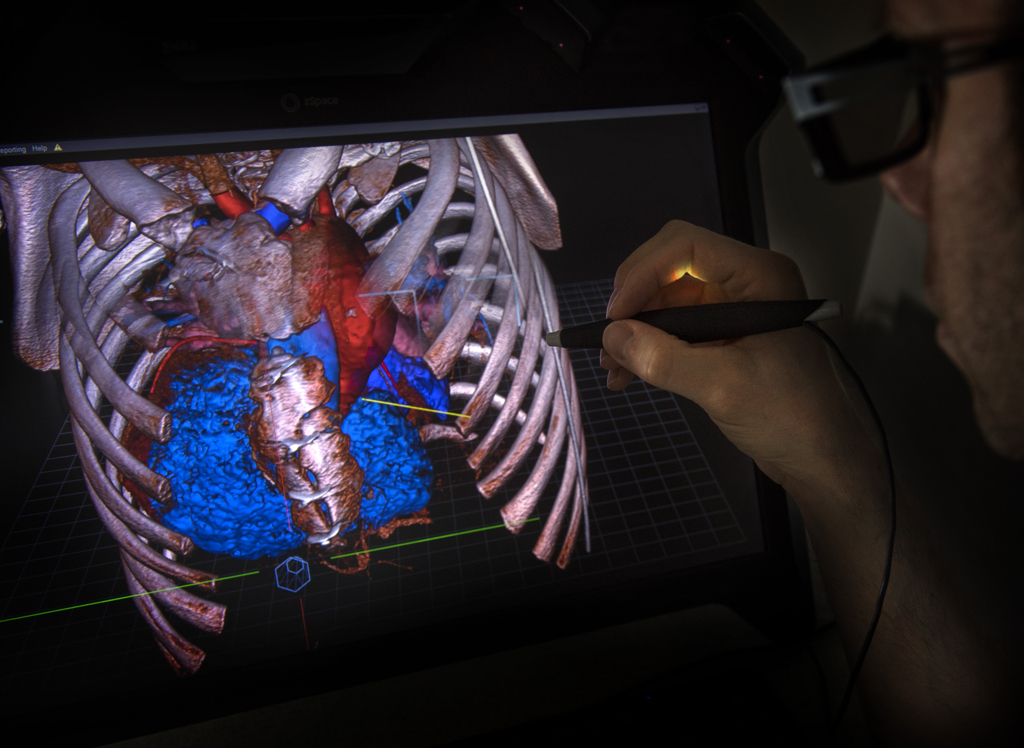
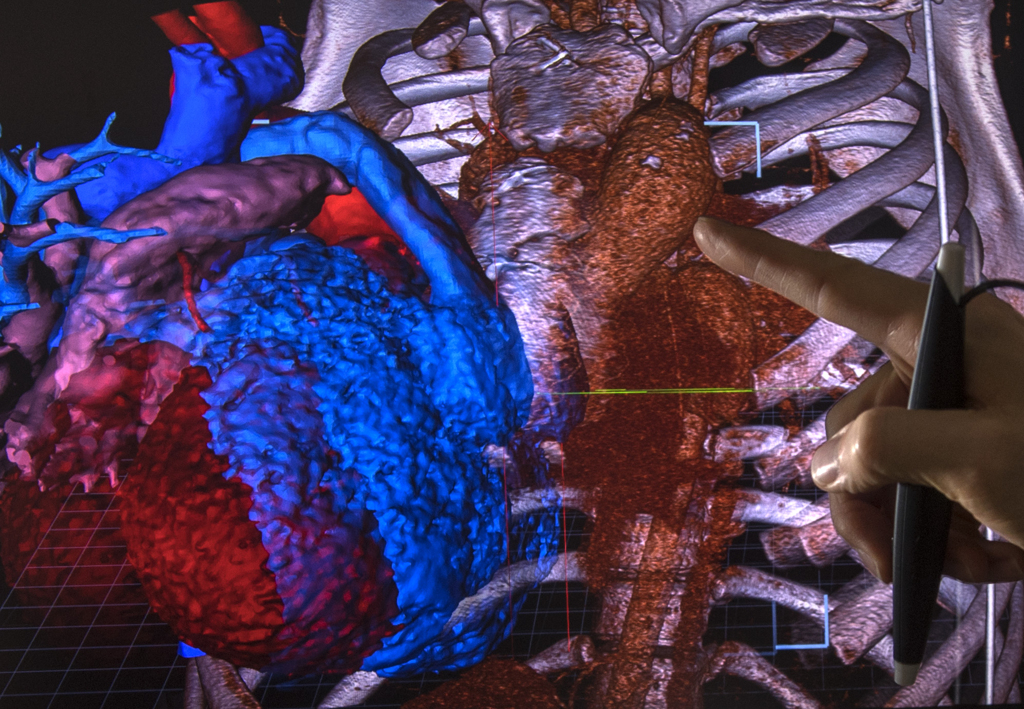
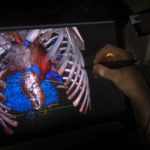
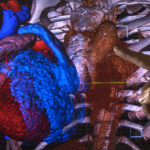
The image of Luke Carpenter’s heart seemed to float off the screen, a hologram in red and blue.
