What does congenital heart patient Nicholas Borgman have in common with the Marianas Trench, Mammoth Cave and UNESCO World Heritage Sites?
The question may sound like the set-up to a bad joke, but the answer is a fascinating glimpse at the crossroads of advanced imaging technology, human ingenuity and the hope for better outcomes for congenital heart patients.
Just as oceanographers use multibeam sonars to map the contours of the ocean floor and geographers and archaeologists push boundaries to three-dimensionally map the earth’s unknown frontiers and ancient sites, physicians and medical imaging specialists are pushing boundaries to map the hidden secrets of the human heart.
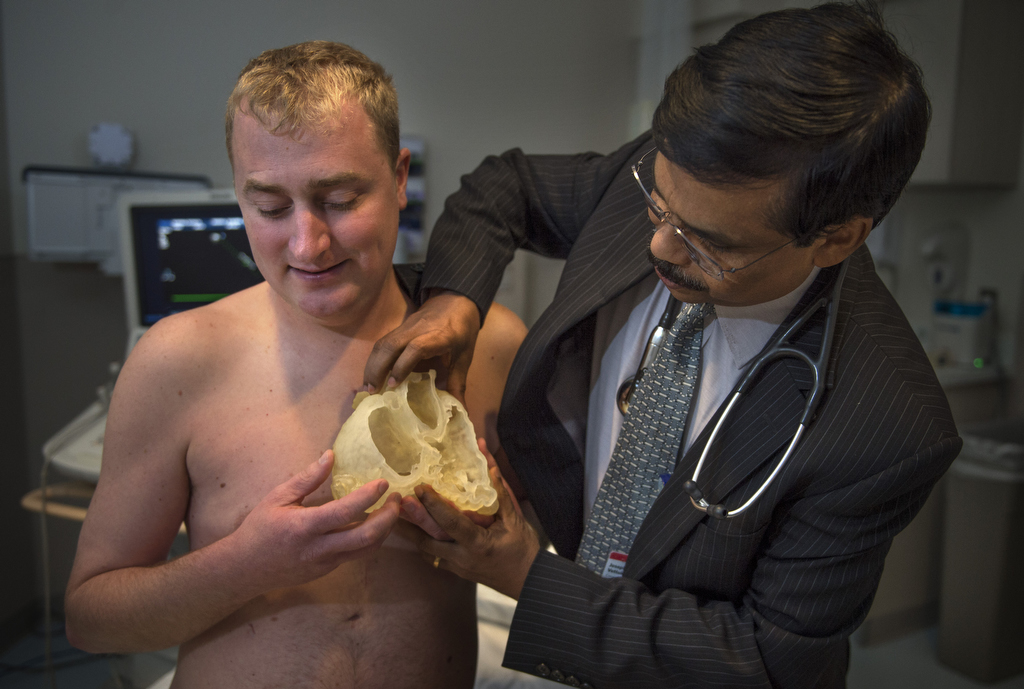
“We are engineering for life,” said interventional cardiologist Joseph Vettukattil, MD, co-director of the Spectrum Health Helen DeVos Children’s Hospital Congenital Heart Center. “You want to have respect for the heart and cause minimum disturbance. Nicholas is the first patient with a 3-D heart to benefit from integrated imaging techniques.”
