It started with a prayer.
Susan, a 12-year-old girl living in an orphanage in Myanmar, made a heartfelt request.
“I prayed to God to please give me the opportunity that I can speak more clearly,” she said.
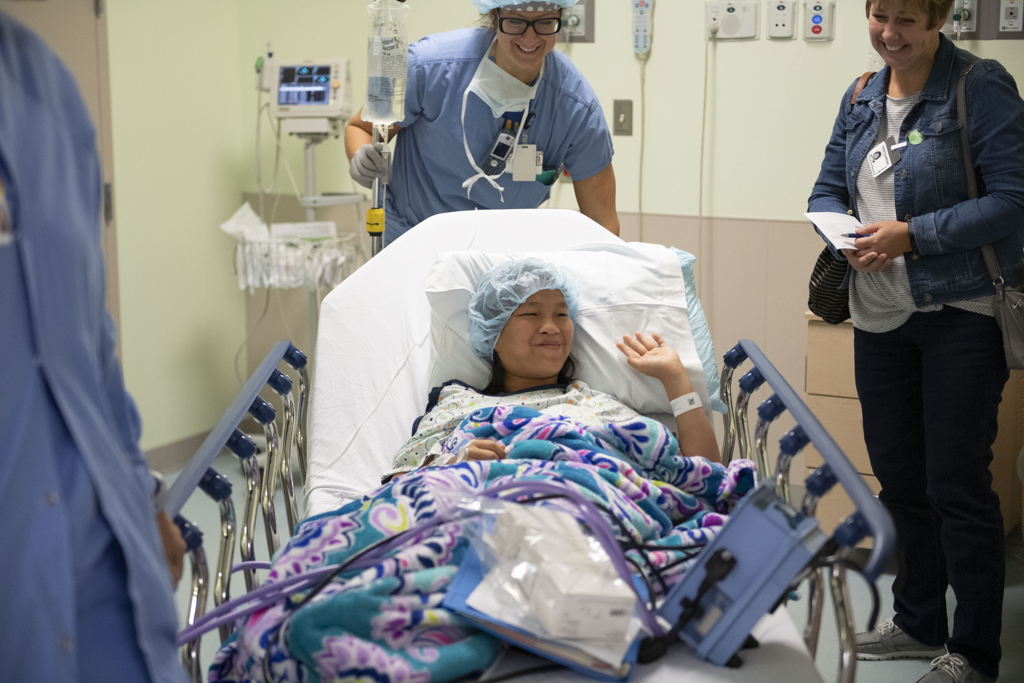
Months later, she sat on her hospital bed, smoothing out the pink and teal fleece blanket spread around her.
“Now I get the results,” she said. “God answered my prayer.”
In a few moments, Susan would undergo her second surgery at Spectrum Health Helen DeVos Children’s Hospital to repair her cleft palate. With help from an interpreter, she told how she prayed every day for two years for this moment.
“I’m really happy,” she said.
A tearful hug
Susan, now 14, lives in a home for orphans with her 16-year-old sister and a dozen other children.
“(Myanmar) is a rough place. The poverty there is just astounding,” said Larry Bauss, MD, an anesthesiologist in Kalamazoo.
Several years ago, he and his wife, Deb, started Living Hope Myanmar, a ministry that supports a home for orphans in Yangon (formerly known as Rangoon).
In 2007, Cyclone Nargis struck Myanmar, leaving 140,000 people dead or missing.
“A lot of kids became orphans or separated from their families without the ability to reunite them,” Dr. Bauss said. “A lot of kids in Susan’s age group are in children’s homes now because they lost their parents or they couldn’t find their parents. They were just toddlers at the time.”
When Dr. Bauss traveled to Myanmar to visit their children’s home in January 2019, an aid group asked him to visit another orphanage in the area.
On the last day of his trip, he set out for the orphanage. He almost didn’t make it. He wandered for more than an hour through a tangle of unnamed dirt streets and shacks before he found the home.
