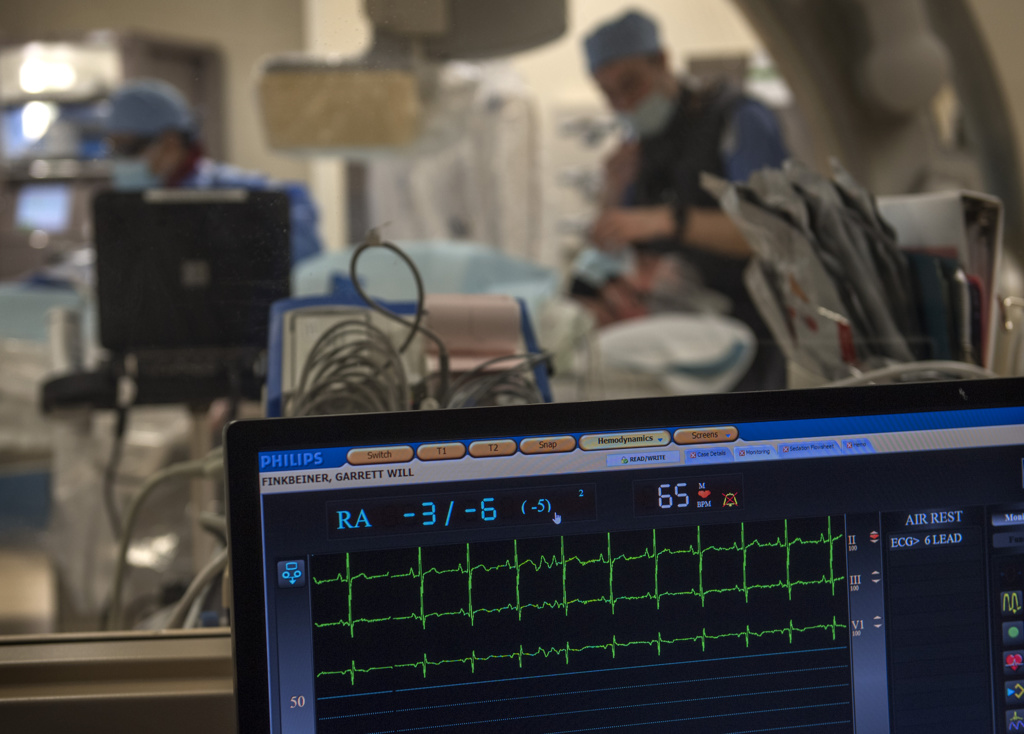
Garrett Finkbeiner has no memory of June 7, 2020, or the days immediately before and after.
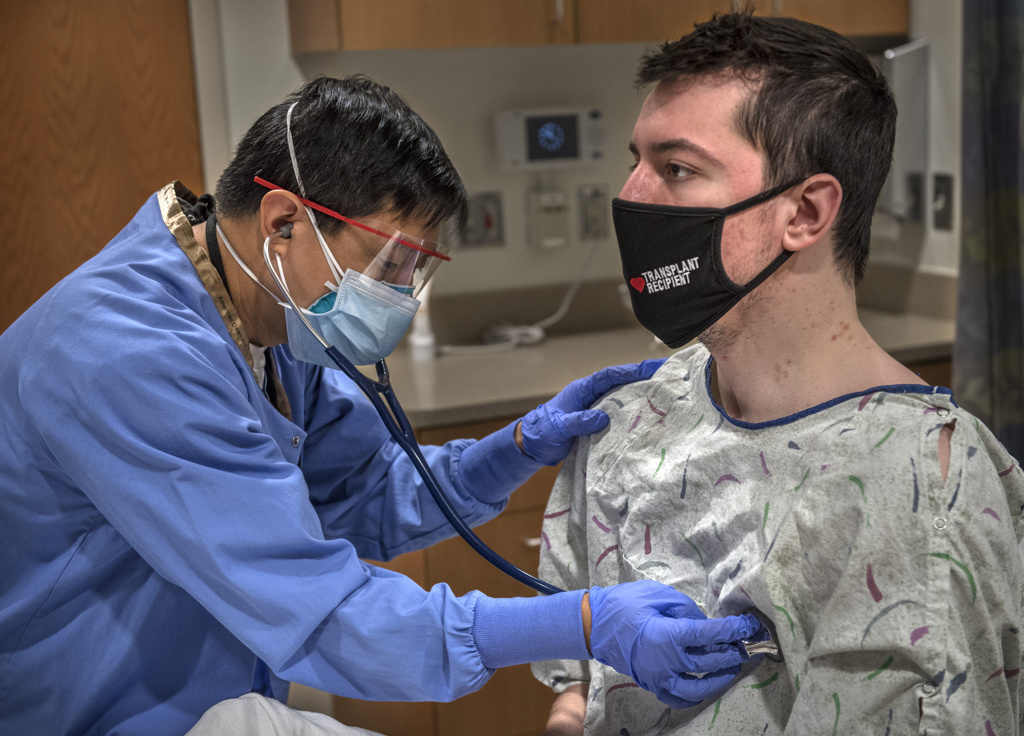
Yet for this former college athlete from Michigan’s Upper Peninsula, that Sunday marks life’s biggest event—the day he received a new heart.
Garrett, then 21, had never given a thought to needing a heart transplant.
Like any healthy, active young person, he had no reason to. His family has no history of cardiac issues, let alone severe heart failure.
All he knew is he’d had abdominal issues since late fall 2019, during his junior year at Central Michigan University.
Nausea. Upset stomach. Trouble keeping his food down.
The situation didn’t improve over time.
Enlarged heart
On an early-March trip to see his family in Marquette, Garrett called his primary care doctor, who referred him to a gastrointestinal specialist at Spectrum Health Big Rapids Hospital, an easy drive from school in Mount Pleasant.
“Basically, we thought Garrett had an ulcer,” said Wendy Finkbeiner, Garrett’s mom.
Garrett’s specialist found nothing wrong with his stomach but clocked his resting heart rate at 130.
Alarmed, she sent him to her colleagues in the emergency department, who ran some scans that revealed a dangerously enlarged heart.
The next morning, the Big Rapids team transferred Garrett by ambulance to Spectrum Health Butterworth Hospital.
There he saw David Fermin, MD, a cardiologist with the Spectrum Health Advanced Heart Failure Program, who diagnosed him with cardiomyopathy and admitted him to the Spectrum Health Fred and Lena Meijer Heart Center ICU.
“His heart was severely enlarged and his function was only about 10%,” Dr. Fermin said. “In addition to that, he had a blood clot in his heart, so at that point he was in severe heart failure.”
Doctors have since attributed the issue to a likely viral infection that attacked his heart, unrelated to COVID-19.
Dr. Fermin started Garrett on medications to strengthen his cardiac function. The cardiology team kept him inpatient for several days.
Tricky timing
Garrett’s hospital admission date happened to be March 12—the tipping point for the emerging coronavirus pandemic.
The timing created a unique set of challenges.
“He really wanted to get out of the hospital, and we were trying to weigh out the risks of keeping somebody in the hospital at that point, not knowing what was going to happen with COVID,” Dr. Fermin said.
Because these drugs can take a few months to work, Dr. Fermin sent Garrett back to Mount Pleasant with a supply of medications and a plan for regular follow-up appointments.
But instead of feeling better, Garrett continued to decline.
“I couldn’t eat. It made it hard to even move off the couch,” he said.
In April, Garrett returned to Butterworth Hospital and learned his life hung in the balance. The concept was terrifying—and difficult to comprehend.
“That’s just a lot for a 21-year-old to try and understand, because it kind of came out of nowhere,” Garrett said.
“I was very (focused) on the ‘could die’ part.”