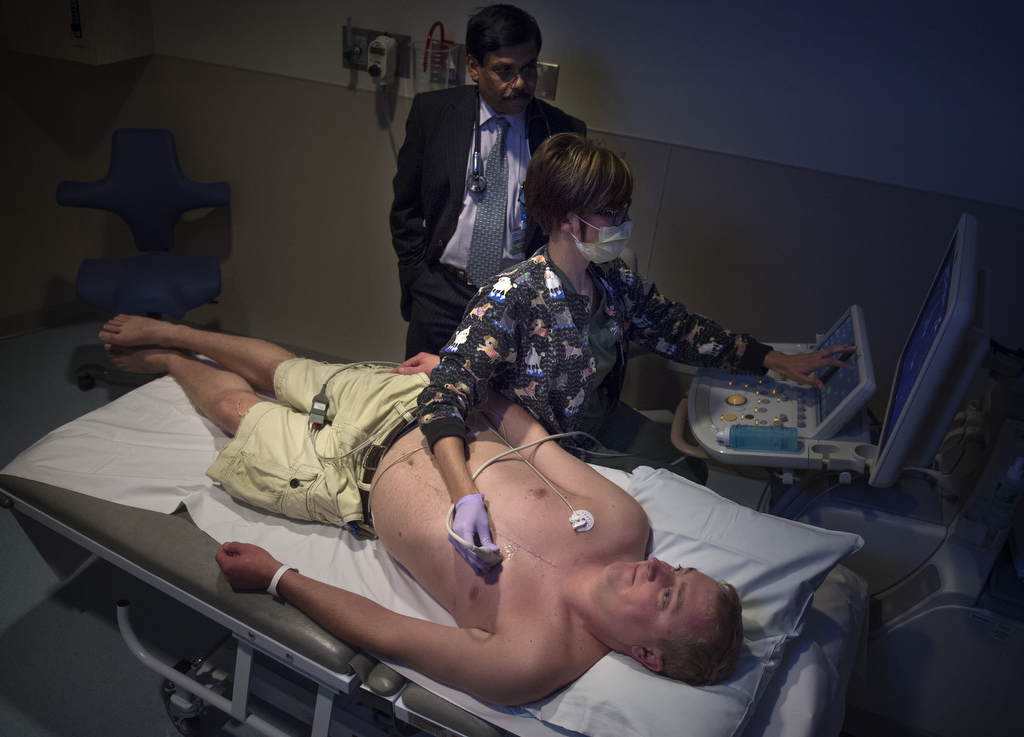
Dr. Vettukattil and colleagues from Helen DeVos Children’s Hospital made headlines in June when they announced the successful integration of computed tomography (CT) and three-dimensional transesophageal echocardiography (3DTEE) to print a hybrid 3-D model of a patient’s heart.
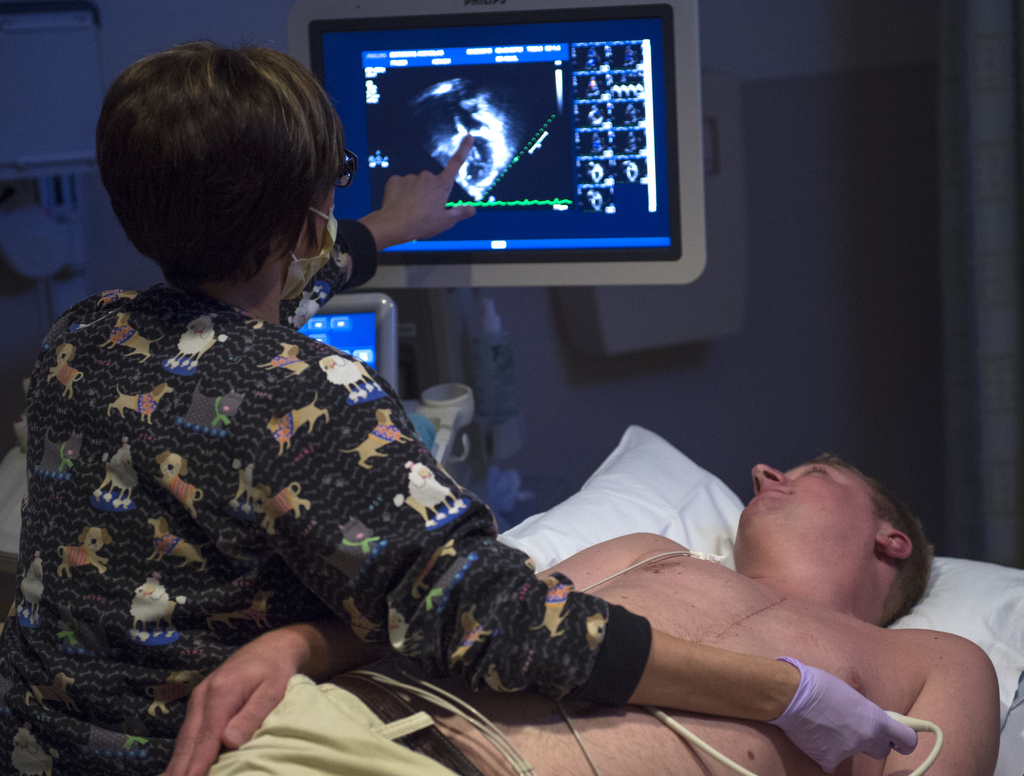
On August 12, Nicholas became the first congenital heart surgery patient to benefit from a three-dimensional anatomic model of his own heart printed by integrating 3DTEE and magnetic resonance imaging, commonly known as MRI.
‘It snuck up on us’
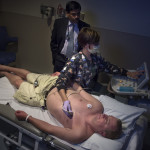
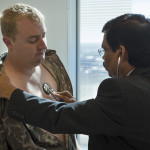
Nicholas, 25, of Zeeland, Michigan, is no stranger to heart surgery, though he has little recollection of his first three procedures. But Vicki Borgman, Nicholas’ mother, remembers every detail.
