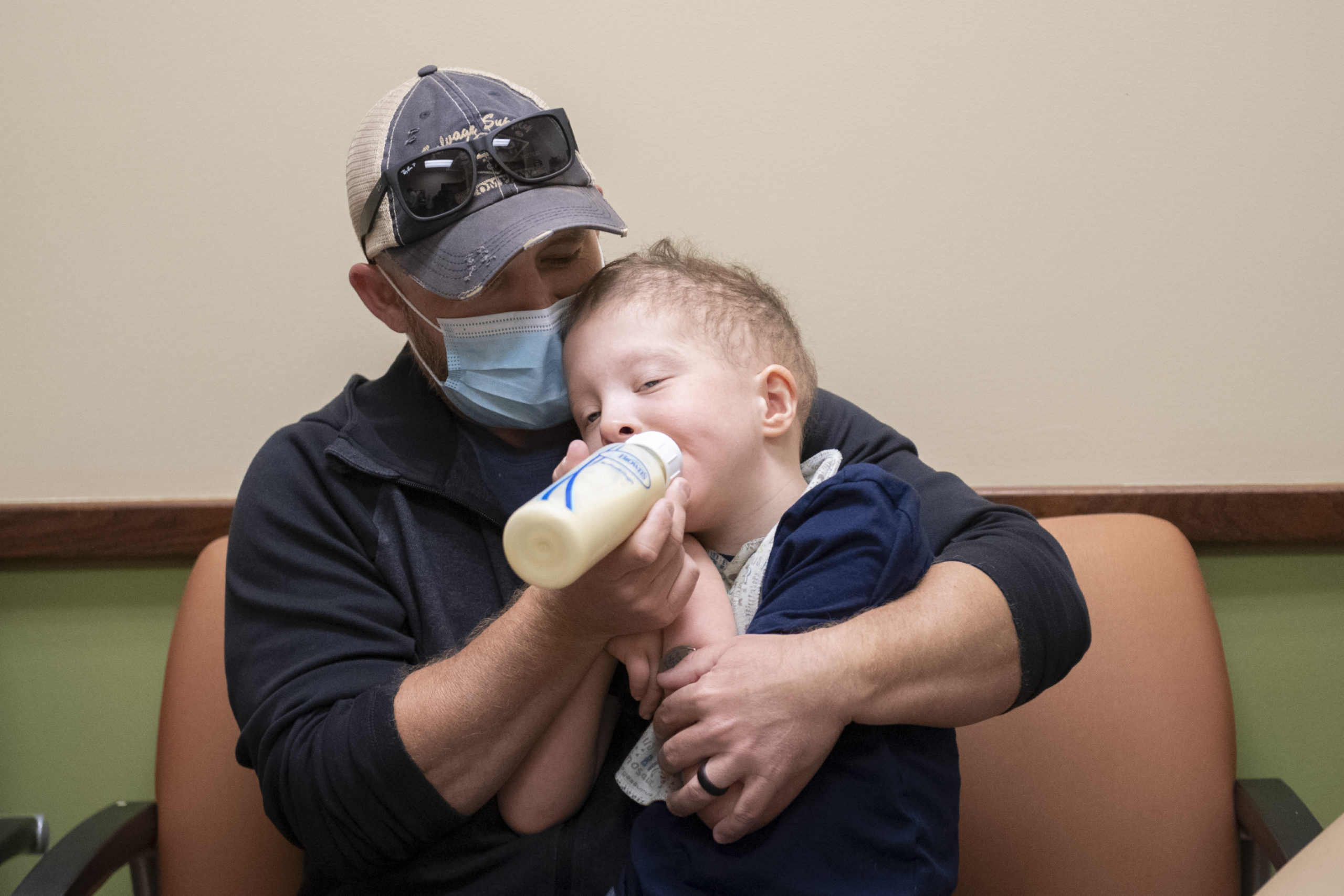
Editor’s note: Spectrum Health requires patients and visitors to wear a mask at all facilities. In this case, however, Jameson Jibben is medically unable to wear a mask.
Darren and Kayla Jibben, of Sacramento, California, began their search for answers for their son Jameson’s rare disease shortly after birth.
Countless visits with doctors and specialists, only to hear it isn’t anything anyone has seen before.
They were looking for answers. Anywhere.
Their son, Jameson Jibben, now 7, had unique health symptoms that seemed to stump doctors.
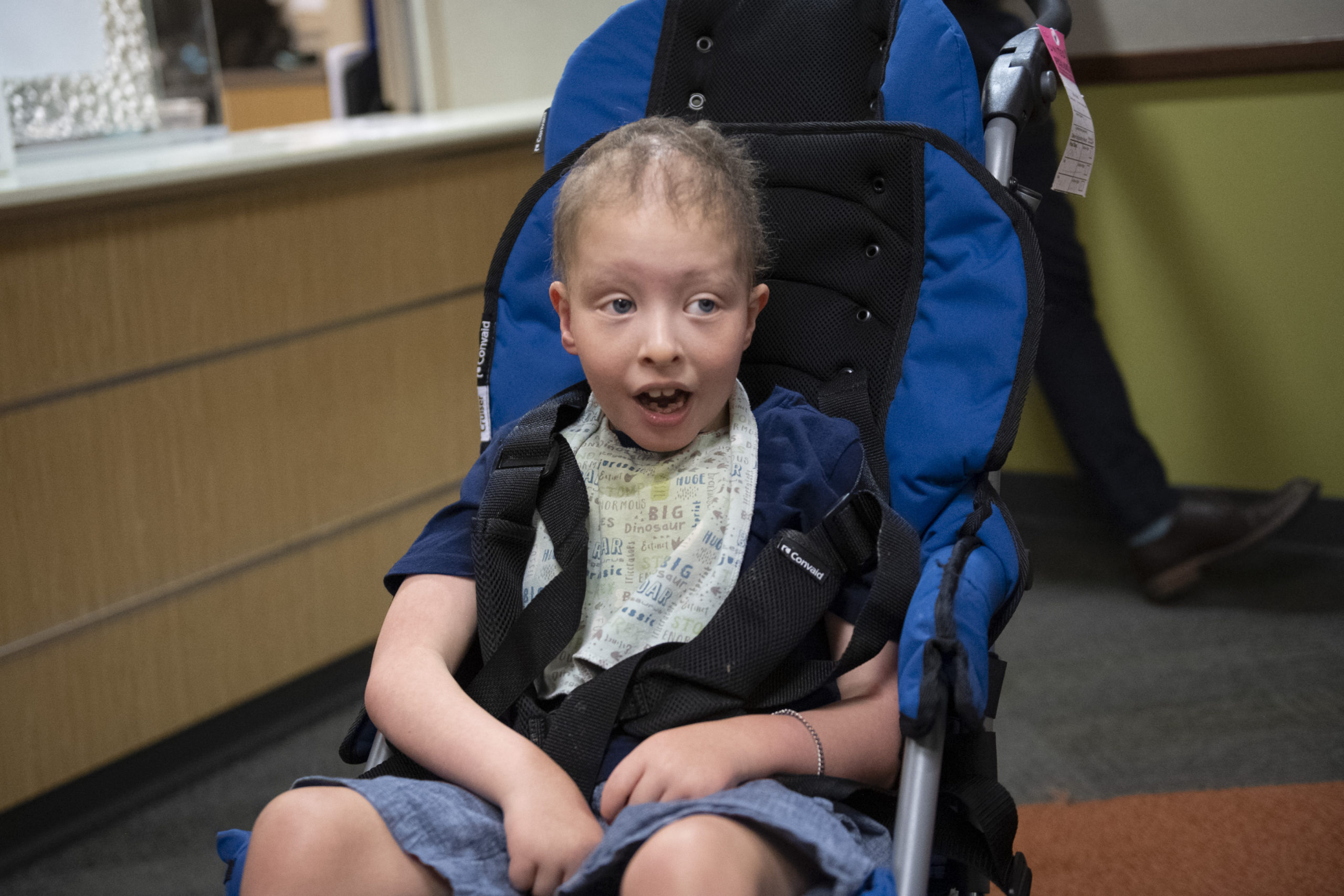
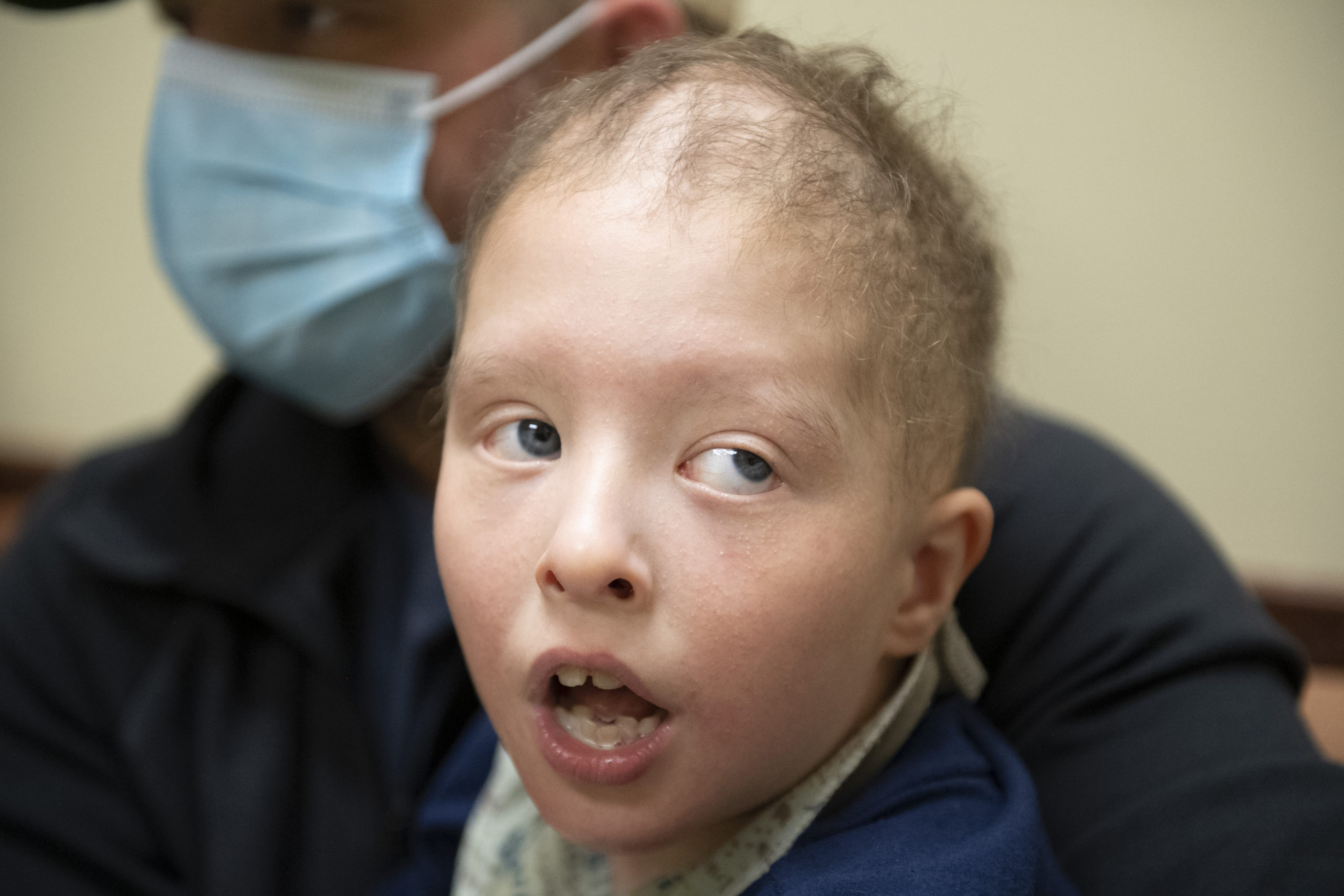
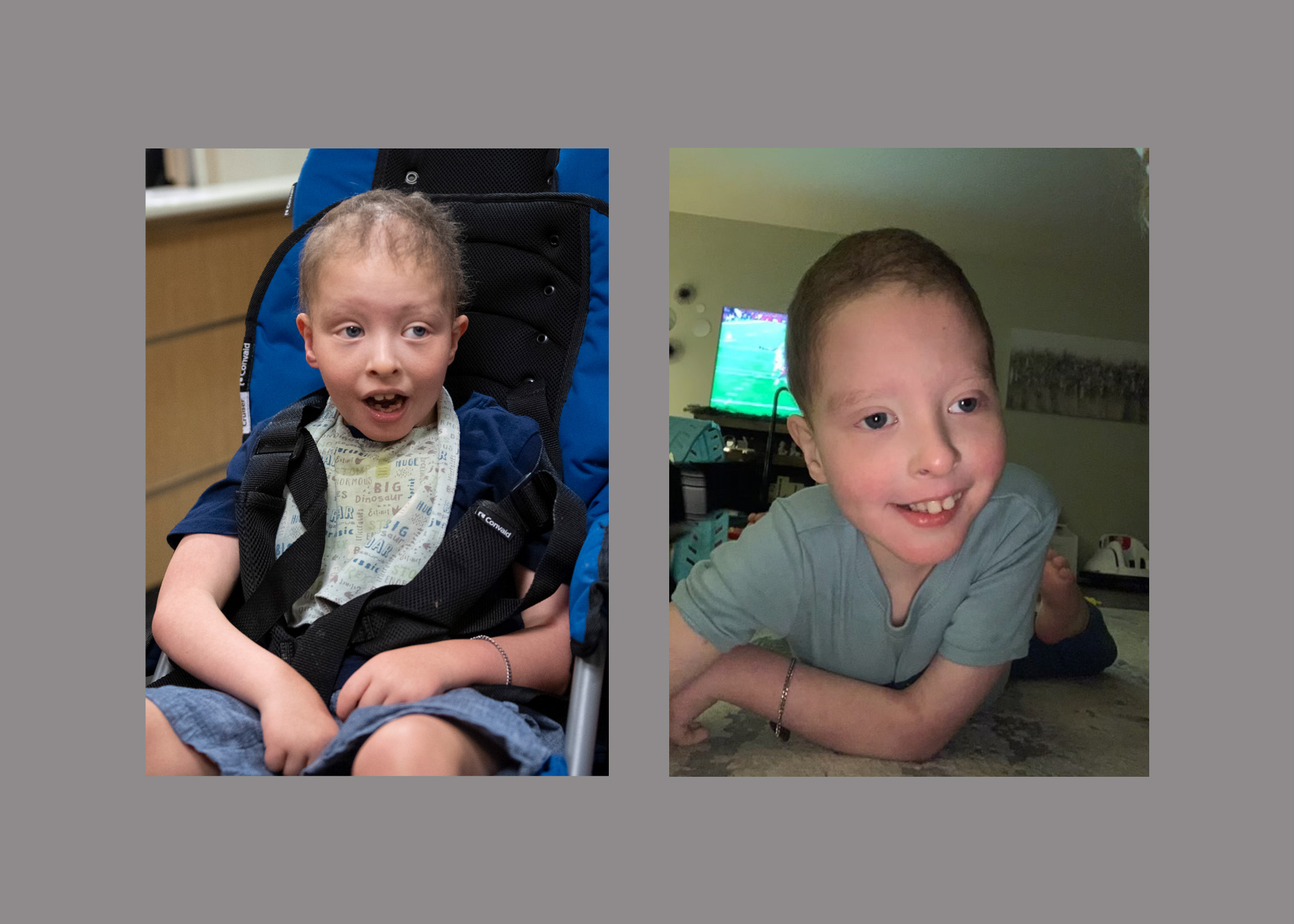
Limited mobility. Developmental delays. Little to no hair on his head. No eyelashes or eyebrows.
Darren and Kayla had genome sequencing done on Jameson in 2019 through the Undiagnosed Diseases Network in hopes of learning more. Whole-genome sequencing looks at the entire genetic code, billions of nucleotides, to uncover genetic influences on a disease or population.
They received a diagnosis in June 2020.
The genetic testing revealed a mutation in Jameson’s ODC1 gene, which is involved in processing polyamines, compounds important to development and growth. It all pointed toward a rare condition called Bachmann-Bupp syndrome.
“The very first thing I did was Google Bachmann-Bupp syndrome,” Kayla said.
“We came across news stories of another little girl in Michigan—Marley—who had the same symptoms and condition.”
In 2019, Marley Berthoud became the first child diagnosed with this condition.
