Amanda and Jeff Miles often held their breath when dealing with their son’s early struggles in life.
Could his heart defect be repaired? What would be the effects of chronic pulmonary disease? Would he ever be out of the proverbial woods?
They held their breath with hope.
They held their breath for guidance.
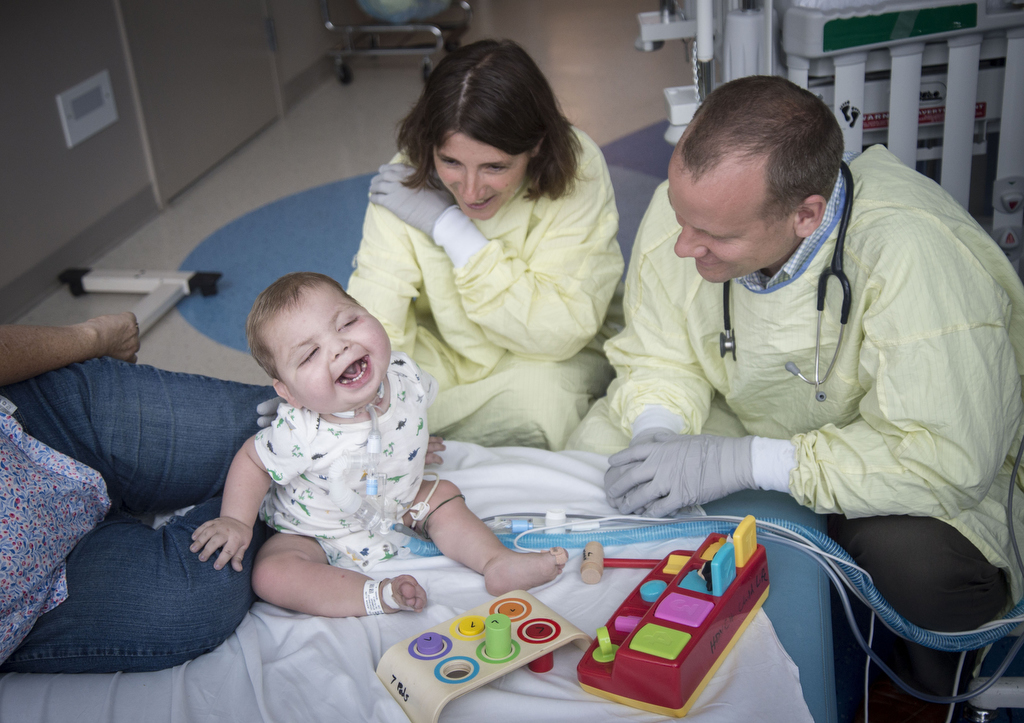
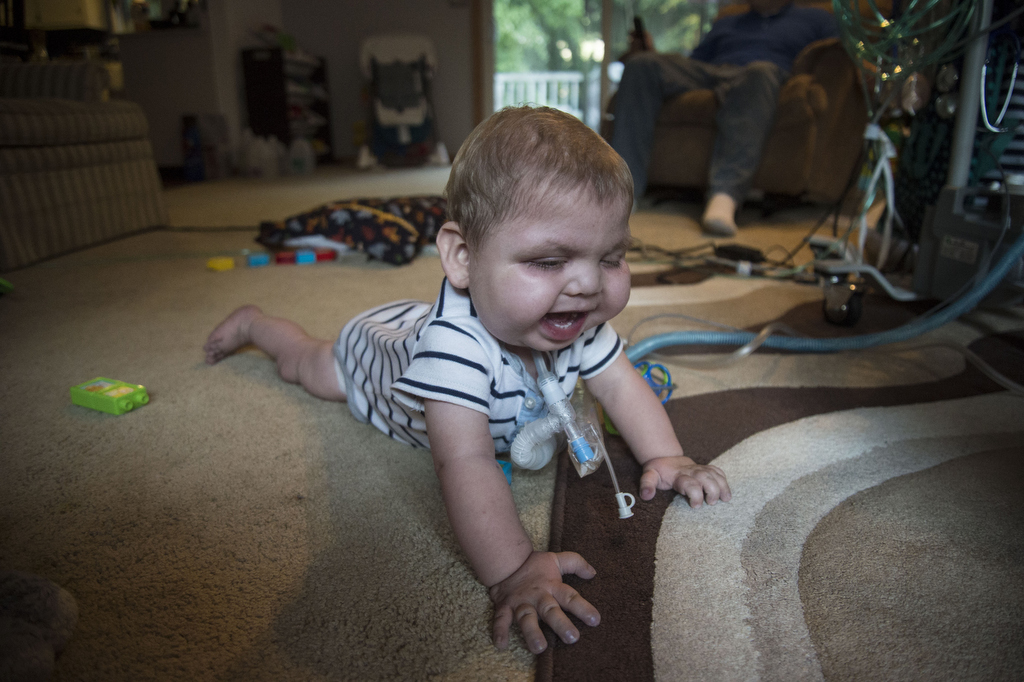
Little Jackson works hard to breathe on his own. He has a tracheotomy that needs constant attention as well as a ventilator and oxygen at home. After more than a half dozen surgeries in his two years on earth, he’ll likely face more as he grows.
But despite the difficulty getting air into Jackson’s tiny lungs, Amanda said the Helen DeVos Children’s Hospital pediatric palliative care team has helped her family breathe easier.
Let’s be clear here: Palliative care is not hospice care.
Although team members do everything they can to make patients comfortable, one of their main missions is to serve as advocates.
“They’re a big stress reliever,” Amanda said of the team members who join her at appointments, both in the hospital and outpatient. “I told them when they entered my life it’s like a weight off my shoulders. I could feel the stress go away.
They have been the medical guides, of sorts, to help the West Olive, Michigan, family on a meandering safari of surgeries, specialist appointments and hospital stays.
For the layperson, it’s a difficult road to travel.
Advocates and assistants