“Nicholas was born without a pulmonary valve, which moves blood toward the lungs and keeps it from flowing from the pulmonary artery back into the heart,” she said.
“He was born on Nov. 22, 1989—the night before Thanksgiving,” she recalled. “The first three surgeries were done in Ann Arbor at University of Michigan Hospital. I’m thankful for Spectrum Health—it’s so nice to be close to home.”
When he was only 6 days old, Nicholas received a shunt to temporarily direct blood flow to the lungs. At 7 months, he underwent surgical revision of his pulmonary outflow tract. And at age 2, his shunt was removed and he underwent a procedure to enable blue, deoxygenated blood to flow directly to both lungs.
Both Nicholas and Vicki, and the rest of the family—father Jerry, older brothers Jeremy and Benjamin, and twin sister Alyssa—knew that eventually he might need another corrective surgery, but as Vicki mentioned, “the 25 years kind of snuck up on us.”
“My first thought was that there is no way someone is cutting into me again,” Nicholas said.
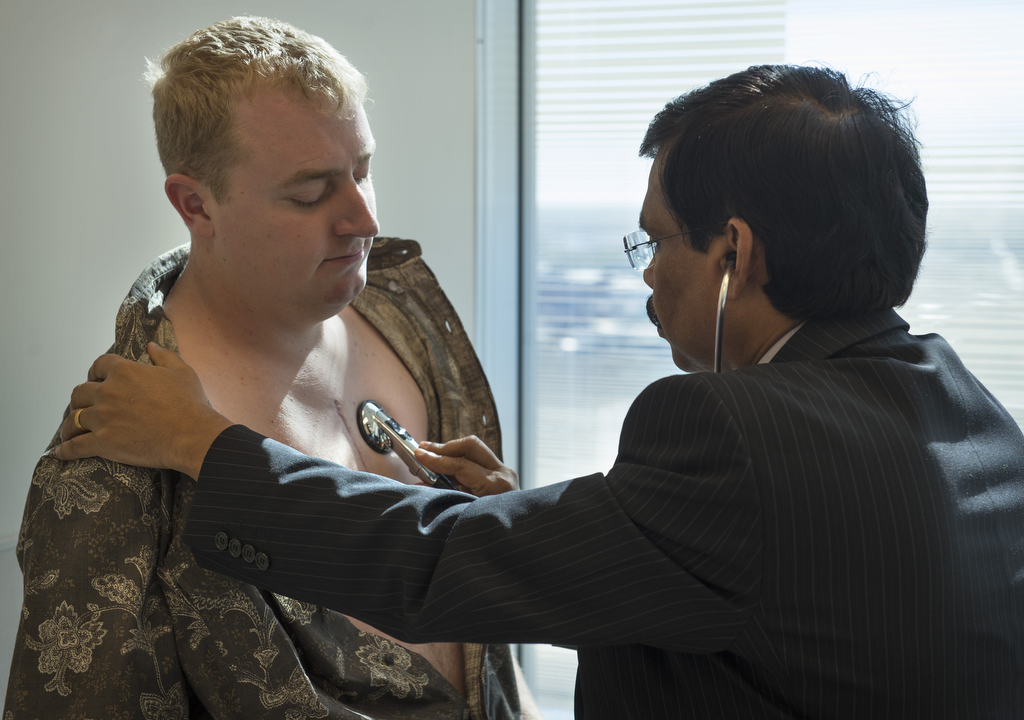
But after tests showed his mitral and pulmonary valves were not closing tightly and several other complications, he changed his mind.
“I decided I didn’t want to risk it,” Nicholas said. “I’d rather go through that than set myself up for risks and complications later in life.”
