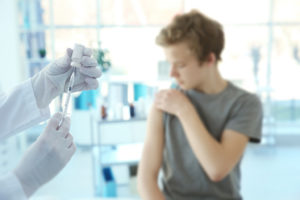
In a finding that might make the HPV vaccine more palatable to many, new research suggests a single dose may provide just as much protection from cervical cancer as the recommended two to three doses do.
“The vaccine is extremely effective and can prevent over 90% of nearly 35,000 cancers caused by HPV every year among men and women,” explained study author Ashish Deshmukh.
He’s an assistant professor with the Center for Health Services Research at the University of Texas Health School of Public Health in Houston.
“And we found that (American) women who received only one dose of HPV vaccine have gained similar benefits to those who received two or three doses,” Deshmukh added.
First introduced in 2006, the multi-dose human papillomavirus vaccine can prevent most cervical and anal cancers among children and young adults exposed to the virus.
It can also prevent the majority of both HPV-driven oral and penile cancers.
Yet vaccine coverage has remained low.
In the United States, vaccination rates hover at about 50%. And in developing nations—where the per-dosage cost of $4.50 is often out of reach—rates are a dismal 10%, the researchers said.
One obstacle is the stigma around a vaccine linked to sexual activity among youth.
Another is that many people remain unaware that HPV can cause cancer.
And then there’s the hassle and expense of the recommended two- or three-dose regimen.
But if a one-and-done vaccine could achieve the same goal, much of that last hurdle could be eliminated, the study team noted.
“We were surprised by the extent of the benefits,” said Deshmukh, whose team’s conclusion followed an analysis of HPV vaccination and diagnosis data on more than 1,600 women between the ages of 18 and 26.
All the women were participants in the U.S. National Health and Nutritional Examination Survey between 2009 and 2016. Nearly two-thirds had not been vaccinated at all. Just over 100 had been inoculated just once. About 125 had received two doses, and nearly 400 had received three.
Current vaccine guidelines advise getting vaccinated beginning at age 11 or 12 up to age 27. Those vaccinated before 15 are supposed to get a second dose six to 12 months later.
Patients with weak immune systems and/or those whose first dose is administered between 15 and 26 are advised to get three inoculations, with a second dose 30 to 60 days after the first, and a third dose at six months.
The researchers confirmed that HPV infections were “significantly less prevalent” among those exposed to at least one vaccine dose.
But there was also “no significant difference” in HPV infection risk between those who had taken one, two or three doses.
So does this definitively mean that one HPV vaccine dose is sufficient? No, Deshmukh said.
For one, his team pointed out that vaccine history was entirely self-reported by survey participants—which is less reliable than medical records—and male patients were not included in the survey.
And the team did not track dosage timing or HPV infection histories.
“(So), we believe that our findings are still early,” Deshmukh said. “To change vaccination guidelines to a one-dose schedule, we need conclusive evidence from clinical trials.”
Such a trial is now underway in both the United States and Costa Rica, he said.
That larger study “will give us a conclusive answer” as to the reliability of a one-dose protocol, says Debbie Saslow, managing director of HPV & GYN Cancers with the American Cancer Society in Atlanta. She was not part of the study.
But Saslow expressed little surprise that one dose appears to do the trick.
“However, it probably won’t be quite as effective as two doses,” she said. But cost, she stressed, is likely the biggest vaccination barrier in developing countries. “And so it is likely that in the U.S. we will continue to recommend two doses, but in lower-income countries one dose will be recommended.”
Regardless, Saslow has a clear message for parents: Eventually nearly everyone is exposed to HPV—and the HPV vaccine “is one of the most effective vaccines in existence.”
She urged Americans to take advantage of a simple, safe and insurance-covered means of protection.
“With the HPV vaccine, we only have to get our children vaccinated with two shots and then they are protected for the rest of their life,” Saslow said.
The study, which was funded by the U.S. National Cancer Institute, was published in a recent issue of the journal JAMA Open Network.
 /a>
/a>
 /a>
/a>
 /a>
/a>