Tabitha Wolters, 44, harbored no worries when she went in for her annual mammogram just before the holidays.
She hadn’t felt any lumps. She had no family history.
Even when she learned she had some calcifications and needed a biopsy, she never felt nervous.
“Believe it or not, I wasn’t even that concerned when they told me I had breast cancer,” said Wolters, 44, of Holland, Michigan. “It was diagnosed as Stage Zero and it didn’t seem like that big a deal.”
But her case quickly began to take twists and turns, revealing just how complex some breast cancers can be.
Further imaging identified it as a fast-growing cancer. That meant aggressive. And the imaging also found cancerous cells in her other breast.
Wolters, a social worker, quickly decided she would keep a positive mental attitude to get through treatment and recovery.
“I have an excellent support system,” she said. “My husband and I told the kids, who are 18, 15 and 11, right away. I kept saying, ‘This is just going to be a bump in the road. We’ll get through it.'”
The importance of screenings
Working with Elizabeth Jeffers, MD, a surgeon at Spectrum Health General Surgery in Holland, Wolters decided it would be best to have both breasts removed.
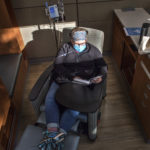
She had her mastectomy on March 10, the week much of the world turned upside down due to COVID-19. And the day she went home, instead of the quiet recovery she had imagined, schools in Michigan closed, throwing her family into a virtual-learning frenzy
And the surgery required some grieving.
“But I just said to myself, ‘Look, God gave me breasts to feed my children—and I did that. Now they are just another body part.'”
But then came more bad news. Pathology reports from the mastectomy recognized the cancer as invasive.
“That meant that the best course of action was to start chemo,” she said. “Which wasn’t something I bargained for. I had hoped the surgery would be the last of it.”
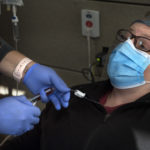
She started chemotherapy within a few weeks. While she worked hard to keep her positivity going, she believes it’s essential to be real, too.
“I was careful to be honest, especially with my family,” she said. “When I was having a hard time—and there were bad days, especially during chemo—I told them so.”
Wolter’s journey is highly instructive.
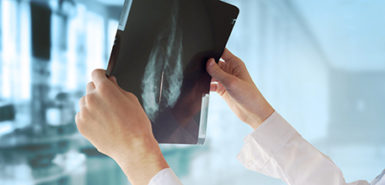
“Tabitha’s case is a complicated one,” Dr. Jeffers said. “And a powerful example of how important screening is. If she hadn’t gotten a routine mammogram or skipped a year, the outcome might have been quite different.”
The doctor’s advice? Undergo screenings and take precautions:
• All women 40 and older should have annual mammograms and conduct monthly breast self-exams. They should also have a yearly clinical exam with a provider.
• Recognize that some communities are at higher risk. White women and Black women develop breast cancer at roughly the same rate, but Black women are 20% to 40% more likely to die from the disease. “It’s especially important to encourage African-American women to get regular mammograms to help find any cancer earlier,” Dr. Jeffers said.
• Learn your family history. It is critical to let providers know the cancer history of parents, siblings, aunts and uncles. Women with a first-degree relative, a mother, sister or daughter who has had breast cancer have almost twice the risk, according to the American Cancer Society. (More distant family is less important.) Still, Dr. Jeffers said it’s important to know that most women who get breast cancer do not have a family history of the disease.
• Look for smart sources of information. Dr. Jeffers recommends Breast360, a site maintained by the American Society of Breast Surgeons.
Breakthroughs
“Breast cancer can happen to anyone,” Dr. Jeffers said. “Young or old.”
And when it does, she’s eager for people to know there has been tremendous progress.
“We stage breast cancer differently than we used to and have made many advances in identifying the biology and genetic components of different types,” she said. “We know better which are aggressive and which are more likely to recur.”
Treatments have improved. There are better medications. Surgery has progressed.
“We can limit the surgery we do,” Dr. Jeffers said. “And the surgeries themselves are becoming less deforming. We work more closely with plastic surgeons.”
Her message is clear: “Screening and self-awareness are the best ways to catch it early. Don’t be afraid to talk to your provider with any questions about breast health.”
