salk’s earlier 1955 vaccine.
Dr. Lampen said there are five different kinds of vaccines and many possible variations.
“It’s important to understand that the first vaccines for COVID-19 may not be perfect, and there will likely be follow-up vaccines developed,” he said.
He points to the vaccination for shingles, commonly given to adults older than 50, as an example.
“The first shingles vaccine was 50% effective,” he said. “Now, it is 90%.”
The recent news from the scientific community about potential COVID-19 vaccines with an up to 95% effective rate, and no known health risks, has largely been received as a blessing of modern medicine. The conversation has turned to how to safely and effectively vaccinate a large enough percentage of the population, and determining how long the immunity will last.
Dr. Lampen said the most important lesson to take from America’s polio history is optimism.
Thanks to vaccination, polio has been virtually eliminated from the Western hemisphere. The U.S. hasn’t had a single case originating here since 1979.
“The COVID-19 virus won’t disappear,” he said. “But through vaccination, we can win.”
When Salk discovered the first polio vaccine, he quickly became one of the world’s most admired scientists.
Today, many people openly–and frequently–disparage vaccinations.
“There was a very different national attitude toward science back then,” Dr. Lampen said.
Polio could (and did) strike people of all ages.
“But because it harmed children the most, it was somehow easier for people to rally around fighting it,” he said. “COVID-19, conversely, occurs more in older people—and I do think that complicates the picture. If COVID-19 impacted kids, it’s possible people would react differently.”







 /a>
/a>
 /a>
/a>
 /a>
/a>
Very scary times.
Very informative and interesting article.
Thank you, Gwen, for your kind words and for being a Health Beat reader. We’re glad this article proved interesting and useful for you. Best, Cheryl
Thank you so much for the article. My mother is pictured in the last picture in the polio ward at Blodgett Hospital. She contracted polio in 1954 as a 30 year old young mother.
Thank you for sharing, Kathy. Your mother was absolutely beautiful in this photo. Was your mother able to recover from it?
She was left with multiple deficits, but was able, after many years of physical therapy, to live a very independent life. She was quite the woman! Thanks for asking, Cheryl.
So glad to hear this. Thank you, Kathy!
Very interesting read and I am happy that your mother has done well. My favorite aunt had polio too,and after a very long,long time of being sick and near death. She finally recovered and is doing well.
I’m so glad your aunt eventually recovered, Deborah. Thank you for sharing!
Very interesting article. My aunt Marjorie Cooper lived in an iron lung for 40 years after contracting polio. She got sick in 1945 and died in 1985. She was in Blodgett Hospital for two years until my uncle John took her home and cared for her the rest of her life.