COVID-19 left Grace Biermacher feverish, coughing and oh-so-tired.
But when she donated plasma to help others with the disease?
Such a different story.
“That’s so awesome,” said Grace, a 20-year-old East Grand Rapids, Michigan, resident.
Thanks to donors like Grace, Spectrum Health recently treated its first three COVID-19 patients with antibody-rich plasma donated by survivors of the disease. They are among the first to receive this therapy in Michigan.
To help others, Spectrum Health is contacting recovered patients to ask for plasma donations. One donation can help two to four patients.
So far, three people have donated plasma. Grace and Corey Noaeill, a truck driver from Newaygo, are among them and share their stories of recovery and hope. They urge others to join with them in helping others.
“We really need donors,” said Gordana Simeunovic, MD, the infectious disease specialist leading COVID-19 work for Spectrum Health. “I would really encourage anybody who wants to donate to get in touch with (Versiti Blood Center of Michigan through their website).”
“We will guide potential donors through the whole process.”
Grace, who became sick while studying in Spain, was so eager to answer the call that she became the first COVID-19 plasma donor in Michigan.
“I figured since I was a young person who was able to recover from it, then it’s the least I can do—to offer up plasma,” she said. “I want to help out in any way I can.”
Power of antibodies
When a person is infected by a pathogen—like the novel coronavirus that causes COVID-19—the immune system creates antibodies. These antibodies help decrease inflammation and fight the infection.
Once the body successfully eliminates the virus—and the person recovers—the antibodies remain in the blood to guard against future infections.
With plasma therapy, doctors hope to harness the power of the antibodies from those survivors, by transfusing it to other patients fighting the disease.
The use of plasma from recovered patients—called convalescent plasma therapy—dates to the late 1800s. Doctors later used it during the 1918 Spanish flu pandemic and to treat measles, mumps and polio.
“Over the years, we have had multiple other medications—antivirals and antibiotics—and somehow this treatment was left behind,” Dr. Simeunovic said.
In recent years, doctors and researchers have used the therapy during the 2009 H1N1 pandemic, to treat Ebola in 2014, and with another coronavirus disease, Middle East respiratory syndrome (MERS), in 2015.
When COVID-19 surfaced in late 2019, doctors again turned to plasma therapy.
Research studies, involving 15 patients, showed good outcomes and no side effects from the treatment, Dr. Simeunovic said.
“Based on the reported cases now, we have very promising data. And we have a very good safety profile,” she said.
The U.S. Food and Drug Administration recently approved the use of plasma therapy as an experimental treatment in clinical trials and in cases involving critically ill patients who don’t have other options.
Spectrum Health received FDA approval to treat three patients under emergency treatment protocols, Dr. Simeunovic said.
“Transfusions were given without complications. Patients are still in the hospital and are under close observation,” she said.
It will take time to see the long-term outcome of the treatment, she added.
By working with Mayo Clinic, the national site for coordinating expanded treatment access, Spectrum Health can now treat severely ill patients with plasma therapy without seeking individual FDA approval in each case.
Dr. Simeunovic hopes eventually the FDA’s approval will expand to more patients, including those who are moderately ill.
Shocked by test result
Grace, a junior at the University of Michigan, went to Spain on Jan. 7 for a semester study-abroad program. As COVID-19 cases emerged across Europe, the program ended abruptly, and Grace returned home March 12.
Her mom suggested Grace get tested for COVID-19 because she had suffered what she thought was a cold. In her last week in Spain, Grace had a fever for several days, as well as nasal congestion and a cough. However, she never had body aches or shortness of breath—two other possible symptoms of COVID-19.
Four days after the specimen collection, Grace learned the result: Positive for COVID-19.
“I was a little shocked,” she said. “It was a little scary, but I was glad it wasn’t worse. By the time I got the results, I was showing no more symptoms.”
Before she could donate plasma, Grace underwent a second COVID-19 test—and the result was negative.
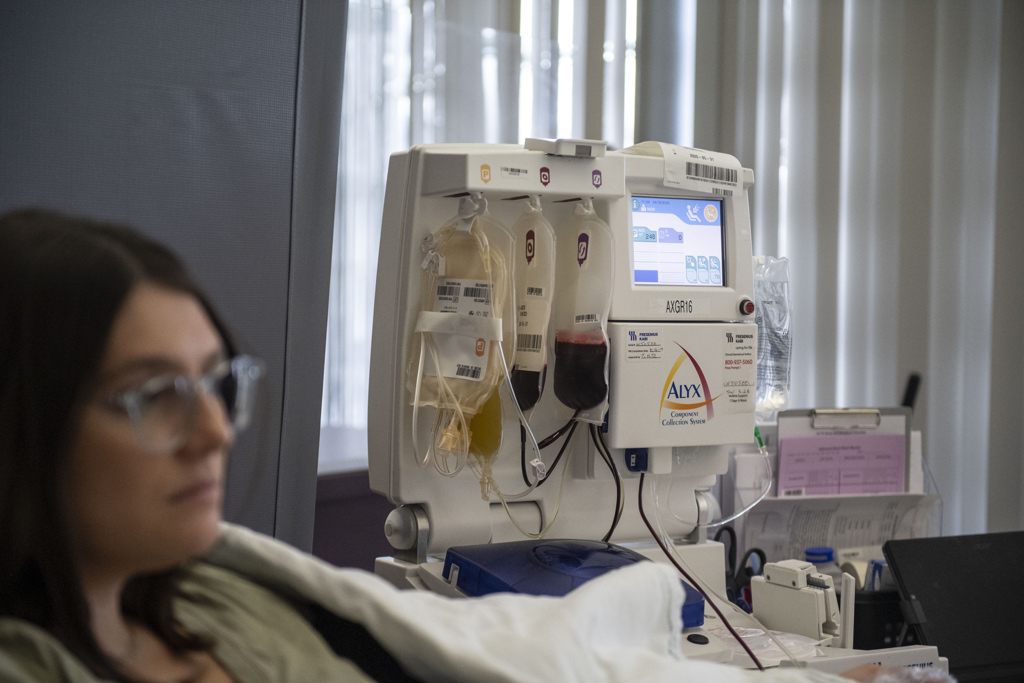
On April 9, she donated plasma at Versiti. The process took about 50 minutes and was similar to blood donations she has experienced in the past.