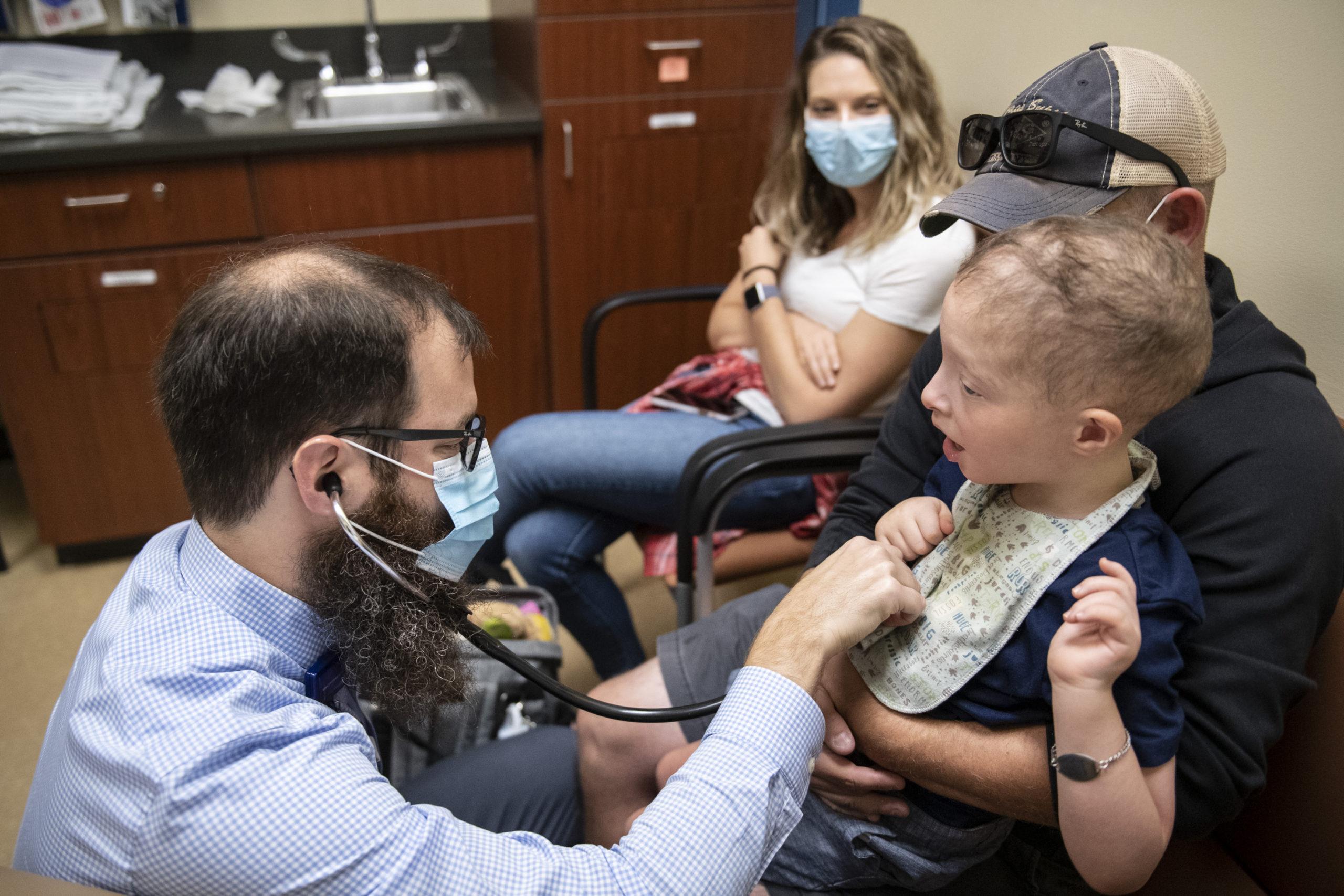
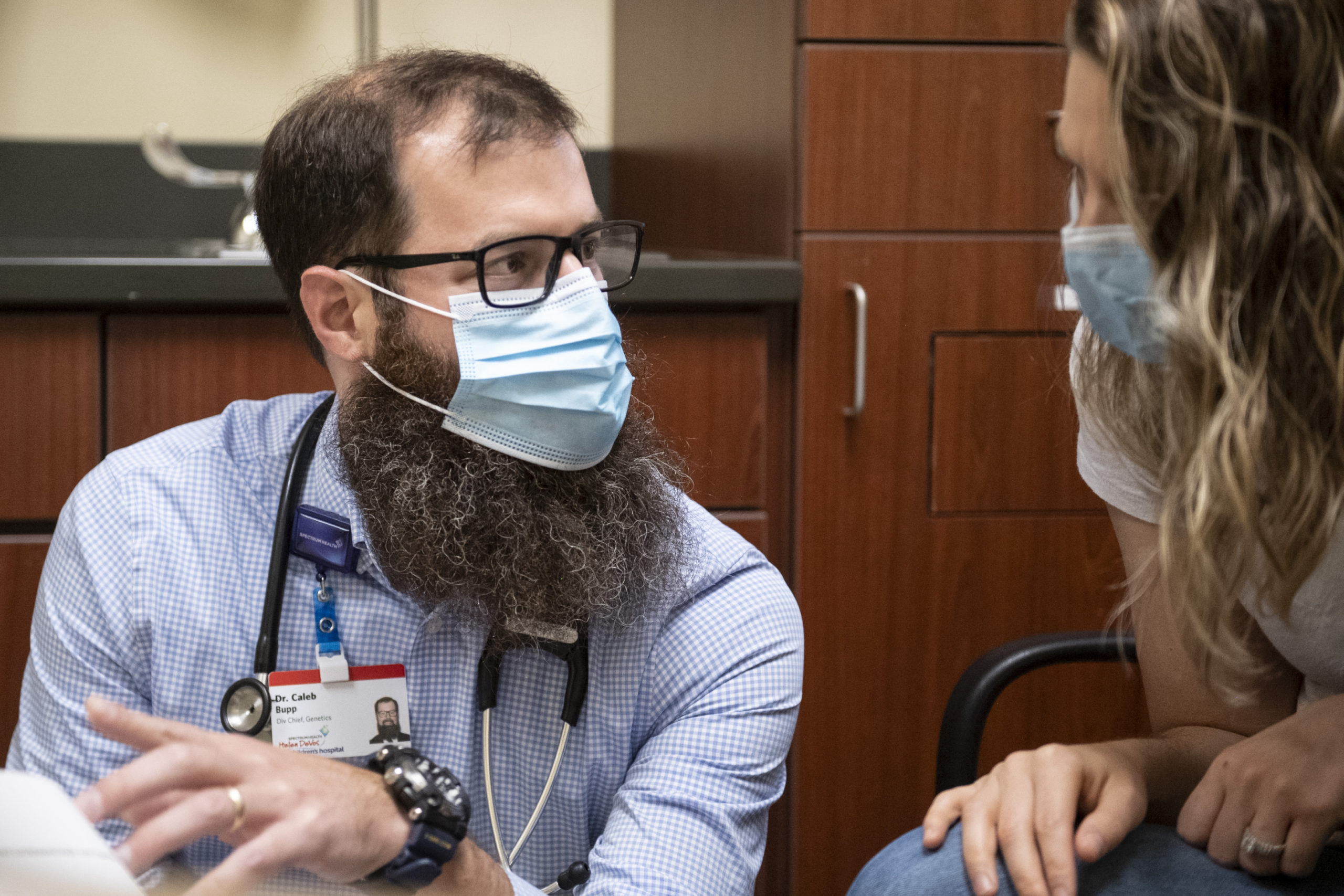
Spectrum Health division chief for genetics Caleb Bupp, MD, and his team at Spectrum Health Helen DeVos Children’s Hospital treated her.
Marley saw amazing outcomes on treatment with difluoromethylornithine, a medication well known for treating tropical diseases. Also known as DFMO, it has been in use for pediatric neuroblastoma and colon cancer and is also used in treating sleeping sickness.
Kayla said it really hit home when she saw pictures of Marley.
“They looked so similar,” she said. “The fact that we knew we were not alone in this journey is pretty incredible.”
Darren and Kayla reached out to Marley’s parents and were soon introduced to Dr. Bupp.
A dose of hope
The Jibbens were determined to get the same treatment for Jameson that appeared to be working so well for Marley.
Their journey led them to West Michigan.
