The possibility of a big heart surgery loomed before 11-year-old Trent Ahlefeld. His mother couldn’t decide what to do.
Trent had already been through so much, coping with multiple heart defects. Did she want him to undergo this groundbreaking procedure to reconstruct his heart?
In the end, she listened to Trent. He told his mom he wanted the operation.
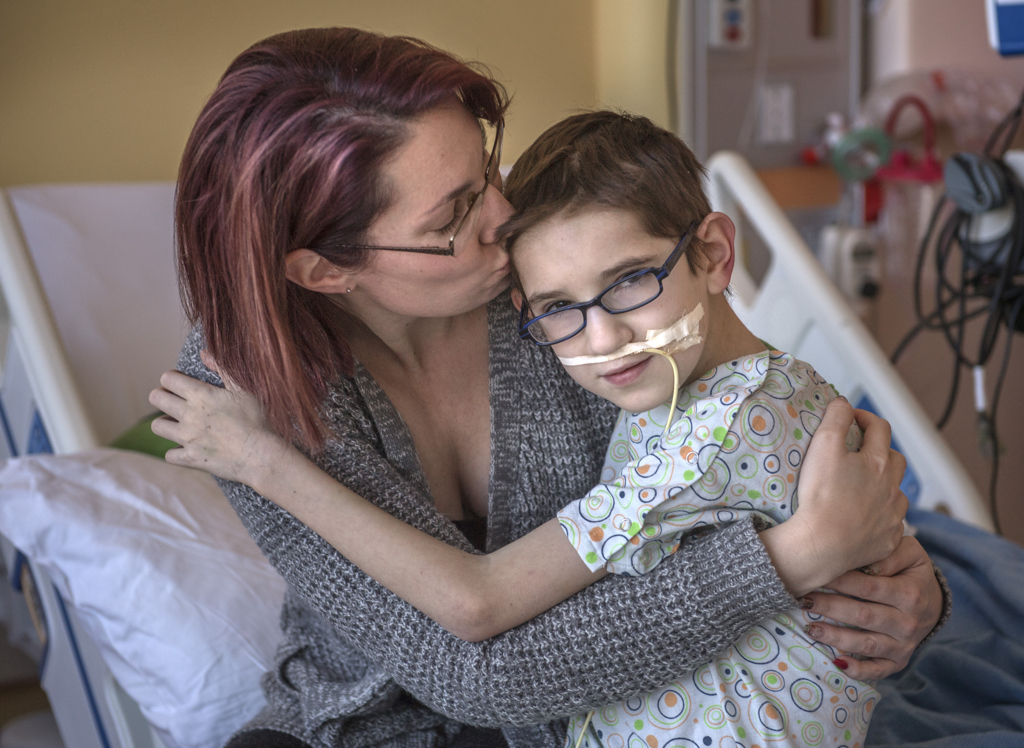
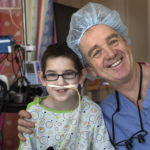
“I’ll take a risk to make myself feel better,” he said, as he sat in his bed at Spectrum Health Helen DeVos Children’s Hospital, holding Pichu, his yellow stuffed Pokemon character. “I’m glad I did it.”
“You’re a real pioneer,” said Marcus Haw, MD, the congenital heart surgeon who performed the operation. “You are one of the very, very first to have benefited from this.”
You were the only one who took a chance. And you did it and gave us life again.
The complex repairs to Trent’s heart came after his mother, Megan Thompson, consulted congenital heart specialists around the country during the past decade.
Although Trent underwent procedures to improve his heart function, a more complete repair remained out of reach until she consulted Dr. Haw and the Congenital Heart Center at Spectrum Health Helen DeVos Children’s Hospital.
“You were the only one who took a chance. And you did it and gave us life again,” she said. “After 11 years of ‘No, no, no,’ you said ‘I think I can’ and you did.”
Looking for answers
When Trent, born in California, came home from the hospital as a newborn, his mother knew he had several serious congenital heart defects.