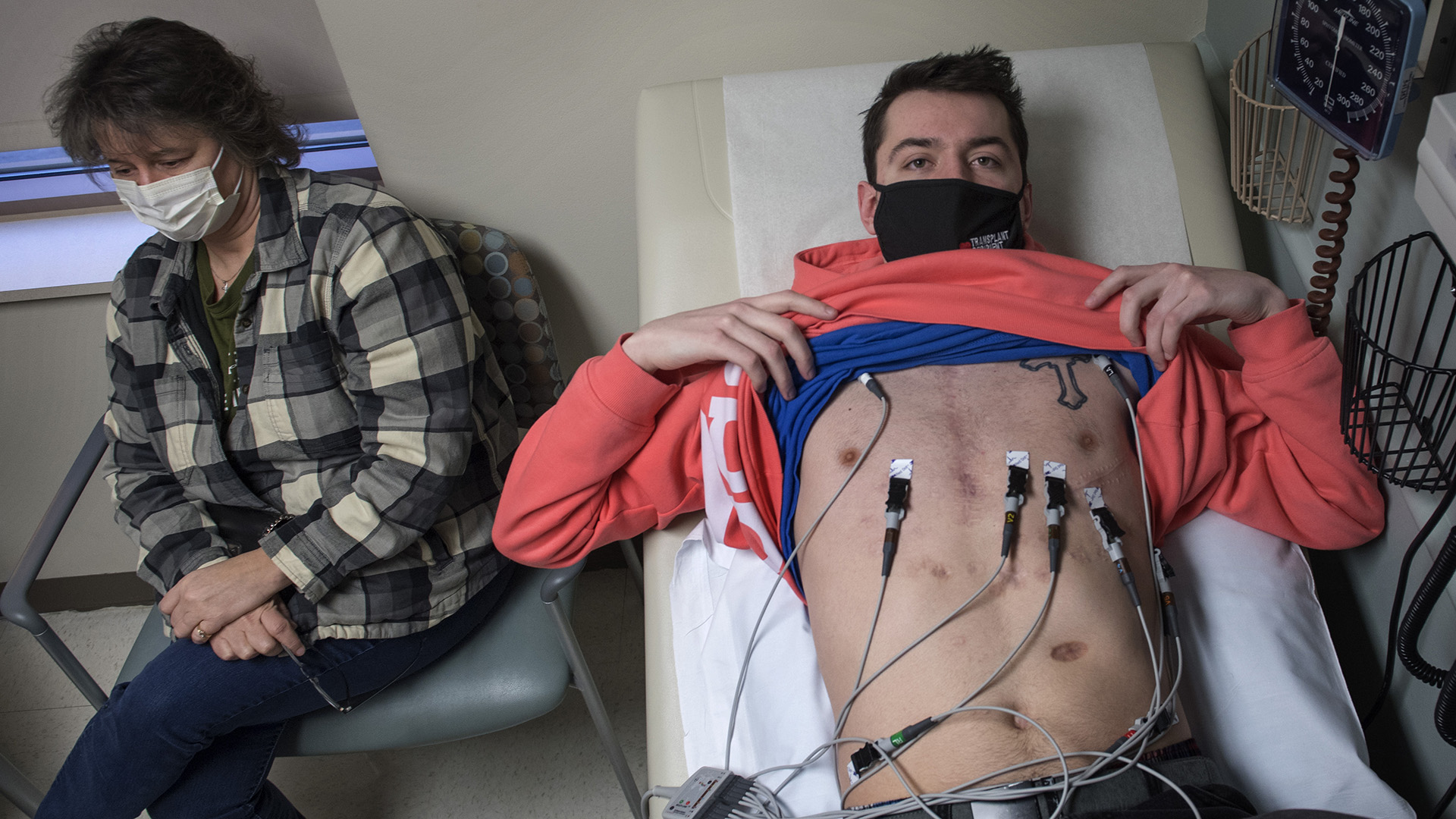
Hearing Garrett was being admitted again, his parents, Wendy and Bill, packed up and made the six-hour drive from Marquette to Grand Rapids—during the strictest phase of the state’s coronavirus lockdown.
