There’s something of a time machine on the lower level of 2902 Bradford St. NE in Grand Rapids.
Check your skepticism at the door, then head on in and plop yourself down on one of the two beds that await.
Lean back and get ready. You’ll be sent back a good 10 years or so, to that special time before all of humanity buried its collective nose into social media.
Yes, you’ll go back to that glorious era: The Pre-Smartphone Age.
Because it’s pretty much impossible to get social when you’re hip-deep in enhanced external counterpulsation.
You simply can’t do it, no matter how deft your Twitter finger.
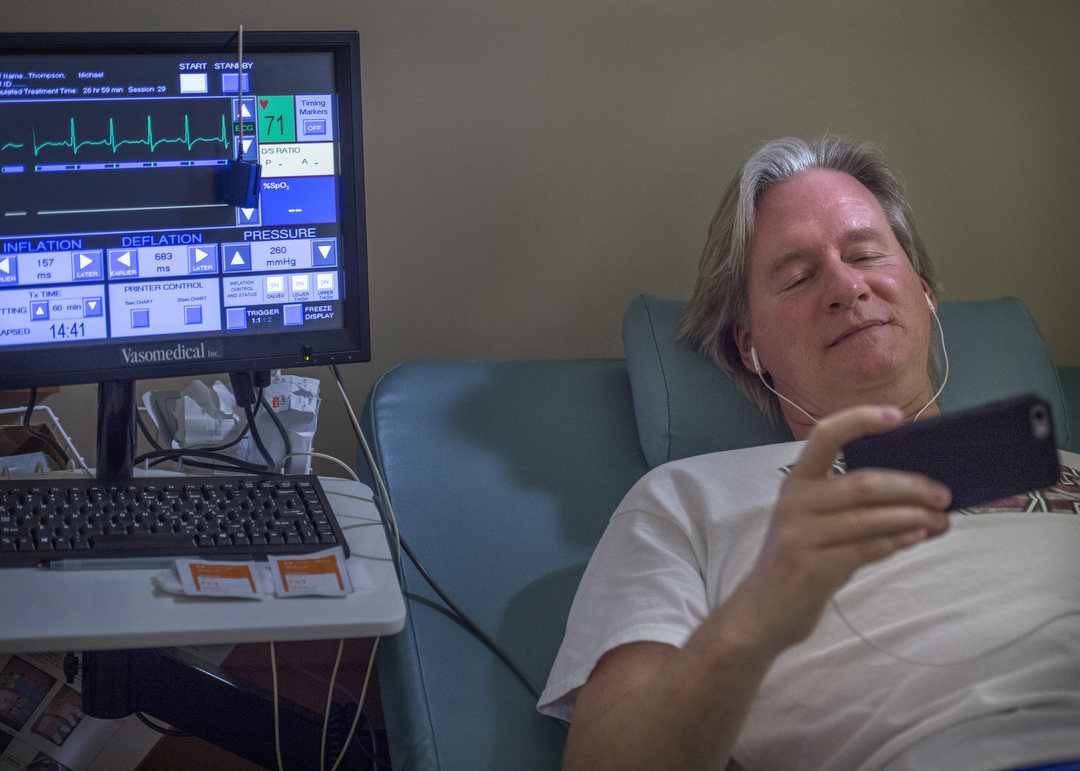
“You’re bouncing on that bed like crazy,” said Michael Thompson, 54, who wrapped up a series of counterpulsation treatments at Spectrum Health in mid-March. “I’ve tried Facebooking and texting on that bed. It’s not an easy thing to do.”
But as for counterpulsation, this Rockford, Michigan, resident swears by it.
“I’m a firm believer in it,” he said. “It’s well worth any amount of pain if it keeps me alive. And so far, it has.”
Here, in fact, is where counterpulsation is more analogous to a time machine: It takes many patients back to their pain-free, pre-angina days.
Over its 35-session regimen, the procedure mimics the effects of exercise to alleviate angina, a symptom of coronary artery disease. Angina is essentially chest pain in a heart that isn’t getting enough oxygenated blood, although it’s typically indicative of more serious heart problems.
Refractory angina, in particular, is unresponsive to medication, which makes counterpulsation so useful.
“Before I went in, my chest pain was every day,” Thompson said.
Nothing provided relief. He couldn’t walk, couldn’t lift heavy objects, couldn’t do simple everyday tasks without experiencing shortness of breath and chest pain.
“Since I’ve finished (counterpulsation), I’m able to walk again,” he said. “I’m not winded so easily, I can pick things up, move things around without chest pain. It’s nice not having the chest pain.”
A hammer
Thompson’s latest go-round with counterpulsation is actually his second since 2006.
Counterpulsation is a noninvasive treatment specifically for refractory-angina patients who previously had heart surgery, stents, congestive heart failure or stable angina.