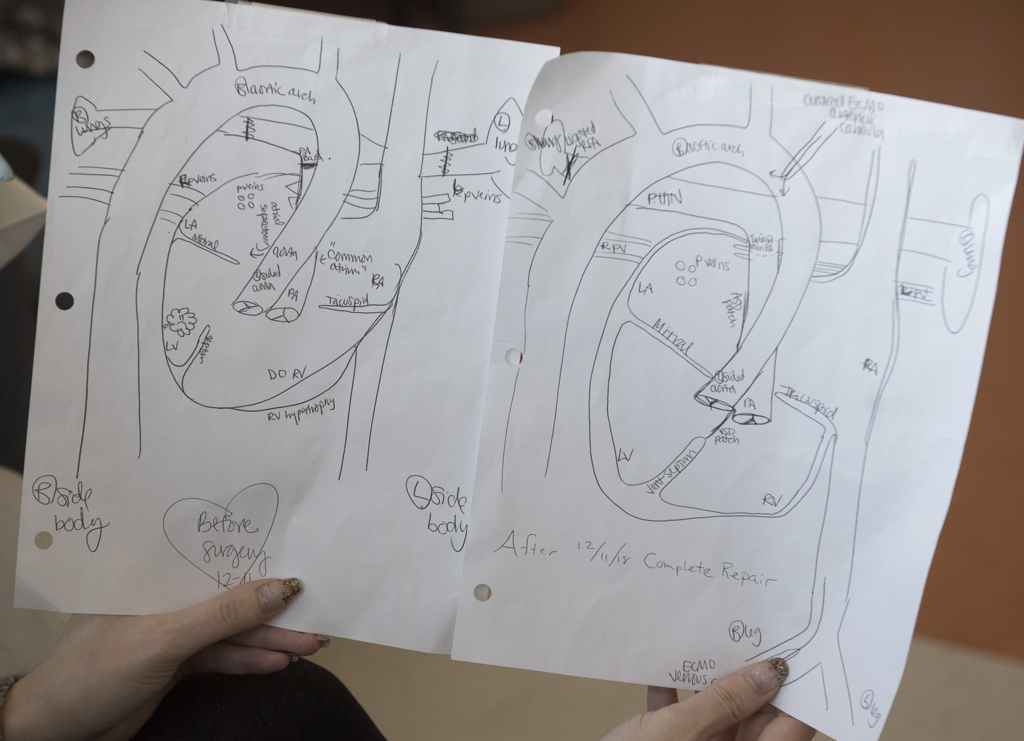
Instead of four chambers, his heart essentially had only two. A gaping hole lay in the wall that separates the two atria, the two upper chambers of his heart. Another large hole lay in the wall between the two ventricles.
His heart also had formed on the right side of the chest, instead of the left, and faced the opposite direction of a typical heart. The veins that bring blood from the lungs were connected to the wrong side of the heart.
As an infant, Trent underwent surgery on his pulmonary veins and later had stents placed. Although he no longer had a functioning right lung, his heart function improved.
But by the time Trent turned 10, his heart had a harder time meeting the demands of his growing body. Simple activities left him winded. Thompson, now living in Greenville, Michigan, consulted the specialists at Helen DeVos Children’s Hospital.
Joseph Vettukattil, MD, who co-directs the Congenital Heart Center with Dr. Haw, specializes in advanced imaging techniques that provide a clearer picture of complex hearts.
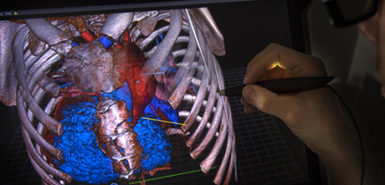
Working with a sonographer, he had a 3D model of Trent’s heart printed.
Although Trent was considered inoperable by three major heart centers, Dr. Vettukattil’s assessment suggested that his heart could be repaired. To achieve this, he first had to have further procedures to reduce the high pressure in his lung.
Dr. Vettukattil performed a cardiac catheterization to expand the stents to improve blood flow to Trent’s heart. This led to significant improvement, and Trent developed excessive blood flow to his lungs. To control the high flow and prepare him for the final repair, Dr. Haw placed a band on the pulmonary artery, which improved his condition further.
But a few months later, Trent was admitted to the hospital in heart failure, with fluid collecting in his chest. Scans showed he also had a blood clot in his right ventricle.
I want to feel better and be like my brother and friends.
