Leanne Parker won’t soon forget the two most frightening moments of her life—the night she first witnessed an epileptic seizure in her daughter Lily, then age 4, and the day Lily underwent brain surgery, two years later, to make the seizures stop.
“I used to be somebody who had everything in control. And when epilepsy came into our life, I realized we had no control over that—and that was really, really hard,” Parker said.
“It was the scariest thing of my life.”
Throughout the turbulent months between Lily’s 2017 epilepsy diagnosis and her 2019 surgery to remove a portion of her brain, her mother learned the importance of trust and optimism.
And young Lily became her guide.
“With all of our visits and our stays at (Spectrum Health Helen DeVos Children’s Hospital), Lily loved every moment of it. And that brought so much peace to me as a mother,” Parker said.
“She always wanted to go back, so when I booked appointments, it was like, ‘Oh, yay!’”
And when surgery emerged as the best treatment option, Lily led the way.
“She was so positive. She talked about it like it really was no big deal,” Parker said.
“You know—‘I’m in good hands. This is going to be OK, because I trust my mom and I trust my doctors and I trust the team. And they’ve all been there taking care of me, so let’s do this.’”
Drug-resistant epilepsy
In the beginning, Lily’s seizures happened roughly once a month, usually at night.
Over time, they increased in frequency to every two weeks.
Each one left her “in a fog,” said Lily’s pediatric neurologist, Angel Hernandez, MD.
Dr. Hernandez tried a succession of anti-seizure medications with Lily, but each one failed to control her seizures. Her diagnosis changed to intractable, or drug-resistant, epilepsy.
“None of the meds worked and she started building up a tolerance to the rescue med that would stop the seizures,” Parker said. “I felt like I was running out of time.”
As the months passed, the risks to Lily’s long-term health increased. Unchecked seizure activity can spread to other parts of the brain and lead to developmental disabilities, Dr. Hernandez said.
To learn whether surgery could be a viable treatment option for Lily, the pediatric epilepsy team worked to identify the source of her seizures.
This meant repeated admissions to Helen DeVos Children’s Hospital for assessments and testing.
“We have to go through a process that typically requires admission to the hospital for a minimum of five days, during which we remove medications, provoke seizures and do imaging studies to help clarify where seizures are coming from,” Dr. Hernandez said.
The process proved stressful for Parker, who had a second daughter at home in Muskegon, Michigan, 40 miles away from the hospital in Grand Rapids.
But the Child Life Services staff brought smiles and fun—sometimes even therapy dogs—with every visit to Lily’s bedside.
And the epilepsy team brought diligence and clear communication.
“I really appreciated that Dr. Hernandez is a very straightforward person,” Parker said. “You want all the cards on the table, and he definitely gave that to us. I just think that he’s the best.”
MRI studies showed that Lily had an abnormality on her occipital lobe—the smallest of the brain’s four lobes, situated at the back of the head.
Dr. Hernandez identified this congenital malformation as the cause of Lily’s seizures. He believed removing this part of the brain could stop her seizure activity.
But surgery would come with a downside: Because the occipital lobe helps the brain process visual information, removing all or part of the lobe would damage Lily’s peripheral visual field.
With the clock ticking, the family met with Casey Madura, MD, a pediatric neurosurgeon, to learn more about the procedure.
Occipital lobectomy
Relying on the epilepsy team’s extensive testing data, Dr. Madura recommended moving forward with an occipital lobectomy, the surgical removal of the occipital lobe.
This procedure is standard but uncommon, Dr. Madura said, because epilepsies stemming from the occipital lobe are relatively rare.
Dr. Madura offered to perform the lobectomy, despite the visual impairment it would cause, because if it worked—a likelihood he put at 60%—the trade-off would be worth it.
“Typically patients will tolerate a new deficit like that if it means that their seizures are gone,” he said. The effects of repeated seizures over time would be “far worse.”
After their meeting with Dr. Madura, the family decided to go ahead with the lobectomy.
Four weeks later, on surgery day, Parker watched her daughter skip through the hospital doors.
“Lily went into that surgery with the best mindset. It’s like, ‘We’re going to do this; it’s going to be fine.’”
The young patient’s prediction came true.
Dr. Madura performed the surgery on a Thursday, and Lily went home that weekend. Two weeks later, she returned to school—no big deal.
Dr. Madura’s thoughtful approach reinforced Lily’s attitude, Parker said. During pre-op, he braided and clipped back her hair, minimizing the area to be shaved.
“You could barely even tell that any of her hair was shaved—which I just think is amazing,” Parker said.
The surgeon also used unobtrusive bandages to protect Lily’s incisions.
“He’s like, ‘If we don’t wrap her head, then things seem a little bit better than (if) we treat her as if there’s something seriously wrong,’” Parker said.
“It was the most amazing experience.”
The best outcome
The best part of Lily’s story, of course, is her successful outcome.
As Dr. Hernandez gradually weaned her off epilepsy medications, the seizures remained at bay.
April 2021 marked two years free of seizures, with no medications. And all signs point to this trend continuing.
“Making it this far out without a seizure is a pretty good indication that she has a very good chance to live a life without seizures,” Dr. Madura said.
“That really is what matters—that Lily has gotten the best outcome that we could have hoped for.”
Lily’s positive results include her eyesight. Though she did lose her right-side visual fields, she adjusted easily. Now, at age 8, she plays basketball and baseball at the local YMCA as if nothing happened.
“I thought that was going to be another mountain that we were going to have to climb, and it wasn’t,” Parker said. Instead, Lily has “flourished and gained by leaps and bounds.”
For Parker, it’s all been a lesson in holding onto hope. She counsels parents facing similar situations “to trust the process, to trust your doctors and to lean into them.”
Though it’s hard, “it can be so amazing on the other side.”

