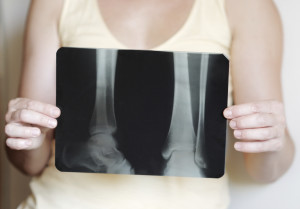
Women prescribed a common class of antidepressants to ease menopausal symptoms may face a long-term rise in their risk for bone fracture, a new study suggests.
The antidepressants in question are selective serotonin reuptake inhibitors (SSRI) medications such as Celexa, Paxil, Prozac and Zoloft.
Besides being used to treat depression, these drugs are often prescribed as an alternative to hormone replacement therapy to tackle hot flashes, night sweats and other problems that can accompany menopause.
However, “SSRIs appear to increase fracture risk among middle-aged women without psychiatric disorders,” wrote a team led by Dr. Matthew Miller of Northeastern University in Boston.
Our Take
Fracture risk in women is a combination of many factors. There are cells in the bone which build it up, and other cells which tear it down; there is constant turnover and remodeling that keeps bones healthy and constantly renewed.
For this process to work, there must be adequate calcium (building blocks) and vitamin D is necessary for the calcium to be absorbed from the gut. The bones also have to know they are needed, and physical activity stimulates bone growth.
Up until 32, a woman is building bone overall, and after 32, she starts to lose it slowly over time, and at menopause the drop is faster because of the loss of estrogen; the drop is much less in women who take estrogen after menopause. SSRIs are being looked at to see if they have a side effect of increasing bone loss.
“The studies are conflicting at best,” said Diana Bitner, MD, an OB/GYN, certified menopause physician and women’s sexual health specialist with Spectrum Health Medical Group. “The medical study quoted in this article looks at insurance claims for fractures in women taking SSRIs. …In older studies, which carefully look at bone mineral density and a bone turnover marker in women on SSRI and not, there is no difference in bone metabolism.”
As a prescriber of SSRIs, Dr. Bitner said she will take this information as a precaution, and perhaps consider alternatives for women who already have many risk factors for bone loss and fragility fractures, multiple medical conditions, or who have inactive lifestyles.
“However, if the SSRI is the best drug for her to feel better and re-engage in life without hot flashes after a breast cancer diagnosis, and the use of the medicine could give back her quality of life, I will continue to prescribe this drug which has helped so many women,” Dr. Bitner said. “But at the same time I will encourage her to take calcium, vitamin D and exercise with strength and balance training.”
The team added that the effect seems to be “sustained over time, suggesting that shorter duration of treatment may decrease [this effect].”
The study authors acknowledged that their work did not establish a direct cause-and-effect link between SSRIs and a boost in fracture risk. However, they point out that prior research has highlighted bone-thinning as a possible side effect of antidepressants.
Findings from the study were published in the journal Injury Prevention.
For the study, researchers sifted through data from the PharMetrics Claims Database, which collects information on drug treatments involving roughly 61 million patients nationally.
In this case, investigators specifically focused on more than 137,000 women between the ages of 40 and 64, all of whom began SSRI treatment at some point between 1998 and 2010.
The SSRIs in question included citalopram (Celexa), escitalopram (Lexapro), fluoxetine (Sarafem, Prozac), fluvoxamine (Luvox), paroxetine (Paxil) and sertraline (Zoloft).
The SSRI group was compared with more than 236,000 other women who had been prescribed indigestion medications instead of an SSRI.
They found that women in the SSRI group faced a 76 percent higher risk for fracture after a single year of SSRI use, compared with the non-SSRI group. That figure fell slightly, to 73 percent after two years and 67 percent after five years, the study said.
One expert in bone health said a relationship between SSRIs and bone weakening does have some basis in biology.
“The authors speculate that the mechanism of action involves the activation of osteoclasts, cells which break down bone, by the SSRIs,” explained Dr. Caroline Messer, an endocrinologist at Lenox Hill Hospital in New York City.
She said that, “While more studies are needed, the trial does suggest that women might want to limit the duration of treatment with SSRIs and perhaps consider taking the lowest effective dose to minimize bone loss.”
 /a>
/a>
 /a>
/a>
 /a>
/a>