Wester Rodriguez arrived from the Dominican Republic, showing little outward sign of a heart condition.
As the 3-year-old bounded into his host parents’ home—and hearts—they hoped that, just maybe, his condition was not that serious.
It was. In fact, Wester’s medical team would soon discover an extraordinarily rare and challenging problem.
Crafting a solution for the boy’s ailing heart would take the combined skills of world-renowned experts in surgery and interventional cardiology at Spectrum Health Helen DeVos Children’s Hospital.
“We call him our miracle boy,” said Carol Nyeholt, as Wester searched through a pile of toys in the living room of her Hudsonville, Michigan, home.
“Minnie! Pluto!” he cried. He pulled out the figures and set them in a pink playhouse. “Dinosaurio!”
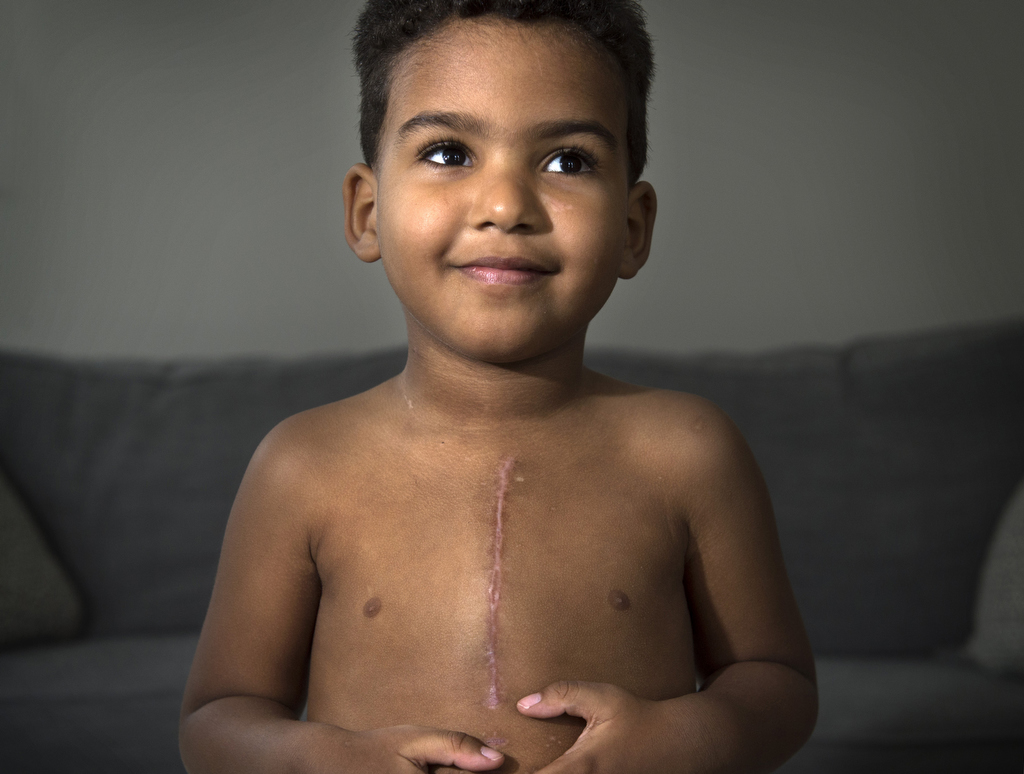
The only sign of Wester’s medical ordeal is the scar on his chest, already healed and blending in. But just a month earlier, he was in the hospital recovering from heart surgery.
Far from home
Wester lives in Santo Domingo, the capital city of the Dominican Republic, with his parents, Julia Casteryn Dilone and Wilfredo Rodriguez.
Healing the Children, an agency that works to arrange medical care for children worldwide, brought him to Grand Rapids, Michigan, for heart surgery.
Carol and Bryan Nyeholt, veteran host parents, cared for Wester for three months. He became one of the family, calling them Mama and Daddy.
He soon learned enough English to understand what they said. All three of the couple’s children know some Spanish, and the oldest, 22-year-old Whitney, is fluent.
Wester settled into the Nyeholts’ home, enjoyed familiar movies and iPad games, and discovered the joys of snow. When he climbed a flight of stairs, he huffed and puffed. But in general, he seemed to be a healthy 3-year-old.
The medical team at the Congenital Heart Center at Helen DeVos Children’s Hospital volunteered to provide his care. Leading the effort were two experts who have teamed together for years to repair children’s hearts: Marcus Haw, MBBS, FRCS, the hospital’s chief of pediatric cardiothoracic surgery, and Joseph Vettukattil, MD, MBBS, the chief of pediatric cardiology.