Thompson qualifies—and then some. Doctors have placed 16 stents in his arteries in various procedures since 2002, when he first began experiencing cardiovascular problems.
He remembers the first time the pain struck him. In 2002, age 39. It came down like a blow from on high one weekend as he drove to his boat dock in Grand Haven.
“I felt this hammer hit my chest,” he said. He stopped his truck on the highway for a moment, but then decided to continue on. “I thought it was heartburn.”
It happened again moments later. He pulled over again, waited a moment, then continued to the boat dock.
“When I got to the boat, I called 911,” he said. “They brought me back to the hospital and said I was having some kind of heart issue.”
Doctors discovered he suffered a mild heart attack.
“Throughout that year of 2002 I was in and out of hospital,” he said.
You could wrap up his ensuing 15 years thusly: 15 stents in his right coronary artery, one in his left coronary artery, procedures to clear blockages, a first round of counterpulsation, dramatic changes in diet, exercise and lifestyle.
Riding the cycle
Here’s a picture of counterpulsation: The patient lies supine on a bed, each leg enveloped in what looks very much like a giant blood pressure cuff—only these cuffs are bigger and they run the length of the leg, from calf to waist.
The cuffs are hooked to six tubes connected to a pulsating airflow system. The patient is outfitted with three wires that provide a precise read on the patient’s cardiac rhythm.
As the patient’s heart beats, each cuff pulsates with air, inflating and deflating in sync with the patient’s cardiac cycle.
“It sounds almost like torture,” Thompson said. “You go into this room and you see these machines and you think, ‘Oh my God, what am I getting myself into?’”
The treatment mimics the effects of exercise. For patients whose chest pain keeps them from strenuous activity, it’s life-changing.
Thompson is quick to caution that it’s a challenging treatment.
“It is kind of painful,” he said. “If you’ve ever had a blood pressure cuff put on, that goes up to 80 (pounds per square inch) when they squeeze that thing. This, they tell me, is up to 260 psi.
“When that squeezes, you feel it,” he said. “But it’s that tight for a reason. It’s supposed to be that way. They make it as comfortable as they can for you, but if it’s going to work, you’re going to have to go through some pain to get better.”
Even so, patients well into their 80s have completed the treatment, albeit with a firm nod to the difficulty.
“In my opinion, it’s a good pain,” Thompson said. “After the first week, you get used to it.”
He adds: “You know you’re doing it to make yourself better.”
Counterpulsation is successful in about 80 percent of patients, said Lisa Sawyer, manager of preventive cardiology and rehab at Spectrum Health.
“With each heartbeat, it’s squeezing the blood up to the heart,” Sawyer said. “It does this through the squeezing of the cuffs—it increases the blood and oxygen supply to the heart muscle. …The goal is to get blood flowing to build microvascular and collateral arteries in the heart.”
It is perhaps a lesser-known treatment for certain heart problems, although it has proven tremendously successful in the right circumstances.
Commitment
Most counterpulsation patients are just like Thompson—they’ve been through prior heart treatments, Sawyer said.
“(You’ll have) some where they’ve been stented a handful of times, bypassed,” she said. “But they’re still getting chest pain, angina, and they’re on medications … to try to control their chest pain.”
Spectrum Health began offering counterpulsation at the Bradford Street location about midway through 2016.
“We brought it on when we started the preventive cardiology program,” Sawyer said, explaining how it meshes nicely with Dr. Thomas Boyden’s patients. “It just streamlines with cardiac rehab well.”
Given the time demand the treatment places on patients, the counterpulsation room places some premium on comfort, offering TV, dimming lights, curtains, privacy and such.
Each treatment lasts a full hour. The entire regimen is 35 sessions. At five days a week, that’s seven solid weeks of treatment.
“It’s a large commitment,” Sawyer said. “But the reward, in the end, is well worth it.”
While the bulk of patients rely on counterpulsation to alleviate chest pain, Thompson is unique in that his doctors are also hoping the treatment will help open his coronary collateral arteries.
If this happens, it could present an opportunity to clear the blockage in his right coronary artery.
“I have three layers of 15 stents,” Thompson said. “It’s a full metal jacket, as they call it.”
But no matter what happens, he said, the counterpulsation has alleviated his chest pain.
Most important of all, of course, is his wife is rooting him on.
“She’s all for it,” Thompson said. “She’s happy I’m doing it. She wants me around a lot longer—I want to be around a lot longer, too. I’m not done on this earth yet.”














 /a>
/a>
 /a>
/a>
 /a>
/a>
One of the best US-FDA approved treatments for heart patients. Especially life saving for patients who are unfit for angioplasty stents and bypass surgery, where these have failed and for patients who want to avoid surgery for cultural, social, religious, econolim or any other reason.