With flicks of a stylus, the heart moved forward, rotated left and right, and then settled back into position among the ribs.
For Luke, a 15-year-old from Middleville, Michigan, the virtual image matches the reality of his life.
For the specialists at the Congenital Heart Center at Spectrum Health Helen DeVos Children’s Hospital, it’s a roadmap that helps them plan the best way to fix what ails him.
The 3D imaging software, True 3D Viewer by EchoPixel Inc., is the latest high-tech tool used by the congenital heart team to understand the complex anatomy of a beating heart.
The physicians used scans of Luke’s heart to create the virtual image, which they consulted as they decided whether to do surgery, and how to prepare for the operation.
‘Tired pretty quick’
Luke, the son of Pam and Jason Carpenter, was born with several rare congenital heart defects, including dextrocardia, a condition in which the heart is situated on the right side of the chest, instead of the left. And he had transposition of the great arteries—which means the two major blood vessels that carry blood from the heart were switched.
By the time he entered Thornapple Kellogg High School last fall, Luke had undergone four open-heart surgeries. Surgeons patched holes in his heart, replaced the mitral valve and rerouted major blood vessels.
The fixes helped him grow and thrive in school and activities. He couldn’t play contact sports because of the blood thinners he took, but he loved to watch football and basketball. And he played golf and joined the high school team.
One day, he would like to become an athletic trainer for sports teams.
In the fall of his freshman year, however, he noticed difficulty in keeping up the same level of activity.
“I’d get tired pretty quick,” he said. “I would feel like (my heart) was beating really fast.”
“He was fine (when he was) resting,” his mom said. “But when he was running around the yard or doing something even mildly active, his heart would be pounding really hard.”
His pediatric cardiologist, Jeffrey Schneider, MD, consulted Joseph Vettukattil, MD, an interventional pediatric cardiologist and the co-director of the congenital heart center.
Pioneering a solution
The congenital heart team focused on the tube that had been placed in Luke’s heart to connect the right side of the heart to the lung arteries. A surgeon first created the conduit when he was 14 months old because he was born without a pulmonary artery. A surgeon replaced it when Luke turned 9.
Dr. Vettukattil examined the structure in a heart catheterization procedure. He hoped to use a balloon catheter to expand the tube and improve blood flow.
But he discovered the conduit lay between the heart and the breast bone, a tight spot that compressed the tube. The congenital heart team determined he needed open-heart surgery to replace the tube—and to place it in a different spot.
Getting a clear picture of Luke’s unique heart became crucial to planning the surgery.
“In a complex heart like this, when the heart is on the right side of the chest, it is important for the surgeon to orient themselves,” Dr. Vettukattil said.
A pioneer in 3D imaging techniques, Dr. Vettukattil used scans of Luke’s heart to create a 3D printed model, printed in a clear plastic resin.