The doctors understood Wester’s desperate need of surgery.
He had tetralogy of Fallot with absent pulmonary valve syndrome, a rare and complex birth defect that affects the structure of the heart. He had a hole between the lower chambers of his heart, along with obstruction to the right ventricle flow, and there was no valve to regulate the flow of blood from the right ventricle to the pulmonary artery.
The condition caused the mixing of oxygenated and deoxygenated blood—so he could not get fully oxygenated blood circulating through his body.
Before he underwent surgery, he had a CT scan and heart catheterization to examine his heart.
Those tests revealed an even more unusual problem: Wester had no left pulmonary artery. This impaired blood flow to Wester’s lungs.
The main pulmonary artery should have divided into two branches and delivered blood to both lungs. Instead, it pumped blood only to the right.
This additional complication would limit the benefit Wester could get from surgery to correct the other defects, Dr. Haw said.
Creating a lung artery
Dr. Vettukattil saw hope for a fix. It meant attempting a procedure he performed only in infants. He could not find reports of the repair ever being performed on a 3-year-old.
A CT scan did not show any remnants of the left lung artery demonstrable on the CT angiogram. However, cardiac catheterization suggested Wester once had a left lung artery supplied by a blood vessel that is normally only open in the womb. The vessel closes soon after birth.
On Nov. 9, 2015, Dr. Vettukattil performed a cardiac catheterization and, working slowly and carefully, managed to guide a wire to that vessel. He passed the wire through it and down to the left lung, where he found the network of blood vessels in the lung. He inserted two stents to connect the lung’s blood vessels to the heart.
An X-ray image of the lung showed what happened when he did: a web of blood vessels lit up, as blood pumped into them.
“See how the blood smoothly flows,” Dr. Vettukattil said, as he reviewed video of the procedure. “There’s a lot of blood going through. It’s a normal lung.”
It wasn’t a permanent fix—but it marked the location of the lung’s blood vessels.
The next day, Dr. Haw performed open heart surgery to repair the birth defects caused by tetralogy of Fallot.
With the stents to guide him, he also inserted a tube to connect the pulmonary artery to the left lung.
For the first time in his 3-year life, Wester had two working lungs, which received blood with every heartbeat. He also inserted an artificial pulmonary valve.
A scary five weeks
Complications following the operation kept Wester in the hospital for five weeks. He suffered respiratory failure and had to be sedated and put on a ventilator.
He required a second heart surgery to close what remained of the opening between the lower chambers of his heart.
As his medical team worked to help him recover, his host family provided emotional support around the clock—through November, the Thanksgiving holiday and the first two weeks of December.
Carol stayed at the hospital Monday through Thursday. On the weekends, shifts were shared by Bryan and their 20-year-old son, Trevor, and their daughters, Whitney, 22, and Brooklyn, 17.
“It was very scary,” Carol said. “You just wonder if you are ever going to get out of this pit.”
Throughout Wester’s stay, Carol communicated with his mother on Facebook and through texts. But she didn’t know how to tell her about the complications. Wester’s doctors had a conference call with a doctor in the Dominican Republic, who explained the situation to Wester’s mom.
“As a mother, it just breaks your heart,” Carol said.
Helen Salan, the director of the Ohio and Michigan chapter of Healing the Children, was amazed by Wester’s medical care.
“Oh my gosh, that was a groundbreaking procedure,” she said.
And she praised the Nyeholts for providing a loving home. “It’s a commitment they make, and they believe in what they do,” she said.
A fast rebound
After three weeks, Wester came off the ventilator. He then seemed to progress at top speed, the Nyeholts said.
He left the hospital Dec. 15. On an afternoon just a month later, he ran around the Nyeholts’ house, exuberant and playful.
“He has a lot more energy now,” Bryan said. “We were joking with Dr. Haw that he may need a flow meter to slow him down.”
Carol laughed but shook her head.
“We would never,” she said. “We sat in the hospital for five weeks just praying that he would be OK.”
Carol said she’s impressed by Wester’s good nature, especially given how much he endured in a short time.
“I can count on one hand the number of times he has cried,” she said.