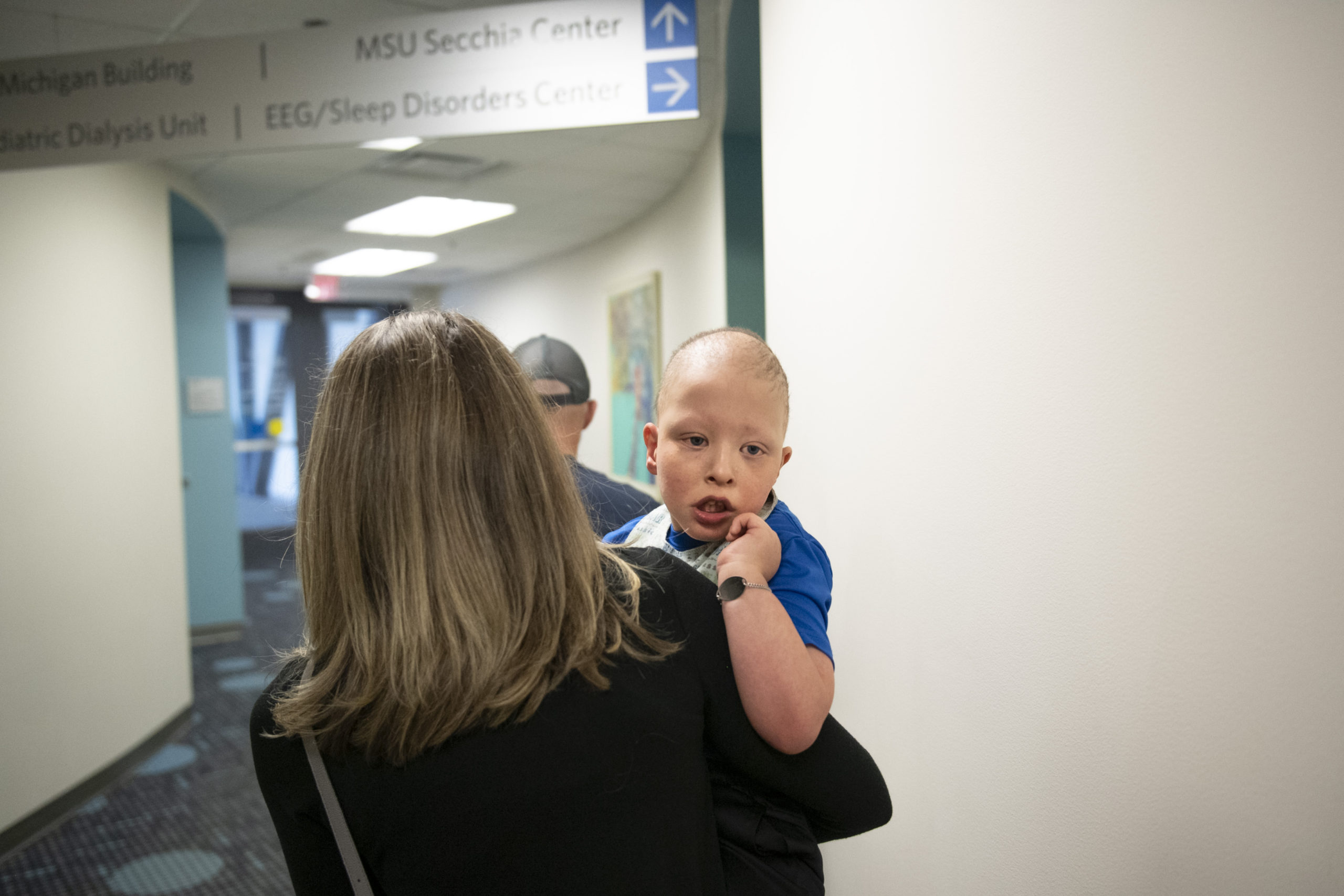
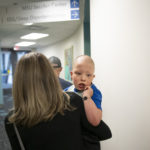
In April 2021, they get off the plane in Grand Rapids and headed directly for Helen DeVos Children’s Hospital for their first meeting with Jameson’s new care team.
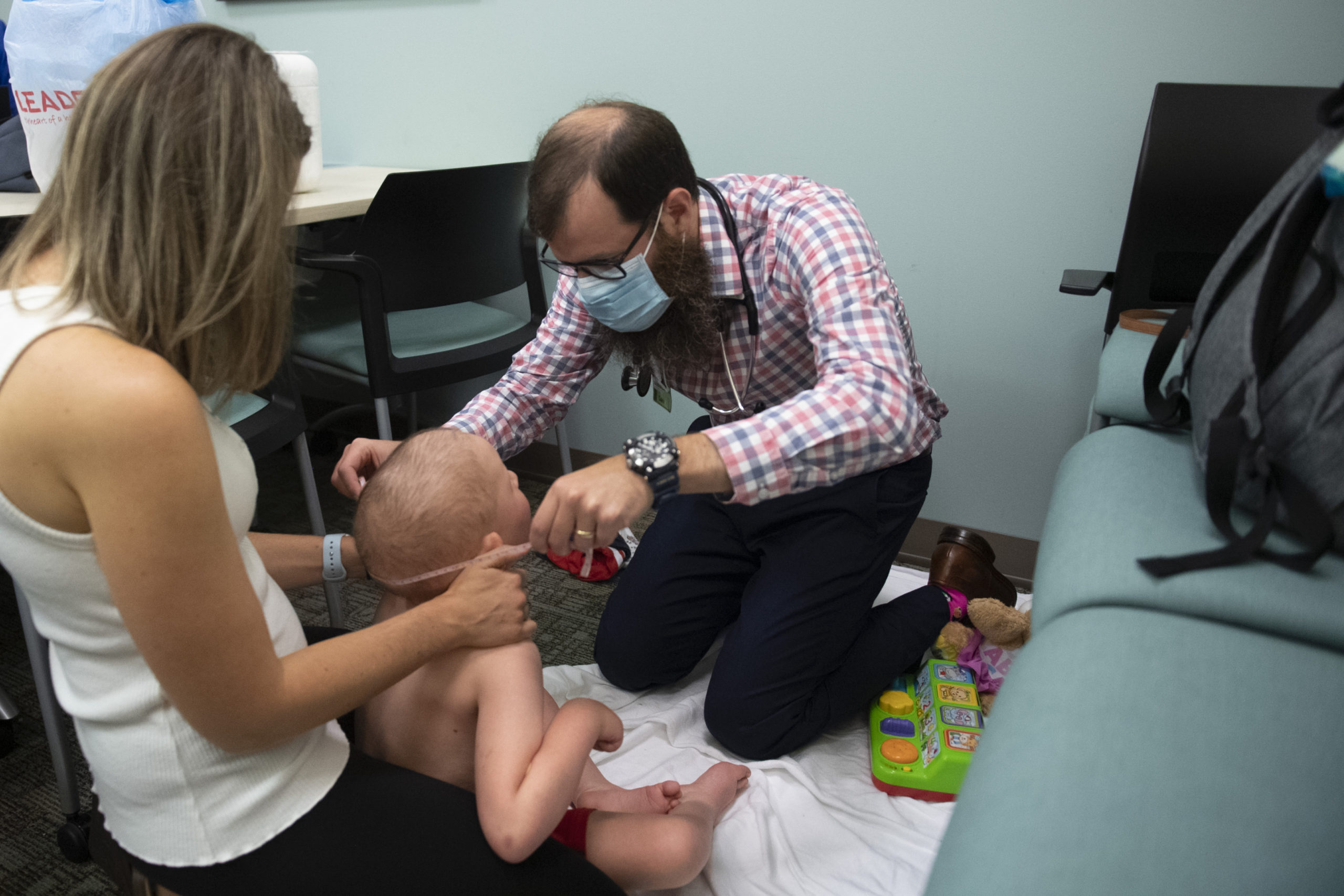
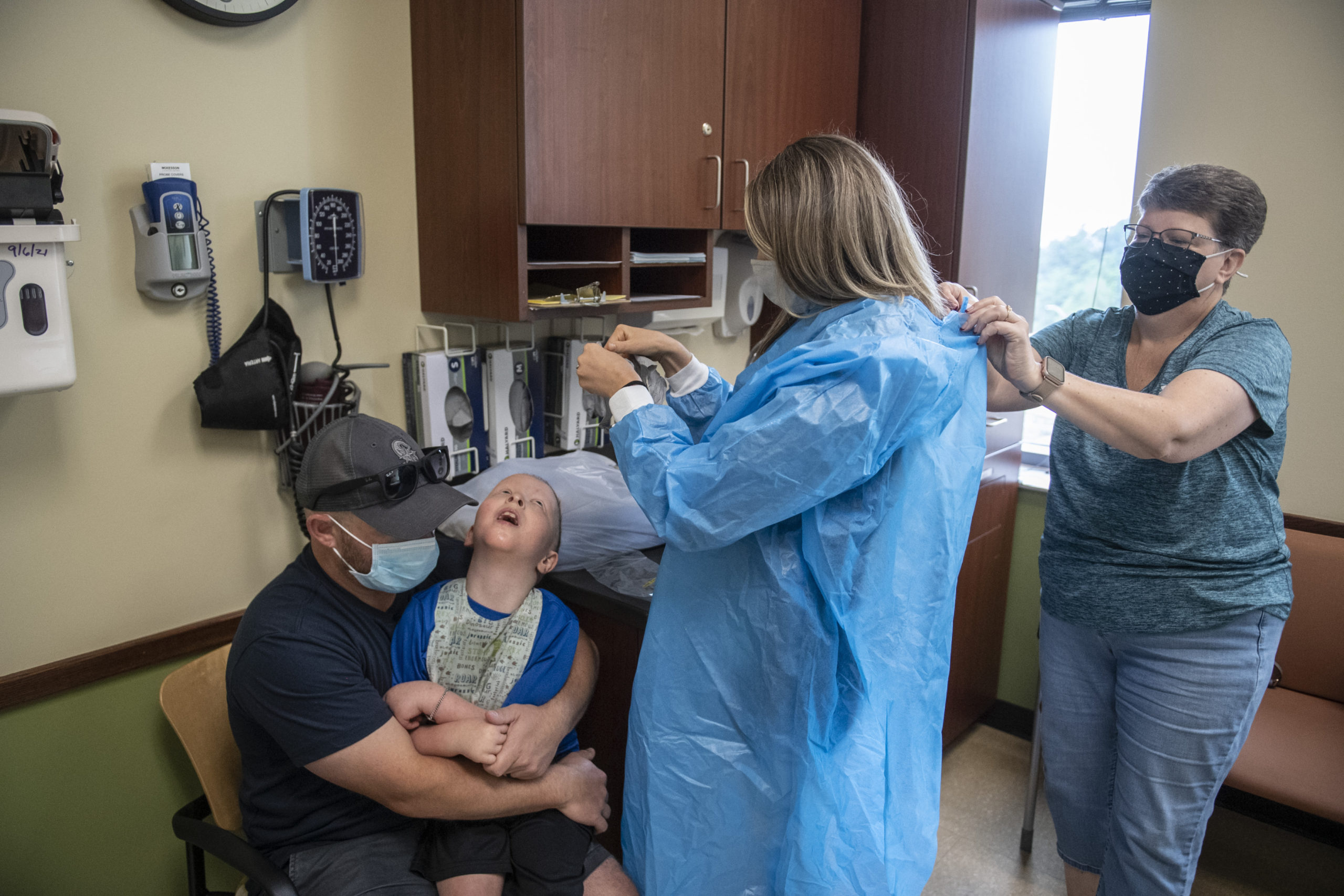
He had a full day of appointments scheduled—physical measurements, dermatology checks and more.
