Alexis Gering had been through childbirth three times before, so she knew what to expect.
But her fourth child brought the unexpected.
On Nov. 6, 2015, Alexis attended a routine appointment with her obstetrician in her hometown of Sturgis, Michigan.
“I had three kids with no issues,” she said. “The doctor did a mini ultrasound and said it looks like I’m going to have a 7 pound, 5 ounce baby.”
Her due date passed, and her doctors decided to induce. But during the process, monitors alerted everyone in the room—baby in distress.
Doctors suspected the umbilical cord may be wrapped around the baby’s shoulder and neck, and they prepared for an emergency cesarean section.
Alexis and her husband, Jacob, prayed. Hard.
“When he came out, I heard crying for what felt like a second then it stopped and everything went into panic mode,” Alexis said. “That’s when I started losing it. I asked, ‘What’s going on, can someone tell me something?’”
But unfortunately, answers were few.
“They didn’t show me the baby, they just left the room with him,” she said. “I’m just lying there trying to figure out what’s going on. Jake came back and said, ‘He’s really, really small. He’s tiny, 3 pounds, 12 ounces.’”
Jake and Alexis later learned that when Mikah took his first breath, he inhaled meconium, and stopped breathing.
“He was crying when he came out, but then he breathed it all in,” Alexis said.
Staff transported Mikah to a Kalamazoo hospital.
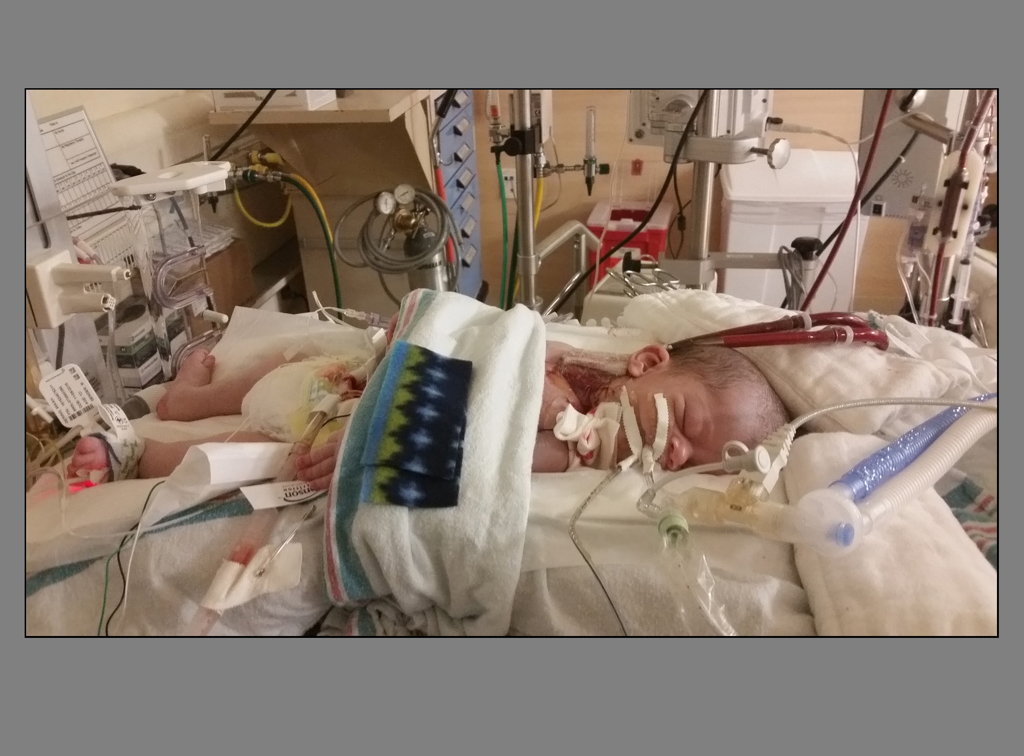
“He was so tiny,” Alexis remembers about seeing Mikah for the first time. “I thought, ‘How on earth did this happen?’ His lungs were so tiny they couldn’t tolerate the meconium aspiration. His lungs were collapsing.”