“There was nobody on the roads,” Wendy said, recalling the unsettling experience. “When we crossed over the (Mackinac) Bridge, the only car at the bridge was a state police officer.”
Arriving at the hospital, the couple learned COVID-19 restrictions would prevent them from seeing their son, despite his dire diagnosis.
They found themselves in the parking lot, staring up at Garrett’s hospital window, his backpack visible through the glass.
Eventually, because of their son’s age and life-or-death circumstances, they won an exception that allowed them to be with him, one at a time.
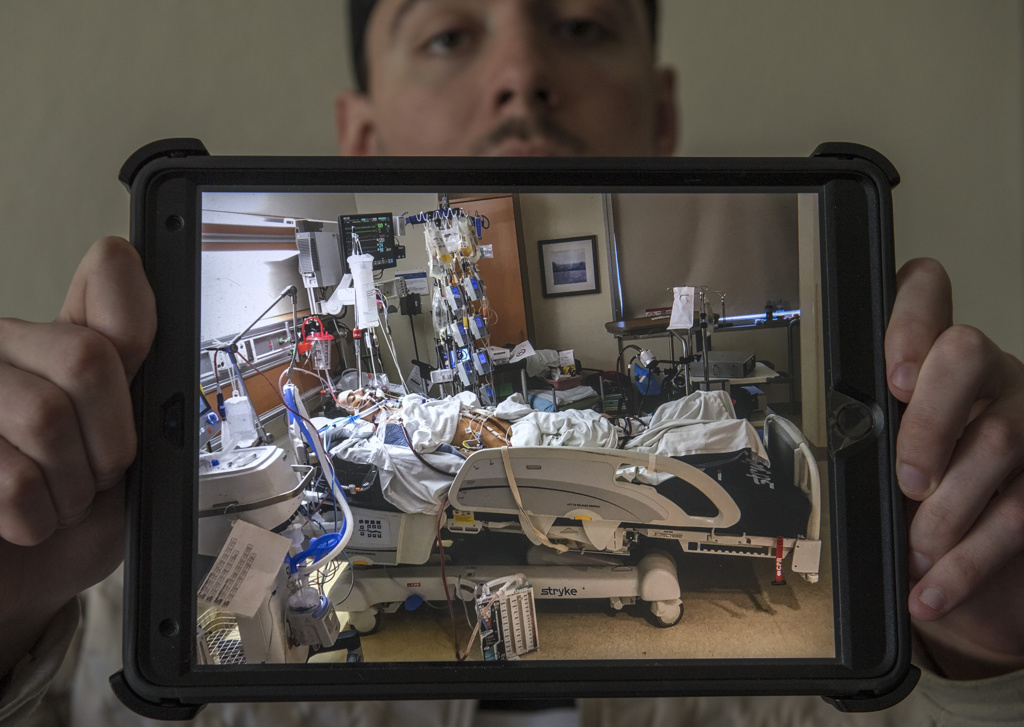
The couple stayed in Grand Rapids—at Garrett’s side—for the next six months as he underwent multiple surgeries, moved in and out of medically induced comas and languished on life support before ultimately sustaining a successful heart transplant.
He traveled an exceptionally rocky road to transplant.
The Finkbeiner family chronicled his journey for hundreds of concerned family and friends on Future for Fink, a Facebook page using Garrett’s nickname.
Exhausting the options
Initially, Garrett did not meet the criteria for a heart transplant. Yet, the advanced heart failure team thought he had a shot at recovering with help from a mechanical heart pump.
In the course of a month, he had a series of emergency surgeries to place various cardiac support devices:
- In April, an intra-aortic balloon pump—an inflatable device inserted via catheter to increase blood flow in the short term
- In May, a left ventricular assist device, or LVAD—a mechanical pump surgically implanted on the left ventricle, in hopes his heart could recover over time
- Soon thereafter, a right ventricular assist device, or RVAD—a mechanical pump placed to support his failing right ventricle
After those, Garrett had additional emergency procedures to deal with bleeding complications. And he spent time on ECMO, a machine that provides support for both heart and lungs.