‘A tremendous relief’
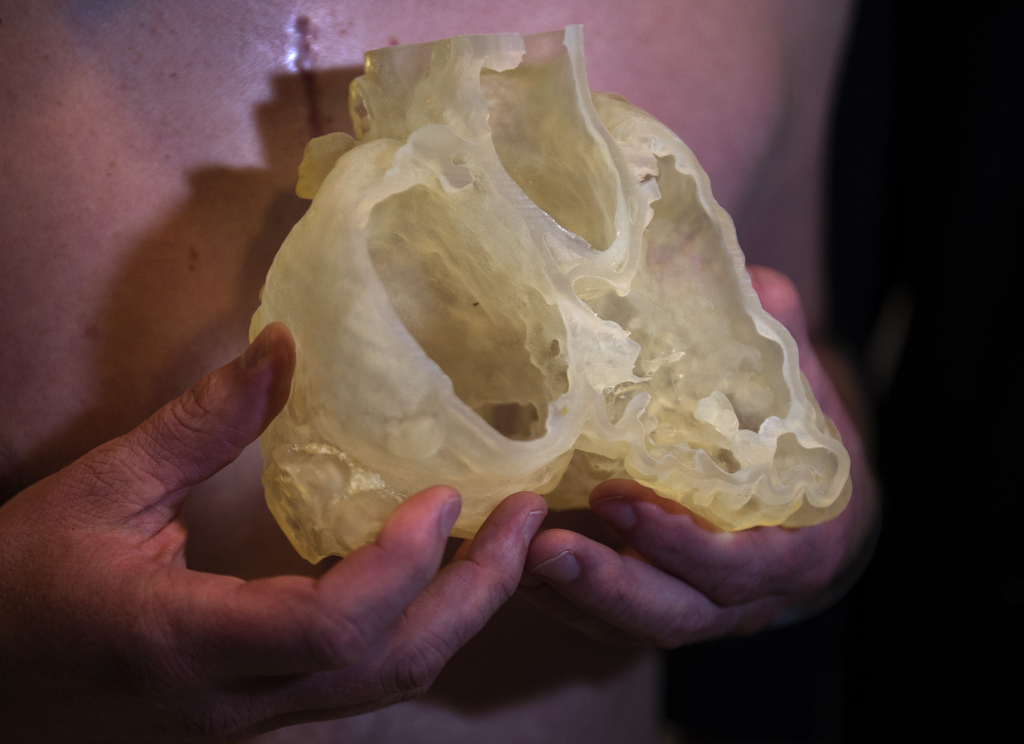
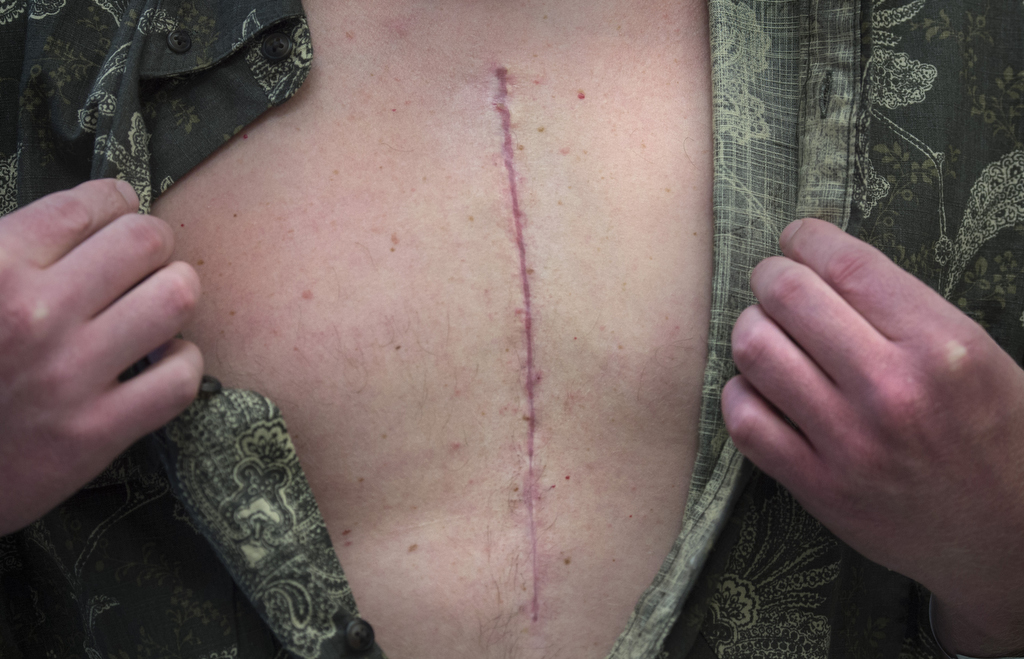
The 3-D model, which was printed by Burton Precision and Engineering 4 Life of Comstock Park, Michigan, made things easier for Nicholas, whose surgery took a mere two hours.
It also made the procedure more efficient and precise for his surgical team, which was led by Marcus Haw, MS, FRCS, co-director of the Congenital Heart Center. Dr. Haw was assisted by congenital cardiothoracic surgeons Neal Hillman, MD, and Giedrius Baliulis, MD.
The 3-D model allows cardiovascular surgeons to make a more precise determination of what actually lies ahead before opening the chest of a patient like Nicholas.