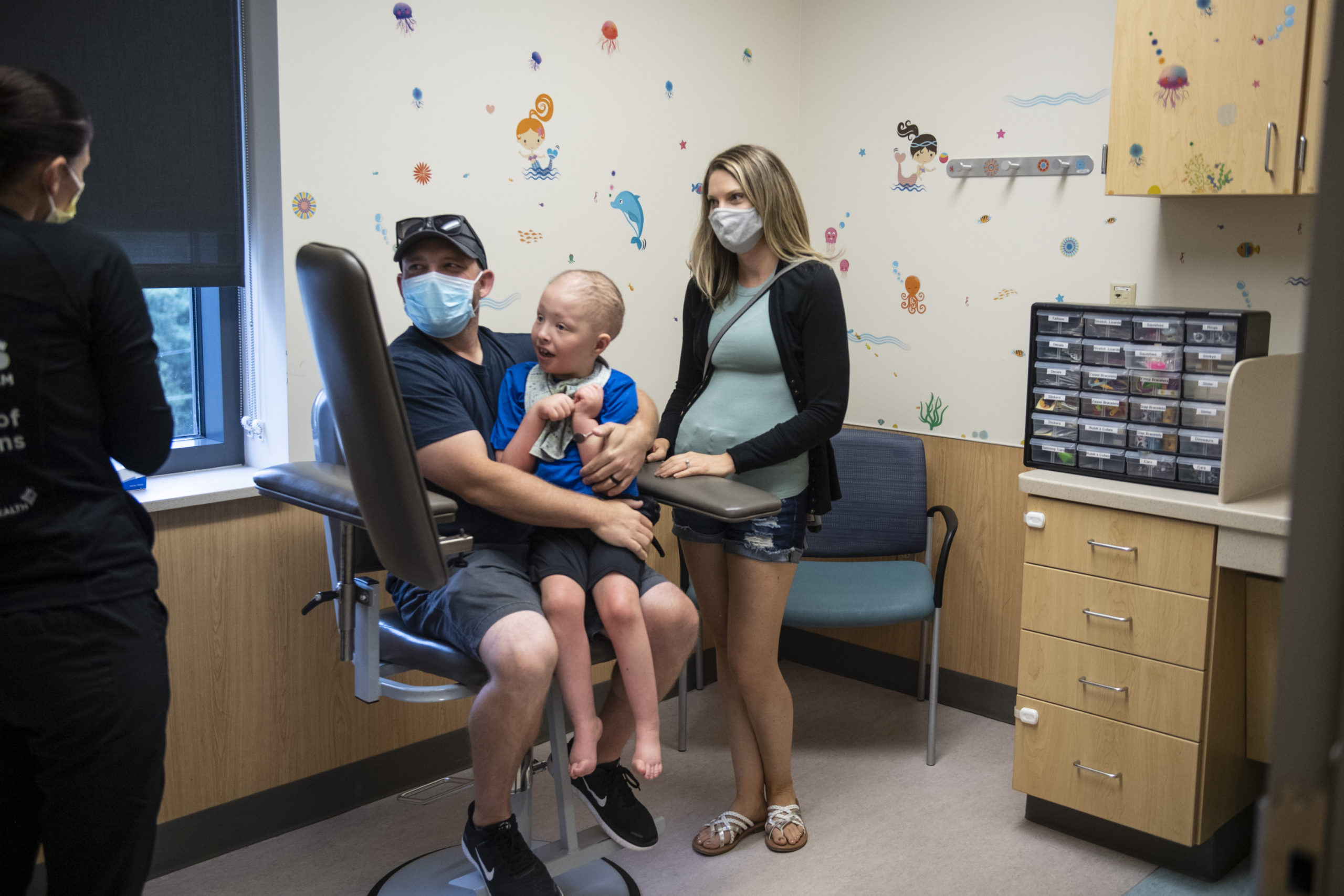
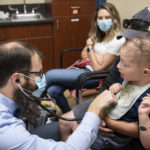
A pediatric dermatologist entered the room to check his skin and the tiny hair follicles on his head. A research team gathered at a table to chart his progress.
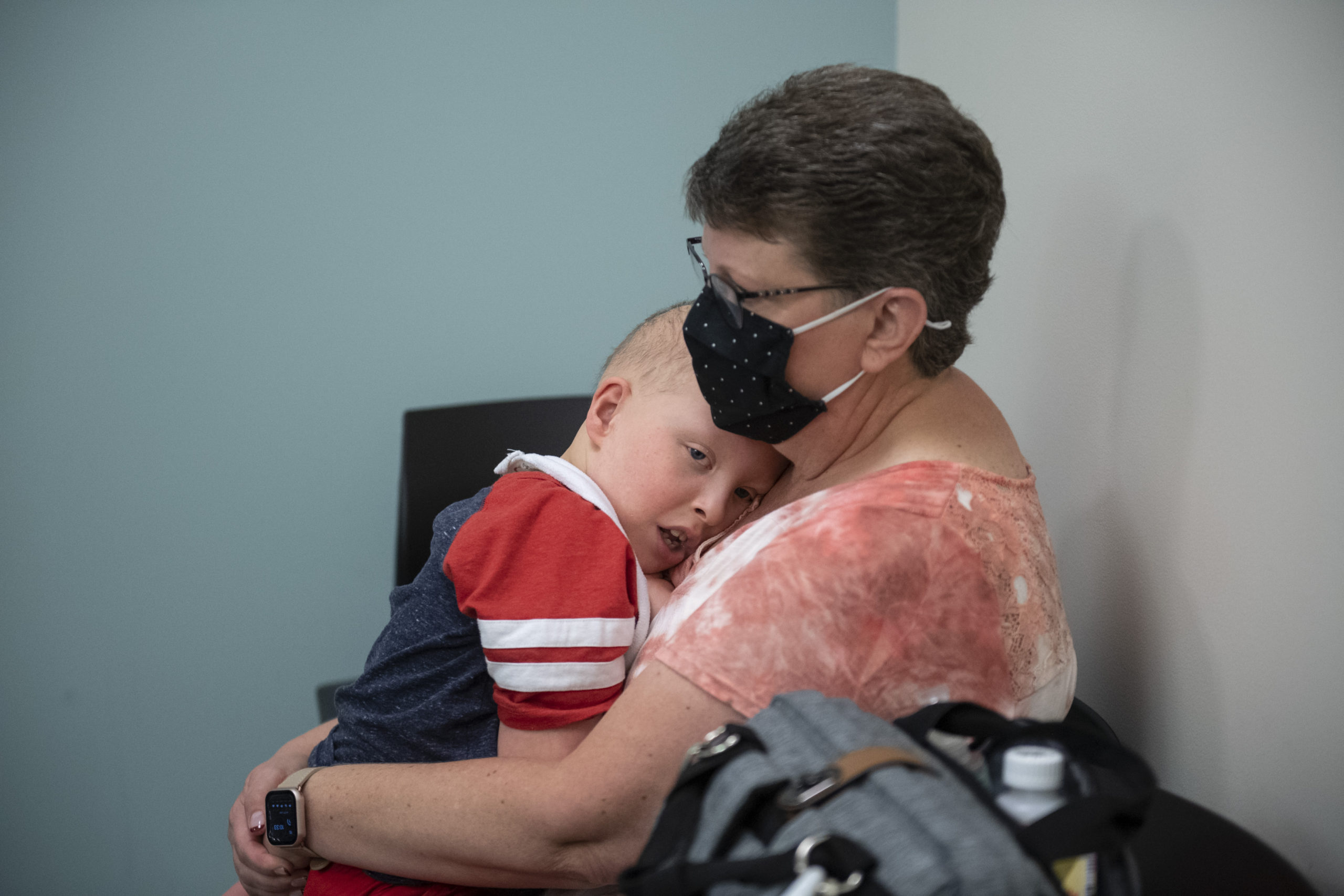
Jameson smiled and let out a squeal.