He needed open-heart surgery to remove the blood clot. Before the operation, Dr. Haw discussed the possibility of doing a complex reconstruction of the heart—patching the holes and rebuilding two valves—during the operation.
If that was not possible, or if Thompson opted against it, he could tighten the band around Trent’s pulmonary artery. This would be a less involved procedure, but the benefits would not be as long-lasting.
Thompson struggled to decide what to do.
“We were told for basically 10 years of his life that there was nothing we could do for him,” she said. The possibility and risks of the operation “flipped my world upside down. I had to sit on that for a while and weigh my options.”
Trent, though weakened and tired, said he wanted the operation.
A sixth-grader at Greenville Middle School, he is an active, curious kid. He loves to draw, especially sketches of his stuffed animals. He loves Pokemon and writes imaginative stories featuring Pokemon characters. He builds complex Lego creations. He enjoys cooking.
He is best buddies with his 10-year-old brother, Aiden, and a good big brother to their two little brothers, Declan, 4, and Brennan, 2.
But he has always lived with some limits on his physical activities. He longed to be more active.
“I want to feel better and be like my brother and friends,” he said.
Rebuilding his heart
On the morning of Dec. 11, 2018, Trent went into surgery at Helen DeVos Children’s Hospital.
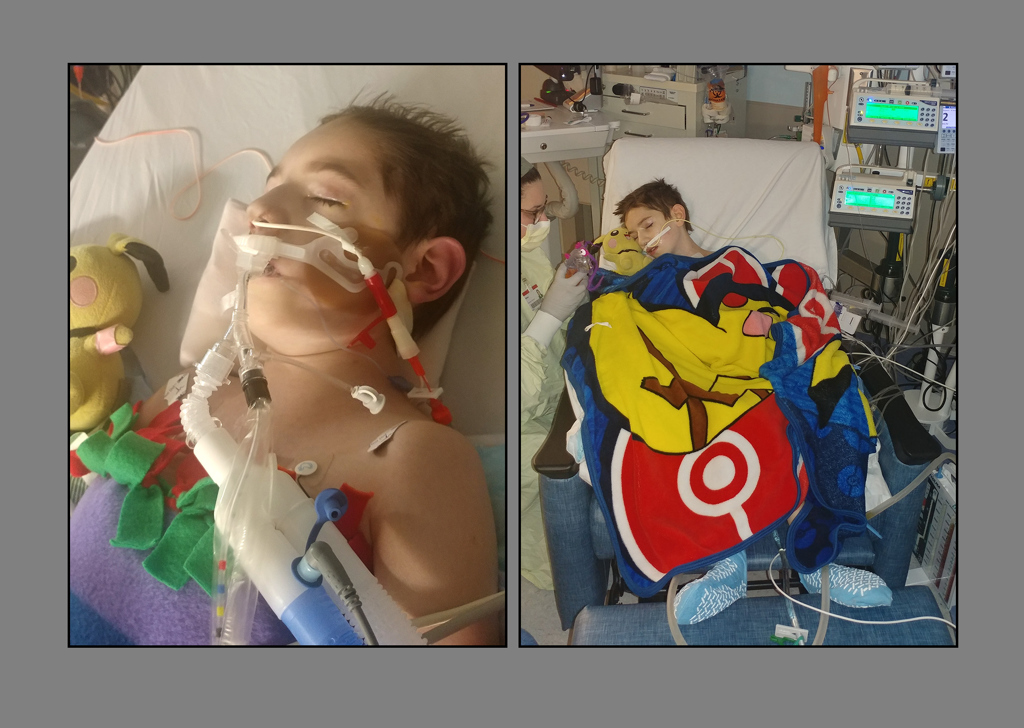
Because his condition was so unstable, before surgery the medical team connected him to a heart-lung machine, called extracorporeal membrane oxygenation, or ECMO.
During the surgery Dr. Haw patched the holes in Trent’s heart. He divided the single valve in his lower heart to create two functioning valves. And he created a tunnel through the right ventricle to connect the left ventricle to the aorta.
“In a patient like this, it’s never standard,” Dr. Haw said. “The access is completely inverted and (the holes) are so huge that even judging how big to make a patch was very, very difficult.”