Before long, it became clear the implanted pumps would not provide the level of support his heart needed.
Recognizing he might never leave the hospital, the Spectrum Health Richard DeVos Heart & Lung Transplant Program selection committee reevaluated him and agreed to list him for transplant.
“When we put him on the second device and there was no recovery from the right side, but he continued to bleed … then we thought that the only option for him was transplantation,” said Marzia Leacche, MD, the cardiothoracic surgeon who performed most of Garrett’s surgeries, including his eventual heart transplant.
“We put him on the list for transplant as a Status 1,” she said.
That’s the highest status for transplant, reserved for the most medically urgent patients.
With Garrett in a coma for much of his time in the ICU, his care team spent more time in consultation with his parents than with him.
Milena Jani, MD, an advanced heart failure specialist, developed a close connection with Wendy, Garrett’s mom.
“She was broken, but she had so much faith,” Dr. Jani said.
“When we gave them the news that he was going to be listed for transplant, I think that family … felt as if we told them Garrett is going to have a second life.”
Five days later the team selected a donor heart for Garrett.
Dr. Jani had the privilege of delivering the news.
“I was on call when we found the perfect heart for Garrett,” Dr. Jani said.
“I was crying when I went to her, and at that time we still had to wear a bunch of masks and a bunch of shields … but she could see me and I could see her.
“It was so emotional.”
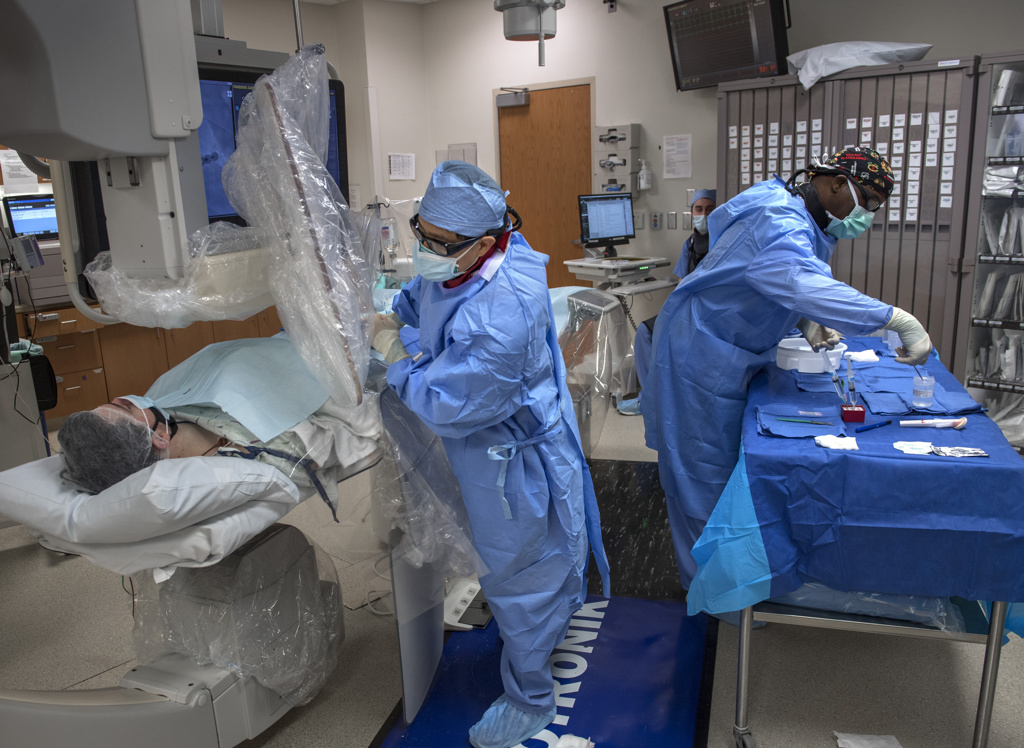
The surgical team, Dr. Leacche and Theodore Boeve, MD, performed the transplant in a 14-hour surgery that involved first removing both VAD devices before placing the donor heart.