“His new thing is making noise,” Kayla said. “He has quite a strong voice.”
He’s a little love bug, his mom said.
“He loves to tell everyone hi as they walk into the room,” she said. “And I mean everyone.”
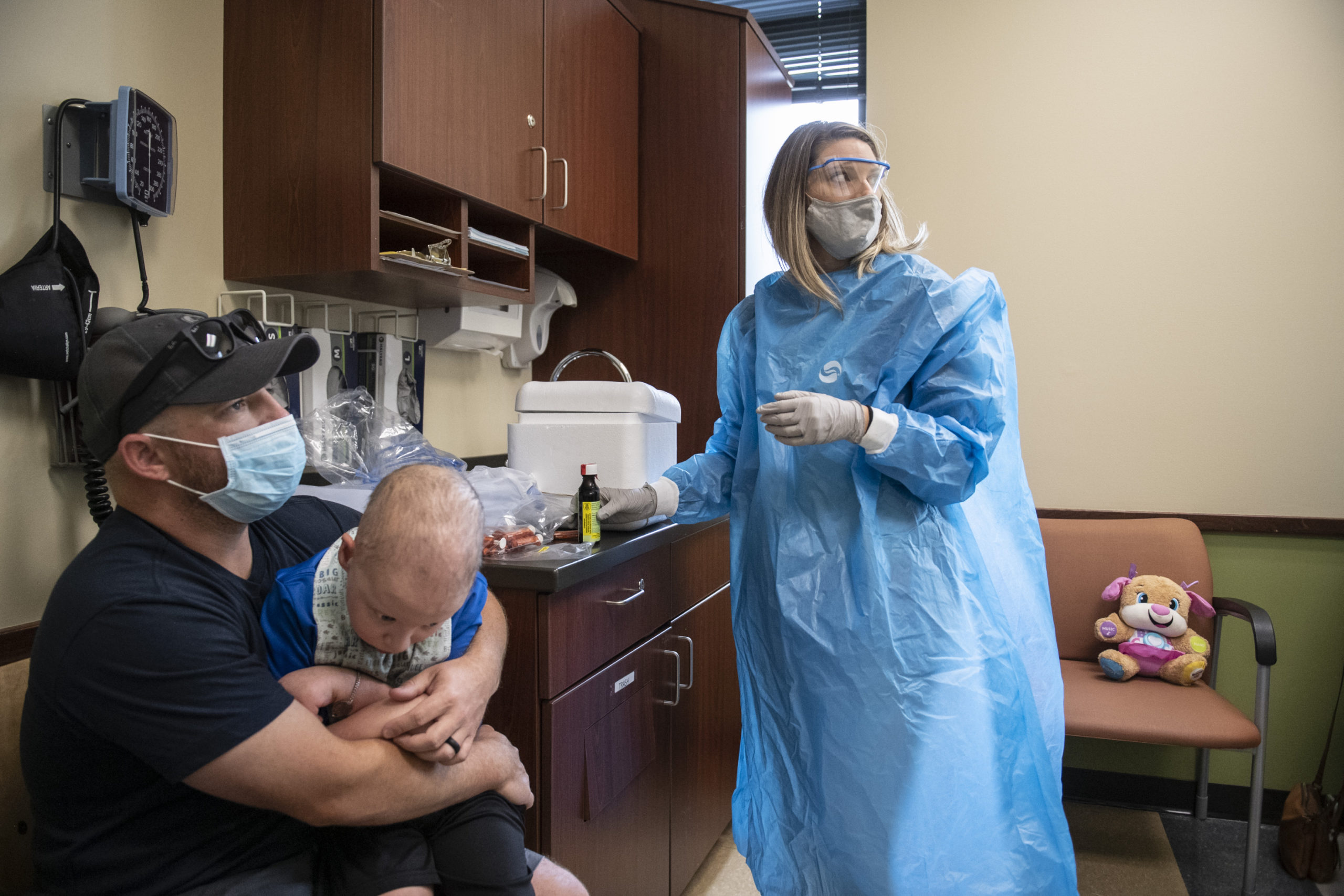
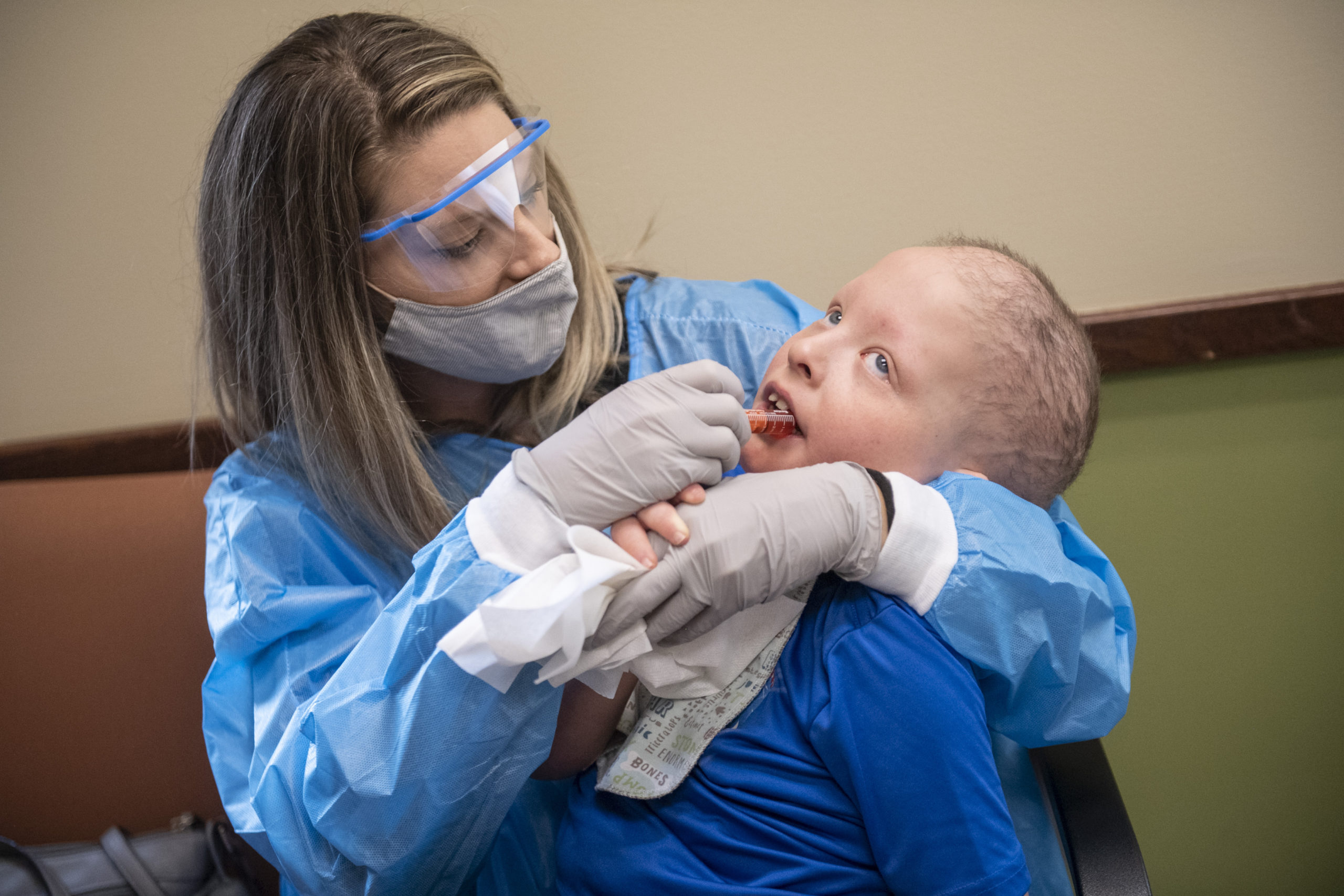
Jameson’s next visit would be in July 2021, when he would get his first dose of difluoromethylornithine, marking the start of his treatment.