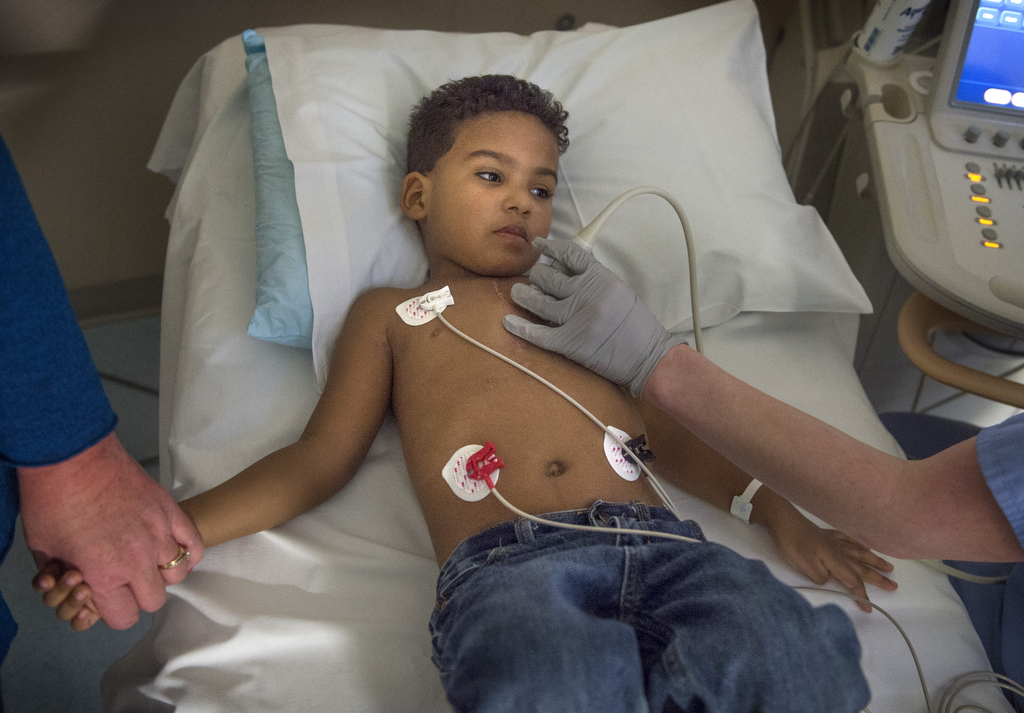
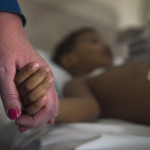
On Jan. 21, she and Brooklyn took Wester to the 10th floor of Helen DeVos Children’s Hospital for a last checkup before he went home to his mother.
Wester was all smiles as he climbed on a bed for an electrocardiogram.
“No dolores,” Carol said in Spanish. “It won’t hurt.”
Wester held her hand. His eyes remained fixed on the TV above, where a movie began in Spanish. He pointed excitedly and cried, “Minions!”
A short time later, he met with Heather Sowinski, DO, a pediatric cardiologist. She listened to his heart with a stethoscope.
With a prosthetic valve, his heart beat “is still noisy,” she said. “But it’s much better.”
She put the earpieces in Wester’s ears and held the stethoscope to his chest. He looked up at her through long eyelashes, his expression intent and serious.
“You always amaze me, dude,” Dr. Sowinski said. “You are wise beyond your years.”
Back home
Three months after he arrived in West Michigan—and glimpsed his first snowfall—Wester returned home to his parents in sunny Santo Domingo.
His family sent photos to the Nyeholts to let them know he is doing well. In one, he holds a smartphone displaying a picture of Carol and Bryan. And, in a video, Wester says in English, “I love you, Mama.”
Wester’s mom seems overwhelmed with gratitude for the care her son received in Michigan.
“She told us multiple times she is very thankful,” Carol said.
For Carol, the transition is bittersweet. After hosting six kids through Healing the Children, saying goodbye does not get any easier.
“It’s heartbreaking. You love these kids like they are your own,” she said. “I’m afraid I love them too much because it’s so difficult to give them up. But you aren’t doing your job if you don’t love them.”
Photos showing Wester wrapped in his parents’ arms help.
His mom “is thrilled, and that makes my heart happy,” Carol said. “She loves him a lot. And she missed him a ton.”















 /a>
/a>
 /a>
/a>
 /a>
/a>
Just a beautiful work, the story and how you wrote it, Sue.
Thanks so much, Lori!
That’s a blessing! My son has that same scar, he was born with a Teratoma over his lungs and heart at birth. He is 5 months old now, he had surgery at 1 week old at Children’s Hospital. So glad the both of you are fine.
I am so glad your son is doing well, Charda! Thanks for reading.
I’m so impressed and inspired by the team of physicians and the host family, and so thankful for a wonderful outcome! Such a beautiful story 😊
Thank you, Teresa! I loved little Wester’s story, too. Wouldn’t it be a fantastic experience to host children? 🙂
So happy to read the story of little Webster ! And what Dr Haw did for him! Because he will be doing surgery on our little great granddaughter and major task ! Shows he has great skills! Thank you Lord for Dr Haw!