The house mother greeted him warmly and introduced him to the children as they came home from school.
“I was very impressed by the children’s home,” he said. “It’s very much a family-based model. The kids are close to each other.”
The house mother mentioned in passing that Susan had surgery as a child, but it “didn’t work.” Dr. Bauss asked for details.
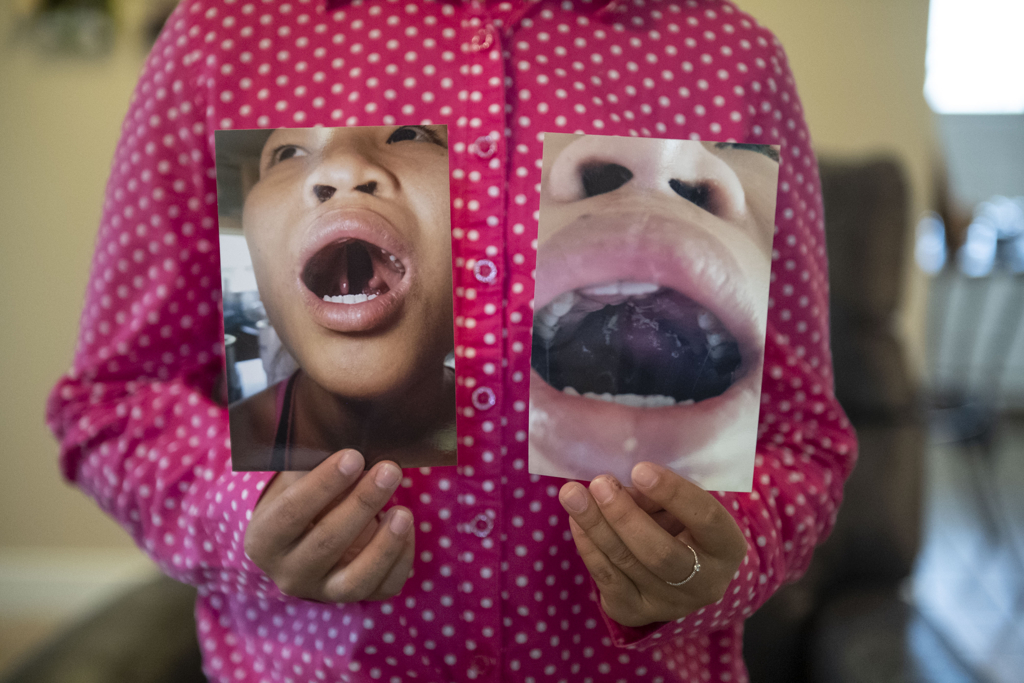
He learned Susan was born with a cleft lip and palate. She underwent surgery as a young girl, but it appeared the surgeon repaired only the lip, not the palate.
In the roof of her mouth, Susan had a double cleft. This interfered with her ability to make certain sounds and made it difficult for her to speak clearly.
Dr. Bauss had no idea if he could help her, but he wanted to try. He asked if the house mother could arrange a passport for Susan if he could find a way to bring her to the U.S. for surgery. When the woman translated his words for Susan, the young girl burst into tears and hugged him.
The house mother explained that she and Susan prayed every night that someone would show up one day and help her.
“The first thing I thought to myself was, ‘What a ridiculous prayer. You can’t even find this place,’” Dr. Bauss recalled.
“And then I thought, ‘Wait, maybe it’s right now.’”
When he returned home, he contacted Helen Salan, the director of the Healing the Children Michigan-Ohio chapter. She quickly made arrangements for Susan’s trip to the U.S.