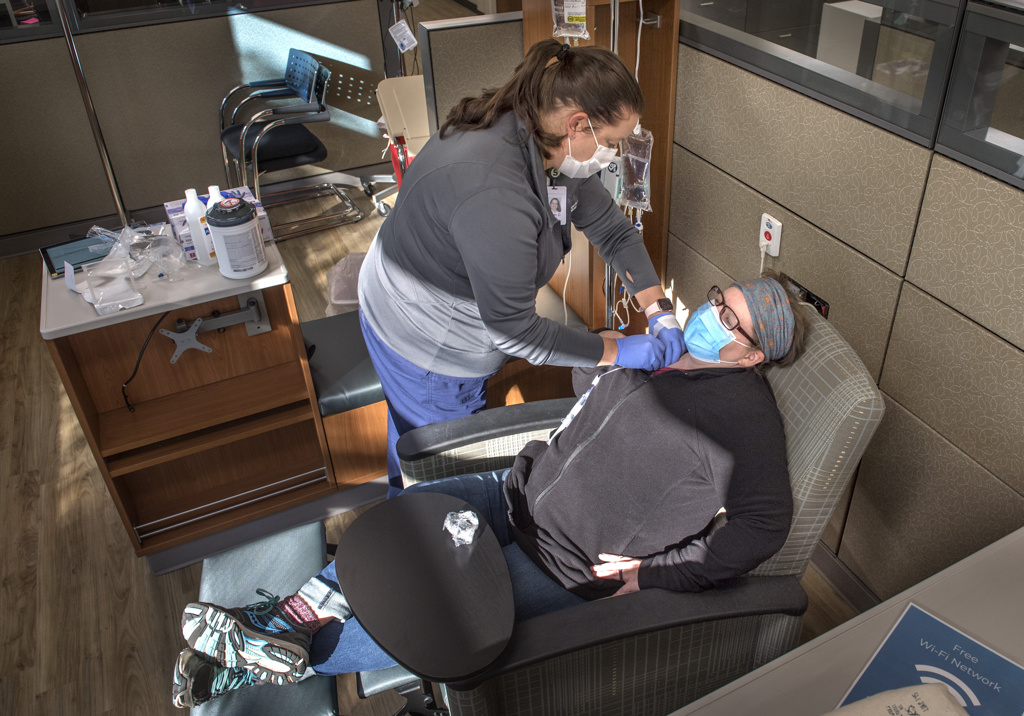
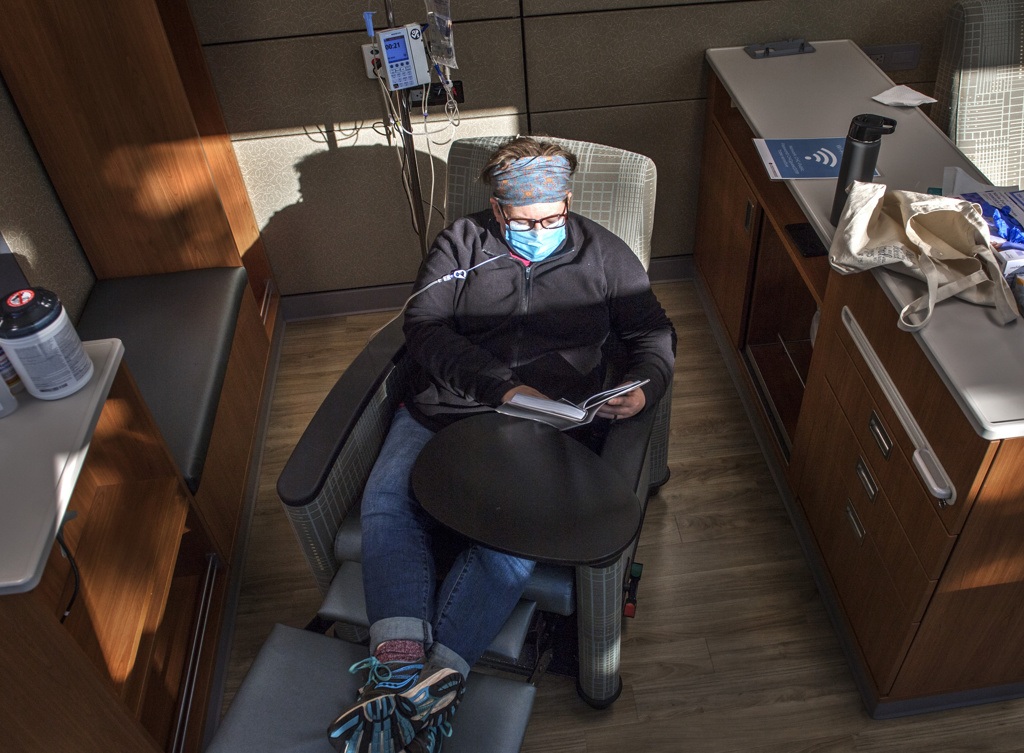
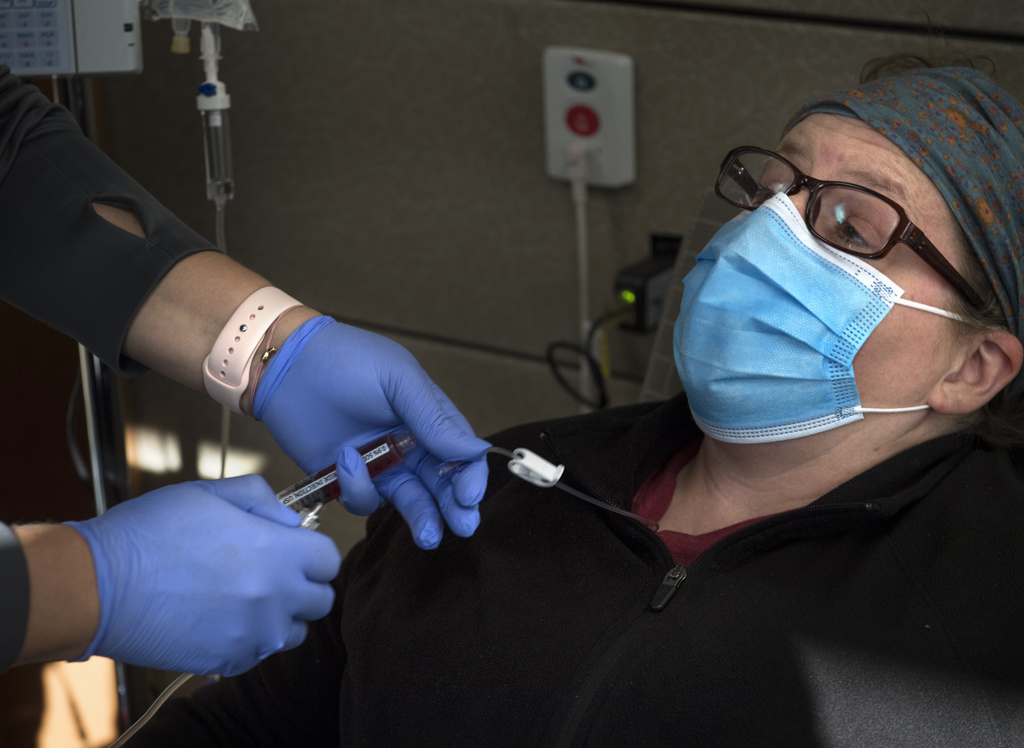
Wolters is glad she did. Now cancer-free, she is still getting IV infusions every three weeks and will do so for several months.
For the next 10 years she’ll be on Tamoxifen, a drug that blocks the effect of estrogen in breast tissue.
“I’m back at work, exercising again,” she said. “I’m just living life.”
She hopes to team up with Dr. Jeffers to help support other young moms with breast cancer.
“I’d like to be able to help,” Wolters said. “It’s a tough diagnosis for anyone, but especially hard when you’re juggling family and work.”
She has developed a deep respect for the unique aspects of each person’s cancer story.
“Everyone does it differently,” she said. “My journey is not the same as anyone else’s.”






 /a>
/a>
 /a>
/a>
 /a>
/a>
As a part of Jon and Tabitha’s family we are amazed at her strength going through this.
i’m so thankful to know tabitha and her family. her faith is inspiring and i’m so super grateful she can share this with my spectrum health family. so proud to be a part of this organization.
Such a strong person. I graduated with her father Russ Johnson and know the Lord is and was with her through out her journey. Prayers to all.
Thank you all for your kind words. She is truly a remarkable woman.