Having seen the 3D model proved invaluable in performing the surgery because of the unusual position and angle of Trent’s heart.
Ten hours later, Trent emerged from the operation. For the first time in his life, his heart had four separate chambers, each collecting or pumping blood, as designed, with every beat.
This meant his body now got the fully oxygenated blood it needs—to move and grow.
Six days after the surgery, the doctors removed the ECMO device. After another five days, they removed the ventilator.
Trent, having spent nearly two months in bed, began the long battle to recovery.
The road back
At first, just sitting up proved difficult.
Occupational therapists worked with Trent’s fine motor skills, guiding his hands as he relearned to hold a pencil. Physical therapists helped him straighten his legs and get the strength to stand.
One day, he made a visit to the pediatric intensive care unit and walked slowly around the floor, wheeling his walker in front of him. The nurses and aides who had cared for him when he was so ill greeted him with surprised smiles and warm hugs.
I think the approach and fundamental impact of the new imaging software is going to benefit a small number of very complex patients who wouldn’t have otherwise been offered surgery.
Nearly a month after surgery, Trent transferred to Mary Free Bed Rehabilitation Hospital to continue his therapy. His goal: to return home, to sleep in his own bed and hang out with his brothers.
For Trent, the future now involves gaining weight and building muscle.
“He has always been nutritionally very depleted,” Dr. Haw said. “He has also lost a lot of muscle mass. That will take a year or two years to build back up.”
With just one lung, he will still have some limits on activity, but not as many as before.
“From a heart point of view, there is no reason his heart shouldn’t sustain a reasonable level of exercise,” Dr. Haw said.
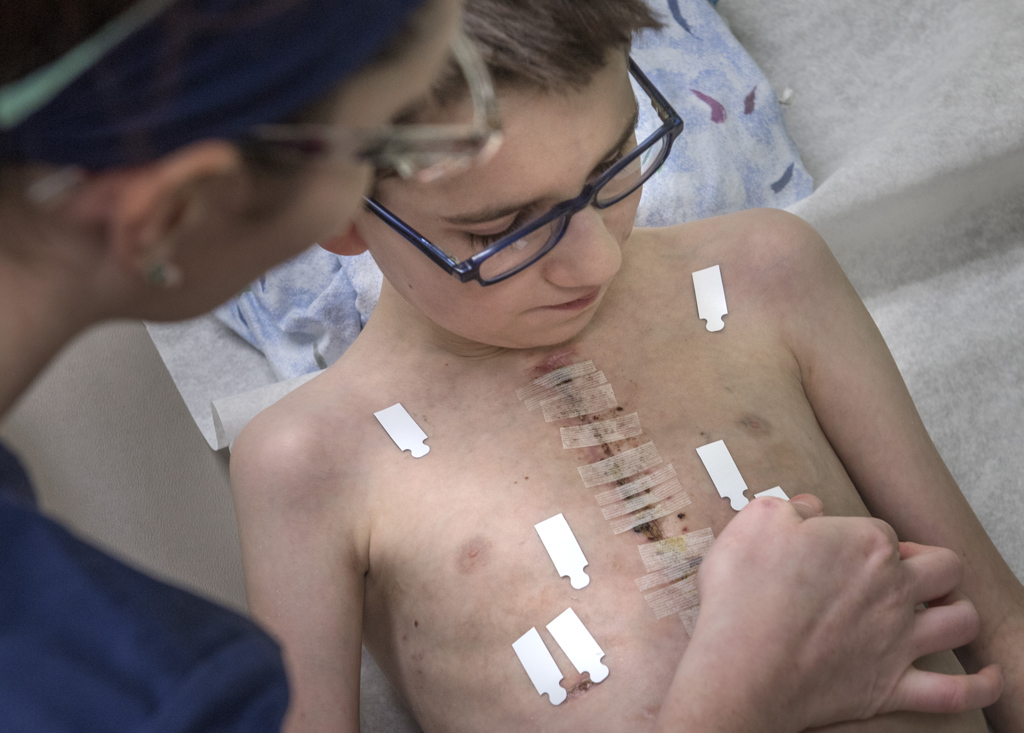
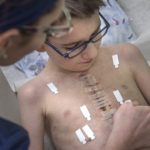
One afternoon about a month after surgery, Trent visited the congenital heart center for an EKG and checkup. He proudly showed the incision running the length of his chest.
