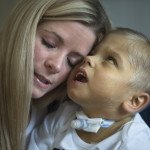
Musical nursery rhymes and Disney tunes softly play as 3-year-old Ethan DeHoek cuddles with his mom in the den of their Grand Rapids, Michigan, home.
Outside, a squirrel bounds through freshly-fallen snow in a backyard where Ethan will never play.
As mom and Ethan cuddle, snowflakes gather upon a basketball hoop next to the driveway where Ethan will never dribble.
The mound of snow pushed to the side of their driveway that’s the perfect incline for sledding? Ethan will never slide down it.
Ethan is dying.
No one knows when the hour will arrive. It could be weeks, months, longer even, if fate smiles upon this beautiful little blue-eyed boy who so easily smiles back.
“It’s a small world after all,” mom Lindsey DeHoek sings along to the CD as she rocks the little boy in her arms.
Ethan can’t see her. He’s blind. To him, mom is shape, a shadow at best, but for certain, a familiar warm and enveloping hug.
It’s a time of laughter, a time of tears…
Ethan was born prematurely at 28 weeks with severe complications.
“Anything bad that could happen, happened,” Lindsey said.
Little Ethan’s stomach perforated, he has no bowels. He has brain damage.
Sometimes I bawl my eyes out. …He has a lot of issues, but he’s very loved.
The world that we all might wish for him is so different from what he is living.
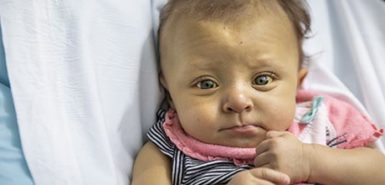
He is fed through a central line in his chest. He breathes through a tracheotomy in his throat. His stomach contents empty into a small bag at his side.
His liver is weak, his skin jaundiced, the whites of his eyes miniature pallets with shades of yellow.
Lindsey tickles Ethan. She recites silly lines that make him laugh.
Despite a prognosis that turns any nursery rhyme into tears, Ethan DeHoek smiles. He clutches his mom’s right hand. His mom clutches back, knowing this is a moment to treasure, to file away for a day when Ethan is no longer among us.
They all are.
“He’s in liver failure,” Lindsey said. “He’s terminal. The only way he could survive is by a multi-organ transplant—large intestine, small intestine, liver and pancreas.”
Last summer, after seeking several medical opinions—and learning the outcome may not be what they would wish for—Lindsey and her husband, Brian, made a decision to not put their little angel through any more rigorous medical procedures, in essence, a decision to let him go.
“At first we thought, we’re going to do (a transplant),” Lindsey recalled. “Then we really thought about it and watched his progress and thought, how fair was that to Ethan? Even though we want him here, that’s how I always look at it—what’s in his best interest?”
Lindsey cries about that decision most every day. But as a mother, would it hurt her heart more to let him go, or hurt her heart more to watch him suffer?
There is no good answer.
“We decided not to put him through that because his quality of life wouldn’t be any better,” Lindsey said. “We’re firm believers in quality of life. My faith is what gets me through each day because I know he is not going to get better.”
A realistic outlook, with palliative care
Lindsey and Brian are realistic. That’s why they so much appreciate Spectrum Health Helen DeVos Children’s Hospital pediatric palliative care and pain specialist Bradd Hemker, MD.
Dr. Hemker and his team assisted 123 families in the past year, families going through difficult times like the DeHoeks. He visits family homes. Attends doctor appointments with the young patients and their families. Offers advice. And a shoulder to cry on.
“We have to think outside the box and make these patients’ lives as good as possible, knowing their lives are going to be shortened,” Dr. Hemker said. “As challenging as it is to have these conversations, they need to be had.”
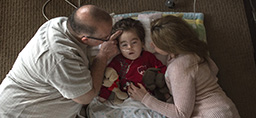
Dr. Hemker visits Lindsey and Brian in the family den on this snowy, winter day. Dressed in a brown suit coat and copper-color tie, Dr. Hemker sits on the floor next to Ethan and his mom.
“You look awful cute,” Dr. Hemker tells Ethan.
Lindsey fills Dr. Hemker in on Ethan’s recent fussiness. They determine he may be in pain.
“Let’s make sure there’s nothing going on, but let’s treat it like pain,” Dr. Hemker says. “Our goal here, obviously, is that he’s as comfortable as possible.”