‘We don’t know’
Doctors expressed the gravity of Mikah’s condition, words no parents ever wants to hear: “We don’t know if he’s going to make it.”
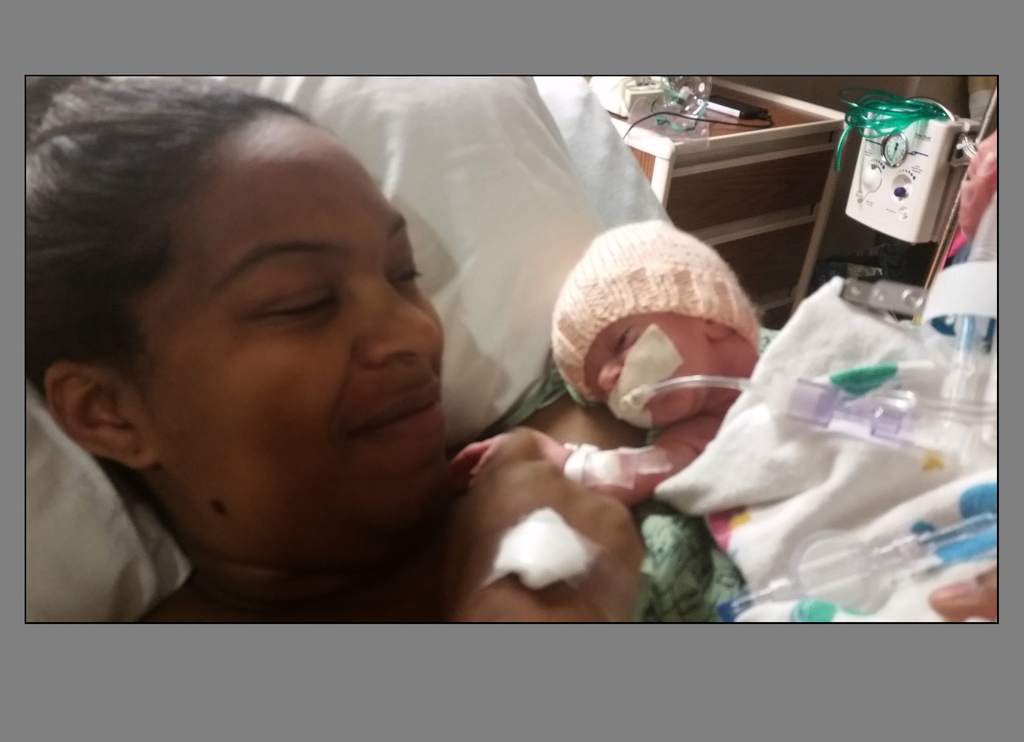
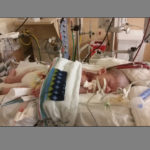
They let Alexis hold her newborn son. She, and they, thought the first time may be the last time.
“We took a couple of pictures because we didn’t know,” she said. “The next day he was still alive.”
Doctors wanted to transfer Mikah to a hospital with ECMO service, a machine that provides cardiac and respiratory support to sustain life.
A hospital on the east side of the state refused to take Mikah because of his size.
“Spectrum Health said, ‘Yes, we’re going to try our hardest, but we don’t know if he will make it because he is so small,’” Alexis said.
A Spectrum Health Aero Med helicopter transported Mikah to Helen DeVos Children Hospital in Grand Rapids.
“It was a roller coaster,” she said. “You think it’s going to be OK, then you think it’s not.”
The couple signed paperwork to have their little boy hooked up to an ECMO machine, acknowledging the risk, which soon became reality.
Jacob had to leave for work, so Alexis and her mom waited for updates on fragile little Mikah. Unfortunately, they heard words that numbed their souls.
