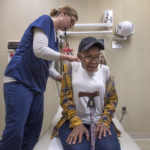
Macquilene Brown walked briskly through the Spectrum Health Lemmen-Holton Cancer Pavilion, her cane barely tapping the floor with each step, as she headed to her first radiation treatment.
“I still move around good,” she said. “I can’t run, but I can fight.”
The petite 81-year-old woman, who goes by Mac, held up her flowered cane and burst into laughter.
“I can fight with this,” she said.
In her fight against lung cancer, Mac is armed with more than a pretty cane and a sense of humor.
She also has the latest in diagnostic techniques. Recently, she underwent a first-in-the-U.S. biopsy that combined three leading-edge technologies—robotics, a real-time CT scan and electromagnetic navigation.
The precision medicine approach allowed her lung specialists at the Spectrum Health cancer clinic to safely biopsy and diagnose a stage 1 tumor that lay in the outer reaches of her upper left lung.
“It’s a good thing they caught it early. Thank God for that,” said Mac’s daughter, Sheila.
Mac’s lung specialists at Spectrum Health are excited about the potential the innovative approach offers to diagnose lung cancers in challenging cases, said interventional pulmonologist Gustavo Cumbo-Nacheli, MD. He performed the bronchoscopy along with John Egan, MD, also an interventional pulmonologist.
“We hope that our experience with this technology enhances our ability to reach difficult lesions and ensure a successful procedure,” Dr. Cumbo said.
And researchers are investigating whether the technique could be used not just to diagnose lung tumors, but to deliver treatments directly to them.
A spot on the lung
Mac grew up in Grand Rapids, Michigan, the oldest of 12 children. She moved to Tacoma, Washington, in the 1960s, had two children and began to work with the elderly.
After her mother’s death, she returned to Grand Rapids with her kids, so she could help raise some of her younger siblings.
She found a job as a housekeeper at Grand Rapids Home for Veterans and worked there for 23 years before she retired.
“I loved them old folks,” she said.
She smiled and added, “I knew one day I would be one of them.”
Now, she lives with her daughter, Sheila, who helps handle her medical details.
Last summer, as Mac underwent tests for another medical condition, her doctor found a lesion on her left lung that measured about ½ inch by ¾ inch.
To determine if it was cancerous, her pulmonologists needed to perform a biopsy. But the location, on the upper lung, would be challenging to reach.
In a traditional biopsy, physicians insert a needle through the chest into the lung. Given her age and emphysema, the doctors worried about the risk of a lung collapse.
In other cases, doctors perform a bronchoscopy, reaching the lesion with a scope inserted in the airway.
“Some spots are pretty easy to get to from the outside. And some lesions are easier to get to from the inside,” said Mac’s pulmonologist, Marc McClelland, MD. “Some, like the one Ms. Brown had, are kind of tough to get to from both ways.”
The interventional pulmonologists decided to bring the resources of three technologies together for a special kind of bronchoscopy.
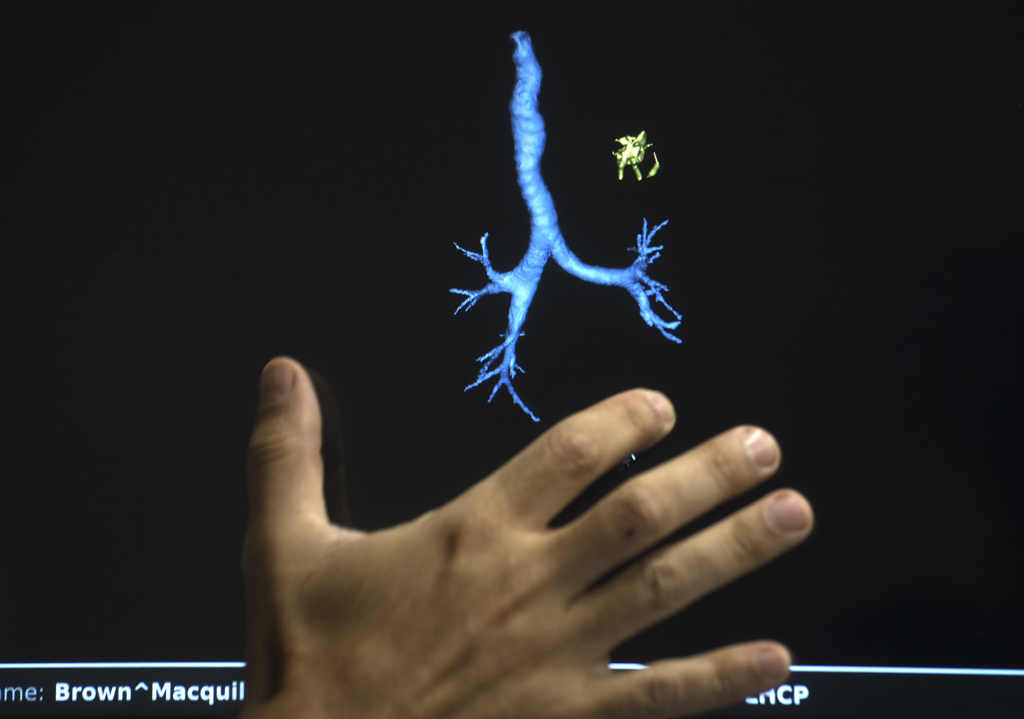
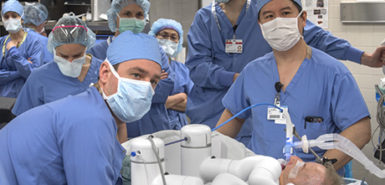
In an operating room at Spectrum Health Fred and Lena Meijer Heart Center, Drs. Cumbo and Egan performed the procedure. Above the operating table, a screen showed a 3D image of Mac’s lung, with a path to the lesion marked through her airways.