The outcome brought elation and relief.
“He did exceptionally well with the new heart, despite it being a very difficult situation,” Dr. Leacche said.
“And the result is exceptional. He’s doing very well.”
Resilience
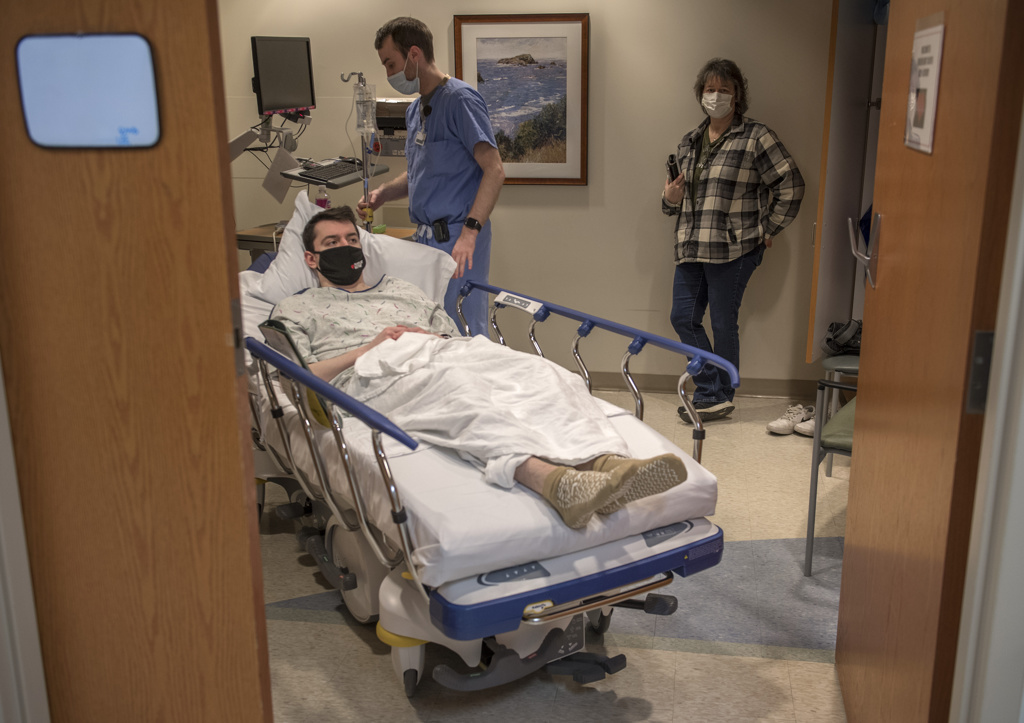
After a grueling two-month recovery that required him to relearn how to eat and walk, Garrett transferred to Mary Free Bed Rehabilitation Hospital for a short stay.
Upon his discharge, Garrett joined his parents in a local apartment. For the next four months, he stayed in the area to attend frequent post-transplant appointments. His two siblings continued to keep their mom’s business running in Marquette.
The first time Dr. Jani saw Garrett walk into the transplant clinic last fall, her jaw dropped.
“There he was, looking perfectly normal, perfectly handsome, perfectly like nothing had happened to him,” she said.
“He had bounced back to his normal level.”
By December, Garrett had progressed so far that Dr. Jani allowed him to go home to the Upper Peninsula for the holidays.