“‘I’m so sorry, I think this is it,’” Alexis recalled a staff member gently telling them. “She asked for our presence in the room and said, ‘I think he’s about to make his transition’ (into the afterlife).”
She and her mom ran to the room to be with Mikah. Emotions exploded. Hearts pounded.
Crying, Alexis took a moment in the waiting room.
“I dropped down to the ground and just yelled out,” she said. “I just yelled out to the Lord, ‘Please, whatever you do, please save my child.’” I was crying.”
Alexis’ mom found her in the waiting room and delivered a message of miracles. She told Alexis everything was hooked up to the machine and all appeared to be fine.
“That was the turning point in the whole thing,” Alexis said. “I felt release in that moment.”
But it wasn’t over. A few days later, Mikah developed the complication everyone had feared. An ultrasound showed signs of bleeding in the brain.
Risks and rewards
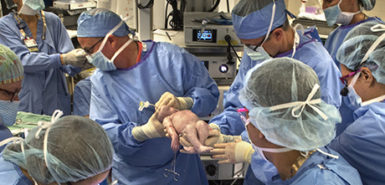
Emily Durkin, MD, medical director of pediatric surgery at Helen DeVos Children’s Hospital, said Mikah is the smallest patient to ever go on ECMO at the children’s hospital, and probably one of the smallest in the world. With tininess comes big risk.
“When he got here he was very, very sick,” Dr. Durkin said. “I had a real upfront conversation with his dad: ‘If we don’t do this, we know he’s going to die. If we do do this, he may die as a result of us doing it, but at least we’ve tried.’”
The ECMO machine is not set up for such tiny humans. The team had to rebuild the ECMO circuit and adjust settings to get to a flow rate that would be safe for Mikah.
“He did remarkably well,” Dr. Durkin said. “He had some bleeding in his brain—that’s the complication we fear. But he’s alive today because we did this.”
Mikah was discharged from the hospital a month later, with an unknown future.
“They removed the feeding tube and we got the OK to go home,” Alexis said. “We were happy to have him home. We were loving on him. We brought him home and just did the family thing.”
They drove Mikah to Helen DeVos Children’s Hospital every couple of weeks for appointments. Eventually, staff told the family they could transition follow-up appointments to Kalamazoo to be closer to home, but Alexis and Jacob wanted to continue the trek to Grand Rapids.
“I had so much faith in the staff,” she said. “We told them we wanted to go to Grand Rapids because we trust you guys.”
Mikah continued to grow and thrive. Doctors diagnosed him with cerebral palsy at age 1.
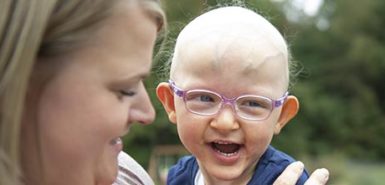
“He gets around and does really well,” Alexis said. “You really wouldn’t know, because it’s really mild. We’ve just seen some great growth over time.”
Despite slight weakness on his right side, Mikah has full use of his hands. Cognitively, the almost-3-year-old is doing great and starting to speak in complete sentences.
“He’s blossoming,” Alexis said. “He’s really doing wonderful things.”
Jacob agreed.
“He’s up and at it,” he said. “You would be hard to tell anything had ever happened to him.
“He’s doing leaps and bounds at therapy. He went through so many different things. We pretty much signed his life over three different times. God is a big part of our lives and we trust He’s a big part of that. We are very, very thankful. It’s been a blessing to watch him grow.”
Mikah loves basketball, swimming in the backyard pool, riding scooters, swinging and jumping on trampolines.
“We don’t really have to make any real exceptions for Mikah,” Jacob said. “In all honesty, I never would have thought he would be able to do as much as he’s doing. He’s pretty much broken all the rules.”
At one point, during a Facebook prayer chain for Mikah, more than 1,300 people in seven countries prayed for Mikah at the same time.
