
GERD shouldn’t be ignored. Complications could include bleeding, scarring, hiatal hernia, Barrett’s esophagus and even cancer of the esophagus.
But what can you do about it?
Randall Meisner, MD, and David Scheeres, MD, have helped thousands of patients deal with GERD. They agree: If you’re having issues two or more times a week, ask your doctor about stepping up your treatment.
Step 1: Adjust your lifestyle
Prevention, of course, is the best strategy. Changing what you eat, your medications, how you sleep and what you weigh may relieve your symptoms, said Dr. Meisner, a gastroenterologist who helps many patients with GERD and Barrett’s esophagus. But, it’s not always easy.
“Avoiding all heartburn-causing foods religiously isn’t practical. Chances are some of your favorites are probably on that list,” Dr. Meisner said. “Instead, identify and avoid the specific foods that make you feel the worst.”
More advice: “Forget the notion of eating something to coat your stomach before going to bed,” Dr. Meisner said. “It’s sure to backfire when you lie down and acid flows easily from your stomach into your esophagus.”
Another tip: Use bricks or boards to prop up the head end of your bed 6 to 8 inches. Keeping your head elevated puts gravity to work, keeping acid in your stomach where it belongs.
If you’re obese, with a body mass index higher than 30, you’re three times more likely to have GERD symptoms than other people. The obvious (but never easy) solution is to lose weight.
Step 2: Find the right medication
Just walk down the aisle of your pharmacy, watch TV or go online and you’ll be bombarded with information about medications to help your symptoms. In fact, about 80 percent of people can control their GERD symptoms with the lifestyle changes outlined above or using medication.
What are these medications? How do they work?
- Antacids. Rolaids, Maalox, Gaviscon and other antacids are good for treating minor symptoms as they occur. They neutralize existing acid in your stomach, and they may also relieve constipation and diarrhea. For best results, take them after meals and at bedtime.
- Histamine blockers. Zantac, Tagamet, Pepcid and Axid are helpful for treating mild to moderate symptoms. You can also combine them with an antacid. Histamine blockers prevent your stomach lining from making too much acid. Try them at bedtime for best results.
- Proton pump inhibitors. Prilosec, Prevacid, Aciphex and Nexium are a good choice if histamine blockers aren’t helping you. These block the acid-producing enzyme in the wall of your stomach. This not only prevents symptoms, it also lets your esophagus heal. Be sure to take proton pump inhibitors 30 to 60 minutes before eating.
- Prokinetic agents make food move more quickly through your digestive system. Although they were effective, they caused heart problems so are rarely used today, Dr. Meisner said.
If over-the-counter medications aren’t working, your doctor may be able to prescribe higher doses for more effective treatment.
Still having symptoms twice a week or more despite trying a variety of medications?
Step 3: Consider surgery
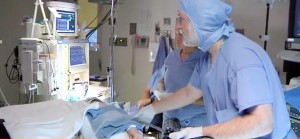
“If medicine doesn’t completely control your symptoms, or if you want a permanent solution, surgery may be your best choice,” said Dr. Scheeres, a surgeon who specializes in laparoscopic surgery and gastrointestinal endoscopy.
Good news: Laparoscopic surgeries don’t require a large incision. This means a quicker recovery than you might expect. Options include:
- TIF (transoral incisionless fundoplication). With TIF, the doctor rebuilds the connection between your stomach and your esophagus by fastening the bottom of the esophagus down into the stomach. “You’ll go home from the hospital in less than 24 hours with little pain except for a sore throat,” Dr. Scheeres said. “In less than a month, you’re usually off your medications and back to a regular diet.”
- LINX Reflux Management System. This procedure uses little magnetic beads to create a “bracelet” that acts as a barrier between the stomach and esophagus. The system allows food to go down into the stomach, but prevents acid from backing up into the esophagus. The LINX system is the only FDA-approved device to treat GERD and stop reflux.
- Laparoscopic Nissen fundoplication. This is the most common surgery for patients with severe GERD. It wraps the upper part of the stomach around the esophagus to prevent acid from backing up into the esphagus. You’ll need to stay in the hospital overnight, and right after surgery you’ll have some restrictions on what you can eat. Gradually, over the course of a month or two, you’ll be able to go back to eating regular food.
Research shows that 90 percent of patients who have laparoscopic anti-reflux surgery are symptom-free after 10 years. Only a small percentage need to take medication for their symptoms.

“We love to travel, but food was always a problem,” Erichson said. “I’ve been curled up in some of the finest places in the world in pain.”
Social events were also a problem because GERD made her voice very weak.
After surgery?
“I get energy from food instead of pain,” Erichson said. “I really am noticing a difference.”
 /a>
/a>
 /a>
/a>
 /a>
/a>