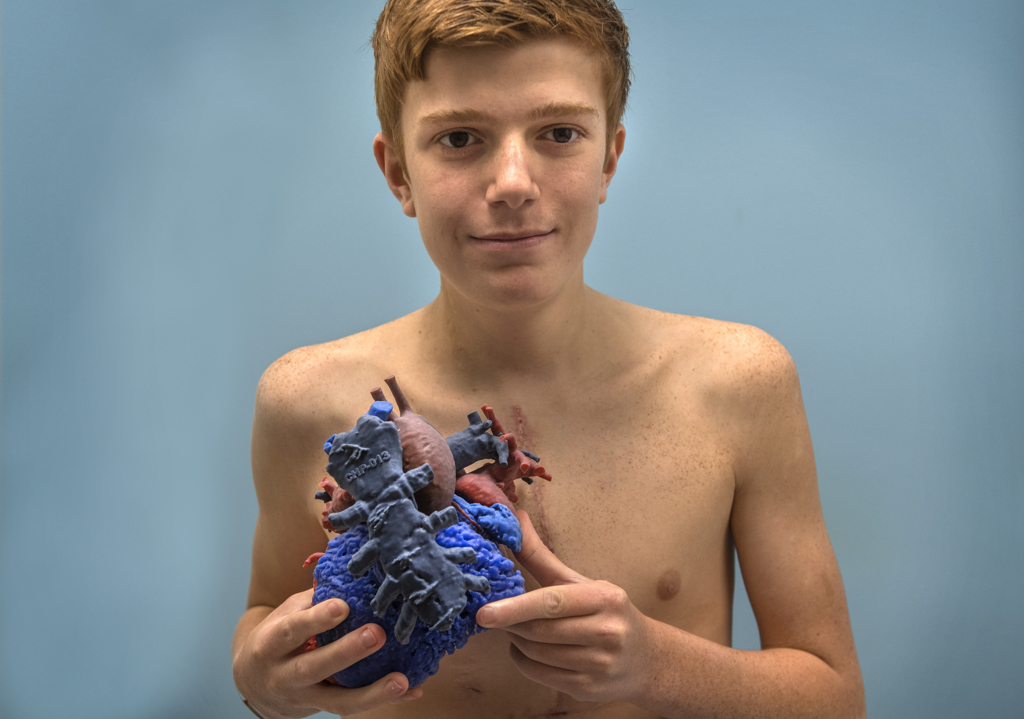
Then, he contacted researchers in Michigan State University’s biomedical engineering department, who printed a model in color, using shades of blue and red to distinguish the vessels and chambers of the heart as well as part of the sternum.
That model also was used to create the image of the heart viewed on the Echo Pixel monitor. Wearing 3D glasses, the physicians examined the heart and its position within Luke’s chest.
“When you do the Echo Pixel model, you are visualizing the whole chest,” Dr. Vettukattil said. “You have a much better spatial understanding—the whole organ system of the patient is represented intact. And you are visualizing it in three dimensions.”
Marcus Haw, MD, pediatric heart surgeon and co-director of the congenital heart center, used the 3D images to plan the operation.
“As soon as I reviewed the printed model, I was able to show Luke and his parents the compressed conduit,” he said.
“More importantly, it showed that there was an extension of his heart cavity that would give room for a larger conduit—and that the coronary artery was not in the way of the potential route for the conduit.”
On April 16, 2018, he placed a new tube between the right side of the heart and lung arteries, this time routing it across the top of Luke’s heart. He also replaced the mitral valve with a larger one.
‘Means everything to us’
Two and a half weeks later, Luke arrived at the congenital heart center for his follow-up visit.