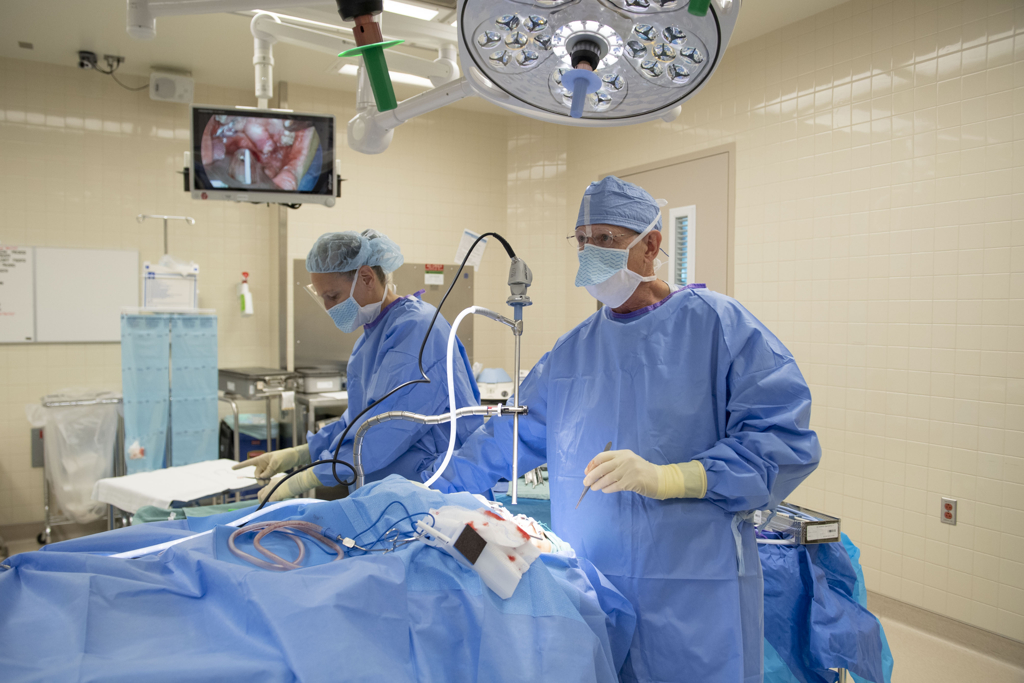
Robert Mann, MD, a pediatric craniofacial surgeon, agreed to perform the surgery at Helen DeVos Children’s Hospital.
For the past 35 years, Dr. Mann has developed and refined an approach to cleft palate repair that helps children achieve the best speech and facial structure possible—in childhood and through their adult years.
His anatomic palate restoration philosophy is a personalized approach involving the replacement of missing tissue, sound wound-healing principles and techniques that minimize disruption to the palate muscles.
Dr. Mann, who lectures and demonstrates his approach internationally, has studied the long-term results of his cleft palate surgeries.
Recently, he examined the outcome of treatment on 116 patients who had complex cleft palates. They underwent surgery as young children and are now 16 and older. He found:
- Less than 7% needed follow-up surgery to improve their speech.
- Less than 5% were recommended for a later jaw surgery to improve their facial structure.
- Altogether, 90% had normal speech and face structure. With the traditional approach, only 9% achieved that outcome.
Fear and determination
For Susan, the trip to Michigan meant leaving her home, making her first trip on an airplane, and living in a strange place filled with people who spoke another language. But she didn’t hesitate.
“I would be scared, but I would like to come,” she said.
On July 11, 2019, Susan arrived in West Michigan and met Roxanne and Tim Bareman, her host parents.
They welcomed her to their home in Hudsonville. Despite the language barrier, Susan soon settled into family life in Michigan.
She enjoyed swimming and boating and made frequent trips to Six Flags Great America theme park in Illinois. She especially liked garage sales—she shopped for crafts and gifts for her friends at the children’s home.
Her cleft palate surgery, scheduled for July 27, had to be delayed because Susan had an illness.
On Aug. 23, she underwent her first surgery.