“It was pretty smooth,” she said.
She returned a week later to donate again.
Plasma donations may be made more frequently than other blood donations because the body replaces plasma more quickly than red blood cells.
Overcoming needle fears
Corey didn’t exactly look forward to plasma donation.
“I was terrified,” the 32-year-old said. “I hate needles. I don’t like hospitals or anything.”
But he didn’t hesitate when asked to be a plasma donor.
“If I can help somebody, I’m going to do what I have to do,” he said. “I have never had that opportunity before.”
He developed COVID-19 symptoms on March 11, a few days after a birthday celebration at a restaurant he later discovered had been visited by someone with the virus.
He had fever and chills for two days, followed by several days with a cough and runny nose. He underwent testing and learned about his positive result a few days later.
“I said, ‘You’re kidding. I feel 100% right now,’” he said.
He self-quarantined for 14 days.
He readily agreed to donate plasma because he worries about how the coronavirus affects people with compromised immune systems. He knows not everyone can overcome an infection as quickly as he did.
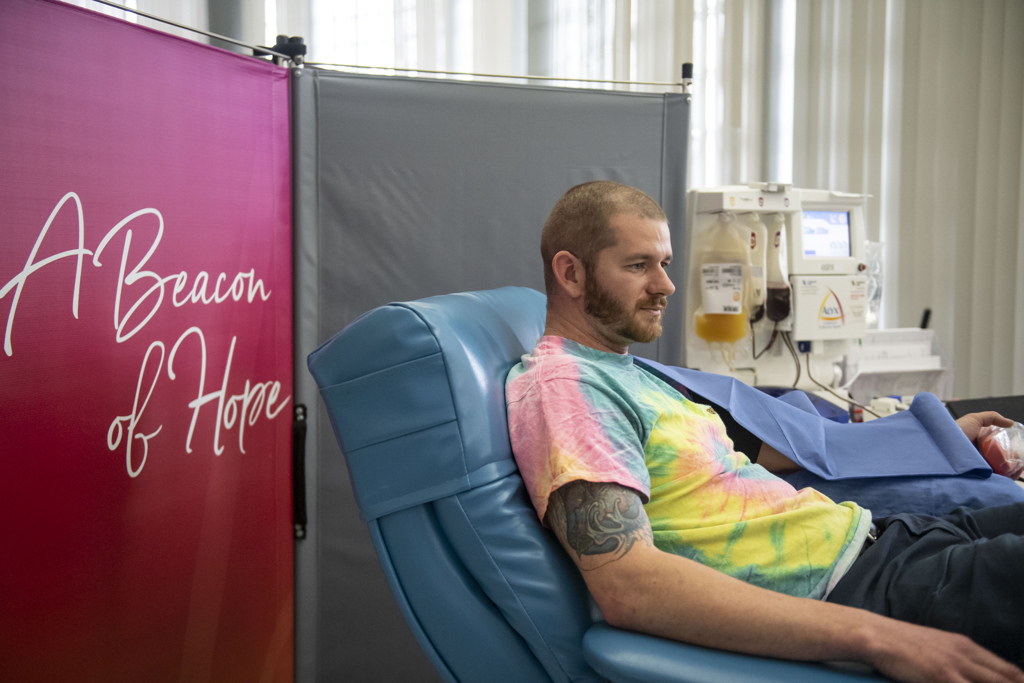
On April 14, he arrived at Versiti Blood Center of Michigan in Grand Rapids for the plasma donation. The staff eased his fears.
“They talked me through it and explained everything going on and helped me calm down,” he said.
Corey made an appointment to donate again a week later.
“I’m actually glad I got coronavirus, because now I can help people,” he said.
Helping each other
To donate plasma, donors must be symptom-free for at least 14 days, Dr. Simeunovic said. Those who have gone 14-27 days without symptoms must undergo a test to make sure the virus is no longer present.
Like blood donations, the plasma is also tested for other diseases.
The patients receive the transfusion like any other blood transfusion, in a process that takes two to four hours.
Dr. Simeunovic urged all those who have recovered from COVID-19 to consider donating plasma.
“It is really important for all of us to get donors on board,” she said.
“Even if you are over the disease, your family members can still become sick. Your neighbors can become sick. This will end much quicker if we help each other.”
Grace urged anyone else who is eligible to do the same.
“It is such a painless thing for you to do, to give back to so many people,” she said. “It could really make a huge difference.”


















 /a>
/a>
 /a>
/a>
 /a>
/a>
Please flood the media with this good news. People are not hearing about this . Please bring awareness. Loved seeing this promising article. It brings hope and a way people can come together and help.
During the week of Thanksgiving, I was diagnosed with COVID-19. Because I have heart disease and asthma, I received the monoclonal antibodies within the 10-day window of exposure and test positivity. The infusion was performed on Tuesday the 30th of November and I was back to work, and life, on the 6th of December. I am grateful that I was able to receive the antibodies and happy to know that its these antibodies that are still working to keep me from becoming reinfected. So very thankful today that my COVID-19 infection did not become anymore than a nasty head cold, cough and a little fatigue.