Dr. Hemker hits the reality head on. We don’t know how long Ethan will be among us. His liver could take him. He could get an infection.
“The bilirubin number (a liver function indicator) is the No. 1 issue,” Dr. Hemker tells Lindsey. “The other part of this is he could have other complications—a line infection, he’s certainly at risk for pneumonia, he could aspirate. The big picture issue is, will one of those things happen or will a liver issue happen first? Unfortunately, that’s the uncertainty you guys are living in.”
Lindsey praises Dr. Hemker for explaining the reality. So many others want to gloss over the expected outcome, and try to wish him out of this.
“I give you a ton of credit for the way you’re handling this,” Dr. Hemker tells Lindsey. “We’re hopeful right there with you that the end will be a long time from now. You’re preparing for it as much as you can but focusing on what you can do to make his life as comfortable as possible, and that may mean making his life as normal as possible, just being a family.”
A delivery person at the door interrupts the moment. He drops mounds of medicine inside the door—Ethan’s liquid nutrition, enough for a week, according to Lindsey.
Dr. Hemker asks if he can hold Ethan.
“I could hang out like this for a while, buddy,” he tells his little patient, who is 3 in age but more like 18 months in size.
Many questions, few answers
Lindsey poses the ultimate question, one she wants to ask her spiritual counselor at church.
“Why do things happen like this?” she asks through tears. “He’s just the sweetest thing in the world. I know I will probably never know until I go to heaven.”
We have to think outside the box and make these patients’ lives as good as possible, knowing their lives are going to be shortened. As challenging as it is to have these conversations, they need to be had.
Dr. Hemker doesn’t have the answer. He tells her medicine doesn’t have the answer, either.
“I always tell families that I think someday it will be clear, after this is done and maybe years from now, after you’ve been able to share with other families,” Dr. Hemker says. “I work with families like yours that are inspiring to all of us. I think we can learn a lot from our patients and families more than the other way around.”
Ethan’s labored breathing interrupts the moment. Lindsey grabs a suction machine and puts a small tube into Ethan’s trach.
As she suctions, she tells Dr. Hemker how when some people hear Ethan is in palliative care, they automatically think hospice.
Dr. Hemker clarifies that hospice is for patients with an expected six months or less to live. Palliative care is about managing pain, and making patients comfortable, for months or years.
“Skinnamarinky dinky dink, skinnamarinky do, I love you,” is playing in the background. Ethan tilts his head back and smiles.
If only the situation were this silly and light-hearted.
“How can we help with the situation the best we can, knowing we can’t fix everything?” Dr. Hemker asks Lindsey. “We have to do everything we can to make him as comfortable as possible.”
As Ethan’s breathing again becomes gurgly, Lindsey suctions again.
The song continues: “I love you in the morning and in the afternoon, I love you in the evening, underneath the moon.”
Lindsey squeezes then grasps Ethan’s right hand.
“It’s not about the death and dying part,” Dr. Hemker continues. “It’s about living with a serious illness. He looks happier than when I saw him in clinic. This is why I like home visits.”
The other side of the mountain
It’s not the first time Dr. Hemker has been to the house to check on Ethan. Dr. Hemker and the pediatric palliative care staff also attend doctor appointments with Ethan and his family.
“Who comes to your house to talk for two hours?” Lindsey asks. “We were just blown away by him. Dr. Hemker has made us feel so good about our decision. He talked us through everything. If we didn’t have him I think I’d be very depressed. He’s a blessing.”
Ethan’s eyelids start drooping. He’s looking tired.
“The Other Side of the Mountain” serenades from the speakers.
It’s a place Ethan will travel someday, with love and heart strings reaching back to this side, and precious times with his family, times like right now.
The moments are fleeting for sure. Lindsey knows this. Brian knows this. Perhaps even little Ethan knows this as he looks upward and smiles in the direction of his mom.
Lindsey scoops up her beloved boy and cuddles him on the couch. A stream of light from the window illuminates the love.
“Sometimes I bawl my eyes out,” Lindsey says. “We know he is going to pass. We know we’ve done everything possible for him. He has a lot of issues, but he’s very loved.”
As “It’s a Small World” reprises, Lindsey, too, looks upward, toward the light.
“He’s our world,” she says.



