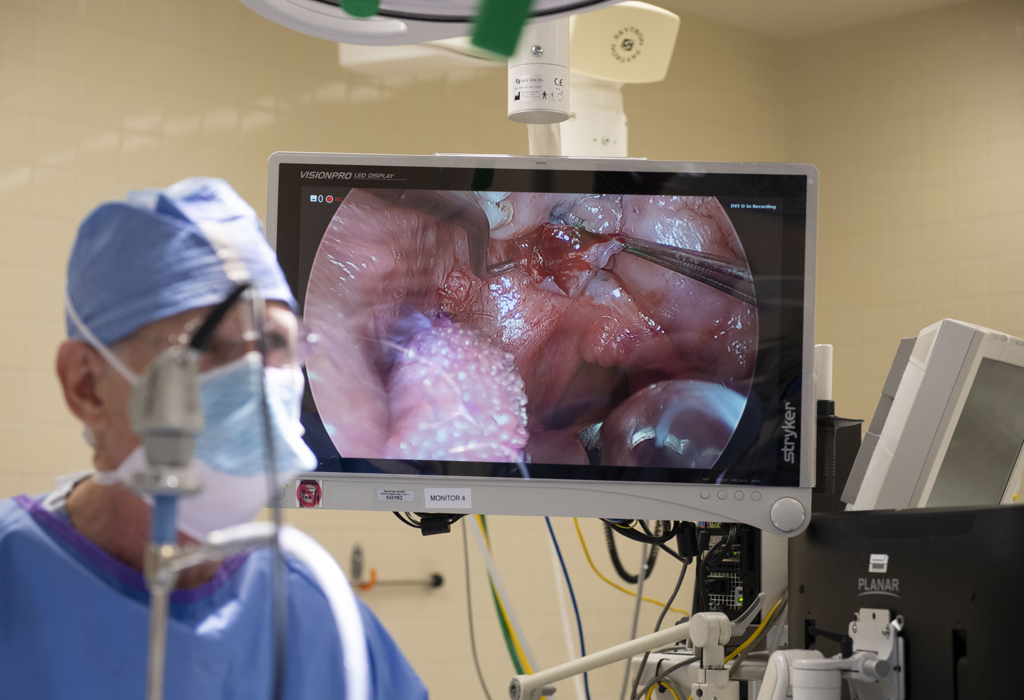
Dr. Mann used inner cheek tissue—buccal flaps—to replace the missing tissue in the double clefts that ran from the front to the back of her palate. Although she lacked some of the muscles that control the palate, he was able to reposition her existing muscles so they could compensate.
During the operation, Dr. Mann noticed Susan bled more than expected. After the surgery, he referred her to a hematologist for testing.
The doctor diagnosed her with Von Willebrand disease, a genetic bleeding disorder caused by a missing or defective clotting protein.
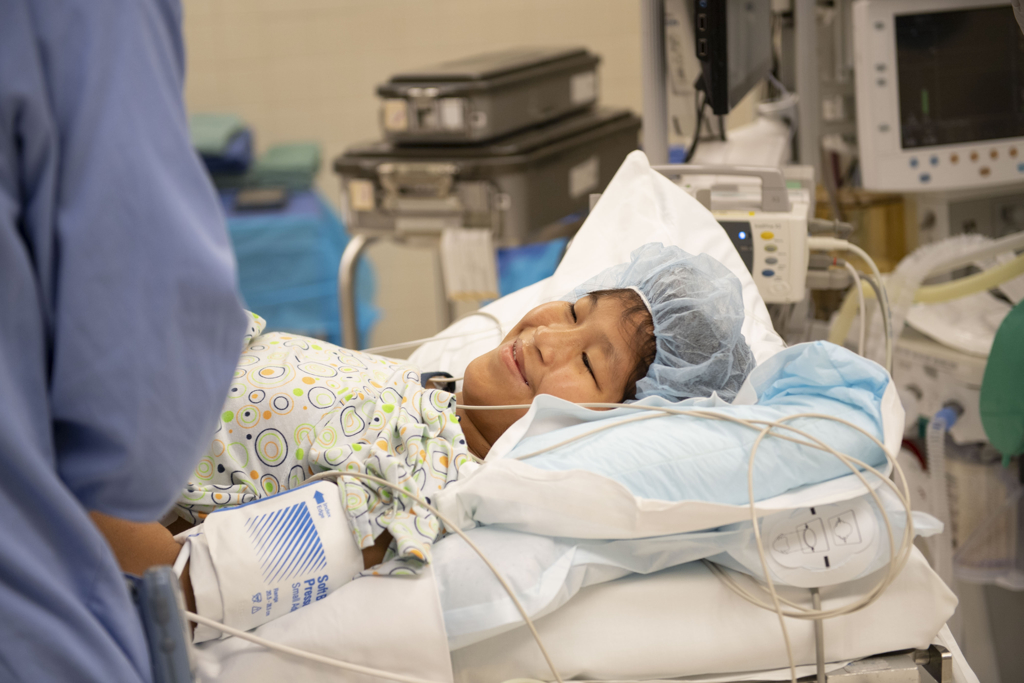
On Oct. 7, Susan returned for the second operation on her palate. This time, she received medication before surgery to help control bleeding.
As she waited before surgery, Susan sat on her hospital bed and talked about her hopes for the future. Someday, she would like to be a pastor or a doctor.
Through the interpreter, she added, “I am so happy, because there are opportunities by his grace, by the grace of God.”
During the second surgery, Dr. Mann addressed the missing bone in the front arch of her palate. He closed the gap with gum tissue that will generate bone growth.
Progress already
A few days later, Susan stood at a craft table set up in the Baremans’ living room, with a view of woods aglow with the orange and yellows of fall.
In front of her lay a scrapbook surrounded by stacks of photos and stickers. Page by page, she placed pictures of the people, events and places that held special memories of her trip to Michigan.
One photo showed her in front of Helen DeVos Children’s Hospital, looking tiny in front of the 11-story building. She added text above and below that read “Glory to God” and “Give thanks to the Lord.”
Although shy about speaking English, Susan showed with nods and smiles that she often understood Roxanne.
