The memory is still vivid in Emily Seroka’s mind.
The 76-year-old Big Rapids resident remembers it as if it was yesterday—even though it happened in the 1980s.
“I was in New York City on a buying trip for my employer,” she said. “I work in retail. Still do—it’s a job I enjoy. I had been to New York before, but this time, the weather was horrid, and I suddenly became short of breath. I had a panic attack when I couldn’t get my breath.”
During this event, Seroka learned she had asthma. She began using an inhaler.
“I had been a smoker for a long time, but I had quit before then,” Seroka said. “Back when I started, we didn’t know that smoking was bad. It was considered glamorous.”
With passing years and more awareness of the health risks, Seroka put her cigarettes aside—but her breathing problems persisted.
For some years, using the inhaler on occasions when she felt short of breath was enough.
“No big deal,” she said. “It wasn’t until Donald, my husband, and I moved to Big Rapids in 1995 that I got really sick. It was around Thanksgiving, and I felt like it was a sin to call on Black Friday, but since we didn’t yet have doctors in the area, I called the hospital to ask what I should do.”
The emergency department staff at Corewell Health’s Big Rapids hospital told her to come on in. No time to be shy.
A new diagnosis
The emergency department team did not release Seroka to return home.
“They put me in the hospital for five days,” Seroka said. “I felt fine, but my oxygen level was low, and it kept dropping.”
Seroka was diagnosed with COPD—chronic obstructive pulmonary disease, a progressive lung disease causing airflow blockage and breathing-related problems.
“I continued using inhalers for the COPD, not much more than that,” Seroka said.
In the early 2000s, however, physicians at Big Rapids hospital diagnosed Seroka with lung cancer.
The bottom left lobe was surgically removed from her lung. Assured that the cancer was fully removed, Seroka opted not to receive further treatments, chemotherapy or radiation.
As the COVID pandemic took hold, Seroka received all her vaccinations and boosters. She was considered high-risk due to her lung issues.
“I thought I had avoided COVID, and for a long time I did, but then I got it. That got me back into the hospital,” she said.
She spent 2022 in and out of Big Rapids hospital throughout 2022 for breathing problems.
Pulmonary rehab changes everything
Seroka heard that Corewell Health offered a pulmonary rehabilitation program. That sounded like something she wanted to try, to alleviate her many breathing issues.
Pulmonary rehabilitation programs are specially designed to help people with lung diseases such as COPD and emphysema.
She was also referred by Katelin Aris, G-NP, DNP, to see John Egan, MD, director of interventional pulmonology at Corewell Health.
“When I met Emily, she had chronic bronchitis,” Dr. Egan said. “Her left side airway was twisted, so it was hard for her to clear mucus out of her lungs.”
The team performed a pulmonary function test to determine the type of COPD she has.
“We get a good patient history, find out what makes the patient short of breath, what are the times it happens. We have the patient walk for six minutes while we measure the oxygenation in their blood,” Dr. Egan said.
Referencing test results, Dr. Egan determined the optimal inhaler type for Seroka.
“There are three classes of inhalers with six or seven in each class,” Dr. Egan said. “There are inhalers that dilate the airways and steroids that reduce inflammation. When Emily had an allergic reaction to one type of inhaler, we were able to switch her to another.”
In addition to daytime inhalers and a BiPAP ventilation machine to help her breathe at night, the pulmonary rehab program was an ideal match for Seroka.
“It was great!” Seroka said. “I soon realized pulmonary rehab was key to living with lung problems.”
She attended one-hour sessions several times a week for 24 weeks.
“A therapist treated mind and body, taught us how everything works together,” Seroka said.
She learned breathing techniques, nutrition, information about lung issues and exercise techniques. In the program, Seroka lifted weights, walked on a treadmill, rode a stationary bike, rotating exercises.
“I usually had to go up stairs slowly because it was hard to breathe, but one day I ran up the stairs and suddenly realized—I can do this!” she said.
Not least, Seroka said, was the emotional support she received by meeting others dealing with similar lung issues.
Labor Day weekend 2022, Seroka had another breathing attack. Struggling to get air, she found herself needing emergency care.
“Suddenly it was a dire emergency,” she said. “I learned later that one of my lungs had collapsed. I was immediately intubated and put on a ventilator, so when I was told later that I was airlifted to Corewell Health, I thought, ‘Darn, I missed the whole thing!’”
Seroka laughs as she recalls the memory, but at the time, the situation was serious. Hospitalized, she was put through a battery of tests—bronchoscopies, MRIs, PET scans and ultrasounds.
Life lessons
Even though the primary purpose of the tests was to understand her lung issues, another unexpected result showed up.
“The top part of my liver showed tumors,” Seroka said. “It turned out that I had cancer, stage 4, but I was told I should have another eight years. At my age, that’s fine. I have lived a good life.”