“They’re part of the advocacy for Jackson to make sure everyone is on the same page and that nothing gets dropped or missed,” Amanda said. “They make sure all my questions are getting answered.”
Jackson has about a dozen specialists. It’s difficult to keep track of everything. The palliative care team helps with that, too.
“It’s just stressful,” Amanda said. “I was doing it before palliative care showed up. They try to make it as easy as possible to get Jackson everything he needs. They’re there to help oversee any aspect of his care. I have their phone number and they say I can call anytime.”
That’s comforting for parents of a child whose medical chart matches their last name—miles long.
When Jackson arrived in this world at Spectrum Health Butterworth Hospital on Oct. 15, 2014, doctors already knew he suffered from a congenital heart defect.
But that turned out to be just the beginning.
Little Jackson also had a cleft palate, lung disease and a horseshoe kidney, a condition in which his kidneys grew together to create a single “horseshoe” shape.
After spending his first five days of life in the Helen DeVos Children’s Hospital neonatal intensive care unit, Jackson underwent open heart surgery. The rest of the week was a string of open heart procedures and a heart catheterization.
But that wasn’t the end of the procedure line for little Jackson. Next, up? Acute kidney dialysis, lung biopsy and a tracheotomy.
‘He’s happy all the time’
On the cusp of celebrating his second birthday, life began to ease a bit for the Miles family. Their smiley boy had learned to sit up, communicate a bit, crawl and walk.