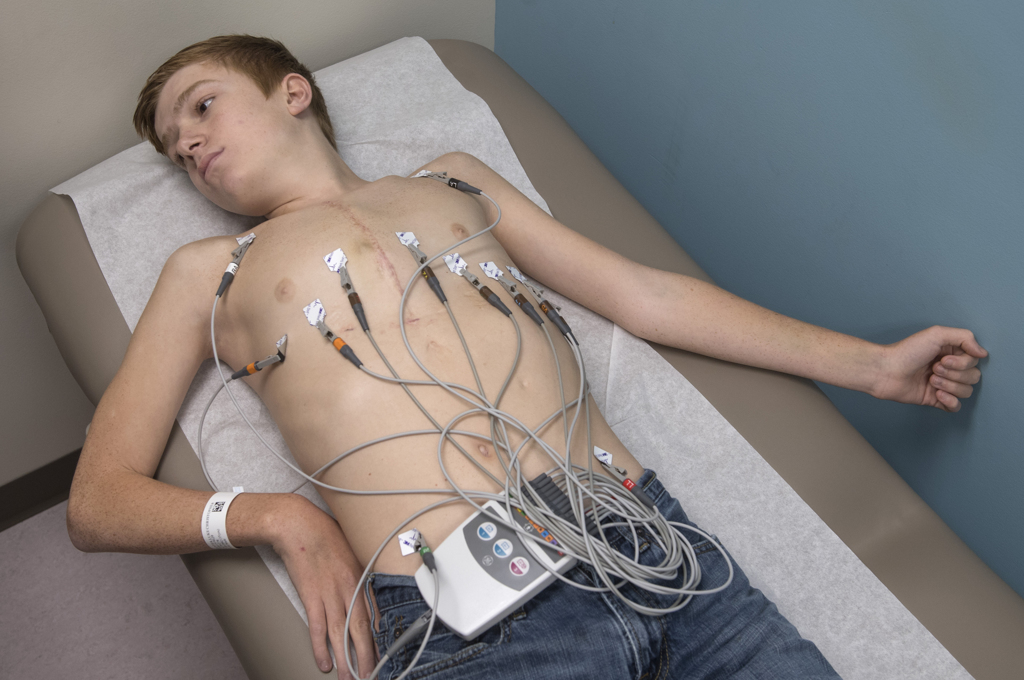
“You’re healing nicely,” said physician assistant Sarah Yarger, PA, as she examined the incision.
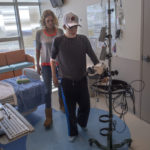
As he recovered from surgery, Luke said he was slowly regaining energy and appetite. He received approval to return to school the next week.
He hoped the new connector in his heart would make a difference. He looked forward to getting back on the golf course.
“I hope it will make me have more energy and able to do more things,” he said.
He had a chance to look at the colorful 3D model of his heart pre-surgery.
“It’s crazy,” he said, turning the heart over in his hands.
He pointed out the tube that lay compressed under the sternum—the one that had just been replaced.
For the specialists at the congenital heart center, the use of 3D imagery—including the printed model and the virtual image seen with 3D glasses—helps further the diagnosis and treatment of complex congenital heart defects.
“The capability to see the structures of the heart in this way is opening up new possibilities for patients who’ve previously been told there is no more we can do or that surgery is too dangerous,” Dr. Haw said.
The physicians continue to work on ways to better see the interrelated parts of a beating heart so they can fine-tune each patient’s treatment.
“That means everything to us,” Dr. Vettukattil said. “If we can use the best technology for the best treatment for our patients, that means a lot.”














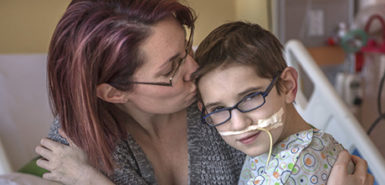 /a>
/a>
 /a>
/a>
 /a>
/a>
Love this story and love this family. Thank you to the physicians and medical team at HDVCH congenital heart center for saving Luke’s life! ❤️
I loved this story . So very similar to my brother’s case—he was born a “blue baby”, with no pulmonary artery, & also his heart on the right side, with all his organs reversed. My brother was born before they could fix the problem-he passed away in 1980. So thankful for the care Luke received & all those who are born with congenital heart defects.Thank the Lord for His help to all the Drs.who are helping those with heart problems.
Thank you, Ray, for your kind comments. I am so sorry to hear about the loss of your brother. It is remarkable how far medicine has come in the past 40 years, and I only expect even greater strides to be made in the next 40. Best wishes to you and your family and thank you for being a Health Beat reader. Best, Cheryl