“Even the doctors say they can’t believe he’s progressed so well,” Jacob said. “It’s an answer to a lot of prayers.”
Dr. Durkin said she’s pleased with Mikah’s progress.
“I just felt he deserved a chance,” Dr. Durkin said. “I think his prognosis is great. He’s alive today because of the ECMO he got. He very much would have died if he hadn’t had it. He’s a joy to his family. They love him and are grateful for him being part of their family.”





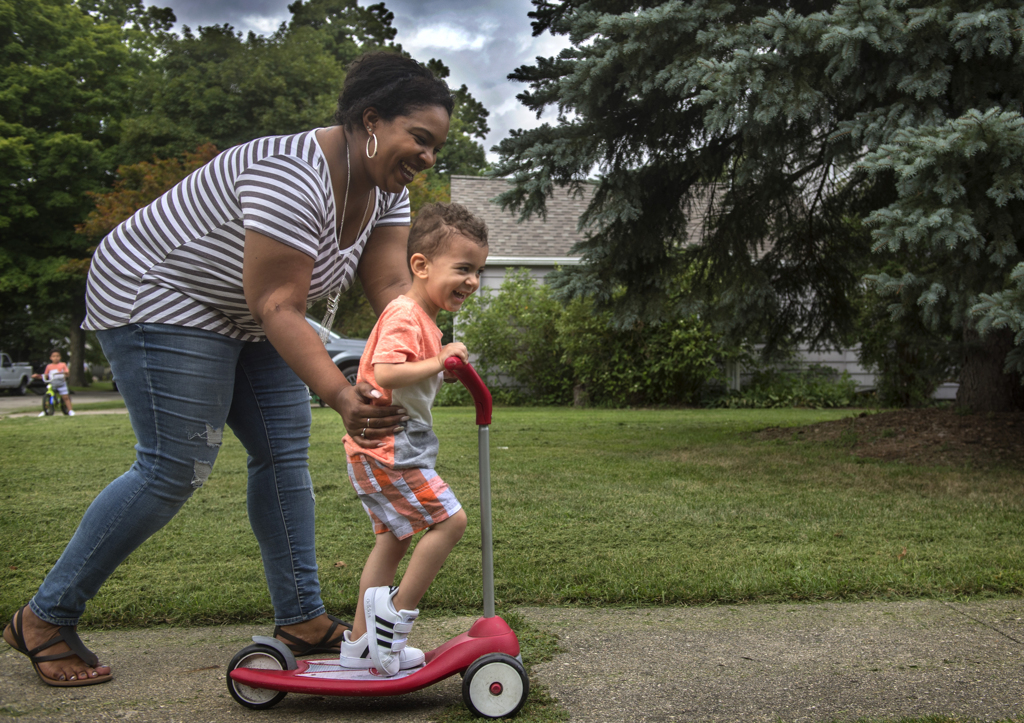












 /a>
/a>
 /a>
/a>
 /a>
/a>
My daughter had ECMO in November of 1994.She was the 219 person to ever have it.Riley Childrens Hospital in Indianapolis Indiana did a wonderful job.She is now 23 yrs old and you would never know she had such a rough start.
Thank you, Christina, for sharing. So glad your daughter is doing so well. Cheers, Cheryl
Praise God for the amazing miracle of Mikah! He certainly does answer prayer!
My son was on Ecmo for 36 days in 1995 he weighed 3 lbs 10oz at birth. He is now a 164 lbs 6 ft 4 22 year old man, I was told the same thing when he was put on the machine and I thank God everyday that I made the choice I did. Childens Hospital in Detroit saved my baby noys life and I will be eternally grateful for them. Never give up when it comes to your childs life, there is always hope ❤
Thank you for sharing, Katherine, and for your encouraging comment! Cheers to you and your son!
Yes, we do love him, and we are extremely grateful to have him as such a precious member of our family.