To make her life one of quality and easy breathing, Seroka has continued the pulmonary rehab program.
“The rehab program helps me not only with lung issues,” she said. “It has helped cope with the cancer, too. From that program I have learned that you don’t wait for someone to take you by the hand to take care of yourself. A positive attitude makes a difference.”
Seroka isn’t even considering retirement yet. She loves her work too much. With her husband, Donald, the pair is planning more travels to favorite destinations, including Michigan’s Upper Peninsula.
“And I think I will join a gym to keep exercising and stay strong,” she said. “It is up to you, you know, to put a plan in place from the knowledge you gain in the pulmonary rehab program. Then you just make daily adjustments.”


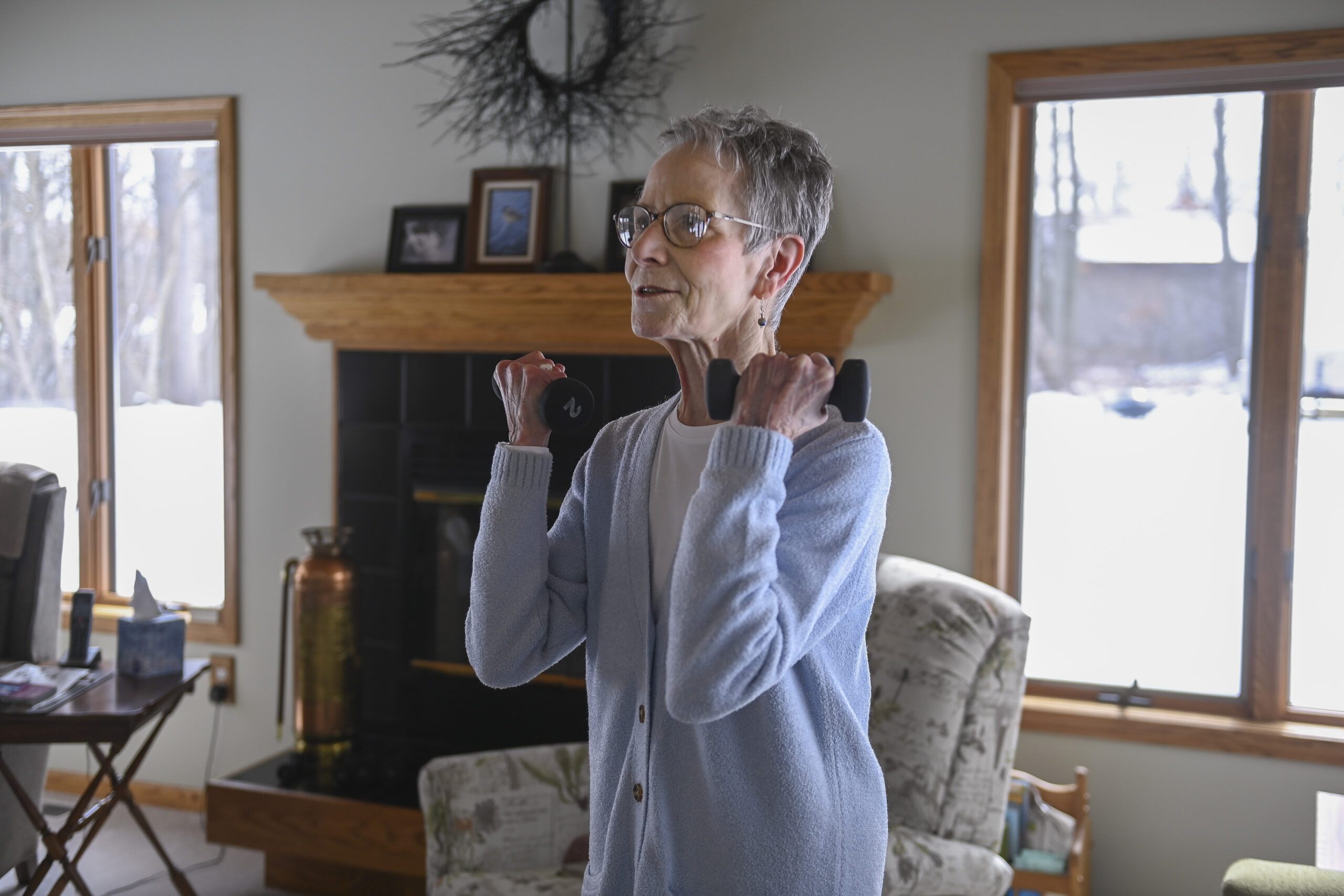







 /a>
/a>
 /a>
/a>
 /a>
/a>
Living with lung disease can feel isolating, but this article reminds us that we’re not alone. There are so many people out there who are thriving despite their illness. It’s important to focus on what we can do, rather than what we can’t. Thank you for sharing these inspiring stories!