He stood and took small steps across the exam room, showing his ability to walk on his own.
“I’m getting stronger,” he said.
Nurse practitioner Anna Weller, PNP-AC, held the stethoscope on his chest and listened.
“He still has a slight murmur,” she said. “But it isn’t even close to what it was before.”
She called up an X-ray image of Trent’s chest, pointing out his heart and lungs on the monitor.
“It looks beautiful,” she said.
Trent smiled. “Cool,” he said.
Helping other kids
A crucial factor in the success of the surgery was the ability to examine and visualize the heart in three dimensions, Dr. Haw said. He predicted the development will provide hope to other children like Trent.
“With this technology, we have been able to deliver an anatomical result that will give him a sustainable life for decades hopefully,” he said. “I think the approach and fundamental impact of the new imaging software is going to benefit a small number of very complex patients who wouldn’t have otherwise been offered surgery.”
He also credited Thompson and her devotion to her son.
“This mom never stopped looking (for answers),” he said.
As for Trent and his willingness to undergo the tough challenges of surgery and recovery—Dr. Haw has great admiration.
“I’ve been doing this game a long time, and there’s not too many young men of your age who have that courage and force to go for it,” he told him. “We are just very, very proud of you.”







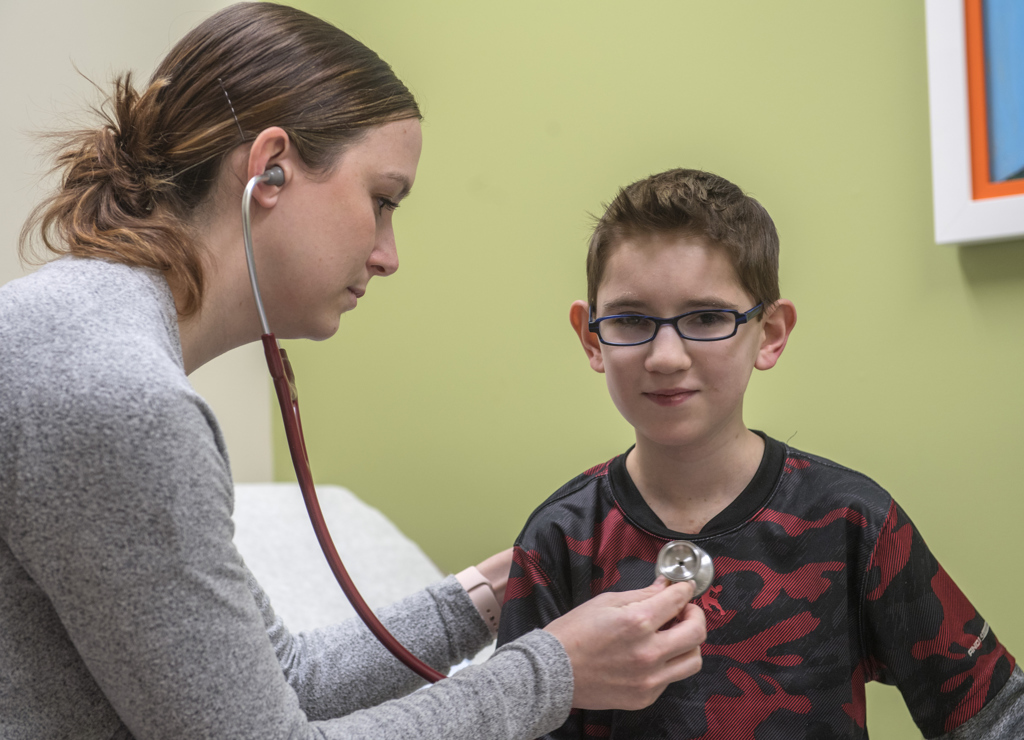

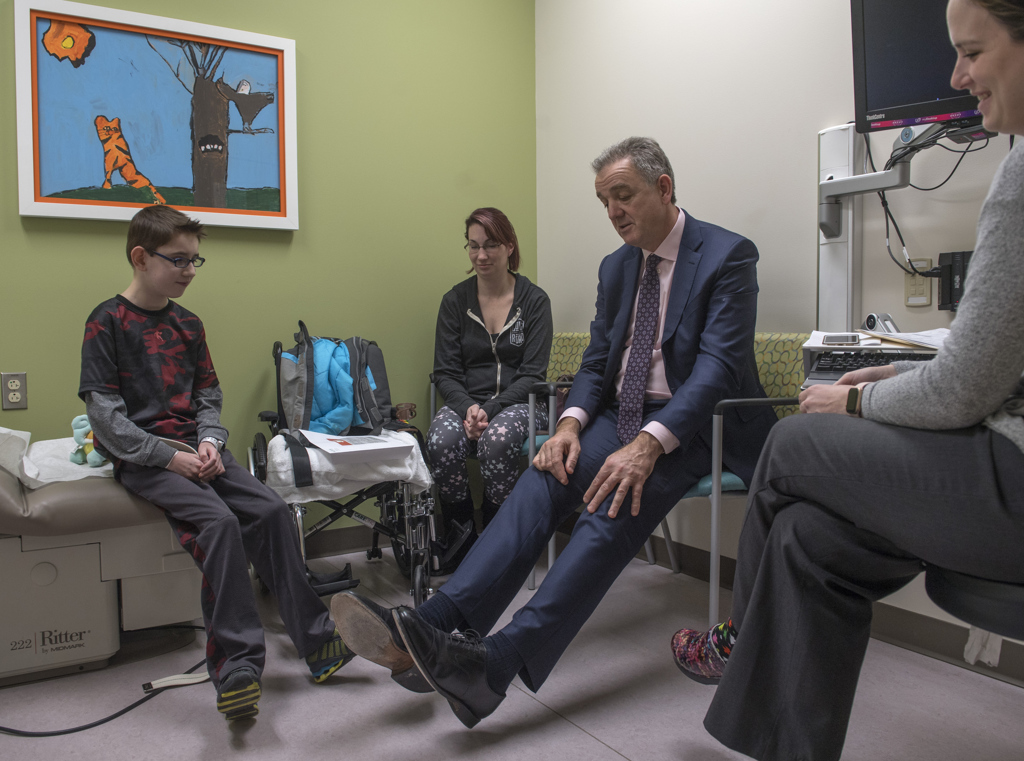






















 /a>
/a>
 /a>
/a>
 /a>
/a>