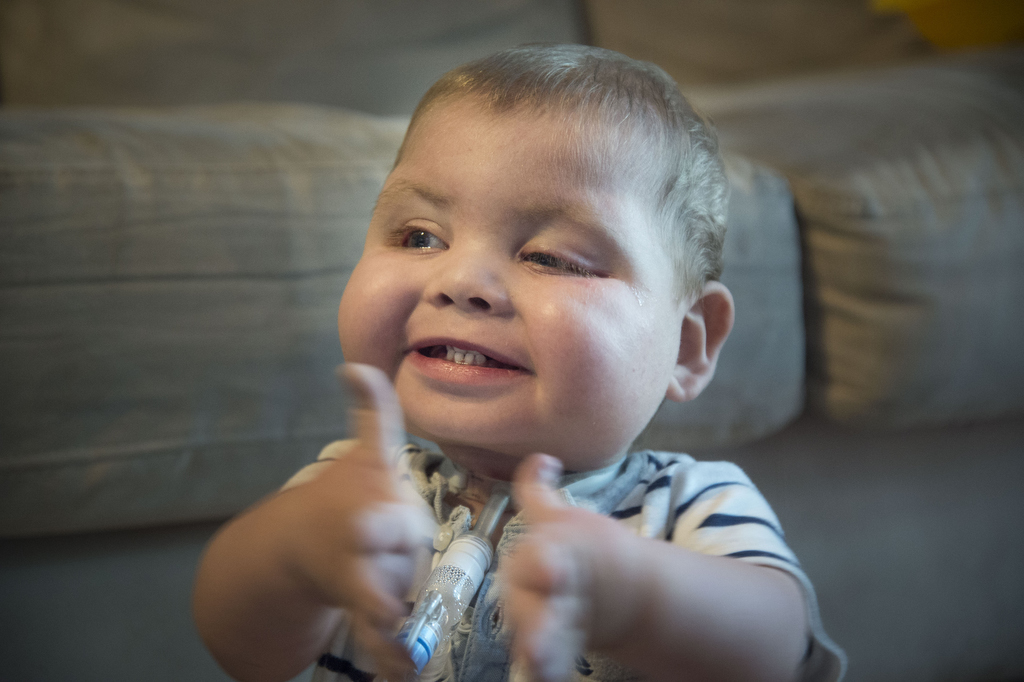
“He’s happy all the time,” Amanda said. “He smiles a ton. He likes to clap for people and give them little side smiles.”
Mom and Dad are smiling a lot more these days, too. Their calendar is free of surgery dates at the moment.
They take Jackson to Helen DeVos Children’s Hospital once a month for steroid treatments to help his lungs. Palliative care team members pop in to see if the family has any questions or if there is anything they can do.
On the ride to and from the hospital, someone always has to be in the back seat with Jackson, to keep his airway clear.
While a majority of their time is spent at home, they enjoy visits from family and close friends. They have learned to enjoy the little things in life. They delight in watching Jackson clap or shake a rattle to the beat of “Wheels on the Bus” or “Itsy Bitsy Spider.”
An extra layer of support
Bradd Hemker, MD, Helen DeVos Children’s Hospital pediatric palliative care and pain specialist, said his team’s role is to control pain, coordinate care between Jackson’s various medical teams and help the family through potentially difficult medical decisions.
“Our goal is to help families we work with focus on giving their child the best quality of life possible, even as they face chronic, complicated medical illness,” Dr. Hemker said.
Even though Jackson has been doing well lately, he said the reality is painfully real.
“Given his underlying diagnosis, he will continue to be at risk for significant complications leading to additional hospitalizations, procedures and surgeries,” Dr. Hemker said.
By getting to know the patients and families well, team members are better equipped to be on the ready when new issues arise.
“Our involvement with Jackson and his family is a great example of long-term palliative care,” Dr. Hemker said. “I believe our involvement is helpful in providing this extra layer of support for some of our most medically complex children.”
He said team members strategically help families navigate “an incredibly confusing medical system” and keep things from falling through the cracks.
In the case of the Miles family, that can lead to a healthier child and happier parents, and bigger cause for celebration in November, which is national pediatric palliative care month.
“We are extremely happy that he has been doing well lately, and certainly hope that continues to be the case,” Dr. Hemker said.

























 /a>
/a>
 /a>
/a>
 /a>
/a>