 /a>
/a>
 /a>
/a>
 /a>
/a>
Lindsey & Brian, You are strong. You are brave. What courage and strength it took for you to make such a decision for your son! No one can put a measure on the quality you are adding to his life. I pray God will comfort you and keep you, your son, and your marriage in His mighty hands.
What a heartbreaking story, and what courageous parents little Ethan has. God bless you all.
Praying for him to not be in pain. Jesus will hold him and his family during this hard time.
What love & faith you both have.God bless you all.
Thank You for your story and God Bless ALL of you!!
So glad to know Lindsey, Brian and Ethan as well as the rest of their family have the support of such a carrying doctor and program. Our thoughts and prayers are with them all.
Lindsey and Brian you are such wonderful courageous parents. Stay strong in your faith,God be with your family at this very difficult time.
What a beautiful story Marie! A real tearjerker. Cannot imagine their emotional rollercoaster. Sweet, sweet boy.
To anyone reading this article, who has a TPN dependent child, please look into omegaven! It’s an intravenous fish oil lipid being used to reverse liver damage and protect the liver, with amazing success! It is not FDA approved, so it’s only available at certain hospitals. But it offers an alternative to transplant, and gives these kids an opportunity to grow!
To Lindsay and Brian- I’m so sorry for all you’ve been through. I’m sorry this treatment wasn’t made available to you, when it could’ve helped Ethan. I’m sorry for Ethan. My son, Dominic, is two years old and 100% TPN dependent. He has 10cm of small bowel, due to a one in a million variation of Hirschsprung’s disease. I have read, for hours, about transplant and it is such a poor option, in my opinion. I respect you for making the best decision for Ethan. And I can only imagine the weight that decision must hold. Sending you love and prayers for peace and acceptance.
Thank you for sharing your little Ethan with us. Your strength is remarkable. Ethan is a gift from God no doubt. Continue to cherish ever moment. Prayers for your family and the team of doctors and nurses that have gotten you through this thus far. <3
I have been a pediatric nurse for over 20 years. I know this sweet little boy, Ethan, and his loving parents, Brian and Lindsey. I had the wonderful opportunity to take care of Ethan in his home for two years. He has an infectious smile, and though he is blind, his little face lights up when his older brother, Parker, comes in the room. Ethan loves to be held, especially by his Mom. It’s hard not to fall in love with Ethan, and his very loving family. They are extraordinary! The love and devotion they give to Ethan everyday is never ending. Their lives revolve around Ethan and his needs. They set the bar very high in being the most devoted and loving parents of a child with special needs. I am not sure who has been blessed more, Ethan, for having the most caring and devoted family to love him; or, Brian, Lindsey, and Parker, for having such a special, sweet little boy placed in their care. I will always cherish my time spent with this family. They have shown me what true devotion and selflessness really is!
Lindsay and Brian, you are absolutely wonderful parents, and astoundingly wonderful people. Your faith is amazing! ( I am friends with your cousins, Sarah and Heather 🙂 You are a true inspiration to so many reading this. This is absolutely heart-breaking, reading and hearing about what you are going through with Ethan. I am so very sorry. It does not seem fair that such a sweet precious little person has to go through all of this. Thank you for sharing all of your story. You are in my thoughts and prayers.
So many things are hard to understand, but someday in Heavens light we will see clearly. Prayers for you and yours.
When I was a teenager, I worked in a facility that had severely profoundly handicapped and deemed “retarded,” children. Our census hovered around one hundred children. Many of the caregivers were adults who were disabled too. I had so many children like your precious Ethan. I’d sleep under their crib all night, holding just a little finger extended through the rails. I remember Kimmy and Gerry; they were both seven years old and were dying. They were best friends, always reaching to each other. As one died, the other–though completely non-verbal–experienced deep, incapacitating grief. I could share hundreds of stories, but I’d like you to know that love is love. Why can’t we live this passionately and gently and jubilantly every moment, every day? I’m now an old hospice nurse, and reflect on “my” babies and their families every day. Thank you for living life passionately, loving deeply and for simply keeping us enlightened.
My thoughts & prayers are with Ethan & his entire family. So glad you have Dr. Hemker & the pediatric palliative care staff. You have many blessings. God be with all of you.
Ethan and family….your story is so inspiring. I’m so overwhelmed with the closeness you all share each and every day! Keep smiling. God bless.