She led the way to her bedroom to show her collection of stuffed animals. She hugged her favorite, a soft gray bunny. And she pulled out bags of craft projects and gifts she had bought for her friends at the children’s home.
With the repairs to her cleft palate, Susan’s speech quickly showed progress, Dr. Mann said. When asked, Susan was able to make “Ba” and “Da” sounds, showing the repaired palate was doing its job. Without a functioning palate, those hard consonants come out with a nasal sound, and can be difficult to understand.
“There is no reason she can’t talk from a functional standpoint,” he said.
That will continue to improve over the next couple of years as scar tissue softens and the muscles move more freely.
“I’m fairly confident if we give her a few years, she is going to do very well,” Dr. Mann said.
Opening doors
In late October, Susan returned home, bringing suitcases packed with gifts to share with the orphanage.
Dr. Bauss plans to put the house mother in touch with a speech therapist who can teach her exercises for Susan.
“This will be life-changing for her,” he said.
Although accepted and loved at home, Susan encountered teasing and ostracism at school because of her speech defects. The ability to speak clearly will help her at school and in society as she grows up.
“This is really going to open up doors for her,” he said. “She can go out in the marketplace and find a job. It is tough there, but there is some hope for her.
“It’s just a blessing.”
































 /a>
/a>
 /a>
/a>
 /a>
/a>
This is an amazing story, congratulations to the entire team!
Susan was blessed to have such an opportunity. Having worked with an orphanage on the Thai-Burmese border (2008-2010), this story speaks volumes to me! There are still so many children globally in need of medical care, which is why it is great that Dr. Bauss found her through his travels abroad. There are still many countries with extremely vulnerable populations. Keep searching, keep travelling, keep helping!