The family would return to Michigan every three months for checkups and to increase dosage.
“We’re getting answers, but we really don’t know the cause of any of this,” Kayla said. “We know that with genetics there are so many things that can make an impact, so we might never know.”
If Jameson’s health journey mirrors Marley’s, the Jibbens have much cause for hope.
Marley’s treatment has progressed quite well.
Dr. Bupp says DFMO is an interesting drug and is well-suited to kids with this condition.
“It acts in this pathway in a way so uniquely suited to Marley and Jameson’s condition,” he said.
How it works: The gene is essentially broken and stops working, causing toxic polyamines to build up in the body. The drug helps the excess to be cleared very quickly.
“Most genetic changes will cause a gene to stop working,” Dr. Bupp said. “The gene is in overdrive—and that puts you in a position where you can cool the system down with a drug and get rid of the extra gene product.”
In Marley’s case, Dr. Bupp said his team was fortunate the drug proved so effective.
“For Marley, many of her abnormalities got better when she started on the drug,” he said.
She grew eyebrows, then eyelashes, and now has a full head of hair.
“She sits, scoots, uses sign language,” Dr. Bupp said. “The developmental progress she has made is outstanding.”
He hopes, in time, the same will happen for Jameson.
‘Definitely working’
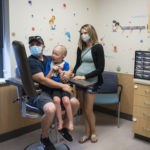
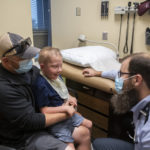
Three months after the first dose of treatment, Jameson and his family returned to Michigan to track his progress.
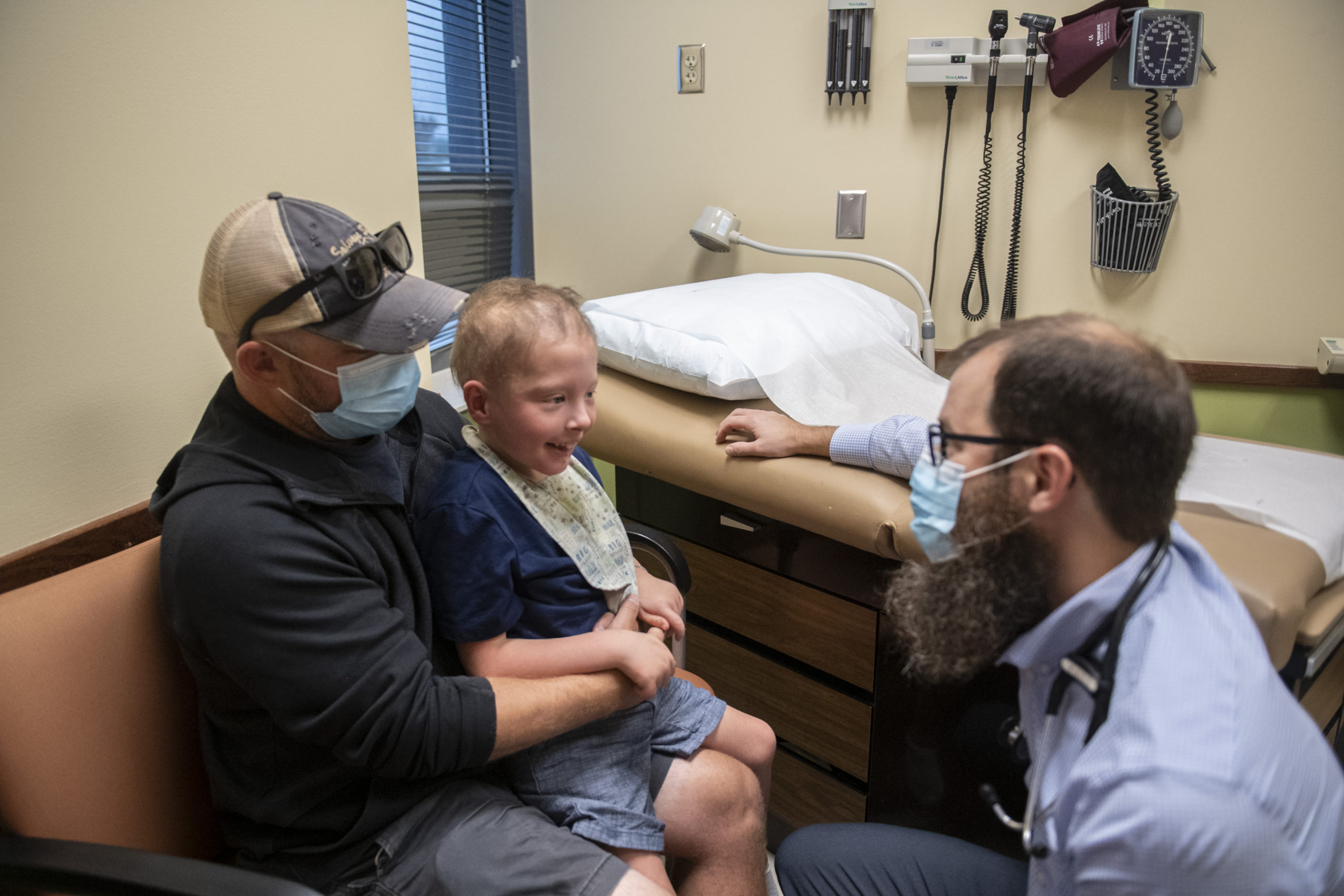
Jameson looked happy and, true to form, offered a friendly hello to all who entered his room.
He had learned the “Wheels on the Bus” song and seemed to be picking up on things much quicker.
He could sit up on his own and walk in his gate trainer. His muscle tone had improved.
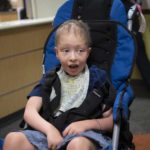
He also had hair on his head. He had eyebrows and eyelashes, too.
“The medicine is definitely working,” Dr. Bupp said.
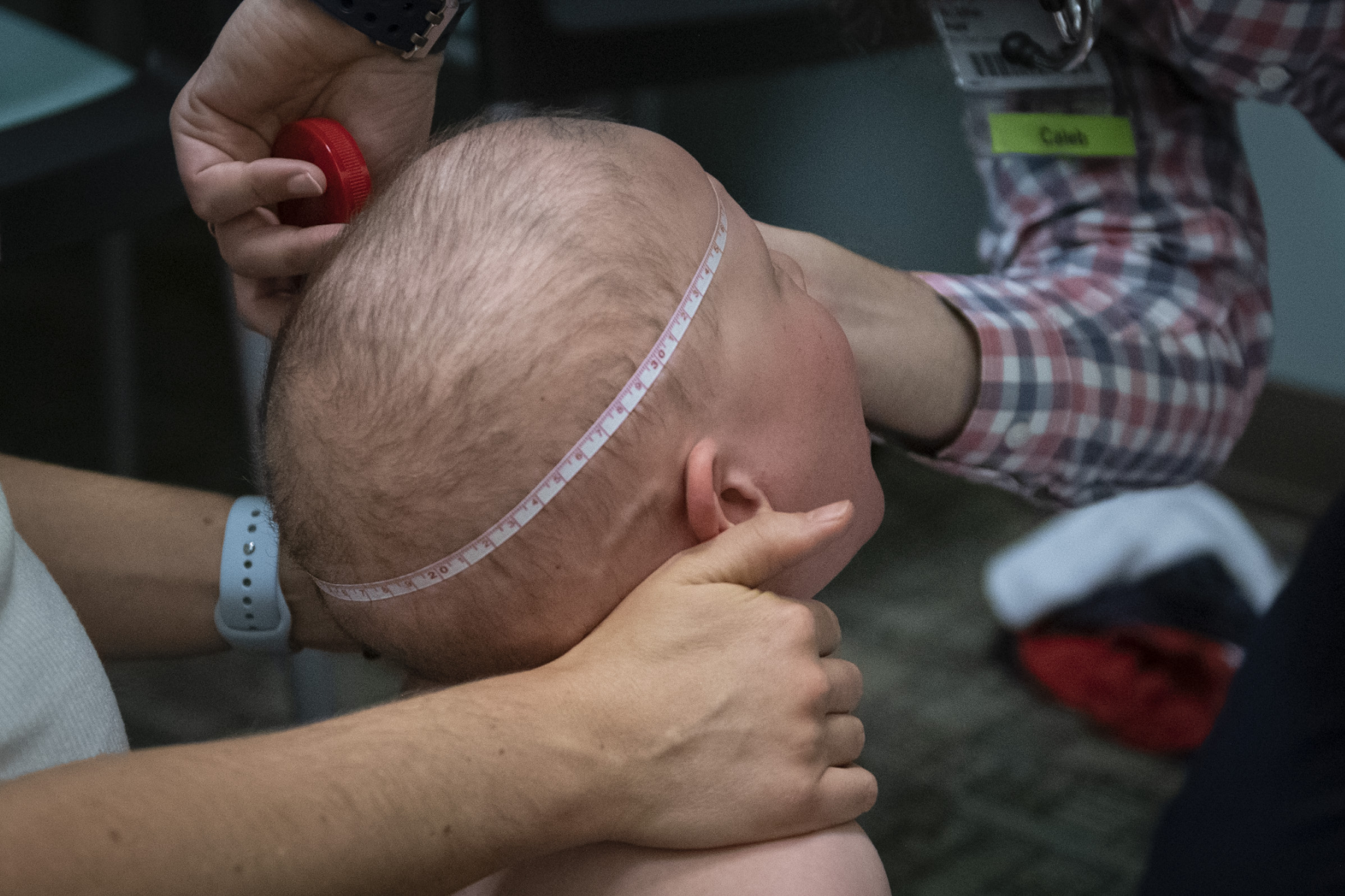
As the doctor measured Jameson’s height and weight, the little guy cooed cheerfully.