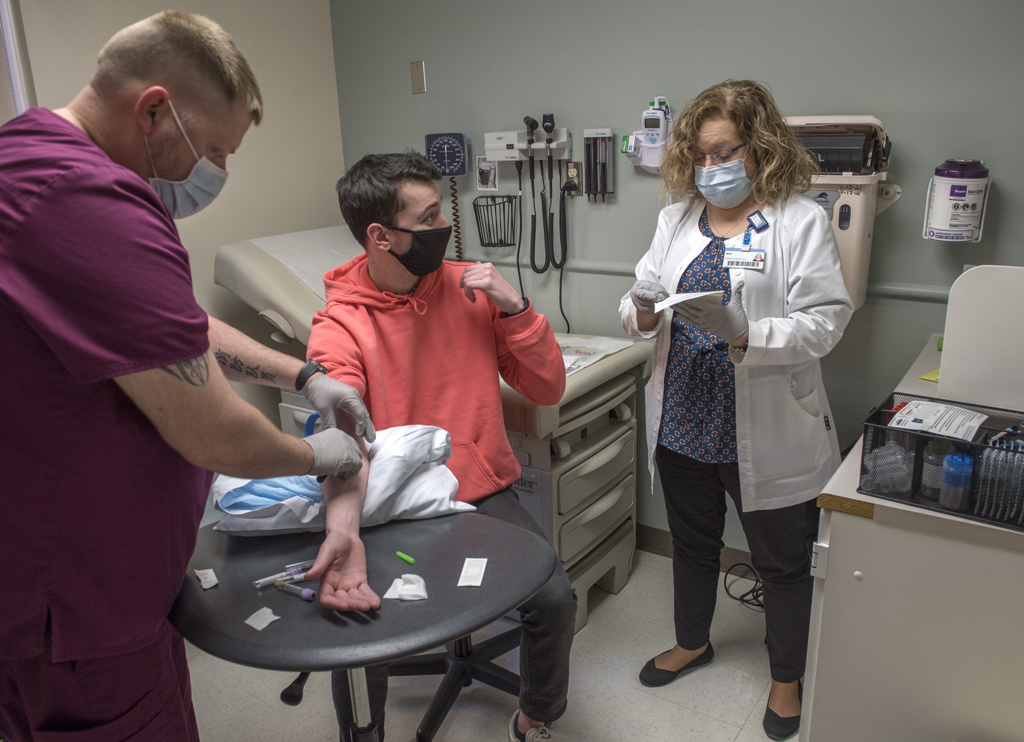
In January, he returned to Mount Pleasant to resume work on a bachelor’s degree in sports management.
Garrett lives on his own now, with his young husky, Zeke. He meets up with his parents in Grand Rapids for regular clinic visits.
Amy Galle, Garrett’s post-transplant coordinator, gives Wendy and Bill credit for much of their son’s success.
“They’ve been phenomenal,” she said. “They have been with him every step of the way … and without that kind of unwavering support, transplant may not have been an option for him.”
In the lead-up to transplant, Garrett was sedated and unable to verbalize his desires, she explained.
“Being able to see how steadfast and reliable (his parents) were helped to make the team feel more comfortable.”
Garrett deserves kudos for his resilience and maturity in the face of life-changing events, Dr. Leacche said.
“You know, he came in as a young man. He came in, he was in college, like any college student. But then when he left the hospital, he was an adult,” she said.
“It’s very remarkable the maturation that he had done during this very hard time.”
For his part, Garrett is still coming to grips with everything he’s been through.
“It’s kind of a process, I think,” he said. “And I’m still in the middle of it.
“I think the main way … is just talking about it but trying not to overanalyze things.”
He’s grateful for the dozens of people who helped keep him alive during his months in the ICU.
“For him to be where he is today is just—it’s his will to be alive and his parents’ support and the team that worked with him,” Dr. Jani said. “He has made us extremely proud.”



















 /a>
/a>
 /a>
/a>
 /a>
/a>
What an amazing story. Faith carries you a long way. I hope you continue to strive with your new heart.
Praise God! Continued prayers for Garrett and his amazing family. We love you! 💕
A traumatic experience with a positive outcome shows what faith, family, community, and outstanding healthcare providers can do together. This family’s strength and Garrett’s resilience are an inspiration.
I am praying for you Garrett Finkbeiner we love you I hope you doing well
What a wonderful story. Wendy & Bill you and Garrett are so remarkable and we are so happy for you all because this was definitely a family affair.
What a amazing journey. I am praying for you Garrett!