What a wonderful story with Doctors and medical staff willing to go all out for Trent. The real Hero is Trent ,willing to take the risk to get better and pave the way for others suffering a life of no hope. We are so fortunate to have this specialized Heart Hopital right here in Grand Rapids Mi. We are Thankful for Richard DeVos and the vision he could see when he started the Hospital after he himself had to travel out of the country to receive a new heart. With his Family and Friends the building project continues to give people life and hope. We continue to keep Trent in our prayers for Strength and Healing. Thank You to all the Medical Stall. Job well done! 👍
Thank you for your kind comments, Judy! We’re blessed to have such an innovative and compassionate health care team here in Grand Rapids!
God bless Dr. Haw for giving Trent a new life! Thank you to all the staff at the hospital. Now Trent can have a more normal life and be the big brother.
Both these amazing men helped keep my son David alive when he was only days old. He was born with hyperplastic left heart syndrome. He is now 10 years old, will still need a heart transplant when in his late teens. But without Mr Haw and Joseph he would not be here today. Fantastic to see they are still carrying on the fantastic work in the USA. Sad to see them leave Southampton General.
Thank you so much for sharing your testimony, Stuart! Best wishes to you and David. Cheers, Cheryl 🙂
Truly amazing how they could reconstruct his heart! It is so wonderful to have more and more life saving surgeries done right here in Grand Rapids.
Yes, we are fortunate to have such skilled specialists here. Thanks for reading, Christina.
Praying for complete healing! Love your courage. God is your Great Healing Physician!
Welcome to the pioneer club buddy! Back in 1962 I became the first infant to get a pacemaker. I’m now a great grandma! The world is yours!!
Congratulations, Rocky! Glad to hear you are doing so well. Thanks for sharing your encouraging words.