You probably understand more than any of us what this means for Susan.
It’s amazing they connected — and that he was able to help link her to Healing the Children and Dr. Mann.
Thanks for reading and commenting.
What a wonderful and inspiring story. I am filled with joy over those who help this your girl. This story causes me to pause and thank God for His goodness and faithfulness to man kind. Truly there are some kind and compassionate people in the world. This story brought tears to my eyes. I am going to pray for Susan and for littles ones like her. You don’t know how blessed you are until you encounter people who are less fortunate.
Awww, thank you, Stanley, for your heartfelt comments and for sharing how much this story impacted you. These kinds of stories definitely drive home how compassionate and incredible people are in this community. We’re truly fortunate. This story also brought tears to my eyes as she truly had an answer to her prayers. So amazing. 🙂
A wonderful story and, again, well-told. Thank you, Sue. God bless this beautiful young lady as she returns to her homeland. I hope her desire to be a pastor or doctor is realized.
Thank you, Harvey, for your kind comment. We’re also hopeful she is able to achieve her dreams, and know this surgery and the loving care she received at Helen DeVos Children’s Hospital and in this community will certainly help her along her life path. Many blessings to you!
Thank you, Harvey! It does touch my heart to see Susan’s dreams of becoming a doctor or pastor. She has a kind, compassionate heart.
Dr Mann is our angel. He did 9 surgeries on my sons Bilateral Cleft Palette as a child. He’s an amazing Plastic Surgeon and an amazing person. My son still keeps in contact with him! A man that changes children’s lives forever is one good soul.
Pat, this is so uplifting. Thank you for sharing your testimony regarding Dr. Mann and how well your son is doing. This is absolutely wonderful news.
Cheers, Cheryl
Dr Mann is an excellent surgeon and very caring person. He has helped so many children and adults through out his career and all of his patients love him! Grand Rapids is very blessed to have him here.
We certainly are, Jill. Thanks for your kind comment and for being a Health Beat reader!
Thanks, Roxanne and Tim, for your part in her story! You guys are awesome examples of living as Christ calls us to do! ❤️
What an incredible story of hope, courage and answered prayers! Our family is also so blessed to have the HDVCH Plastic and Craniofacial Surgical team on our journey to correct our adopted daughter’s cleft lip and palate. They have been an answer to our prayers pouring out Christ’s love into these kids. Thank you so much for all you do and many blessings to you for the incredible impact you have in so many lives!
How wonderful! Many blessings to you and your family, Lyndsey!
Dr. Mann cared for my bilateral cleft lip daughter. It is amazing to watch the work he does. We are so blessed to have him so close to us, as goes for his whole team. My daughter gets sad to think she will outgrow getting to see Dr. Mann every year in follow up.
Dr Mann is the best that we could ever get. He did the same surgery on my Son Sergio Reyes 19 yrs ago he was his first patient he used glue with instead of stitches and you can not tell unless we tell you that my son had this condition. Dr Mann has went well beyond his limits to help my son and family!! We will never be able to Thank him enough!
Never doubt the impact you make Dr. Mann! I feel so lucky to work with you and the world class team at HDVCH!
Thank you for sharing this spectacular young person’s story! Congratulations to the entire team for helping this child.
Wonderful story! Dr. Mann is a wonderful, kind man and takes after his father.
To think that I work for an organization as SH and see the many miracles and answers to prayer!! Wonderful outcome for a very deserving young lady!!
This article was especially touching for me: Of the 5 children in my family or origin, one of my sisters & i were spared cleft
palates. The other 3 (a boy & 2 girls) weren’t. I believe the girls were more affected than my brother. The youngest of the girls told our parents that she would rather have additional surgery than pursue post secondary education. Our parents gave her both. (She became a nurse practitioner with a faculty position in a university medical center.)
Thank you for sharing, Jim, and all our best to you and your family.