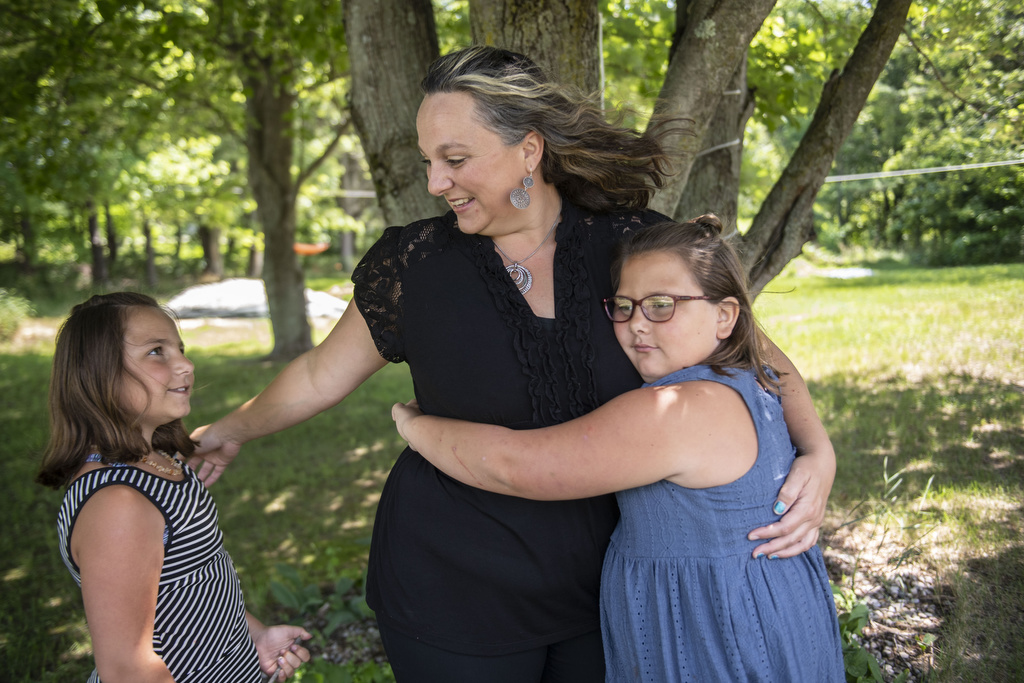

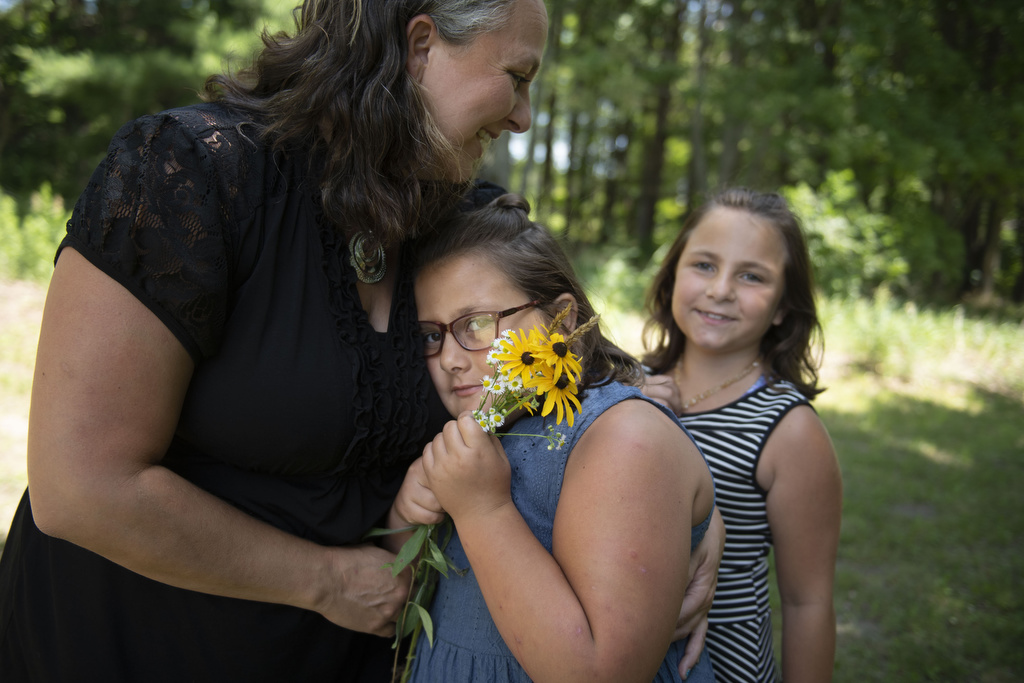








 /a>
/a>
 /a>
/a>
 /a>
/a>
What a beautiful story. My sister is a patient of Dr. Madura’s, and he has been amazing throughout our journey with her. We met him 4 years ago, and he has been an integral part of her journey and care all this time. An absolutely wonderful physician and person. So great to hear your story and see how well you have done since your procedure.
Thank you for your kind comment, Jana! We’re so glad to hear this. All the best to you.