“Without the 3-D model, the surgery would be more time-consuming and more stressful,” Dr. Haw said. “It is very experimental, but a tremendous relief to me. If I can have the model, I know if it is wise to do it.”
The technique also has implications for the larger population of congenital heart patients, he added.
“A better understanding of the 3-D spaces will reduce the number of pediatric patients in need of palliative surgery, and in turn, the number of adult patients in need of corrective surgery,” Dr. Haw said. “This type of surgery is especially applicable to those congenital heart patients age 20-50. These are the ones who are dying early of untreated problems such as arrhythmia.”
The 3-D printed model of patients’ hearts has become more common in recent years as part of an emerging, experimental field devoted to enhanced visualization of individual cardiac structures. The Spectrum Health 3-D Heart Model project opened the way for CT and 3DTEE techniques to be used in combination with a third tool—magnetic resonance imaging, commonly known as the MRI.
According to Dr. Vettukattil and his colleagues, each imaging tool has different strengths, which can improve and enhance 3-D printing:
- CT enhances visualization of the outside anatomy of the heart
- MRI is superior to other imaging techniques for measuring the interior of the heart, including the right and left ventricles or main chambers of the heart, as well as the heart’s muscular tissue.
- 3DTEE provides the best visualization of valve anatomy
“This is a huge leap for individualized medicine in cardiology and congenital heart disease,” Dr. Vettukattil said.
As for Nicholas, he says he’s eager to get back to work at a Zeeland-area car wash, where he works as a self-described “jack of all trades.”
“I feel great,” Nicholas said. “I’ve gone for couple mile walks each day, I’ve been able to drive for a few weeks, I feel as though I have more energy.”
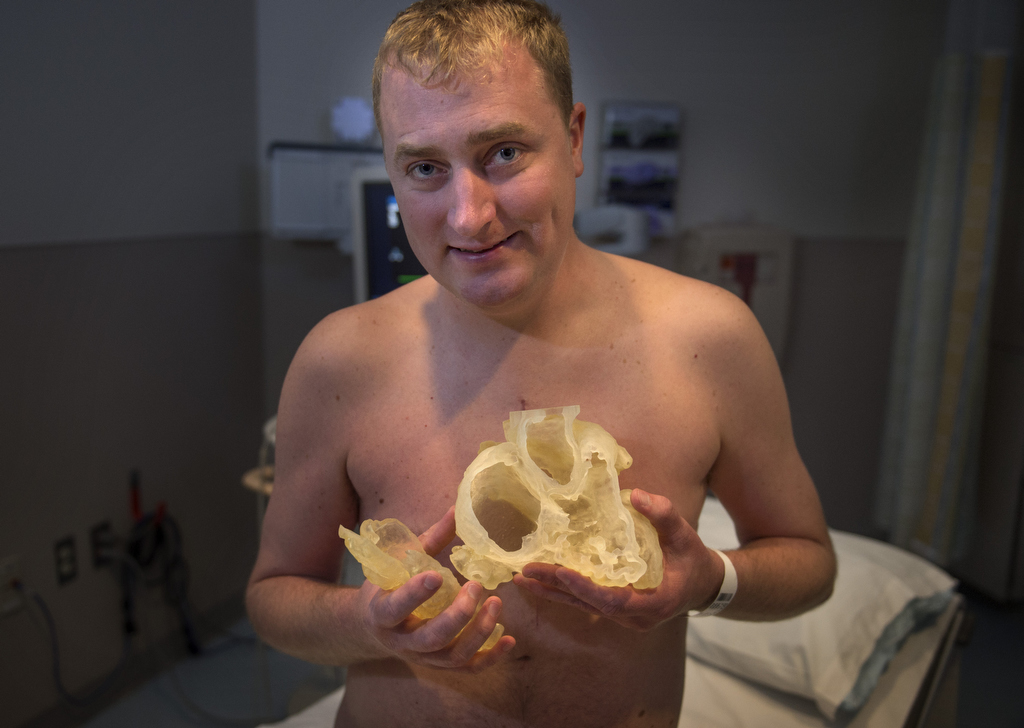
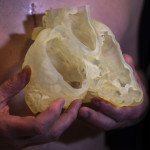
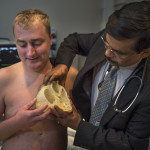
Asked what it was like to see a 3-D model of his own heart, he pauses for a moment to gather his thoughts.
“It’s just amazing what they can do nowadays,” he said. “They didn’t have all of this technology back in the day. Who knows what would have happened?”
“I can’t believe that’s what my heart looks like.”














 /a>
/a>
 /a>
/a>
 /a>
/a>