“He’s giving us the business this morning,” Dr. Bupp joked.
“The hair on his upper lip is going to turn into to a full-on mustache pretty soon,” Kayla said. “He’s got some pretty sweet sideburns, too.”
Hair growth isn’t the only win for Jameson. Kayla and Darren said they’ve had some luck potty-training him, too.
“I never really thought this would be a possibility,” Darren said. “You can tell he’s proud of himself. The toilet in our room is right in front of the TV. He’s got it made.”
Jameson will now focus carefully and look you right in the eye. His eyes used to wander and he would have trouble focusing. He loves waving with his hands open and clapping too.
Dr. Bupp said all his labs are looking good and he’s not seeing any side effects from the medicine.
‘A lot to say’
By January 2022, Jameson had been on difluoromethylornithine for six months.
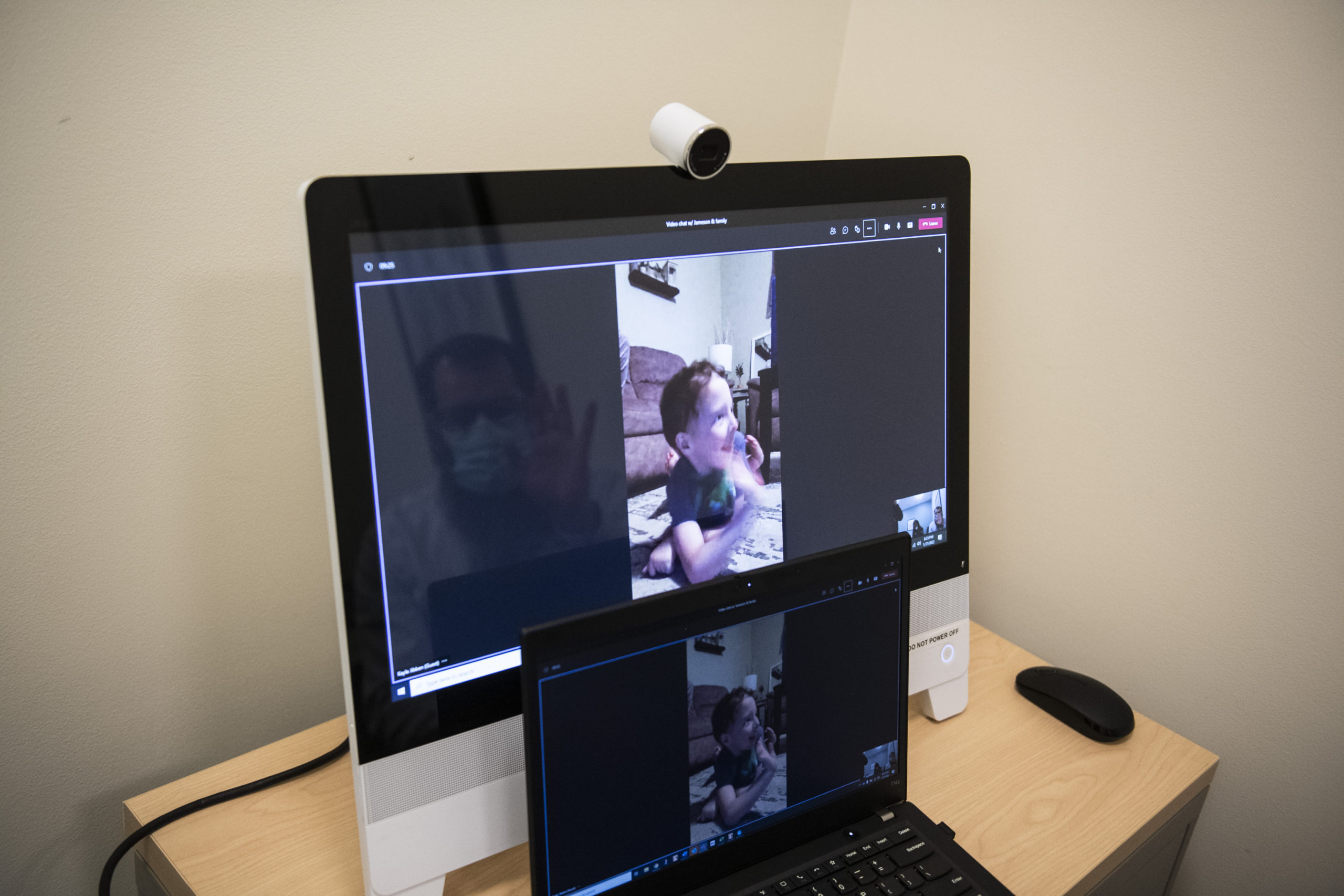
For his next visit, he and his family stayed in California and connected virtually with Dr. Bupp and Julianne Michael, a genetics counselor at Spectrum Health. It saved them a frigid January visit to Michigan.
“Look at all that hair,” Dr. Bupp said, eyeing Jameson on the monitor.
“You are looking great, little man,” Michael echoed in excitement. She has been a part of Jameson’s care as his genetics counselor since day one, and is excited to track progress.
His health had improved further. He’d grown more independent, too.
“He doesn’t fuss hardly at all,” Kayla said. “We used to have to sit and entertain him, but not any longer.”
His attention span had gotten better—he could watch TV, listen to music and bop along to his favorite tunes.
“It’s pretty crazy,” Kayla said. “We never imagined he would be able to do these things.”
During the virtual visit, his mom encouraged him to show his new skills.
He played tug of war with his dog. He sat up and climbed on and off the couch by himself.
“He tries so hard to do things on his own,” Darren said. “He’s so much more mobile that we had to do some child proofing.”
Jameson waved at the camera.
“He has lots to say,” Kayla said. “He doesn’t know his words yet but is using sign language.”
Dr. Bupp Julianne Michael updated the family on the progress of the trial medication.
“We heard from several other patients from around the world,” Dr. Bupp said.
The clinic is aware of a dozen patients with Bachman-Bupp syndrome now, with medical teams from across the globe reaching out for guidance.
The road ahead
Jameson and his family plan to return to Michigan in April to see Dr. Bupp and his team, marking the end of the dose increase phase of treatment.
Jameson can now scoot around a bit, but Kayla hopes he will be crawling on his own soon.
And she would like to see get him up on his hands and knees. She’s also hoping he’ll learn to eat on his own and perhaps even walk at some point, too.
“I can’t believe all this took was an actual diagnosis,” she said.
She hopes to continue spreading the word about rare diseases.
And, for parents and those who provide care to children with an undiagnosed condition, she says never give up.
Keep on seeking answers.
She suspects it will be bittersweet in April when the family reaches the point in treatment where their regular visits to Helen DeVos Children’s Hospital become less regular.
“These people been a part of our life for the past year,” she said. “It’s crazy how everything fell into place. I guess the rest will be history.”

































 /a>
/a>
 /a>
/a>
 /a>
/a>
This is truly amazing and a miracle and blessing for Jameson, Kayla and Darren. Thank you to the doctors and staff who have helped so much in Jameson’s Journey, as well as others journeys. Thank you for giving hope and light to those who are in need of answers and miracles.
What an amazing story. So happy that Jameson is getting stronger and on his healing path! Thank you for sharing.
What an amazing story! We just saw Dr. Bupp on TV this week about this very rare disease. How fortunate West Michigan is to have doctors like him here! Best wishes to these families in their ongoing journeys.
Congratulations to all of you and our warm best wishes.
It’s so exciting to see how genetic research can lead to medications that can target the abnormalities caused by the defect. These advances give so much hope to those impacted genetic diseases.