Using a bronchoscopy robot, the doctors operated a controller—which resembled a video game controller—to guide a bendable scope equipped with a camera through the airways and toward the lesion.
They were aided by an electromagnetic navigation system, similar to GPS for a car. But navigating lung airways is far more complicated than following a street map.
“The lungs are a dynamic organ. Every time a patient breathes, the lungs are moving,” Dr. Egan explained. “The airways are increasing in caliber and decreasing in caliber. And the lungs are constantly generating little bits of mucus.”
Once it reached the target area of the lung, the robotic scope placed a needle where they believed the lesion lay.
And that’s when the doctors performed a cone beam CT scan to obtain a 3D image of the lung at that moment.
It showed the instrument was placed in the precise location for a biopsy. If not, they would have made adjustments and rechecked their position.
“Even a few millimeters can make a difference between getting a diagnosis and not getting a diagnosis,” Dr. Egan said. “The cone beam CT allows us to get confirmation that we have arrived at our spot in real time.”
The scan was especially helpful for Mac, because she did not have a solid tumor, but one that grows along the airways, he added.
The physicians removed a specimen for examination. The lab analysis revealed stage 1 cancer.
Radiation therapy begins
For Mac, the advantage of the procedure was that she didn’t have a needle lung biopsy through her chest wall.
“I don’t like needles,” she said.
Because of health concerns, she did not undergo surgery to remove the tumor. Instead, she began a five-day series of radiation treatments.
She met with Dr. McClelland before the first one. They talked about options for her to quit smoking—such as taking Wellbutrin and using nicotine patches.
“I’m doing what you said to do. I’m trying to ease up on those cigarettes,” she said.
She recalled when she started smoking at 19.
“I was trying to be popular with the other girls and I got hooked,” she said.
Over the years, she has tried to kick the habit many times.
“Keep trying,” Dr. McClelland encouraged. “A lot of times people need to try several times before they actually quit.”
Mac is trying to take her diagnosis and treatment in stride.
“I haven’t worried over having this, because I put it in the hands of God,” she said. “Everything’s been wonderful.”
Exploring the next steps
In the future, Dr. Cumbo said interventional pulmonologists may use the system to treat the cancer in the same procedure—perhaps to deliver chemotherapy or perform an ablation. Researchers are investigating that possibility.
“I share the vision that a patient will someday come to Spectrum Health with an area of concern and walk out cancer-free the same day,” Dr. Cumbo said.
“This is really cutting edge,” Dr. Egan said.
“To treat and one day cure cancer, we are going to have to think out of the box. And using a robot and a live CT scan is thinking completely out of the box.”

















 /a>
/a>
 /a>
/a>
 /a>
/a>
What a blessing for Mac whom I know very well. Glad they were able to help her out with the tools and medicines. God is good all the time and God is good.
God is Good Auntie Mac, When you told me this back in September, Awesome story Trust Believe And have Faith you did all of this.
Latashia Bennett